Abstract
Objectives
The both values of neutrophil lymphocyte ratio (NLR) and platelet lymphocyte ratio (PLR) were reported as indexes of systemic inflammation and readily available and inexpensive prognostic markers in patients with solid cancer. The objective of this study was to clarify whether the NLR and PLR were significant prognostic markers in Korean diffuse large B-cell lymphoma (DLBCL) patients treated with R-CHOP as a first line therapy.
Methods
: We retrospectively collected the clinical data of ninety nine DLBCL patients treated with R-CHOP from 2004 to 2012 and analyzed. NLR and PLR were calculated from complete blood count (CBC) and differential leukocyte count.
Results
: In univariate analysis, NLR was significantly associated with 5-year progression free survival(PFS) rate (P= 0.039), but not significantly associated with 5-year overal survival (OS) rate (P= 0.276). PLR was not significantly associated with 5-year PFS (P= 0.632) and OS rate (P= 0.855). In multivariate analysis, NLR was not a significant independent prognostic factor for 5-year PFS (P= 0.415) and OS rate (P= 0.991).
Go to : 
References
1. Mantovani A, Allavena P, Sica A, Balkwill F. Cancer-related inflammation. Nature. 2008; 454:436–44.

3. DeNardo DG, Andreu P, Coussens LM. Interactions between lymphocytes and myeloid cells regulate pro-versus antitumor immunity. Cancer Metastasis Rev. 2010; 29:309–16.
5. Roxburgh CS, McMillan DC. Role of systemic inflammatory response in predicting survival in patients with primary operable cancer. Future Oncol. 2010; 6:149–63.

6. Kim DK, Oh SY, Kwon HC, Lee S, Kwon KA, Kim BG, et al. Clinical significances of preoperative serum interleukin-6 and C-reactive protein level in operable gastric cancer. BMC Cancer. 2009; 9:155.

7. Crumley AB, McMillan DC, McKernan M, McDonald AC, Stuart RC. Evaluation of an inflammation-based prognostic score in patients with inoperable gastro-oesophageal cancer. Br J Cancer. 2006; 94:637–41.

8. Chua W, Charles KA, Baracos VE, Clarke SJ. Neutrophil/lymphocyte ratio predicts chemotherapy outcomes in patients with advanced colorectal cancer. Br J Cancer. 2011; 104:1288–95.

9. Smith RA, Bosonnet L, Raraty M, Sutton R, Neoptolemos JP, Campbell F, et al. Preoperative platelet-lymphocyte ratio is an independent significant prognostic marker in resected pancreatic ductal adenocarcinoma. Am J Surg. 2009; 197:466–72.

10. Engelken FJ, Bettschart V, Rahman MQ, Parks RW, Garden OJ. Prognostic factors in the palliation of pancreatic cancer. Eur J Surg Oncol. 2003; 29:368–73.

11. McMillan DC, Elahi MM, Sattar N, Angerson WJ, Johnstone J, McArdle CS. Measurement of the systemic inflammatory response predicts cancer-specific and non-cancer survival in patients with cancer. Nutr Cancer. 2001; 41:64–9.

12. Bachelot T, Ray-Coquard I, Catimel G, Ardiet C, Guastalla JP, Dumortier A, et al. Multivariable analysis of prognostic factors for toxicity and survival for patients enrolled in phase I clinical trials. Ann Oncol. 2000; 11:151–6.

13. Viganó A, Bruera E, Jhangri GS, Newman SC, Fields AL, Suarez-Almazor ME. Clinical survival predictors in patients with advanced cancer. Arch Intern Med. 2000; 160:861–8.

14. O'Mahony JB, Palder SB, Wood JJ, Mclrvine A, Rodrick ML, Demling RH, et al. Depression of cellular immunity after multiple trauma in the absence of sepsis. J Trauma. 1984; 24:869–75.
15. O'Gorman P, McMillan DC, McArdle CS. Prognostic factors in advanced gastrointestinal cancer patients with weight loss. Nutr Cancer. 2000; 37:36–40.
16. Sierko E, Wojtukiewicz MZ. Platelets and angiogenesis in malignancy. Semin Thromb Hemost. 2004; 30:95–108.

17. Alexandrakis MG, Passam FH, Moschandrea IA, Christophoridou AV, Pappa CA, Coulocheri SA, et al. Levels of serum cytokines and acute phase proteins in patients with essential and cancer-related thrombocytosis. Am J Clin Oncol. 2003; 26:135–40.

18. Klinger MH, Jelkmann W. Role of blood platelets in infection and inflammation. J Interferon Cytokine Res. 2002; 22:913–22.
19. He W, Yin C, Guo G, Jiang C, Wang F, Qiu H, et al. Initial neutrophil lymphocyte ratio is superior to platelet lymphocyte ratio as an adverse prognostic and predictive factor in metastatic colorectal cancer. Med Oncol. 2013; 30.

20. Bhatti I, Peacock O, Lloyd G, Larvin M, Hall RI. Preoperative hematologic markers as independent predictors of prognosis in resected pancreatic ductal adenocarcinoma: neutrophil-lymphocyte versus platelet-lymphocyte ratio. Am J Surg. 2010; 200:197–203.

21. Kwon HC, Kim SH, Oh SY, Lee S, Lee JH, Choi HJ, et al. Clinical significance of preoperative neutrophil-lymphocyte versus platelet-lymphocyte ratio in patients with operable colorectal cancer. Biomarkers. 2012; 17:216–22.

22. Cox MC, Nofroni I, Laverde G, Ferrari A, Amodeo R, Tatarelli C, et al. Absolute lymphocyte count is a prognostic factor for diffuse large B-cell lymphoma. Br J Haematol. 2008; 141:265–8.
23. Oki Y, Yamamoto K, Kato H, Kuwatsuka Y, Taji H, Kagami Y, et al. Low absolute lymphocyte count is a poor prognostic marker in patients with diffuse large B-cell lymphoma and suggests patients survival benefit from rituximab. Eur J Haematol. 2008; 81:448–53.

24. Kim DH, Baek JH, Chae YS, Kim YK, Kim HJ, Park YH, et al. Absolute lymphocyte counts predicts response to chemotherapy and survival in diffuse large B-cell lymphoma. Leukemia. 2007; 21:2227–30.

25. Porrata LF, Ristow K, Habermann T, Inwards DJ, Micallef IN, Markovic SN. Predicting survival for diffuse large B-cell lymphoma patients using baseline neutrophil/lymphocyte ratio. Am J Hematol. 2010; 85:896–9.

26. MacDonald N. Cancer cachexia and targeting chronic inflammation: a unified approach to cancer treatment and palliative/supportive care. J Support Oncol. 2007; 5:157–62.
27. Maltoni M, Caraceni A, Brunelli C, Broeckaert B, Christakis N, Eychmueller S, et al. Prognostic factors in advanced cancer patients: evience -based clinical recommendations–a study by the Steering Committee of the European Association for Palliative Care. J Clin Oncol. 2005; 23:6240–8.
Go to : 
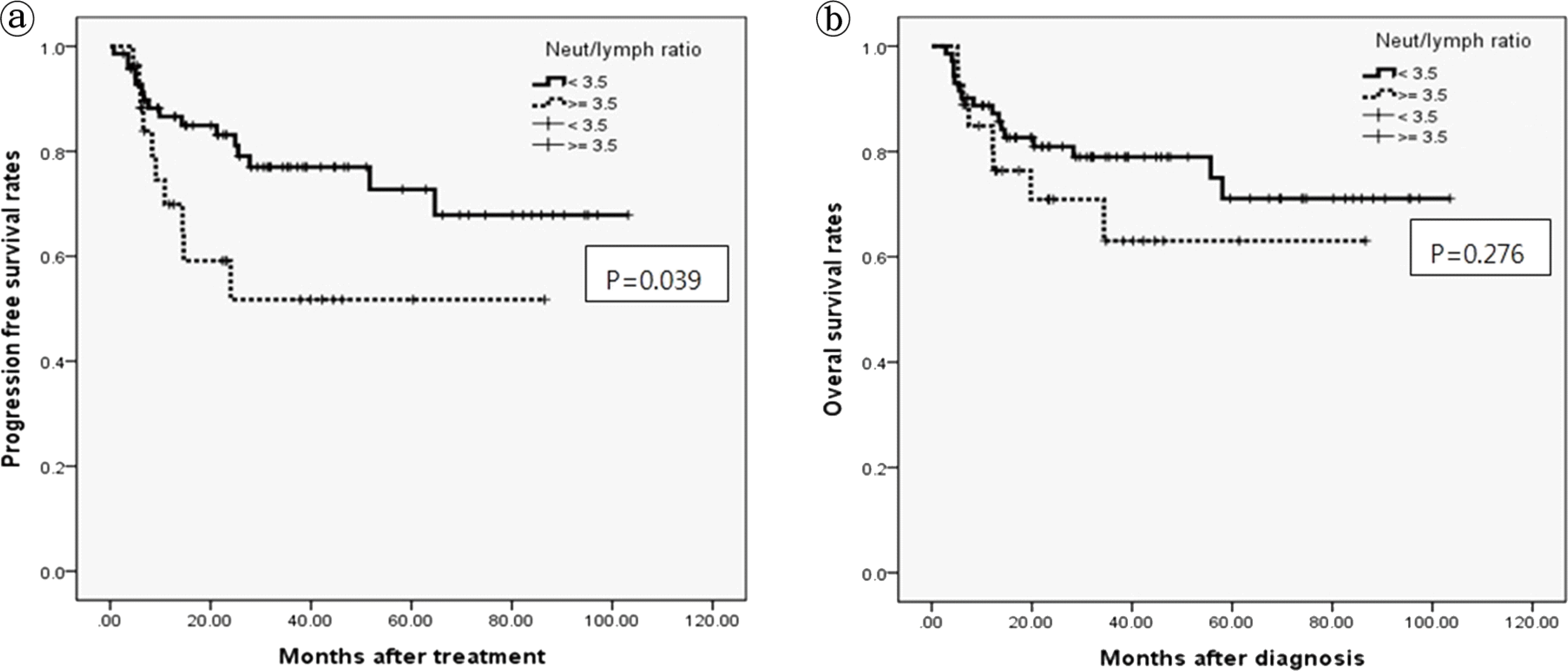 | Fig. 1.Five years progression free survival curves and overall survival curves according to Neutrphil/lymphocyte ratio in patients with diffuse large B-cell lymphoma. a. Five years progression free survival curves b. Five years overall survival curves |
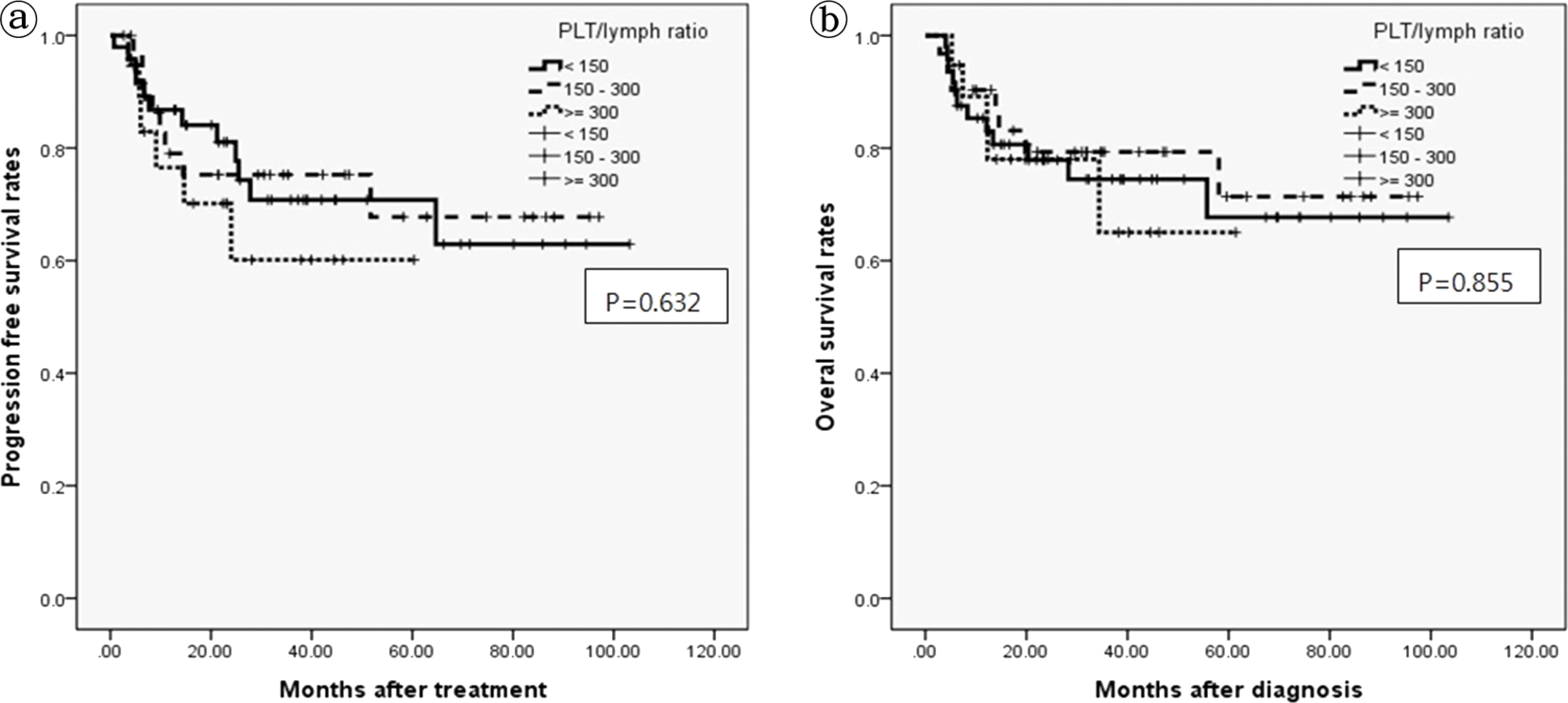 | Fig. 2.Five years progression free survival curves and overall survival curves according to Platelet/lymphocyte ratio in patients with diffuse large B-cell lymphoma. a. Five years progression free survival curves b. Five years overall survival curves |
Table 1.
Patient characteristics
Table 2.
Prognostic factors for survival in patients with DLBCL by univariate analysis
Table 3.
Independent prognostic factors for survival in patients with DLBCL by multivariate analysis




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download