Abstract
Purpose
The presented study aims to evaluate the effects of osteoporosis on dental implants by analyzing a 12-year cumulative survival rate of implants placed in patients with osteoporosis.
Methods
37 patients with history of osteoporosis were selected from a pool of dental implant patients treated at the Department of Periodontology in Yonsei University Hospital between 1993 and 2007. The cumulative survival rate is quantified using data collected from 164 placed implants in the selected 37 patients.
Results
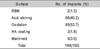
3 out of the 164 implants failed and the cumulative survival rate was observed at 95.1%. The survival rates of the implants according to patients' age were 97.41% (<60) and 100% (60≤. The lower survival rate was directly proportional to younger age, and this relationship is statistically significant (P<0.05). The survival rates of implants according to diagnostic criteria were 95.45% (osteopenia) and 98.59% (osteoporosis; 2 out of 142 implants placed in osteoporosis patients failed). The difference in the two survival rates is statistically significant (P<0.05). The survival rates according to the region of implants do not have statistically significant difference. The survival rates according to the different length and diameter of the implants do not have statistically significant difference. The survival rates of implants accompanied and not accompanied by bone augmentation were 92.11% and 100%, respectively. The difference in the two survival rates is statistically significant (P<0.05). The survival rates of implants placed in patients with and without history of medication for osteoporosis treatment are 96.67% and 99.04%, respectively. The difference in the two survival rates is statistically significant (P<0.05).
Figures and Tables
References
2. An Editorial Department of The Korean society of bone metabolism. Treatment guidelines of osteoporosis. Osteoporosis. 2006. 3rd ed. Seoul: The Korean society of bone metabolism;463–492.
3. Kanis JA. Assessment of fracture risk and its application to screening for postmenopausal osteoporosis: synopsis of a WHO report. WHO study group. Osteoporosis Int. 1994. 4:368–381.

4. Kanis JA, Melton LJ III, Christiansen C, Johnston CC, Khaltaev N. The diagnosis of osteoporosis. J Bone Miner Res. 1994. 9:1137–1141.

5. Okamura A, Ayukawa Y, Iyama S, Koyano K. Effect of the difference of bone turnover on peri-titanium implant osteogenesis in ovariectomized rats. J Biomed Mater Res A. 2004. 70:497–505.

6. Grassi S, Piattelli A, Ferrari DS, et al. Histological evaluation of human bone integration on machined and sandblasted acid-etched titanium surfaces in type IV bone. J Oral Implantol. 2007. 33:8–12.

7. Shibli JA, Grassi S, de Figueiredo LC, et al. Influence of implant surface tomography on early osseointegration: A histological study in human jaws. J biomed Mater Res B Appl Biomater. 2007. 80:377–385.
8. Jiang G, Matsumoto H, Fujii A. Mandible bone loss in osteoporosis rats. J Bone Miner Metab. 2003. 21:388–395.

9. Cao T, Shirota T, Tamazaki M, Ohno K, Michi KI. Mineral bone loss in partially edentulous trabeculae of ovariectomized rabbit mandibles. J Periodontal Res. 2004. 39:37–41.

10. Yang J, Farnell D, Devlin H, horner K, Graham J. The effect of ovariectomy on mandibular cortical thickness in the rat. J Dent. 2005. 33:123–129.

11. Raisz LG. Pathogenesis of osteoporosis: concepts, conflicts, and prospects. J Clin Invest. 2005. 115:3318–3325.

12. Raisz LG, Rodan GA. Pathogenesis of osteoporosis. Endocrinol Metab Clin North Am. 2003. 32:15–24.

13. Keller JC, Stewart M, Roehm M, Schneider GB. Osteoporosis-like bone conditions affect ossointegration of implants. Int J Oral Maxillofac Implants. 2004. 19:687–694.
14. Schliephake H, neukam FW, wichmann M. Survival analysis of endosseous implants in bone grafts used for the treatment of severe alveolar ridge atrophy. J Oral Maxillofac Surg. 1997. 55:1227–1233.

15. Blomqvist JE, Alberius P, Isaksson S, Linde A, hansson BG. Factors in implant integration failure after bond grafting: an osteometric and endocrinologic matched analysis. Int J Oral Maxillofac Surg. 1996. 25:63–68.
16. Toffler M. Osteotome-mediated sinus floor elevation: a clinical report. Int J Oral Maxillofac Implants. 2004. 19:266–273.
17. Friberg B, Ekestubbe A, Mellstrom D, Sennerby L. Brånemark Implants and Osteoporosis. A Clinical Exploratory Study. Clin Implant Dent Relat Res. 2001. 3:50–56.

18. Buser D, Weber HP, Lang NP. Tissue integration of non-submerged implants. 1-year results of a prospective study with 100 ITI hollow-cylinder and hollow-screw implants. Clin Oral Implants Res. 1990. 1:33–40.

19. Buser D, Mericske-Stern R, Bernard JP, et al. Long-term evaluation of prospective multi-center study with 2359 implants. Clin Oral Implants Res. 1997. 8:161–172.

20. Cochran DL, Buser D, ten Burugenakte C, et al. The use of reduced healing times on ITI implants with a sandblasted and etched (SLA) surface : early results from clinical trials on ITI SLA implants. Clin Oral Implants Res. 2002. 13:144–153.

22. Teegarden D, Proulx WR, Martin BR, et al. Peak bone mass in young women. J Bone Miner Res. 1995. 10:711–715.

24. Geurs NC, Lewis CE, Jeffcoat MK. Osteoporosis and periodontal disease progression. Periodontol 2000. 2003. 32:105–110.

25. Esposito M, Hirsch J-M, Lekholm U, Thomsen P. Biological factors contributing to failures of osseointegrated oral implants. Success criteria and epidemiology. Eur J Oral Sci. 1998. 106:527–551.

26. Holahan CM, Koka S, Kennel KA, et al. Effect of osteoporotic status on the survival of titanium dental implants. Int J Oral Maxillofac Implants. 2009. 23:905–910.
27. Kribbs PJ, Smith DA, Chesnut CH, Ott SM, Kilcoyne RF. Relationship between mandibular and skeletal bone in an osteoporotic population. J Prothet Dent. 1989. 62:703–707.

28. Kribbs PI, Smith DA, Chesnut CH. Oral findings in osteoporosis. Part I: measurement of mandibular bone density. J Prosthet Dent. 1983. 50:576–579.

29. Jeffcoat MK, Lewis CE, Reddy MS, Wang CY, Redford M. Post-menopausal bone loss and its relationship to oral bone loss. Periodontol 2000. 2000. 23:94–102.

30. Southard KA, Southard TE, Schlechte JA, Meis PA. The relationship between the density of the alveolar processes and that of post-cranial bone. J Dent Res. 2000. 79:964–969.

31. Elders PJ, Habets LL, Netelenbos JC, van der Linden LW, van der Stelt PF. The relation between periodontitis and systemic bone mass in women between 46 and 55 years of age. J Clin Periodontol. 1992. 19:492–496.

32. Adell R, Lekholm U, Rockler B, et al. A 15 year study of osseointegrated implants in the treatment of the edentulous jaw. Int J Oral Surg. 1981. 10:387–416.

33. Schnitman PA, Rubenstein JE, Whrle PS, DaSilva JD, Koch GG. Implants for partial edentulism. J Dent Educ. 1988. 52:725–736.

34. Lum LB. A biomechanical rationale for the use of short implants. J Oral Implantol. 1991. 17:126–131.
35. Erdogan O, Shafer DM, Taxel P, Freilich MA. A review of the association between osteoporosis and alveolar ridge augmentation. Oral Surg Oral Med Oral Pathol Oral Radiol Endod. 2007. 104:738e1–e13.
36. Watts Nelson B. Osteonocrosis of the jaw. South Med J. 2008. 101:160–165.
37. van Steenberghe D, Jacobs R, Desnyder M, Maffei G, Quirynen M. The relative impact of local and endogenous patient-related factors on implant failure up to the abutment stage. Clin Oral Impl Res. 2002. 13:617–622.

38. Alsaadi G, Quirynen M, Komarek A, van Steenberghe D. Implact of local and systemic factors on the incidence of oral implant failures, up to abutment connection. J Clin Periodontol. 2007. 34:610–617.





 PDF
PDF Citation
Citation Print
Print


















 XML Download
XML Download