Abstract
Dermatomyositis, an idiopathic inflammatory myopathy with characteristic skin manifestations, is associated with several types of cancer. Only three cases of gallbladder cancer with dermatomyositis have been reported world-wide, and none has been reported in Korea. We present a case of a 71-year-old male with proven dermatomyositis associated with gallbladder cancer to emphasize the necessity of work-up for malignancies with low incidence in patients with inflammatory myopathies.
REFERENCES
1. Bohan A, Peter JB. Polymyositis and dermatomyositis (second of two parts). N Engl J Med. 1975; 292:403–7.
2. Stertz B. Polymyositis. Berl Klin Wochenschr. 1916; 53:489–90.
3. Chakravarty E, Genovese MC. Rheumatic syndromes associated with malignancy. Curr Opin Rheumatol. 2003; 15:35–43.

4. Buchbinder R, Forbes A, Hall S, Dennett X, Giles G. Incidence of malignant disease in biopsy-proven inflammatory myopathy. A population-based cohort study. Ann Intern Med. 2001; 134:1087–95.

5. Sigurgeirsson B, Lindelöf B, Edhag O, Allander E. Risk of cancer in patients with dermatomyositis or polymyositis. A population-based study. N Engl J Med. 1992; 326:363–7.
6. Lee SW, Jung SY, Park MC, Park YB, Lee SK. Malignancies in Korean patients with inflammatory myopathy. Yonsei Med J. 2006; 47:519–23.

7. Jung KW, Park S, Kong HJ, Won YJ, Lee JY, Seo HG, et al. Cancer statistics in Korea: incidence, mortality, survival, and prevalence in 2009. Cancer Res Treat. 2012; 44:11–24.

8. Randi G, Franceschi S, La Vecchia C. Gallbladder cancer worldwide: geographical distribution and risk factors. Int J Cancer. 2006; 118:1591–602.

9. Azuma K, Yamada H, Ohkubo M, Yamasaki Y, Yamasaki M, Mizushima M, et al. Incidence and predictive factors for malignancies in 136 Japanese patients with dermatomyositis, polymyositis and clinically amyopathic dermatomyositis. Mod Rheumatol. 2011; 21:178–83.

10. Kundu AK, Karmakar PS, Bera AB, Pal SK. Carcinoma of the gall bladder presenting as dermatomyositis. J Assoc Physicians India. 2005; 53:219–22.
11. Narasimhaiah DA, Premkumar JA, Moses V, Chacko G. Carcinoma of gall bladder presenting as dermatomyositis. Ann Indian Acad Neurol. 2011; 14:44–6.

12. Yiannopoulos G, Ravazoula P, Meimaris N, Stavropoulos M, Andonopoulos AP. Dermatomyositis in a patient with adenocarcinoma of the gall bladder. Ann Rheum Dis. 2002; 61:663–4.

13. Casciola-Rosen L, Nagaraju K, Plotz P, Wang K, Levine S, Gabrielson E, et al. Enhanced autoantigen expression in regenerating muscle cells in idiopathic inflammatory myopathy. J Exp Med. 2005; 201:591–601.

14. Iorizzo LJ 3rd, Jorizzo JL. The treatment and prognosis of dermatomyositis: an updated review. J Am Acad Dermatol. 2008; 59:99–112.

Figure 1.
(A) Gottron's papules on the right hand. (B) Heliotrope rash and a forehead erythematous patch. (C) V sign, Shawl sign, and erythematous patches on both shoulders and the left anterior chest wall.
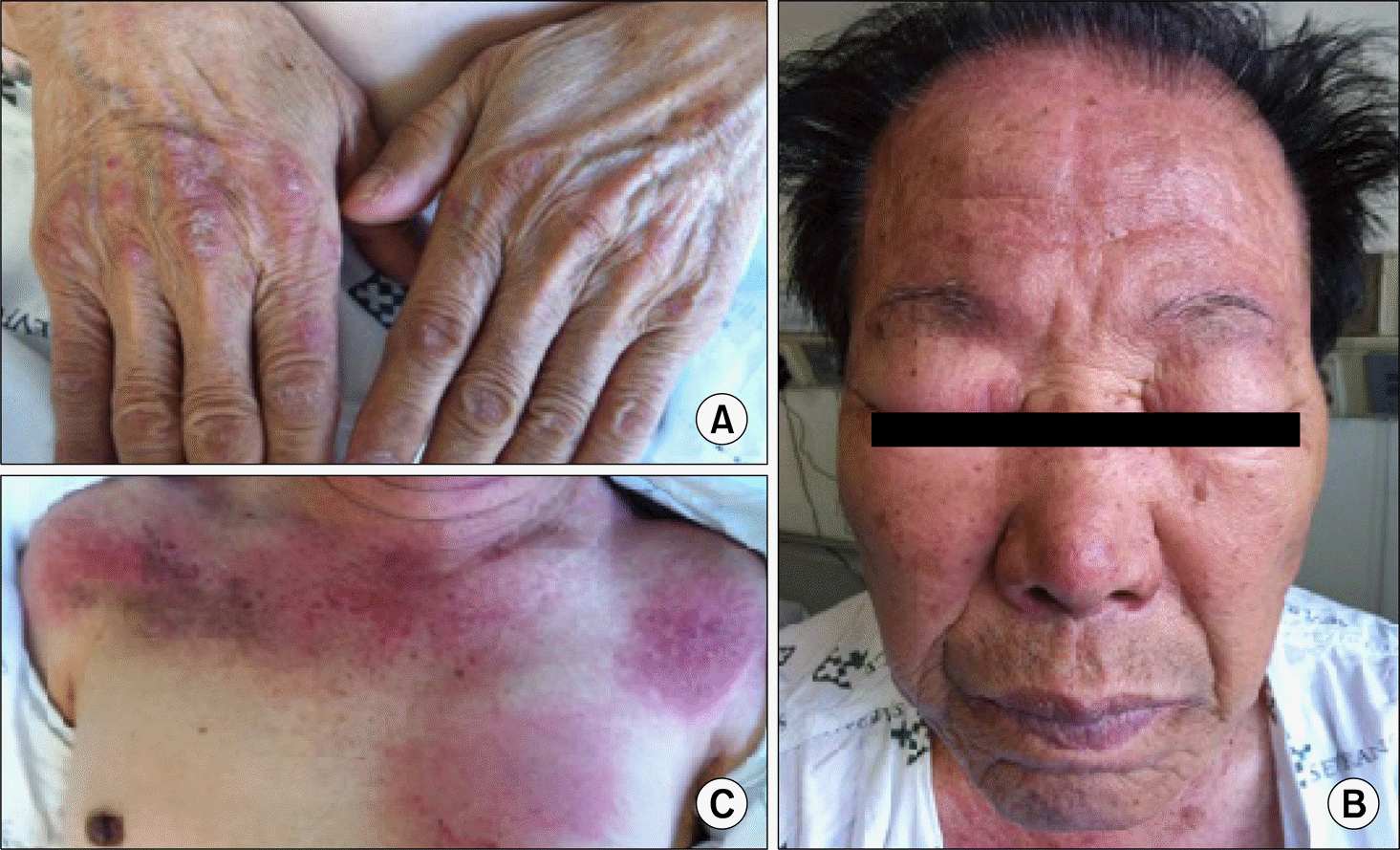
Figure 2.
PET/CT scan. Diffuse and mild fluorodeoxyglucose uptake in skeletal muscle was seen (black arrow), which likely indicates inflammatory changes due to dermatomyositis involvement. Fluorodeoxyglucose uptake in the disrupted gallbladder wall (white arrow) and pericholecystic fat infiltration in the gallbladder body were seen.
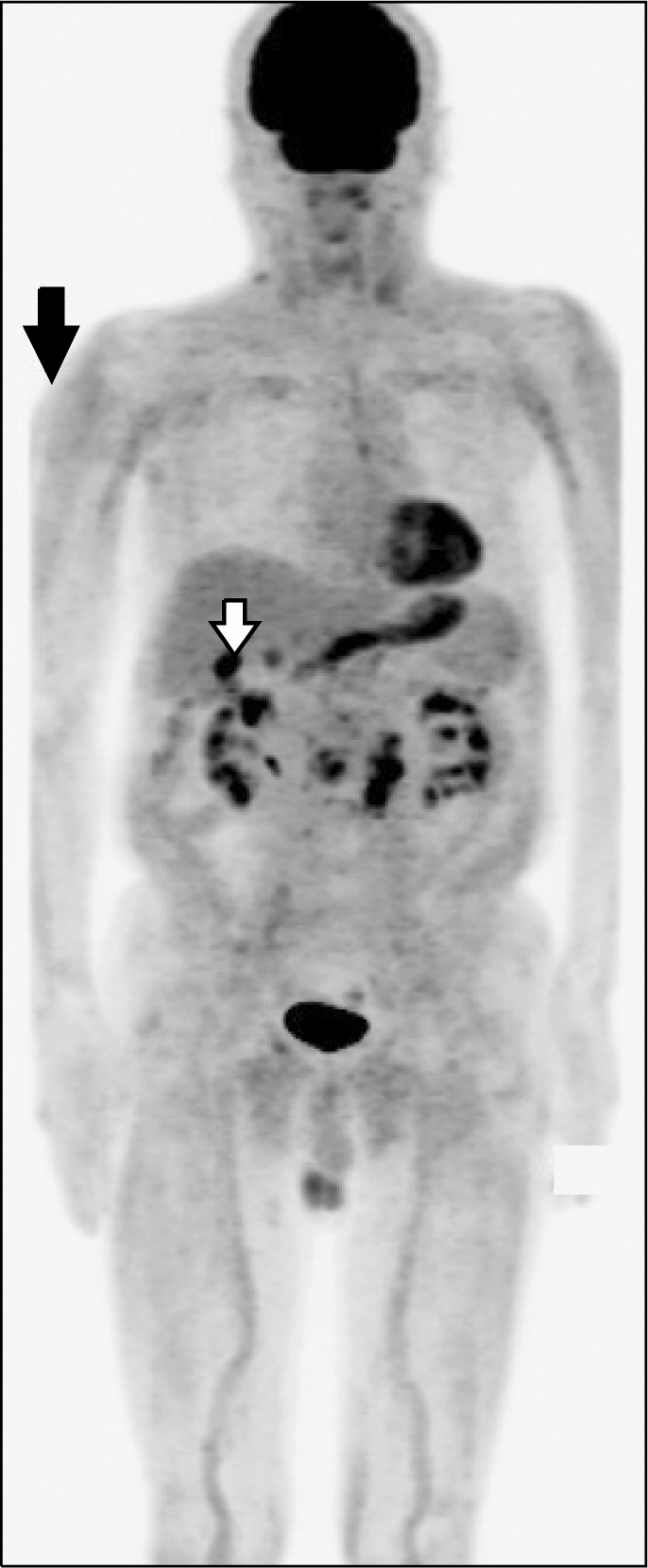
Figure 3.
Biliary dynamic CT scan. (A) Irregular wall thickening of the gallbladder with pericholecystic fat infiltration and GB cancer with serosa invasion (T3). (B) Enlarged lymph nodes were seen at the cystic duct, portahepatis, portocaval, and bilateral para-aortic space, which are suggestive of metastatic lymph nodes.
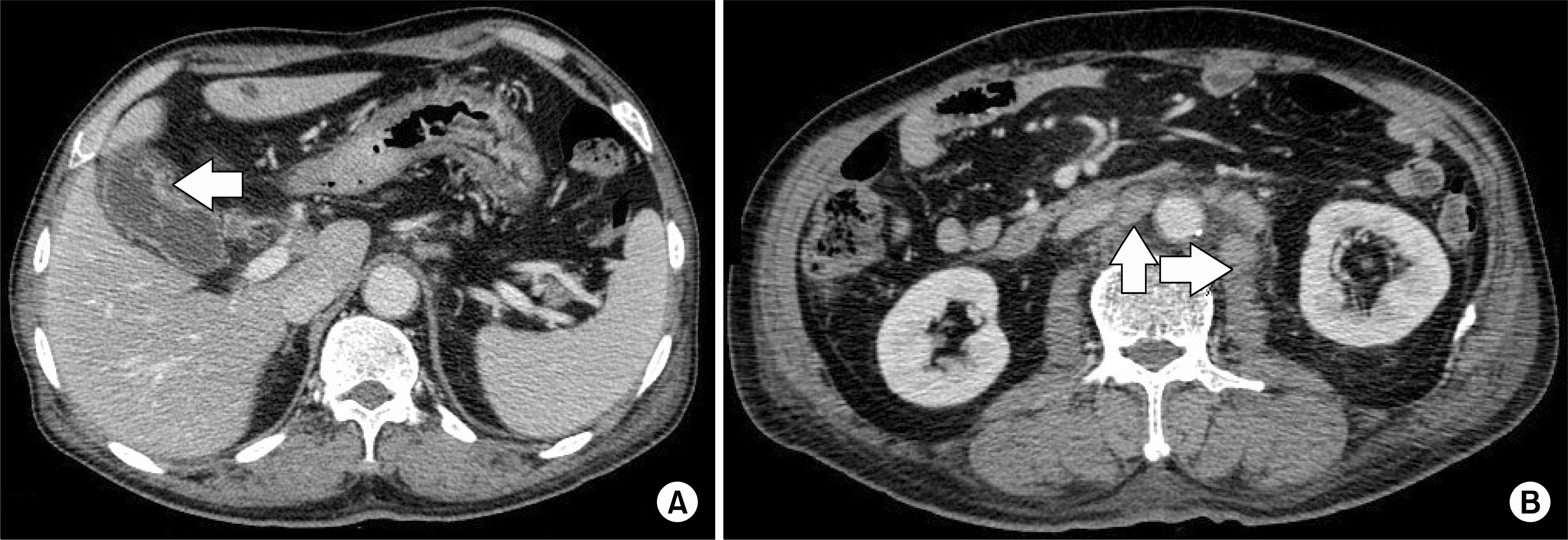
Figure 4.
Changes in muscle enzyme levels. (A) aspartate aminotransferase (AST, normal range: 13.0∼34.0 IU/L), (B) creatine phosphokinase (CK, normal range: 44∼245 IU/L); day 1: admission, day 7: beginning administration of low-dose prednisolone, day 14-day 49: concurrent chemoradiotherapy, day 75: CT imaging after concurrent chemoradiotherapy, day 90: planned chemotherapy, long arrow: administration of prednisolone, short arrows: 5-FU administration.
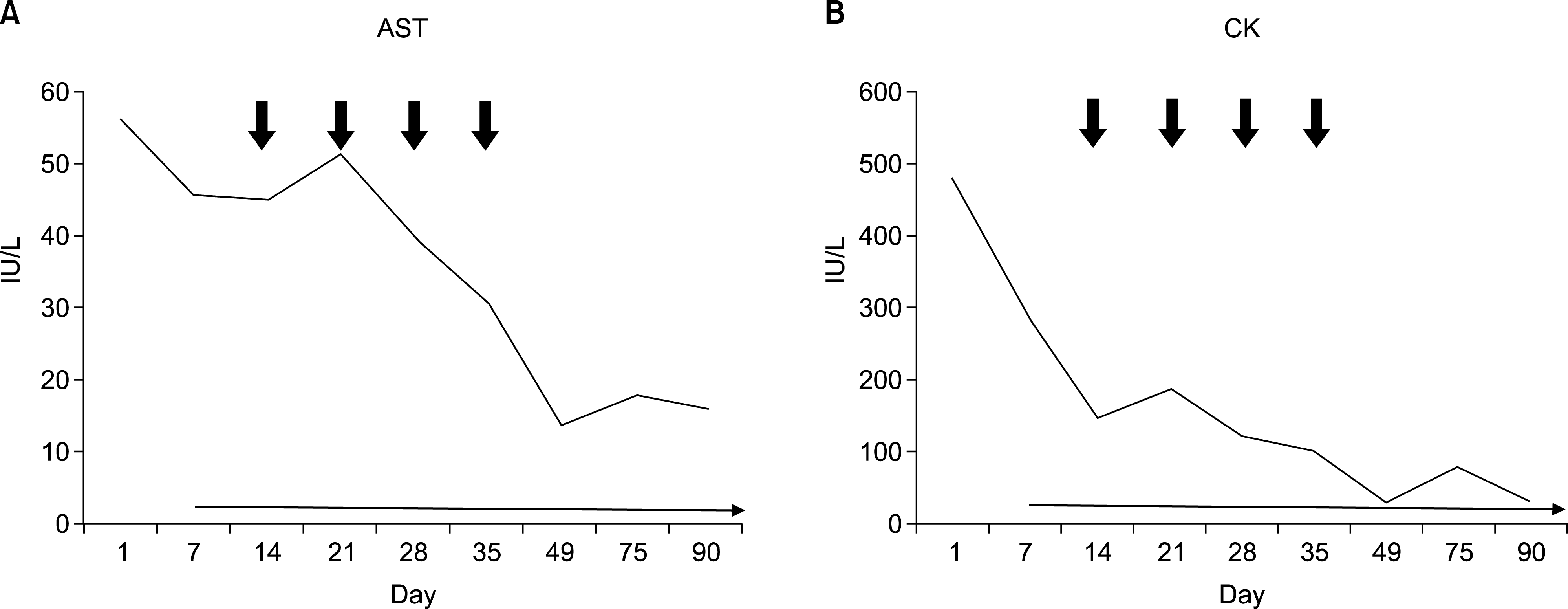
Table 1.
Comparison of three cases of dermatomyositis accompanied by gallbladder cancer that have been reported to date plus this case




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download