Abstract
Vertebral artery dissection (VAD) is one of important causes of posterior circulation strokes in young age patients. Typical presentations of VAD are occipital headache or posterior neck pain, with various signs arising from brainstem or cerebellar infarctions. Muscular weakness or sensory change of an ipsilateral arm owing to cervical nerve root involvement in association with the VAD has been reported very rarely. Herein we describe two unusual manifestations of extracranial VAD, which presented with monoplegia of single upper limb.
Figures and Tables
Fig. 1
(A) T1 weighted and (B) T2 weighted C-spine magnetic resonance imaging (MRI) of patient 1. Cervical MRI study shows high and isosignal intensity of the wall thickening in left vertebral artery (arrow) and combined luminal narrowing. Definite spinal cord lesion is not observed.
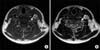
Fig. 2
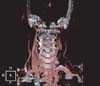
Three-dimensional computed tomography angiography of patient 1. Compared with a diameter of the right vertebral artery, left vertebral artery at the levels from the C6 to the C2 (arrow) is diffusely narrowed.
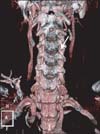
Fig. 3
Cerebral angiography of patient 1. Cerebral 4-vessel angiography shows diffuse narrowing of left vertebral artery (A. arrow) compared with the diameter of right vertebral artery (B). These results are suggestive of left vertebral artery dissection.
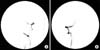
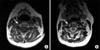
Fig. 4
(A) T1 weighted and (B) T2 weighted cervical spine MRI images of patient 2. In T1 weighted image, signal voiding of right vertebral artery (arrow) is narrower than that of left vertebral artery. Thickening with high signal intensity (arrow) is also noted on T2 weighted image.
References
1. Ropper AH, Brown RH. Adams and Victor's principles of neurology. 8th ed. New York: McGraw Hill;2005.
2. Pullicino P. Bilateral distal upper limb amyotrophy and watershed infarcts from vertebral dissection. Stroke. 1994; 25:1870–1872.
3. Aggarwal A, Burton K. Cervical root injury caused by vertebral artery dissection. J Clin Neurosci. 1999; 6:166–168.
4. Dubard T, Pouchot J, Lamy C, Hier D, Caplan LR, Mas JL. Upper limb peripheral motor deficits due to extracranial vertebral artery dissection. Cerebrovasc Dis. 1994; 4:88–91.
5. Hetzel A, Berger W, Schumacher M, Lucking , Dissection of. Lucking, Dissection of the vertebral artery with cervical nerve root lesions. J Neurol. 1996; 243:121–125.
6. Kang HG, Lee HS, Kim SS, Jeong J, Jo JH, Yi MJ, et al. Brachial plexopathy caused by vertebral artery dissection. J Korean Neurol Assoc. 2011; 29:64–66.
7. McGillion SF, Weston-Simons S, Harvey JR. Vertebral artery dissection presenting with multilevel combined sensorimotor radiculopathy: a case report and literature review. J Spinal Disord Tech. 2009; 22:456–458.
8. Tabatabai G, Schober W, Ernemann U, Weller M, Kruger R. Vertebral artery dissection presenting with ispilateral acute C5 and C6 sensorimotor radiculopathy: a case report. Cases J. 2008; 1:139.
9. Park KW, Park JS, Hwang SC, Im SB, Shin WH, Kim BT. Vertebral artery dissection: natural history, clinical features and therapeutic considerations. J Korean Neurosurg Soc. 2008; 44:109–115.
10. Kwon OH, Yoon BW, Kim BG, Roh JK, Lee HB, Park SH. Dissection of the vertebrobasilar artery. J Korean Neurol Assoc. 1997; 15:493–504.
11. Schievink WI. Spontaneous dissection of the carotid and vertebral arteries. N Engl J Med. 2001; 344:898–906.
12. Benny BV, Nagpal AS, Singh P, Smuck M. Vascular causes of radiculopathy: a literature review. Spine J. 2011; 11:73–85.
13. Rolfe B. Surgical disorders of the peripheral nerves. 2nd ed. London: Churchill Livingstone;2011.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download