Abstract
Lymph node enlargement is a common finding in children suggesting normal or benign. Palpable nodes which are large, hard or fixed must be examined carefully to rule out malignant diseases. In this case, a 15-year-old boy presented to our hospital to inspect the palpable mass at his post-auricular area being found 2 months ago. It was diagnosed as nodal marginal zone lymphoma (NMZL) through excisional biopsy and immunohistochemistry. NMZL is very rare, especially in children and young adults, but occurs locally in most cases with a good prognosis compared to adults. We described a rare case of NMZL diagnosed in adolescent.
REFERENCES
1. Ataş E, Kesik V, Fidancı MK, Kısmet E, Köseoğlu V. Evaluation of children with lympadenopathy. Turk Pediatri Ars. 2014; 49:30–35.

2. Park YW. Evaluation of neck masses in children. Am Fam Physician. 1995; 51:1904–1912.
3. Gosche JR, Vick L. Acute, subacute, and chronic cervical lymphadenitis in children. Semin Pediatr Surg. 2006; 15:99–106.

4. Friedmann AM. Evaluation and management of lymphadenopathy in children. Pediatr Rev. 2008; 29:53–60.

5. Quintanilla-Martinez L, Sander B, Chan JK, Xerri L, Ott G, Campo E, et al. Indolent lymphomas in the pediatric population: follicular lymphoma, IRF4/MUM1+ lymphoma, nodal marginal zone lymphoma and chronic lymphocytic leukemia. Virchows Arch. 2016; 468:141–157.

6. Angelopoulou MK, Kalpadakis C, Pangalis GA, Kyrtsonis MC, Vassilakopoulos TP. Nodal marginal zone lymphoma. Leuk Lymphoma. 2014; 55:1240–1250.

7. Taddesse-Heath L, Pittaluga S, Sorbara L, Bussey M, Raffeld M, Jaffe ES. Marginal zone B-cell lymphoma in children and young adults. Am J Surg Pathol. 2003; 27:522–531.

8. Petit B, Chaury MP, Le Clorennec C, Jaccard A, Gachard N, Moalic-Judge S, et al. Indolent lymphoplasmacytic and marginal zone B-cell lymphomas: absence of both IRF4 and Ki67 expression identifies a better prognosis subgroup. Haematologica. 2005; 90:200–206.
9. van den Brand M, van Krieken JH. Recognizing nodal marginal zone lymphoma: recent advances and pitfalls. A systematic review. Haematologica. 2013; 98:1003–1013.
10. Au WY, Ma SY, Chim CS, Choy C, Loong F, Lie AK, et al. Clinicopathologic features and treatment outcome of mature T-cell and natural killer-cell lymphomas diagnosed according to the World Health Organization classification scheme: a single center experience of 10 years. Ann Oncol. 2005; 16:206–214.

Fig. 1.
A palpable, fixed 3×2-cm-sized mass positioning at the left posterior auricular area (arrowheads).
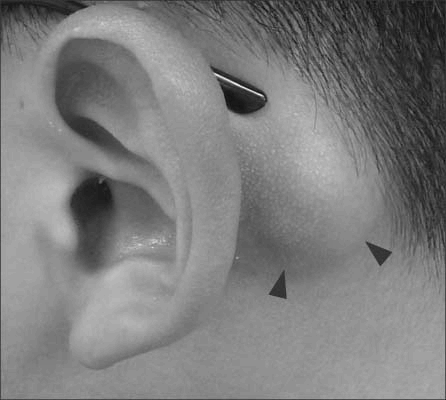
Fig. 2.
Ultrasonographic image showing a hypoechoic lobulated mass, with 2.2×2.4×0.8 cm size and inner vascularity (arrowheads).
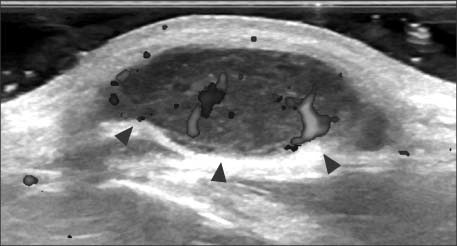
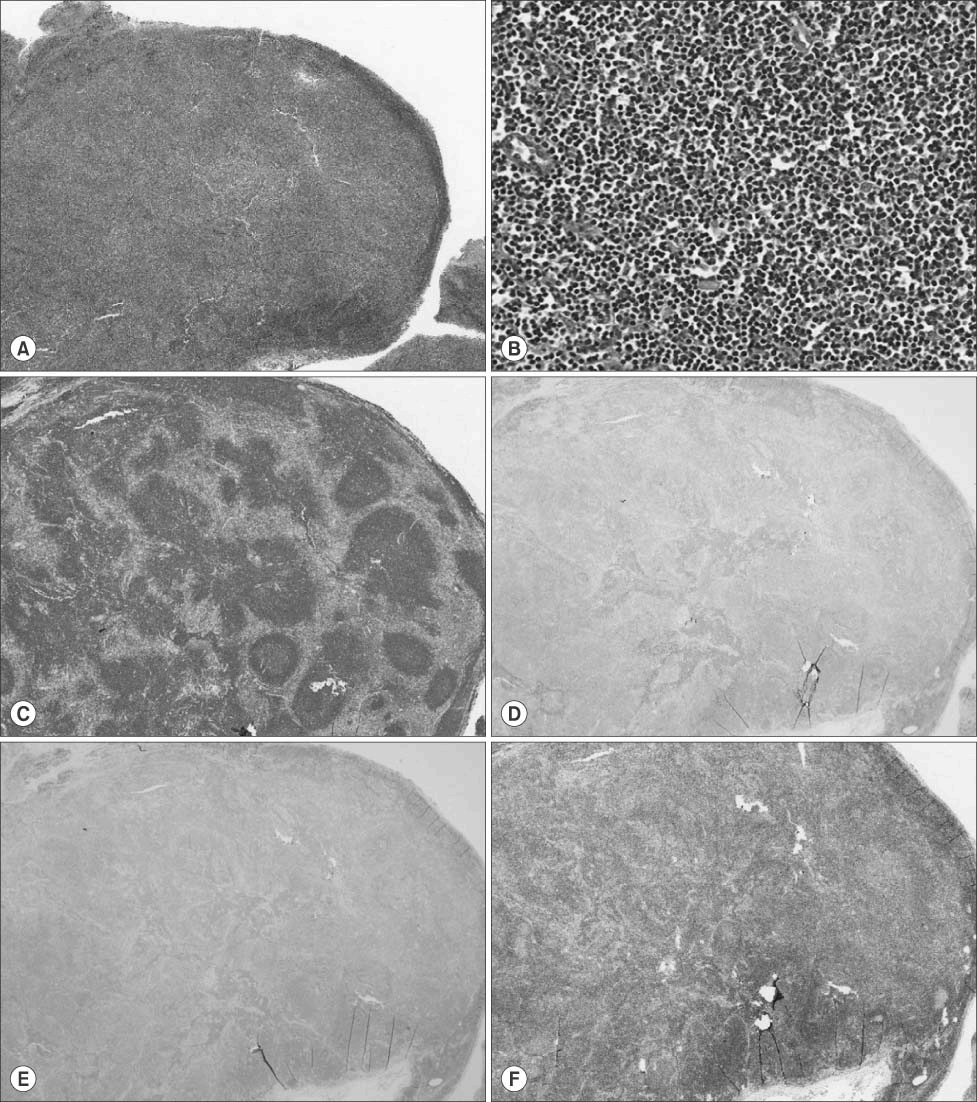
Fig. 3.
Immunophenotypic features of excised mass. (A) H&E stain (×40) showing a gross lymphoid tissue with effaced normal follicular architectures suggesting neoplastic rather than reactive condition. (B) With a few normal germinal centers left, it was mostly filled with diffusely grown small to medium-sized atypical cells (H&E stain, ×200). These cells were positive in CD20 (B lymphocyte antigen; C) and Bcl-2 (F) but negative in CD10 (D) and Bcl-6 (E) (C-F: ×40).




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download