Abstract
Erythromelalgia (EM) is an uncommon disorder characterized by redness, heat, and painful extremities with intense burning sensation. Attacks of EM may be worsened by limb warming, exercise, or dependency of the affected extremity. Although the coexistence of EM and Raynaud's phenomenon (RP) may appear to be opposites in symptomatology and clinical presentation, recent studies provide an explanation based on a dysfunction of the regulation of vasomotor tone. Here, we report a case of EM in a patient with RP.
REFERENCES
1. Kurzrock R, Cohen PR. Erythromelalgia: review of clinical characteristics and pathophysiology. Am J Med. 1991; 91:416–22.

2. Chadachan V, Dean SM, Eberhardt RT. Cutaneous changes in peripheral arterial vascular disease. Goldsmith LA, Katz SI, Gilchrest BA, Paller AS, Leffell DJ, Wolff K, editors. Fitzpatrick's dermatology in general medicine. 8th ed.New York: McGraw-Hill;2012. p. 2108–9.
3. Drenth JP, te Morsche RH, Michiels JJ. From gene to disease; primary erythermalgia–a neuropathic disease as a consequence of mutations in a sodium pump gene. Ned Tijdschr Geneeskd. 2006; 150:194–6.
4. Paira S, Cassano G, Korol V, Ortiz A, Roverano S. Erythromelalgia with subsequent digital necrosis, glomerulonephritis, and antiphospholipid antibodies. J Clin Rheumatol. 2005; 11:209–12.

5. Berlin AL, Pehr K. Coexistence of erythromelalgia and Raynaud's phenomenon. J Am Acad Dermatol. 2004; 50:456–60.

6. Sunahara JF, Gora-Harper ML, Nash KS. Possible eryth-romelalgia-like syndrome associated with nifedipine in a patient with Raynaud's phenomenon. Ann Pharmacother. 1996; 30:484–6.

8. Kalgaard OM, Seem E, Kvernebo K. Erythromelalgia: a clinical study of 87 cases. J Intern Med. 1997; 242:191–7.

9. Werth VP. Clinical manifestations of cutaneous lupus erythematosus. Autoimmun Rev. 2005; 4:296–302.

10. Uva L, Miguel D, Pinheiro C, Freitas JP, Marques Gomes M, Filipe P. Cutaneous manifestations of systemic lupus erythematosus. Autoimmune Dis. 2012; 2012; 834291.

11. Kammer GM, Soter NA, Schur PH. Circulating immune complexes in patients with necrotizing vasculitis. Clin Immunol Immunopathol. 1980; 15:658–72.

12. Badeloe S, Henquet CJ, Nieuwhof CM, Frank J. Secondary erythromelalgia involving the ears probably preceding lupus erythematosus. Int J Dermatol. 2007; 46(Suppl 3):6–8.

14. Eisler T, Hall RP, Kalavar KA, Calne DB. Erythromelalgia-like eruption in parkinsonian patients treated with bro-mocriptine. Neurology. 1981; 31:1368–70.

15. Davis MD, O'Fallon WM, Rogers RS 3rd, Rooke TW. Natural history of erythromelalgia: presentation and outcome in 168 patients. Arch Dermatol. 2000; 136:330–6.
Figure 1.
(A) Diffuse redness with mild swelling on the both sole. (B) Grouped bean sized violaceous macules on the medial side of right heel. (C) Bluish cyanotic changes on the left 2nd, 4th, and 5th fingers.
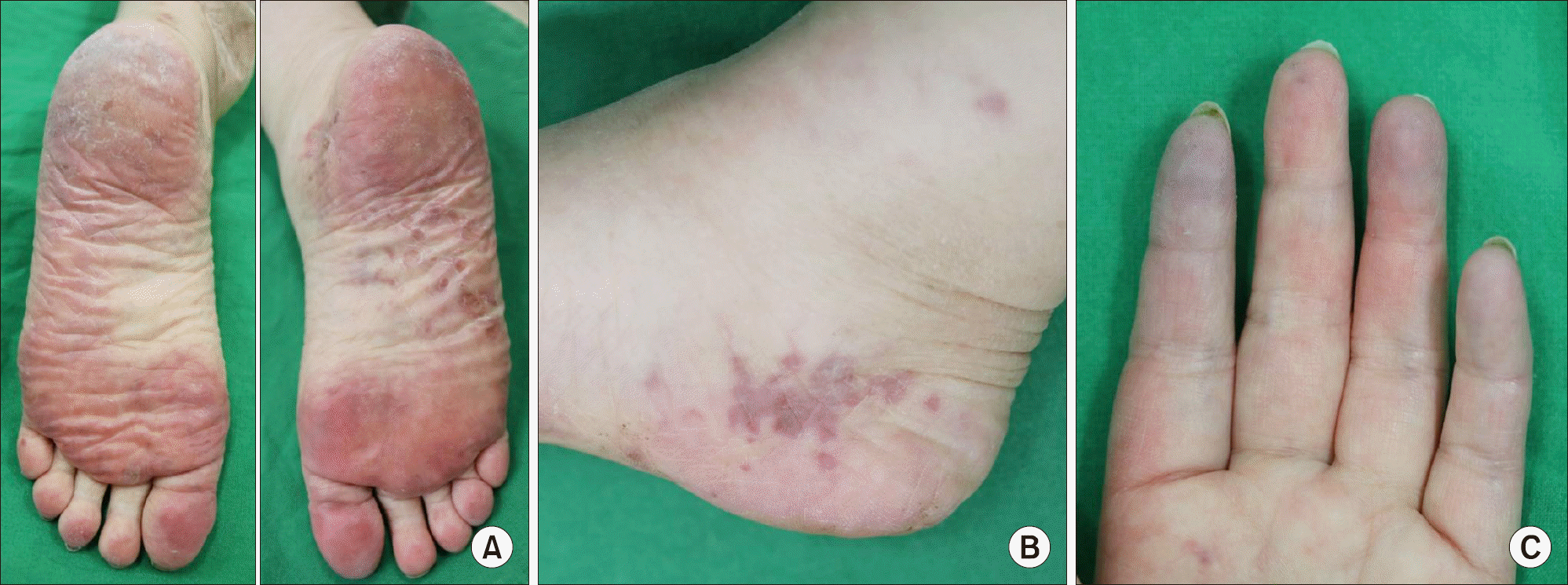
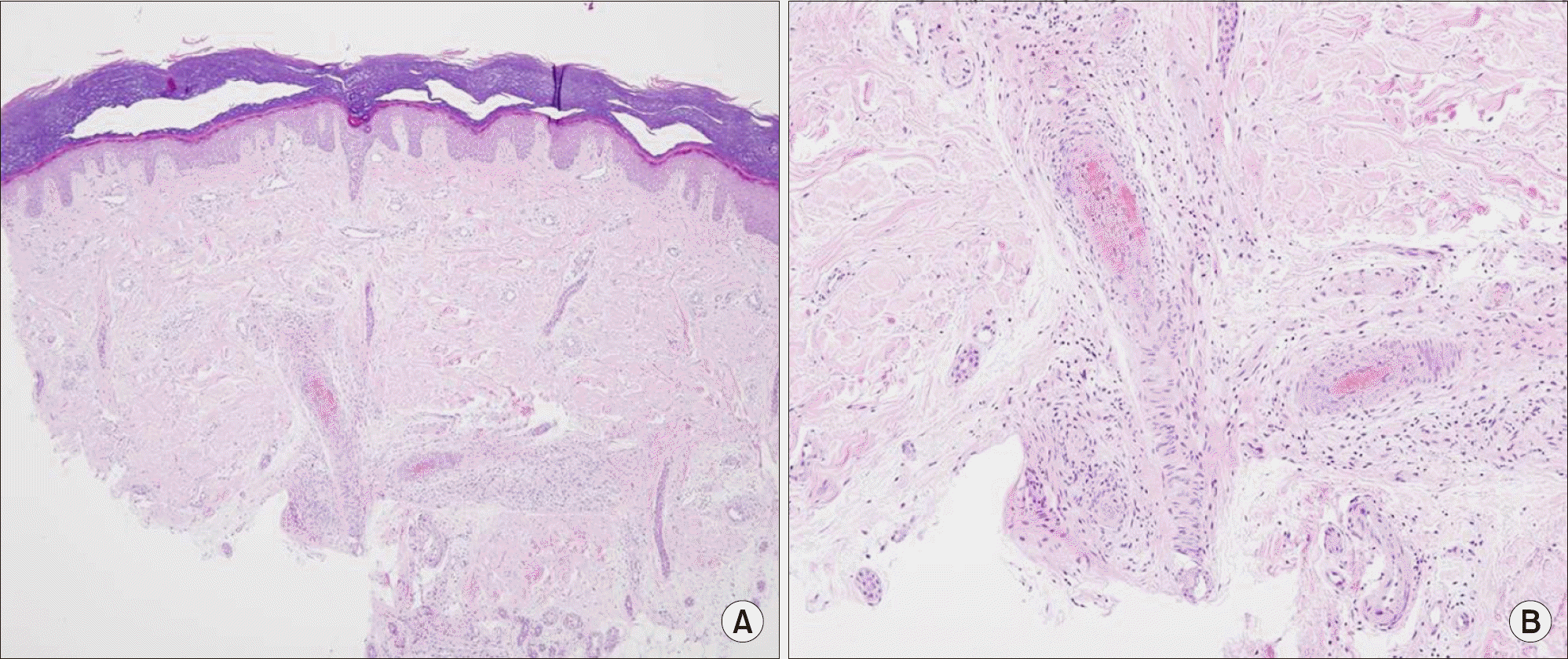
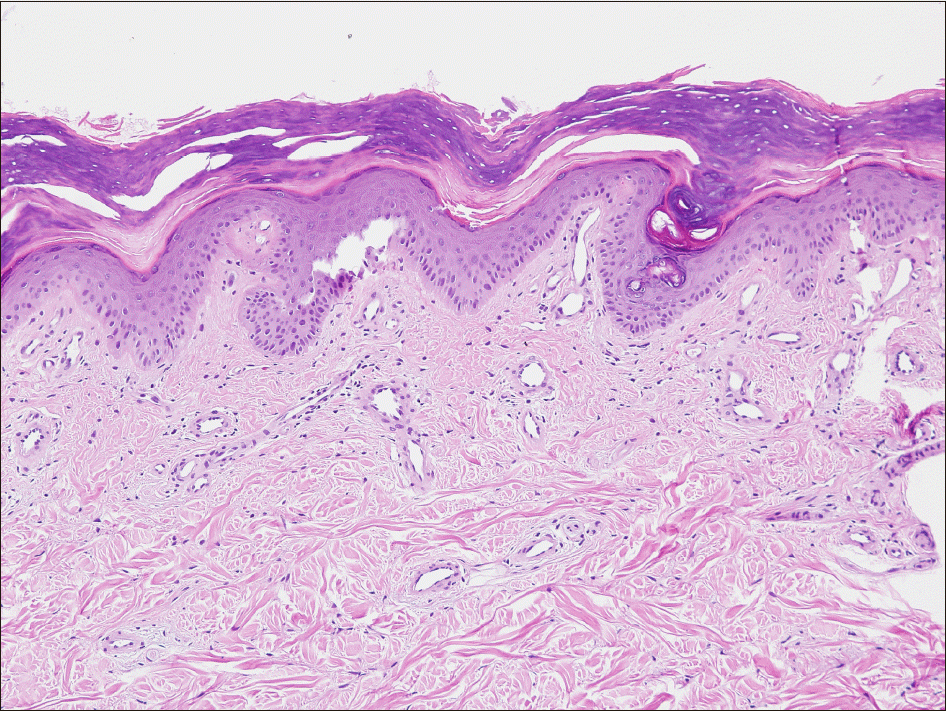
Figure 2.
(A) Compact hyperkeratosis, irregular rete ridge, dilated vessels in the papillary dermis and small sized vessels with fibrin thrombi in the mid-dermis (H&E, ×40). (B) High-power view showing vessel dilatation with vessel endothelial hyperplasia, fibrin thrombi, fibrinous necrosis and mild perivascular and vascular lymphocytic infiltration (H&E, ×100).




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download