Abstract
Objectives
The objectives of this study were to evaluate the effect of smoking on utilization of and expenses in ambulatory dental care.
Methods
The subjects of this study were 5,751 men aged over 20 years selected from the Korea Health Panel data collected during 2010-2012. Pack-years of smoking were calculated based on the survey data. Dental utilization was defined as dental outpatient clinic use least once in three years. The expenses in ambulatory dental care were summed to determine total dental health care spending for three years. To detect the effect of smoking, we used multiple logistic regression analysis for dental utilization and multiple linear regression for expenses in ambulatory dental care after changing log.
Results
The pack-years had a significant effect on dental utilization and expenses in participants aged 40-59 years. After controlling for income level, bedtime brushing, and the presence of chronic disease, dental care utilization rates in the over 10 to less than 25 pack-year and the over 25 pack-year groups were about 1.4 (OR=1.37, (P=0.007)) and 1.6 times (OR=1.59, (P=0.001)) those in the 0 pack-year group. In comparison with the 0 pack-year group, the over 10 to less than 25 pack-year group spent 50,000 won more over dental expenses, while the corresponding number for the over 25 pack-year group was about 100,000 won. Thus, the ambulatory dental care expenses increased with the pack-years of smoking.
References
1. Statistics Korea, News, Press Releases, Social statistics, The Summary Result of the 2014 Social Survey [Internet]. [cited 2015 Nov 05]. Available from:. http://kostat.go.kr/portal/english/news/1/19/5/index.board.
2. Jee SH, Lee JK, Kim IS. Smoking-attributable mortality among Korean adults: 1981-2003. Korean J Epidemiol. 2006; 28:92–99.
3. Yoon SJ, Ha BM, Kang JW, Chang HC. Estimation of attributable burden due to premature death from Smoking in Korea. Korean J Prev Med. 2001; 34:191–199.
4. Johnson GK, Slach NA. Impact of tobacco use on periodontal status. J Dent Educ. 2001; 65:313–321.

5. Scabbia A, Cho KS, Sigurdsson TJ, Kim CK, Trombelli L. Cigarette smoking negatively affects healing response following flap debridement surgery. J Periodontol. 2001; 72:43–49.

6. Sham AS, Cheung LK, Jin LJ, Corbet EF. The effects of tabacco use on oral health. Hong Kong Med J. 2003; 9:271–277.
7. Heasman L, Stacey F, Preshaw PM, McCracken GI, Hepburn S, Heasman PA. The effect of smoking on periodontal treatment response: A review of clinical evidence. J Clin Periodontol. 2006; 33:241–253.

8. Baelum Vibeke. CPITN and the epidemiology of periodontal disease. Community Dent Oral Epidemiol. 1996; 24:367–8.
9. Millar WJ, Locker D. Smoking and oral health status. JCDA. 2007; 73:155–155.
11. Jung YH, Ko SJ, Lee YG, Park SB, Lee JH. Lifetime cost of obesity and smoking and long-term effectiveness of health promotion. KI-HASA. 2010.
12. National Health Insurance Service, Understanding for Korea Health Panel. KIHASA. 2008.
13. Kim HS, Kim MK, Shin HS. Expenditure in ambulatory dental care and factors related to its spending. HPM. 2012; 22:207–224.

14. Ministry of Health and Welfare, Korea Centers for Disease Control and Prevention. 2013 6th(1st year) national health statistics.
15. Han DH, Kim JB. The association between smoking and periodontitis: finding from The Korean National Oral Health Survey 2006. J Korean Acad Dent Health. 2009; 33:634–643.
16. Ryu MH. The effects of smoking on oral mucosa. The Journal of Namseoul Univ. 2004; 10:449–468.
18. Preber H, Linder L, Bergstrom J. Periodontal healing and perio-pathogenic microflora in smokers and non-smokers. J Periodontol. 1995; 22:946–952.

20. Arno A, Waerhaug J, Lovdal A, Schei O. Incidence of gingivitis as related to sex, occupation, tabacco consumption, toothbrushing, and age. Oral Surg Oral Med Oral Pathol. 1958; 11:587–595.
21. Grossi SG, Genco RJ, Machtei EE, Ho AW, Koch G, Dunford R, et al. Assessment of risk for periodontal disease. Ⅱ. Risk indicators for alveolar bone loss. J Periodontol. 1995; 66:23–29.
22. Martinez-Canut P, Lorca A, Margan R. Smoking and periodontal disease severity. J Clin Periodontol. 1995; 22:743–749.

23. Harber J, Kent RL. Cigarette smoking in periodontal practice. J Peri-odontol. 1992; 63:100–106.
25. Park HD. The impact of smoking on the utilization of dental health services [master’s thesis]. Seoul: Graduate School of Public Health Yonsei Univ;2008. Korean.
26. Park JH, Kim YN, Yoo JH, KIM MY, Kim BI, Kwon HK. Relationship between smoking and periodontal pocket formation in Korean adults. J Korean Acad Dent Health. 2005; 29:293–301.
27. Song AR, Park JW. A study on the attitudes about smoking and factor analysis among women students of college -By oriented students of Gimcheon College. Gimcheon College Report. 2004; 25:113–138.
Fig. 1.
Crude utilization ambulatory dental care rate according to smoking pack-years in the 40-59 age group.
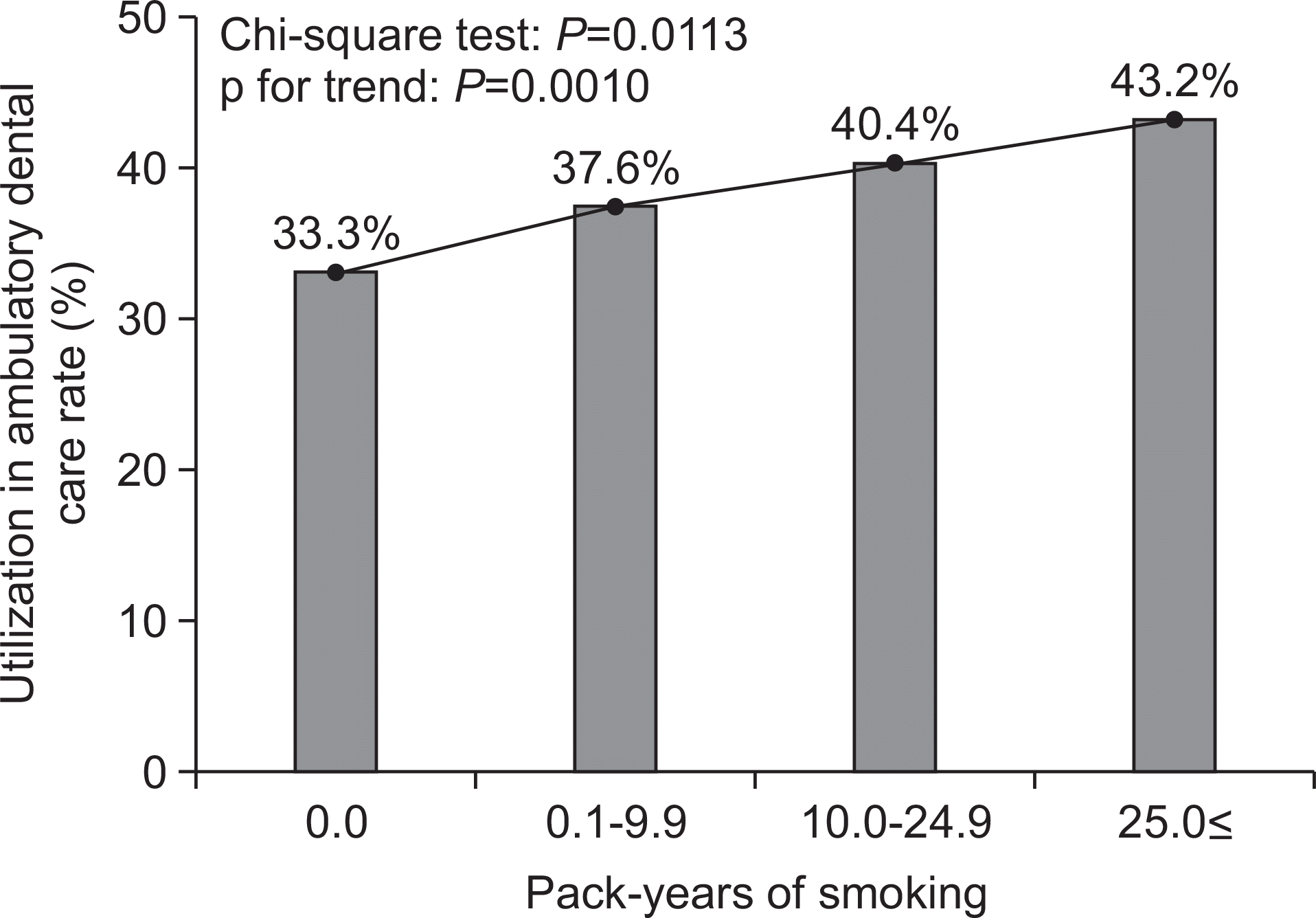
Table 1.
General Characteristics according to experience and pack-years of smoking
Table 2.
Effects of pack-years of smoking on dental utilization by age
Table 3.
Cure rate by treatment contents according to pack-years in 40-59 years (Unit : %)
Table 4.
Effects of pack-years of smoking on expense of ambulatory dental care by age unit: won (₩)
Table 5.
Effects of smoking history on expense of ambulatory dental caer in the group of 40-59 years old




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download