Abstract
For allergists, itch is the most important symptom of atopic dermatitis (AD), and at the same time, the most difficult-to-manage complaint of atopic patient. Rather than just one symptom of AD, itch has more profound clinical significance in the following sense: itch, as a key component of so-called 'itch-scratch' vicious-cycle, plays a central role in the development and persistence of AD, thus, treating itch is not just alleviating one symptom of AD, but stopping genesis and progress of AD. In other words, itch is AD in itself. Pathomechanism underlying development of itch in AD could be summarized as follows: First, exogenous triggering factors penetrate impaired barrier, leading to allergic skin inflammation. Resulting characteristic itch of AD is amplified through the 'itch → scratch → inflammation → (again) → itch →...' vicious-cycle. Thus, pathomechanism-based management strategy could be provided accordingly-avoidance of triggering factor, repair of impaired barrier, control of skin inflammation, and decreasing desire for itch/scratch. Among them, controlling inflammation is thought to be most effective measure based on the clinical experiences, for skin inflammation, as one of key components in 'itch-scratch-inflammation' vicious-cycle, at the same time, is a crucial connecting link between OUTSIDE and INSIDE. However, individualized approach should be taken for patient per se. Finally, following topics may be future topics for doctors always hungry for new weapon against AD and patients suffering from this out-of-place (a-top-y) disease: central itch pathway-emerging new hero; neural sensitization - still in the Dark-Ages in terms of diagnosis and management; and scratch-just in its infancy.
Figures and Tables
Fig. 1
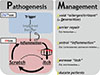
Pathogenesis-based management of itch in atopic dermatitis (AD). On the left panel, simplified version on the pathogenesis of itch in AD is presented. On the right panel, ABCDE management strategy for atopic itch is summarized. For each key pathogenetic factor in left panel, corresponding management strategy appears side-by-side in right panel: Avoid allergen/irritant for trigger; Barrier repair for impaired skin barrier; Control inflammation for flaring allergic skin inflammation; Decrease itch for intractable itchy desire leading to scratch; Educate patients for improved understanding and cooperation on the patients' side (see text for details).
References
1. Elias PM, Hatano Y, Williams ML. Basis for the barrier abnormality in atopic dermatitis: outside-inside-outside pathogenic mechanisms. J Allergy Clin Immunol. 2008; 121:1337–1343.

2. Howell MD, Kim BE, Gao P, Grant AV, Boguniewicz M, Debenedetto A, et al. Cytokine modulation of atopic dermatitis filaggrin skin expression. J Allergy Clin Immunol. 2007; 120:150–155.

3. Siegel DH, Howard R. Molecular advances in genetic skin diseases. Curr Opin Pediatr. 2002; 14:419–425.

4. Akiyama T, Iodi Carstens M, Carstens E. Transmitters and pathways mediating inhibition of spinal itch-signaling neurons by scratching and other counterstimuli. PLoS One. 2011; 6:e22665.

5. Ikoma A, Steinhoff M, Stander S, Yosipovitch G, Schmelz M. The neurobiology of itch. Nat Rev Neurosci. 2006; 7:535–547.

6. Charlesworth EN. Practical approaches to the treatment of atopic dermatitis. Allergy Proc. 1994; 15:269–274.

7. Kim MB. Moisturizer and skin barrier. J Skin Barrier Res. 2009; 11:64–80.
8. Proksch E. The role of emollients in the management of diseases with chronic dry skin. Skin Pharmacol Physiol. 2008; 21:75–80.

10. Buddenkotte J, Steinhoff M. Pathophysiology and therapy of pruritus in allergic and atopic diseases. Allergy. 2010; 65:805–821.

11. Sun YG, Chen ZF. A gastrin-releasing peptide receptor mediates the itch sensation in the spinal cord. Nature. 2007; 448:700–703.

12. Hosogi M, Schmelz M, Miyachi Y, Ikoma A. Bradykinin is a potent pruritogen in atopic dermatitis: a switch from pain to itch. Pain. 2006; 126:16–23.





 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download