Abstract
Vasculitis is a heterogeneous group of diseases that destroy blood vessel walls by inflammation. Approximately half of vasculitis cases are idiopathic, but sometimes associated with genetic factors, medicines, chronic infection, autoimmune diseases, and malignancies. Although the mechanism remains unclear, vasculitis secondary to malignancy, also known as paraneoplastic vasculitis, has been reported. It is generally associated with hematologic malignancies rather than solid malignancies and commonly presents as leukocytoclastic vasculitis or polyarteritis nodosa. We experienced a case of leukocytoclastic vasculitis in a patient with hepatocellular carcinoma and membranous obstruction of the inferior vena cava. Here, we report this case with a brief review of literature.
REFERENCES
1. Lie JT. Nomenclature and classification of vasculitis: plus ça change, plus c'est la même chose. Arthritis Rheum. 1994; 37:181–6.

2. Tai YJ, Chong AH, Williams RA, Cumming S, Kelly RI. Retrospective analysis of adult patients with cutaneous leukocytoclastic vasculitis. Australas J Dermatol. 2006; 47:92–6.

3. Campanile G, Hautmann G, Lotti TM. The etiology of cutaneous necrotizing vasculitis. Clin Dermatol. 1999; 17:505–8.

4. Sánchez-Guerrero J, Gutiérrez-Ureña S, Vidaller A, Reyes E, Iglesias A, Alarcón-Segovia D. Vasculitis as a paraneoplastic syndrome. Report of 11 cases and review of the literature. J Rheumatol. 1990; 17:1458–62.
6. Ghersetich I, Comacchi C, Jorizzo JL, Katsambas A, Lotti TM. Proposal for a working classification of cutaneous vasculitis. Clin Dermatol. 1999; 17:499–503.

7. Buggiani G, Krysenka A, Grazzini M, Vašků V, Hercogová J, Lotti T. Paraneoplastic vasculitis and paraneoplastic vascular syndromes. Dermatol Ther. 2010; 23:597–605.

8. Greer JM, Longley S, Edwards NL, Elfenbein GJ, Panush RS. Vasculitis associated with malignancy. Experience with 13 patients and literature review. Medicine (Baltimore). 1988; 67:220–30.

9. Allen NB, Bressler PB. Diagnosis and treatment of the systemic and cutaneous necrotizing vasculitis syndromes. Med Clin North Am. 1997; 81:243–59.

10. Nowack R, Flores-Suárez LF, van der Woude FJ. New developments in pathogenesis of systemic vasculitis. Curr Opin Rheumatol. 1998; 10:3–11.

11. Simson IW. Membranous obstruction of the inferior vena cava and hepatocellular carcinoma in South Africa. Gastroenterology. 1982; 82:171–8.

Figure 1.
(A) Vascular purpura on both lower limb with the swelling of both ankle joint. (B) Inflammatory cells are predominantly infiltrated in dermal blood vessels. Epidermis is unremarkable (H&E, ×100). (C) Dermal vessels are damaged, showing swollen endothelial cells and deposition of eosinophilic fibrin within and around vascular walls. Infiltrated inflammatory cells are largely neutrophils, and associated with nuclear fragmentation (H&E, ×400).
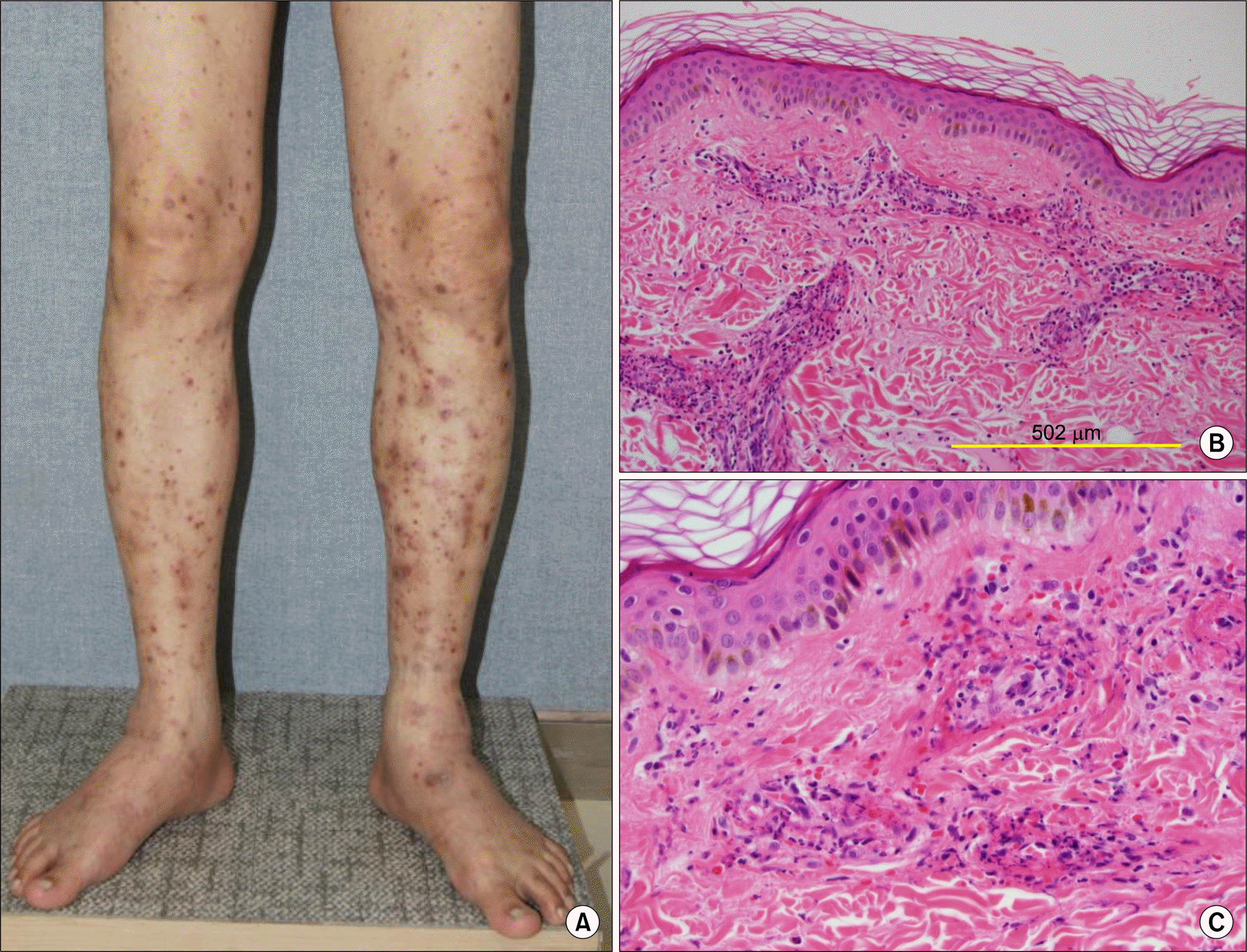
Figure 2.
(A) Axial dynamic-enhanced computed tomography (CT) scan. On an arterial-enhanced CT image, a small enhancing nodule was seen in right lobe of the liver (segment 7) measuring approximately 12 mm in diameter (arrow). (B) Inferior vena cava (IVC) gram shows short segment occlusion in intrahepatic portion of IVC (arrows) and severe distension of IVC distal to occlusive lesion (arrowheads).
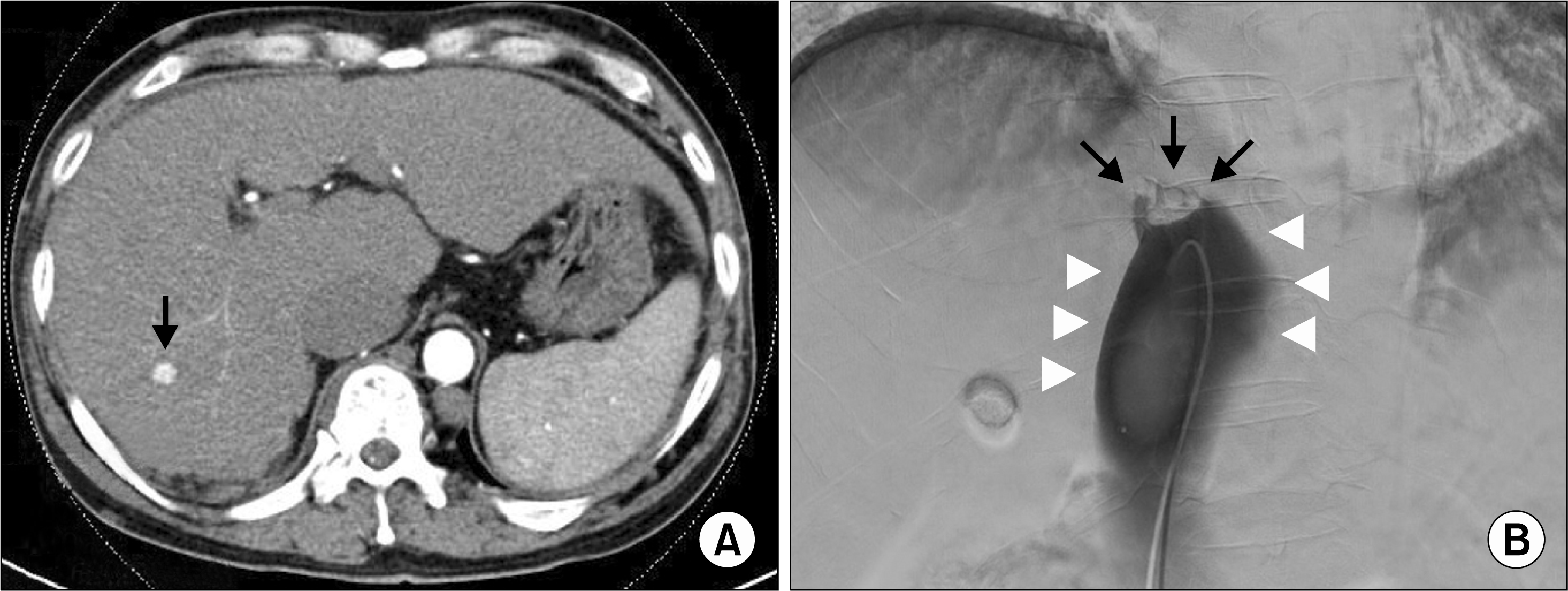
Table 1.
Comparison of characteristics of paraneoplastic LCV and paraneoplastic PAN




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download