Introduction
Kawasaki disease (KD) is the multisystem vasculitis which is a cause of secondary heart disease in children [1]. Coronary artery aneurysm could be a cause of death in some cases of KD, so it is important to diagnose coronary artery complication [2].
KD could be diagnosed by having the following criteria: prolonged fever longer than 5 days and four of the five following main clinical features: (1) changes in the peripheral extremities, (2) polymorphous rash, (3) oropharyngeal changes, (4) acute nonpurulent conjunctivitis, and (5) cervical lymphadenopathy accompanied with lymph node greater than 1.5 cm [13].
Bulbar conjunctival injection and anterior uveitis are dominant ocular manifestation in KD [4]. Posterior segment involvement is rare. Despite early efficient treatment including aspirin and intravenous immunoglobulins (IVIG), the bilateral inflammatory ocular involvement including punctuated keratitis, retrodescemetic precipitates, anterior uveitis, vitritis, and bilateral optic disc swelling with papillitis are observed in KD patients [56789].
Uveitis is the common ophthalmic finding in KD. Manifestation of uveitis is mild. It is bilateral and is sometimes associated with keratic precipitates. In general, it occurs a week after fever onset and recovers within 2–8 weeks after disease onset without any sequelae. According to increasing incomplete KD, uveitis has become a more important factor in early diagnosis of incomplete KD [5].
Inflammation of both anterior and posterior segments does not seem to respond to KD-specific treatment and could justify a specific ophthalmologic therapeutic approach [4].
Grouteau et al. [4] reported severe bilateral global inflammatory involvement of the eyes in KD. It is usually subclinical and self-limited. Eye involvement in KD can lead to severe visual impairment. Kadyan et al. [10] published a case of disciform keratitis and optic disc swelling in KD. Ohno et al. [11] reported bilateral bulbar conjunctivitis, bilateral iridocyclitis, superficial punctate keratitis, vitreous opacities, papilledema and subconjunctival hemorrhage. There has not been a report of optic disc swelling associated with uveitis in the KD patient in Korea.
Case
A previously healthy 3-year-old boy was admitted to our hospital because of fever for 7 days up to 39.0℃, conjunctival injection and right cervical lymph node enlargement 1 day prior to admission. At the time of admission, his vital signs were as follows: body temperature, 38.0℃; pulse rate, 100 beats/min; and respiration rate, 26 breaths/min. Physical examination revealed both conjunctival injection without discharge, strawberry tongue and right cervical lymph node enlargement more than 1.5 cm. He did not have red lip, erythema and swellling of hand and foot. However, there was no tympanic membrane injection or pharyngeal injection. Breathing sounds were clear without rale and wheezing. Initial laboratory results were as follows: erythrocyte sedimentation rate (ESR) 66 mm/hr, white blood cell (WBC) count 9,290/µL, hemoglobin 11.0 g/dL, hematocrit 31.9%, platelet count 323,000/µL, C-reactive protein (CRP) 2.65 mg/dL, N-terminal pro-brain natriuretic peptide (NT pro-BNP) 125 pg/mL. A chest radiograph showed no active lung lesion. Despite antibiotics (ceftriaxone and clindamycin) for treating the cervical lymphadenitis, the fever persisted.
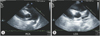
On hospital day 4, laboratory results were as follows: ESR 58 mm/hr, WBC 8,980/µL, CRP 5.31 mg/dL, NT pro-BNP 200 pg/mL. An echocardiogram revealed dilatation of right coronary artery (3.4 mm) (Fig. 1). Left ventricular (LV) function was good (ejection fraction 62.4%, fractional shortening 33.1%). Other echocardiogram findings were no pericardial effusion, no mitral valve regurgitation, and no tricuspid valve regurgitation. Tissue Doppler imaging measures were as follows: early diastolic myocardial velocity (E') 8.36 cm/sec, late diastolic myocardial velocity (A') 3.93 cm/sec, and systolic myocardial velocity (S') 5.26 cm/sec. Isovolumetric contraction time 71 ms, Isovolumetric relaxation time 58 ms, LV ejection time 272 ms. The Tei index was 0.47.
Due to these findings, a diagnosis of incomplete KD was established. Therefore, IVIG 2 g/kg/day (Green Cross Corp., Seoul, Korea) was administered and high dose aspirin (30 mg/kg/day divided three; Bayer AG, Bayer Korea Ltd., Seoul, Korea) was started.
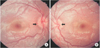
On hospital day 5, the fever and cervical lymphadenopathy subsided and both conjunctival injection was slightly improved. For evaluation of ocular manifestation of KD, ophthalmic consultation was done. The consultation result was uveitis and optic disc swelling on both eyes. He had cells in both anterior chambers which means uveitis. There was no vitreous opacities. Another finding was both blunted optic disc margin (Fig. 2). He also had optic disc swelling and he was treated with intravenous mannitol (JW Life Science, JW Pharmaceutical, Seoul, Korea).
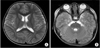
On hospital day 6, the finding of brain magnetic resonance imaging (MRI) was normal (Fig. 3). We consulted a neurologist about the optic disc swelling. The patient did not have any increased intracranial pressure (ICP) sign and no brain edema on MRI. Mannitol was tapered and stopped. We started low dose aspirin therapy (5 mg/kg/day). At this time, we observed the desquamation on his finger.
On hospital day 8, the laboratory results have improved: CRP 0.49 mg/dL, and NT pro-BNP 58 pg/mL. The patient was discharged.
Discussion
Although bilateral nonpurulent conjunctivitis is a diagnostic criteria in KD, other ocular features are found such as superficial punctuate keratitis, vitreous opacities, anterior uveitis, optic disc swelling, vascular occlusions, retinal ischemia, and periorbital vasculitis [8].
Uveitis in KD shows a mild clinical course. In most cases, topical corticosteroid is effective for treatment of KD patients. KD patients with anterior uveitis are needed to follow up evaluation depending on its severity between 1–7 days [5]. Ophthalmic evaluation includes visual acuity, measurement of intraocular pressure, assessment of cell and flare by slit lamp examination [12].
The grading of uveitis is decided according to flare and cell number, so slit lamp examination is necessary to diagnose uveitis. The uveitis improves within 2–8 weeks after disease onset without any sequelae [13]. In our patient, uveitis resolved within 2 week after IVIG and topical steroid treatment.
The causes of pediatric secondary intracranial hypertension include viral infection, hypoparathyroidism, menarche, corticosteroid withdrawal, thyroid treatment, nalidixic acid, tetracycline, vitamin A and D deficiencies, vitamin A toxicity, head trauma, systemic lupus erythematosus, acute lymphocytic leukemia, galactosemia, galactokinase deficiency, Turner syndrome, and nitrofurantoin [14].
Headache is an important symptom of ICP. Nausea and vomiting are frequent. Worrisome features include a positional quality to the headache, usually worsening with recumbency, as well as a diurnal pattern. Headaches associated with intracranial hypertension are classically worse in the early morning. Another classic symptom of ICP is binocular horizontal diplopia resulting from unilateral or bilateral lateral rectus paresis [14].
In our case, the patient did not complain of the headache during hospitalization period. Any symptom of ICP was not found. We did not perform a spinal tap, because the patient did not have headache. Etiology of optic disc swelling was not identified in our case. Optic disc swelling was regarded as infiltration of inflammatory cells.
The stimulus for the cascade of inflammation in KD is unknown. Initially, an intense inflammatory response is elicited by monocytes, macrophages and T cells infiltrating the vascular wall. Inflammation can progress to involve the deeper layers of the vascular wall, compromising structural integrity with resultant dilation or aneurysm formation [15]. In our case, optic disc swelling was completely improved after IVIG treatment without any sequelae.
Choi et al. [5] reported that neutrophil counts and patient age were higher in the uveitis group than in the control group. ESR and CRP level were slightly increased in the uveitis group compared with the control group, but the difference between the two groups was not significant.
There is not any definite guideline to diagnose incomplete KD yet. Early diagnosis is needed to prevent coronary artery complications. Slit lamp examination and echocardiography are very useful for differential diagnosis of incomplete KD. The serum NT pro-BNP levels have been reported as an early diagnostic marker of myocardial involvement in KD [2]. In our case, NT pro-BNP was not increased.
Uveitis is not the only clue to diagnosing KD, but if a patient has conjunctivitis, ophthalmic examination is very helpful in detecting uveitis and optic disc swelling [5]. There is also no specific guideline to determine the timing of slit lamp examination in KD. Meticulous ophthalmoscopic examination is needed to find out uveitis and optic disc swelling in every KD patients.
In conclusion, we reported the first case of optic disc swelling associated with uveitis in KD patient in Korea. Slit lamp and ophthalmoscopic examination are necessary to reveal these findings.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download