Abstract
Objectives
Patients with schizophrenia often present idea of reference in social situations, but there has been a limitation in quantitatively measuring their reactions to the social stimuli. The aim of this study was to investigate behavioral characteristics of patients with schizophrenia in social situations in which idea of reference can be provoked.
Methods
Forty subjects with schizophrenia (21 males) and 26 healthy volunteers (17 males) performed the idea-of-reference-provoking task, which was composed of movie clips with scenes of two women sitting on a bench of 1 or 5 m away. The conditions consisted of “referential conversation”, “non-referential conversation” or “no conversation”. The reactions of the participants were rated by the questionnaires for self-referential perception, malevolent interpretation and anxiety reaction.
Results
There were significant group differences in the reactions on self-referential perception, malevolent interpretation and anxiety reaction. After the treatment, patients with schizophrenia showed improved scores of the reactions. In particular, score changes of malevolent interpretation and anxiety reaction in patients with schizophrenia were correlated with change of paranoia scale (rs=0.65, p<0.05 and rs =0.73, p<0.05, respectively).
REFERENCES
1). Freeman D. Suspicious minds: the psychology of persecutory delusions. Clinical Psychology Review. 2007; 27:425–457.

2). Yung AR, Yuen HP, McGorry PD, Phillips LJ, Kelly D, Dell'Olio M, et al. Mapping the onset of psychosis: the Comprehensive Assessment of At-Risk Mental States. The Australian and New Zealand Journal of Psychiatry. 2005; 39:964–971.

3). Birchwood M, Smith J, Macmillan F, Hogg B, Prasad R, Harvey C, et al. Predicting relapse in schizophrenia: the development and implementation of an early signs monitoring system using patients and families as observers, a preliminary investigation. Psychological Medicine. 1989; 19:649–656.

4). Carpenter WT Jr, Strauss JS, Bartko JJ. Flexible system for the diagnosis of schizophrenia: report from the WHO International Pilot Study of Schizophrenia. Science. 1973; 182:1275–1278.

5). Ceskova E, Prikryl R, Kasparek T, Ondrusova M. Psychopathology and treatment responsiveness of patients with firstepisode schizophrenia. Neuropsychiatric Disease and Treatment. 2005; 1:179–185.
6). Jager M, Riedel M, Messer T, Laux G, Pfeiffer H, Naber D, et al. Psychopathological characteristics and treatment response of first episode compared with multiple episode schizophrenic disorders. Eur Arch Psy Clin N. 2007; 257:47–53.
7). Couture SM, Penn DL, Roberts DL. The functional significance of social cognition in schizophrenia: a review. Schizophrenia Bulletin. 2006; 32(Suppl 1):S44-S63.

8). Brune M, Abdel-Hamid M, Lehmkamper C, Sonntag C. Mental state attribution, neurocognitive functioning, and psychopathology: what predicts poor social competence in schizophrenia best? Schizophrenia Research. 2007; 92:151–159.

9). Addington J, Saeedi H, Addington D. Influence of social perception and social knowledge on cognitive and social functioning in early psychosis. The British Journal of Psychiatry: the Journal of Mental Science. 2006; 189:373–378.

10). Edwards J, Jackson HJ, Pattison PE. Emotion recognition via facial expression and affective prosody in schizophrenia: a methodological review. Clinical Psychology Review. 2002; 22:789–832.
11). Bora E, Eryavuz A, Kayahan B, Sungu G, Veznedaroglu B. Social functioning, theory of mind and neurocognition in outpatients with schizophrenia; mental state decoding may be a better predictor of social functioning than mental state reasoning. Psychiatry Research. 2006; 145:95–103.

12). Kucharska-Pietura K, David AS, Masiak M, Phillips ML. Perception of facial and vocal affect by people with schizophrenia in early and late stages of illness. The British Journal of Psychiatry: the Journal of Mental Science. 2005; 187:523–528.

13). Hooker C, Park S. You must be looking at me: the nature of gaze perception in schizophrenia patients. Cognitive Neuropsychiatry. 2005; 10:327–345.

14). Harrington L, Siegert RJ, McClure J. Theory of mind in schizophre nia: a critical review. Cognitive Neuropsychiatry. 2005; 10:249–286.
15). Greig TC, Bryson GJ, Bell MD. Theory of mind performance in schizophrenia: diagnostic, symptom, and neuropsychological correlates. The Journal of Nervous and Mental Disease. 2004; 192:12.

16). Kaplan HI, Sadock BJ. Comprehensive textbook of psychiatry. 5th ed.Baltimiore Williams & Wilkins;1989.
17). Park IH, Ku J, Lee H, Kim SY, Kim SI, Yoon KJ, et al. Disrupted theory of mind network processing in response to idea of reference evocation in schizophrenia. Acta Psychiatrica Scandinavica. 2011; 123:43–54.

18). Pinkham AE, Brensinger C, Kohler C, Gur RE, Gur RC. Actively paranoid patients with schizophrenia over attribute anger to neutral faces. Schizophrenia Research. 2011; 125:174–178.

19). Hooker C, Park S. Emotion processing and its relationship to social functioning in schizophrenia patients. Psychiatry Research. 2002; 112:41–50.

20). Hoffman EA, Haxby JV. Distinct representations of eye gaze and identity in the distributed human neural system for face perception. Nature Neuroscience. 2000; 3:80–84.

21). Baron-Cohen S, Ring HA, Wheelwright S, Bullmore ET, Brammer MJ, Simmons A, et al. Social intelligence in the normal and autistic brain: an fMRI study. The European Journal of Neuroscience. 1999; 11:1891–1898.

22). Russell TA, Rubia K, Bullmore ET, Soni W, Suckling J, Brammer MJ, et al. Exploring the social brain in schizophrenia: left prefrontal underactivation during mental state attribution. The American Journal of Psychiatry. 2000; 157:2040–2042.

23). Gallagher HL, Frith CD. Functional imaging of ‘theory of mind'. Trends in Cognitive Sciences. 2003; 7:77–83.

24). Hooker CI, Bruce L, Lincoln SH, Fisher M, Vinogradov S. Theory of mind skills are related to gray matter volume in the ventromedial prefrontal cortex in schizophrenia. Biological Psychiatry. 2011; 70:1169–1178.

25). Honea R, Crow TJ, Passingham D, Mackay CE. Regional deficits in brain volume in schizophrenia: a metaanalysis of voxel-based morphometry studies. The American Journal of Psychiatry. 2005; 162:2233–2245.

26). Brunet E, Sarfati Y, Hardy-Bayle MC, Decety J. Abnormalities of brain function during a nonverbal theory of mind task in schizophrenia. Neuropsychologia. 2003; 41:1574–1582.

27). Wible CG. Schizophrenia as a disorder of social communication. Schizophrenia Research and Treatment. 2012; 2012:920485.

28). Horowitz MJ. Spatial behavior and psychopathology. The Journal of Nervous and Mental Disease. 1968; 146:24–35.

29). Green MJ, Phillips ML. Social threat perception and the evolution of paranoia. Neuroscience and Biobehavioral Reviews. 2004; 28:333–342.

30). Freeman D, Garety PA, Bebbington P, Slater M, Kuipers E, Fowler D, et al. The psychology of persecutory ideation II: a virtual reality experimental study. The Journal of Nervous and Mental Disease. 2005; 193:309–315.
31). Valmaggia LR, Freeman D, Green C, Garety P, Swapp D, Antley A, et al. Virtual reality and paranoid ideations in people with an ‘at-risk mental state' for psychosis. The British Journal of Psychiatry Supplement. 2007; 51:s63–s68.

32). Bora E, Gokcen S, Kayahan B, Veznedaroglu B. Deficits of social-cognitive and social-perceptual aspects of theory of mind in remitted patients with schizophrenia: effect of residual symptoms. The Journal of Nervous and Mental Disease. 2008; 196:95–99.
33). Brune M. “Theory of mind” in schizophrenia: a review of the literature. Schizophrenia Bulletin. 2005; 31:21–42.

Fig. 2.
Correlations between score change in paranoid scale and changes in mean scores of self-referential perception, malevolent interpretation and anxiety reaction.
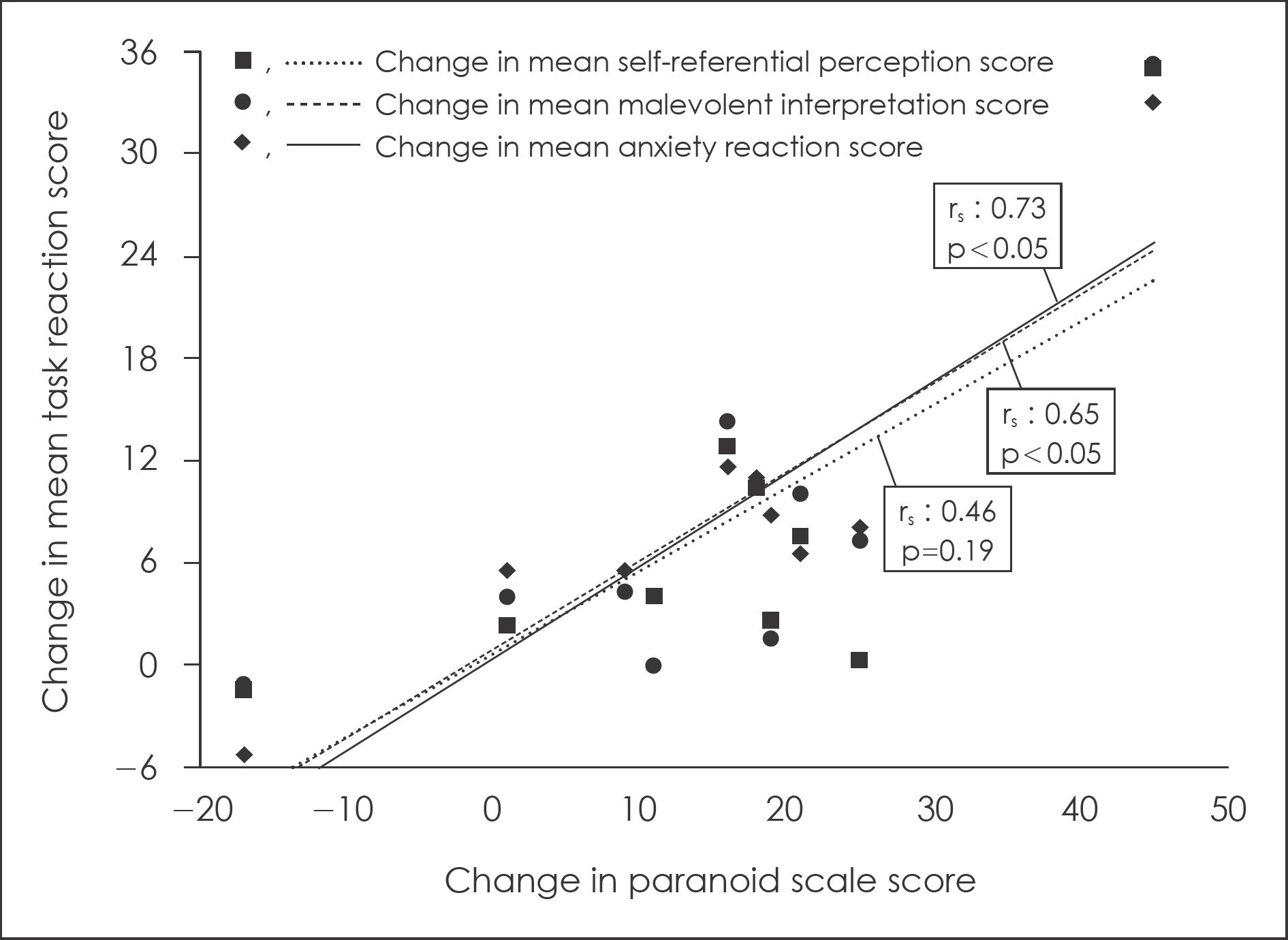
Table 1.
Demographic and clinical characteristics of participants
| Control (n=26) | SPR (n=40) | p-value∗ | |
|---|---|---|---|
| Male/Female | 17 (65.4%)/9 (34.6%) | 21 (52.5%)/19 (47.5%) | <0.301 |
| Age | 028.3±04.3 | 29.6±07.1 | <0.351 |
| Education | 014.9±01.8 | 12.9±02.1 | <0.010 |
| K-WAIS | 108.2±09.8 | 97.3±09.2 | <0.010 |
| Paranoid scale score | 039.2±10.1 | 53.1±19.5 | <0.010 |
| PANSS | |||
| Total score | 62.8±18.0 | ||
| Positive score | 13.6±09.1 | ||
| Negative score | 14.7±05.0 | ||
| General score | 34.4±09.5 | ||
| Duration of illness (years) | 05.9±04.8 |
Table 2.
Task scores for self-referential perception, malevolent interpretation and anxiety reaction
| Control (n=26) | SPR (n=40) | p-value∗ | |
|---|---|---|---|
| 1 m, Referential context | |||
| Perception | 3.37±1.96 | 2.69±1.90 | <0.17 |
| Interpretation | 0.51±0.74 | 1.76±1.69 | <0.01 |
| Anxiety | 0.93±1.09 | 1.95±1.77 | <0.01 |
| 1 m, non-Referential context | |||
| Perception | 0.19±0.52 | 1.24±1.57 | <0.01 |
| Interpretation | 0.18±0.50 | 1.17±1.44 | <0.01 |
| Anxiety | 0.21±0.55 | 1.42±1.70 | <0.01 |
| 1 m, no-Conversation context | |||
| Perception | 0.15±0.47 | 1.37±1.55 | <0.01 |
| Interpretation | 0.19±0.51 | 1.43±1.60 | <0.01 |
| Anxiety | 0.21±0.51 | 1.71±1.71 | <0.01 |
| 5 m, Referential context | |||
| Perception | 2.81±1.66 | 2.48±1.81 | <0.45 |
| Interpretation | 0.65±0.67 | 1.86±1.95 | <0.01 |
| Anxiety | 1.10±0.95 | 2.04±1.88 | <0.01 |
| 5 m, non-Referential context | |||
| Perception | 0.35±0.54 | 1.51±1.76 | <0.01 |
| Interpretation | 0.33±0.56 | 1.54±1.79 | <0.01 |
| Anxiety | 0.38±0.79 | 1.71±1.85 | <0.01 |
| 5 m, no-Conversation context | |||
| Perception | 0.25±0.52 | 1.48±1.53 | <0.01 |
| Interpretation | 0.23±0.50 | 1.34±1.54 | <0.01 |
| Anxiety | 0.24±0.53 | 1.51±1.69 | <0.01 |
Table 3.
Distance effect on self- referential perception, malevolent interpretation and anxiety reaction
| Control group (n=26) | p-value∗ | ||
|---|---|---|---|
| 1 m | 5 m | ||
| Referential context | |||
| Perception | 3.37±1.96 | 2.81±1.66 | <0.05 |
| Interpretation | 0.51±0.74 | 0.65±0.67 | 0.15 |
| Anxiety | 0.93±1.09 | 1.10±0.95 | 0.31 |
| Non-Referential context | |||
| Perception | 0.19±0.52 | 0.35±0.54 | 0.05 |
| Interpretation | 0.18±0.50 | 0.33±0.56 | 0.12 |
| Anxiety | 0.21±0.55 | 0.38±0.79 | 0.13 |
| No-Conversation context | |||
| Perception | 0.15±0.47 | 0.25±0.52 | 0.08 |
| Interpretation | 0.19±0.51 | 0.23±0.50 | 0.40 |
| Anxiety | 0.21±0.51 | 0.24±0.53 | 0.50 |
| Schizophrenia group (n=40) | p-value∗ | ||
| 1 m | 5 m | ||
| Referential context | |||
| Perception | 2.69±1.90 | 2.48±1.81 | 0.33 |
| Interpretation | 1.76±1.69 | 1.86±1.95 | 0.56 |
| Anxiety | 1.95±1.77 | 2.04±1.88 | 0.69 |
| Non-Referential context | |||
| Perception | 1.24±1.57 | 1.51±1.76 | 0.06 |
| Interpretation | 1.17±1.44 | 1.54±1.79 | <0.05 |
| Anxiety | 1.42±1.70 | 1.71±1.85 | 0.07 |
| No-Conversation context | |||
| Perception | 1.37±1.55 | 1.48±1.53 | 0.40 |
| Interpretation | 1.43±1.60 | 1.34±1.54 | 0.42 |
| Anxiety | 1.71±1.71 | 1.51±1.69 | 0.06 |
Table 4.
Context effect on self-referential perception, malevolent interpretation and anxiety reaction
| Referential (R) | Non-referential (NR) | No conversation (NC) | p-value∗ | ||
|---|---|---|---|---|---|
| Control | |||||
| Perception | 3.37±1.96 | 0.19±0.52 | 0.15±0.47 | R >NR†, R >NC† | |
| Interpretation | 0.51±0.74 | 0.18±0.50 | 0.19±0.51 | R >NR†, R >NC† | |
| 1 m | Anxiety | 0.93±1.09 | 0.21±0.55 | 0.21±0.51 | R >NR† R >NC†, NR >NC† |
| Schizophrenia | |||||
| Perception | 2.69±1.90 | 1.24±1.57 | 1.37±1.55 | R >NR†, R >NC† | |
| Interpretation | 1.76±1.69 | 1.17±1.44 | 1.43±1.60 | R >NR† | |
| Anxiety | 1.95±1.77 | 1.42±1.70 | 1.71±1.71 | ||
| Control | |||||
| Perception | 2.81±1.66 | 0.35±0.54 | 0.25±0.52 | R >NR†, R >NC† | |
| Interpretation | 0.65±0.67 | 0.33±0.56 | 0.23±0.50 | R >NR‡, R >NC† | |
| 5 m | Anxiety | 1.10±0.95 | 0.38±0.79 | 0.24±0.53 | R >NR†, R >NC† |
| Schizophrenia | |||||
| Perception | 2.48±1.81 | 1.51±1.76 | 1.48±1.53 | R >NR†, R >NC† | |
| Interpretation | 1.86±1.95 | 1.54±1.79 | 1.34±1.54 | R >NC‡ | |
| Anxiety | 2.04±1.88 | 1.71±1.85 | 1.51±1.69 |
Table 5.
Comparison of scores for self-referential perception, malevolent interpretation and anxiety reaction between pre-treatment and posttreatment in followup patients
| Follow-up schizophrenia group (n=10) | p-value∗ | ||
|---|---|---|---|
| Pre-treatment | Post-treatment | ||
| Paranoia scale | 52.00 (31.00-98.00) | 38.00 (28.00-53.00) | <0.05 |
| 1 m, Referential context | |||
| Perception | 02.38 (0.00-6.00) | 00.75 (0.00-5.25) | <0.29 |
| Interpretation | 01.25 (0.00-6.00) | 00.00 (0.00-1.50) | <0.05 |
| Anxiety | 01.63 (0.00-6.00) | 00.00 (0.00-1.50) | <0.05 |
| 1 m, non-Referential context | |||
| Perception | 00.88 (0.00-5.75) | 00.00 (0.00-1.25) | <0.05 |
| Interpretation | 00.38 (0.00-5.75) | 00.00 (0.00-1.50) | <0.07 |
| Anxiety | 00.38 (0.00-6.00) | 00.00 (0.00-2.50) | <0.08 |
| 1 m, no-Conversation context | |||
| Perception | 01.38 (0.00-6.00) | 00.00 (0.00-2.25) | <0.16 |
| Interpretation | 01.38 (0.00-5.75) | 00.00 (0.00-2.50) | <0.05 |
| Anxiety | 01.00 (0.00-6.00) | 00.00 (0.00-1.50) | <0.07 |
| 5 m, Referential context | |||
| Perception | 03.75 (0.50-6.00) | 01.50 (0.00-5.50) | <0.11 |
| Interpretation | 01.75 (0.00-6.00) | 00.00 (0.00-1.00) | <0.05 |
| Anxiety | 01.75 (0.00-4.50) | 00.00 (0.00-3.50) | <0.07 |
| 5 m, non-Referential context | |||
| Perception | 01.25 (0.00-5.50) | 00.00 (0.00-0.50) | <0.05 |
| Interpretation | 01.25 (0.00-6.00) | 00.00 (0.00-1.50) | <0.05 |
| Anxiety | 01.25 (0.00-6.00) | 00.00 (0.00-2.00) | <0.05 |
| 5 m, no-Conversation context | |||
| Perception | 01.63 (0.00-5.75) | 00.00 (0.00-1.50) | <0.05 |
| Interpretation | 01.63 (0.00-5.75) | 00.00 (0.00-1.25) | <0.05 |
| Anxiety | 01.75 (0.00-6.00) | 00.00 (0.00-2.00) | <0.05 |
Table 6.
Comparison of self-referential perception, malevolent interpretation and anxiety reaction between the control and posttreatment schizophrenia groups
| Control (n=26) | Post-treatment schizophrenia (n=10) | p-value∗ | |
|---|---|---|---|
| 1 m, referential context | |||
| Perception | 3.13 (0.00-6.00) | 0.75 (0.00-5.25) | 0.17 |
| Interpretation | 0.00 (0.00-2.25) | 0.00 (0.00-1.50) | 0.48 |
| Anxiety | 0.63 (0.00-3.50) | 0.00 (0.00-1.50) | 0.27 |
| 1 m, non-Referential context | |||
| Perception | 0.00 (0.00-2.00) | 0.00 (0.00-1.25) | 0.66 |
| Interpretation | 0.00 (0.00-2.00) | 0.00 (0.00-1.50) | 0.57 |
| Anxiety | 0.00 (0.00-2.00) | 0.00 (0.00-2.50) | 0.54 |
| 1 m, no-Conversation context | |||
| Perception | 0.00 (0.00-2.00) | 0.00 (0.00-2.25) | 0.21 |
| Interpretation | 0.00 (0.00-2.00) | 0.00 (0.00-2.50) | 0.54 |
| Anxiety | 0.00 (0.00-2.00) | 0.00 (0.00-1.50) | 0.39 |
| 5 m, Referential context | |||
| Perception | 3.00 (0.00-6.00) | 1.50 (0.00-5.50) | 0.09 |
| Interpretation | 0.50 (0.00-2.50) | 0.00 (0.00-1.00) | 0.17 |
| Anxiety | 1.00 (0.00-3.50) | 0.00 (0.00-3.50) | 0.09 |
| 5 m, non-Referential context | |||
| Perception | 0.00 (0.00-2.00) | 0.00 (0.00-0.50) | 0.37 |
| Interpretation | 0.00 (0.00-3.00) | 0.00 (0.00-1.50) | 0.69 |
| Anxiety | 0.00 (0.00-2.50) | 0.00 (0.00-2.00) | 0.48 |
| 5 m, no-Conversation context | |||
| Perception | 0.00 (0.00-2.00) | 0.00 (0.00-1.50) | 0.90 |
| Interpretation | 0.00 (0.00-2.00) | 0.00 (0.00-1.25) | 0.90 |
| Anxiety | 0.00 (0.00-2.00) | 0.00 (0.00-2.00) | 0.74 |




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download