Abstract
Drug reaction with eosinophilia and systemic symptoms (DRESS) syndrome is a life-threatening adverse drug reaction with systemic manifestations. Dapsone is known to be useful for treatment of leprosy and various dermatologic conditions. We report a patient with prurigo pigmentosa who developed DRESS syndrome after dapsone treatment. She presented with lymphadenopathy, fever, eosinophilia, skin rash, and elevated liver enzymes. Initial lymph node and skin biopsy was suggestive of peripheral T-cell lymphoma. Initially, she was treated with chemotherapy. A week later after complete remission of skin symptoms, new skin lesions recurred. TCR-gene rearrangement was examined to show negative results and she was diagnosed as dapsone induced DRESS syndrome. This case emphasizes the importance of differential diagnosis of lymphoma and DRESS syndrome.
Figures and Tables
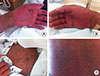
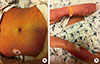 | Fig. 1Diffuse exfoliative erythroderma and maculopapular rash on patient's abdomen (A) and both arms (B). |
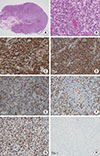 | Fig. 2Histopathologic findings of neck lymph node biopsy (right level 1b). Lymph node biopsy showed a high proliferative activity, immunohistochemistry results suggestive of peripheral T-cell lymphoma. Diffuse polymorphic lymphoid hyperplasia with effacement of the normal lymphoid follicle architecture: (A) H&E, ×40; (B) H&E, ×400; (C) CD3, positive; (D) CD4, positive; (E) CD7, negative; (F) CD8, negative; (G) Ki-67, labeling index 70%; (H) TIA-1, negative. |
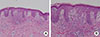
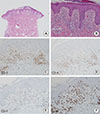 | Fig. 3Biopsy of back skin with recurred skin eruption at second admission. Histological examination of the skin showed lymphocytic infiltration in the epidermis, and perivascular lymphocytic infiltration in the dermis. Epidermotropism is not identified (A, B: H&E, ×400). Similar immunohistochemistry findings with lymph node was observed (C: CD3, positive; D: CD4, positive; E: CD7, negative; F: Ki-67, 80%). |
References
1. Cacoub P, Musette P, Descamps V, Meyer O, Speirs C, Finzi L, et al. The DRESS syndrome: a literature review. Am J Med. 2011; 124:588–597.

2. Chen YC, Chiu HC, Chu CY. Drug reaction with eosinophilia and systemic symptoms: a retrospective study of 60 cases. Arch Dermatol. 2010; 146:1373–1379.

3. Kardaun SH, Sidoroff A, Valeyrie-Allanore L, Halevy S, Davidovici BB, Mockenhaupt M, et al. Variability in the clinical pattern of cutaneous side-effects of drugs with systemic symptoms: does a DRESS syndrome really exist? Br J Dermatol. 2007; 156:609–611.

4. Zhu YI, Stiller MJ. Dapsone and sulfones in dermatology: overview and update. J Am Acad Dermatol. 2001; 45:420–434.

5. Kosseifi SG, Guha B, Nassour DN, Chi DS, Krishnaswamy G. The Dapsone hypersensitivity syndrome revisited: a potentially fatal multisystem disorder with prominent hepatopulmonary manifestations. J Occup Med Toxicol. 2006; 1:9.

6. Chalasani P, Baffoe-Bonnie H, Jurado RL. Dapsone therapy causing sulfone syndrome and lethal hepatic failure in an HIV-infected patient. South Med J. 1994; 87:1145–1146.

7. Mockenhaupt M. Severe drug-induced skin reactions: clinical pattern, diagnostics and therapy. J Dtsch Dermatol Ges. 2009; 7:142–160.

8. Chiou CC, Yang LC, Hung SI, Chang YC, Kuo TT, Ho HC, et al. Clinicopathological features and prognosis of drug rash with eosinophilia and systemic symptoms: a study of 30 cases in Taiwan. J Eur Acad Dermatol Venereol. 2008; 22:1044–1049.

9. Kardaun SH, Sekula P, Valeyrie-Allanore L, Liss Y, Chu CY, Creamer D, et al. Drug reaction with eosinophilia and systemic symptoms (DRESS): an original multisystem adverse drug reaction. Results from the prospective RegiSCAR study. Br J Dermatol. 2013; 169:1071–1080.

10. Lorenz M, Wozel G, Schmitt J. Hypersensitivity reactions to dapsone: a systematic review. Acta Derm Venereol. 2012; 92:194–199.

11. Jeung YJ, Lee JY, Oh MJ, Choi DC, Lee BJ. Comparison of the causes and clinical features of drug rash with eosinophilia and systemic symptoms and stevens-johnson syndrome. Allergy Asthma Immunol Res. 2010; 2:123–126.

12. Choi HW, Song IK, Chung EA, Cha DY, Lim MK, Na DJ, et al. A case of Sulfone syndrome hypersensitivity associated with dapsone. J Asthma Allergy Clin Immunol. 2001; 21:1206–1210.
13. Agrawal S, Agarwalla A. Dapsone hypersensitivity syndrome: a clinico-epidemiological review. J Dermatol. 2005; 32:883–889.

14. Schnetzke U, Bossert T, Scholl S, Freesmeyer M, Hochhaus A, La Rosee P. Drug-induced lymphadenopathy with eosinophilia and renal failure mimicking lymphoma disease: dramatic onset of DRESS syndrome associated with antibiotic treatment. Ann Hematol. 2011; 90:1353–1355.

15. Rim MY, Hong J, Yo I, Park H, Chung DH, Ahn JY, et al. Cervical lymphadenopathy mimicking angioimmunoblastic T-cell lymphoma after Dapsone-induced hypersensitivity syndrome. Korean J Pathol. 2012; 46:606–610.

16. Husain Z, Reddy BY, Schwartz RA. DRESS syndrome: Part I. clinical perspectives. J Am Acad Dermatol. 2013; 68:693.e1–693.e14.
17. Sylvia LM. Adverse cutaneous drug eruptions. Ann Pharmacother. 2012; [Epub ahead of print].




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download