Abstract
Eosinophilic granulomatosis with polyangiitis (EGPA), previously called Churg-Strauss syndrome, is an antineutrophil cytoplasmic antibody associated vasculitis, accompanied by asthma, hypereosinophilia, nonfixed pulmonary infiltrates, and sinusitis. Peripheral neuropathy is common in patients with EGPA; however, a few cases of EGPA with central nervous system (CNS) involvement have been reported. A 45-year-old female referred for right side weakness and posterior neck pain was diagnosed as EGPA with subarachnoid hemorrhage and mononeuritis multiplex. She was effectively treated with a high dose glucocorticoid, cyclophosphamide, and intravenous immunoglobulin. EGPA with CNS involvement is uncommon and causes significant morbidity and mortality. Therefore more rapid and accurate diagnostic evaluation may be required. EGPA should be considered in patients with neurological symptoms and hypereosinophilia.
REFERENCES
2. Masi AT, Hunder GG, Lie JT, Michel BA, Bloch DA, Arend WP, et al. The American College of Rheumatology 1990 criteria for the classification of Churg-Strauss syndrome (allergic granulomatosis and angiitis). Arthritis Rheum. 1990; 33:1094–100.

4. Baldini C, Talarico R, Della Rossa A, Bombardieri S. Clinical manifestations and treatment of Churg-Strauss syndrome. Rheum Dis Clin North Am. 2010; 36:527–43.

5. Cheng MJ, Huang PH, Liao PW, Chen JT, Chiang TR. Multiple cerebral and cerebellar infarcts as the first clinical manifestation in a patient with Churg-Strauss syndrome: case report and literature review. Acta Neurol Taiwan. 2012; 21:169–75.
6. Nam TS, Jung HJ, Kim JT, Park MS, Kim BC, Kim MK, et al. Churg-Strauss syndrome complicated with intracerebral hemorrhage. J Korean Neurol Assoc. 2009; 27:257–9.
7. Go MH, Park JU, Kang JG, Lim YC. Subarachnoid and intracerebral hemorrhage in patients with Churg-Strauss syndrome: two case reports. J Cerebrovasc Endovasc Neurosurg. 2012; 14:255–61.

8. Mouthon L, Dunogue B, Guillevin L. Diagnosis and classification of eosinophilic granulomatosis with polyangiitis (formerly named Churg-Strauss syndrome). J Autoimmun. 2014; 48-49:99–103.

9. Vaglio A, Buzio C, Zwerina J. Eosinophilic granulomatosis with polyangiitis (Churg-Strauss): state of the art. Allergy. 2013; 68:261–73.

10. Calvo-Romero JM, del Carmen Bonilla-Gracia M, Bureo-Dacal P. Churg-Strauss syndrome presenting as spontaneous subarachnoid haemorrhage. Clin Rheumatol. 2002; 21:261–3.

11. Sakamoto S, Ohba S, Eguchi K, Shibukawa M, Kiura Y, Okazaki T, et al. Churg-Strauss syndrome presenting with subarachnoid hemorrhage from ruptured dissecting aneurysm of the intracranial vertebral artery. Clin Neurol Neurosurg. 2005; 107:428–31.

12. Sheerin UM, Barreto J, Brown MM, Brew S, Losseff NA. Subarachnoid haemorrhage as the first clinical manifestation of Churg-Strauss syndrome. J Neurol. 2008; 255:607–8.

13. Menditto VG, Di Rienzo A, De Nicola M, Balzano L, Polonara S. Subarachnoid haemorrhage from PICA aneurysm rupture in a Churg-Strauss patient: a case report and a review of the literature. Clin Neurol Neurosurg. 2013; 115:197–9.

Figure 1.
(A) Non-contrast-enhanced brain computed tomography image demonstrated subarachnoid hemorrhage in basal cistern, suprasellar cistern, perimesencephalic cistern and pre-pontine cistern. (B) Volume-ren-dered cerebral angiography image shows mild segmental stenosis at the P2 segment of left posterior cerebral artery (arrow).
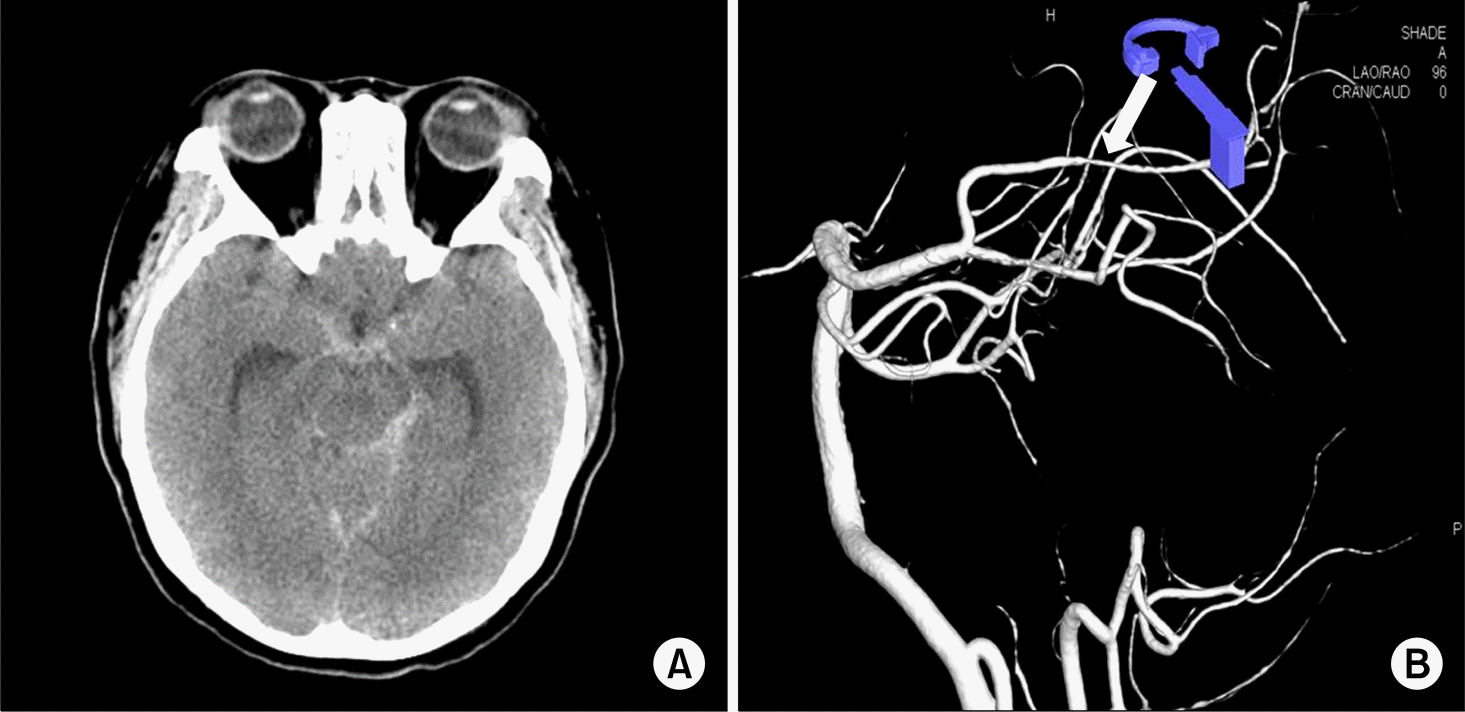
Figure 2.
This chest computed tomography shows diffuse ground glass opacity, interlobular septal thickening. Small nodular lesion was seen in peripheral left upper lobe and right middle lobe (arrow).
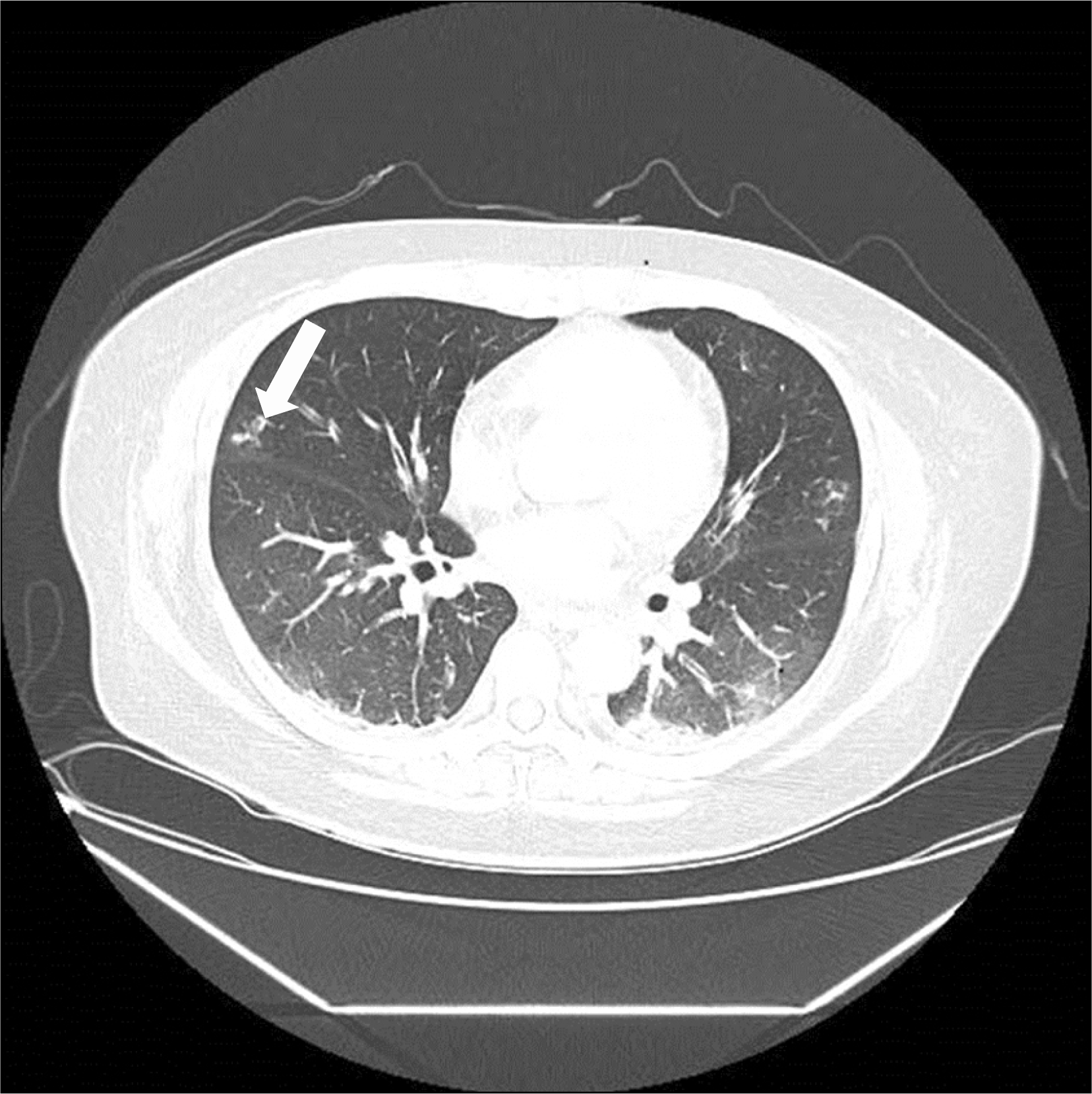
Figure 3.
The progress report of this patient. Eosinophil count, antineutrophil cytoplasmic antibody (ANCA) titer and peripheral neuropathy are improved gradually after administration of high dose methylprednisolone, cylclophosphamide and intravenous immunoglobulin (IVIG).
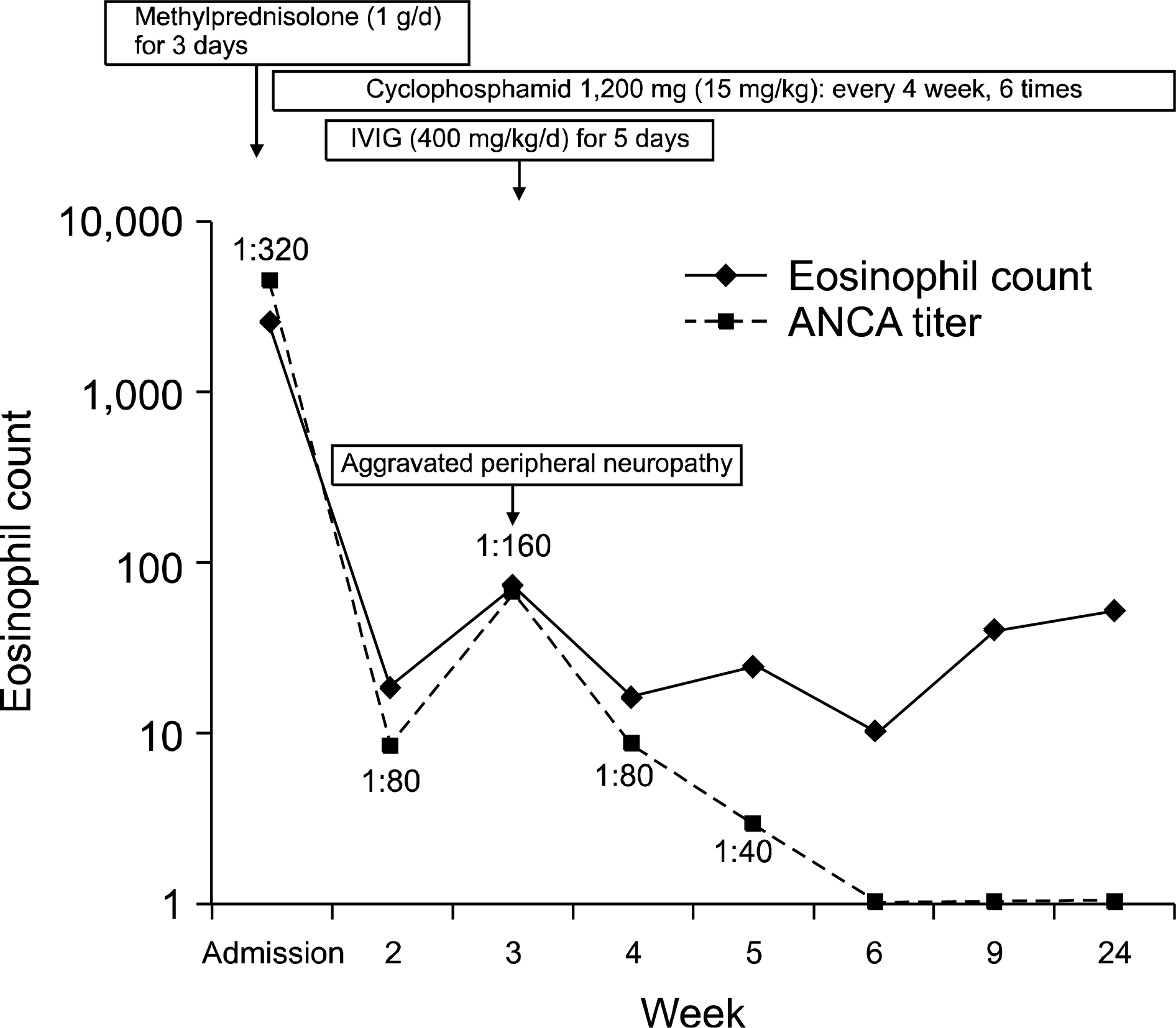
Table 1.
Summary of reports of subarachnoid hemorrhage in eosinophilic granulomatosis with polyangiitis patients




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download