Abstract
Ureteral obstruction caused by a fungal ball is rare. Diabetes mellitus and immunocompromised conditions constitute the predisposing factors. Urosepsis due to unilateral ureteral obstruction with a fungal ball is extremely rare. The radiologic findings of fungal ball have been described as nonspecific. We report on a female patient with urosepsis that occurred by unilateral ureteral obstruction by a fungal ball, mimicking a ureteral stone. She was managed with systemic antibiotics, percutaneous nephrostomy, and ureteroscopic fungal ball removal.
REFERENCES
1. Shimada S, Nakagawa H, Shintaku I, Saito S, Arai Y. Acute renal failure as a result of bilateral ureteral obstruction by Candida albicans fungus balls. Int J Urol. 2006; 13:1121–2.

2. Fisher JF, Chew WH, Shadomy S, Duma RJ, Mayhall CG, House WC. Urinary tract infections due to Candida albicans. Rev Infect Dis. 1982; 4:1107–18.

3. Irby PB, Stoller ML, McAninch JW. Fungal bezoars of the upper urinary tract. J Urol. 1990; 143:447–51.

4. Davis NF, Smyth LG, Mulcahy E, Scanlon T, Casserly L, Flood HD. Ureteric obstruction due to fungus-ball in a chronically immunosuppressed patient. Can Urol Assoc J. 2013; 7:E355–8.

5. Dellinger RP, Levy MM, Rhodes A, Annane D, Gerlach H, Opal SM, et al. Surviving Sepsis Campaign Guidelines Committee including The Pediatric Subgroup. Surviving Sepsis Campaign: international guidelines for management of severe sepsis and septic shock, 2012. Intensive Care Med. 2013; 39:165–228.

6. Anthony JS, Edward MS. Infections of the urinary tract. Wein AJ, Kavoussi LR, Novick AC, Partin AW, Peters CA, editors. Campbell-Walsh urology. 10th ed.Philadelphia: Saunders;2012. p. 268–9.
7. Di Paola G, Mogorovich A, Fiorini G, Cuttano MG, Manassero F, Selli C. Candida bezoars with urinary tract obstruction in two women without immunocompromising conditions. Scientific-WorldJournal. 2011; 11:1168–72.
Fig. 1.
Antegrade ureterography: a filling defect of the right upper ureter, and hydronephroureterosis, due to radiolucent material.
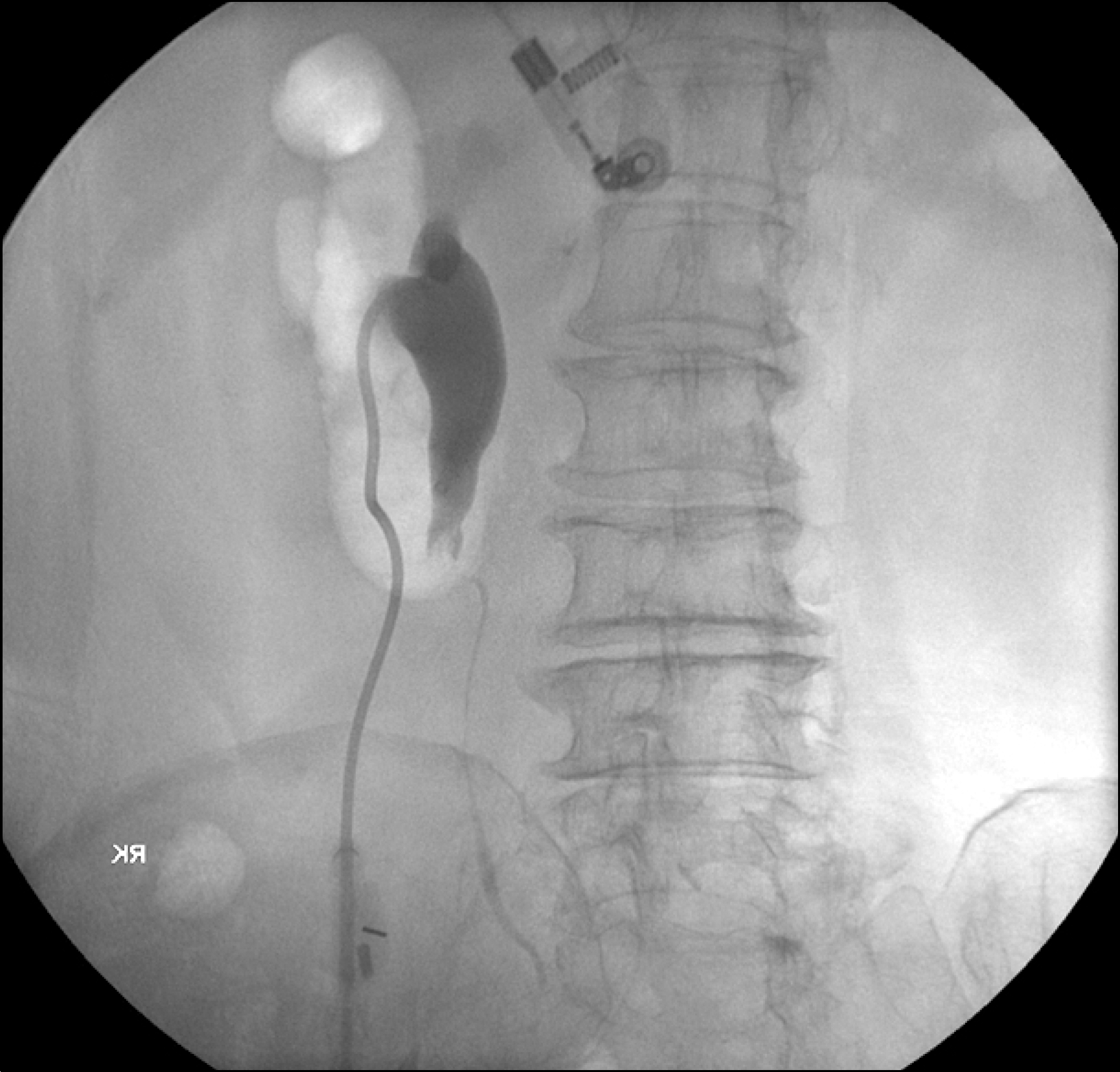
Fig. 2.
Computed tomography of abdomen. (A) Hydronephroureterosis on right-side (arrow). (B) Abrupt luminal narrowing, without findings of urinary stone, extrinsic compression, or enhancing mass (arrow).





 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download