Abstract
Background
Atopic dermatitis (AD) is a common, complex disease that follows a chronic relapsing course and significantly affects the quality of life of patients. Skin barrier dysfunction and inflammatory processes induce and aggravate this skin condition. Proper use of an emollient for hydration is a keystone of AD treatment. Bee venom is known to have anti-inflammatory effects and has been widely used in traditional medicine to treat various inflammatory disorders.
Objective
To find out the beneficial effect of an emollient containing bee venom in the treatment of patients with AD.
Methods
This study included 136 patients with AD who were randomized to receive either an emollient containing bee venom and silk-protein or a vehicle that was identical except for the bee venom for 4 weeks. The patients were instructed to apply the emollient twice daily on their entire body and not to use other medications, including topicals, during the course of the study. The eczema area and severity index (EASI) score, transepidermal water loss, and visual analogue scale (VAS) score of itching were evaluated at the first visit and after 2 and 4 weeks. The investigator global assessment was evaluated at 2 and 4 weeks after the application of emollient containing bee venom or vehicle.
Atopic dermatitis (AD) is a chronic, relapsing skin disorder characterized by defects in epidermal barrier function and cutaneous inflammation1. It is one of the most common skin diseases, estimated to be present in up to 20% of children and 1%~3% of adults worldwide2. Although the pathophysiology of AD remains unclear, epidermal barrier dysfunction due to genetic defects and immunologic responses plays a key role in the development and aggravation of AD1. Whether epidermal dysfunction precedes immune dysregulation ('outside-in' hypothesis) or immune dysregulation precedes barrier abnormalities ('inside-out' hypothesis), it is clear that skin barrier function is important in the pathophysiology of AD3. The 'brick and cement' structure of skin keratinocytes functions as a barrier, protecting skin from exogenous material and preventing moisture loss. Barrier disruption due to abnormal lipid metabolism and abnormal structural protein formation (filaggrin, etc.) facilitates allergen penetration into the skin, increasing the risk of subsequent inflammation and contributing to chronic and recalcitrant eczema2. While acute flares should be managed with topical steroids and immunomodulators, the fundamental therapy for AD is based on skin hydration and restoration of the disrupted skin barrier. As skin xerosis and barrier dysfunction are the main symptoms of AD, regular use of appropriate emollients remains the mainstay of maintenance therapy2. Skin hydration and replacement of membrane lipids improve xerosis, maintains skin barrier function, relieves pruritus, and have a steroid-sparing effect24.
In the acute phase of AD, inflammatory dendritic epidermal cells, differentiated from recruited monocytes, produce the proinflammatory cytokines interleukin (IL)-1, IL-6, and tumor necrosis factor (TNF)-α5. Type 2 helper T (Th2) inflammatory responses occur predominantly in the initiation stage of AD2. Th2 cytokines, such as IL-4, IL-13, IL-17, are also increased in acute skin lesions. The cytokines produced during the initial stage of disease development increase the expression of chemokines and adhesion molecules, which leads to the recruitment of leukocytes in the skin6. In contrast, Th1 cell-mediated responses occur in the chronic phase, with increases in interferon-γ. Thus, application of topical and systemic anti-inflammatory agents is important in the management of AD, resulting in the prevention of these pathogenic reactions.
Patients with AD have a predisposition to colonization and infection by a number of microbial organisms, especially Staphylococcus aureus3. Moreover, a number of reports have revealed a positive correlation between S. aureus colonization density and AD severity37. S. aureus-derived products, such as toxins with superantigenic properties and lipoteichoic acid, can exacerbate disease. The severity of AD can be improved with antistaphylococcal antibiotic treatment8. Moreover, the prevention of colonization by S. aureus in normal skin may prevent secondary eczematous lesions caused by subsequent inflammatory responses. Thus, one of the important goals of AD treatment should be the eradication of S. aureus residing in patient skin.
Bee venom has been used in traditional medicine to treat various inflammatory conditions. Some studies have demonstrated the anti-inflammatory effects of bee venom, reporting downregulation of IL-1 and TNF-α through suppression of nuclear factor (NF)-κB59. Moreover, several reports have demonstrated that melittin, the main component of bee venom, has antimicrobial activity, especially against S. aureus1011. Based on these previous studies, emollient containing bee venom is expected to have a beneficial effect in treating AD, due to its anti-inflammatory as well as anti-microbial properties. Therefore, in the present clinical trial, we aimed to investigate the beneficial effects of an emollient containing bee venom and silk protein, which is known as an emollient for its hydrating potency, with regard to improvement in disease severity, skin barrier function, and pruritus relief.
This study included 136 patients with AD randomized to receive an emollient containing bee venom and silk-protein (Dongsung Pharmaceutical, Seoul, Korea) (experimental group) or a vehicle (vehicle group) that was identical to the test compound except for the bee venom for 4 weeks. Subjects in both the experimental and vehicle groups were instructed to apply the cream twice daily on the entire body and not to use other medications, including topical medication, during the course of the study. The patients were evaluated at baseline, 2, and 4 weeks by a primary investigator. The primary endpoint of the study was the eczema area and severity index (EASI) score in both groups. The secondary endpoints were transepidermal water loss (TEWL), pruritus relief, and investigator global assessment (IGA) score. The EASI score was calculated for the affected area and eczema severity by a primary investigator. TEWL was measured using a Tewameter® TM 210 (Courage-Khazaha, Koln, Germany) on same spot of the right forearm of the patient regardless of the presence of eczema lesion, according to the manufacturer's guidelines. Pruritus relief was assessed with a visual analogue scale (VAS) by the patients themselves. This scale assigns a numeric value to pruritus severity from 1 to 10, with 10 being most severe. IGA was graded on a seven-point scale (1, greatly worsened; 2, moderately worsened; 3, worsened slightly; 4, no change; 5, slightly improved; 6, moderately improved; 7, greatly improved) by a primary investigator during visits 2 and 3. Adverse drug reactions were evaluated in all patients during visits 2 and 3. The severity of adverse drug reactions was classified as mild (does not impair daily activity and does not require treatment), moderate (impairs daily activity and requires treatment), severe (severely impairs daily activity and may require admission), and life threatening.
For appropriate statistical analysis, we calculated the required number of patients. To achieve a statistical power of 1–β ≥0.8 at a significance level of 0.05, it is known that (1+λ)σ2(zα/2+z1-β)2/λ(µa–µb) ≤n is required (µa=the average value of the EASI score in the experimental group, µb=the average value of the EASI score in the vehicle group, λ=the required number of patients in the vehicle group, n=the required number of patients in the experimental group). It is known that λ=1 is needed for minimization of the number of patients. In a previous study12, the average EASI score was 9.51 at baseline. From the results of another study on the use of emollient13, the EASI score of the vehicle group was expected to decrease by 37.5% after 4 weeks. Moreover, from the results of a previous study comparing an emollient containing bee venom and vehicle in NC/Nga mice, the EASI score decrease in the experimental group was expected to be 1.44 times higher than that in the vehicle group. Based on these results, µa–µb was estimated to be 1.57. From the results of a previous clinical study13, Var(Xb)=2.51 and Var(Xa)=5.12 (Xb=EASI score at the baseline, Xa=EASI score after 4 weeks) were assumed, and σ2 was estimated to be 7.63. Finally, the required number of patients for appropriate statistical analysis was at least 49 for each the experimental group and vehicle group. Considering a 20% drop-out rate, the required number of patients for each group was estimated to be 62. Based on this, we decided to enroll at least 124 patients in this study.
For this study, 136 patients with AD who visited Severance Hospital, Seoul National University Hospital, Hallym University Kangnam Sacred Heart Hospital, Chung-Ang University Hospital, or Incheon St. Mary's Hospital were enrolled between the beginning of September 2014 and the end of January 2015. This study was approved by the Incheon St. Mary's Hospital Institutional Review Board (IRB no. OC14MIMI0080). The diagnosis of AD was based on the modified Hanifin and Rajka's criteria. The inclusion criteria were defined as follows: (1) Age 2 years or older; (2) EASI score 5 or higher; (3) Patients who voluntarily agreed to participate in the study (in case of patient under age 18, a legal guardian agreed to participate in the study). The exclusion criteria were defined as follows: (1) Treatment with any systemic immunosuppressive agents or immunomodulators within 1 month of the study; (2) treatment with any anti-histaminergic agents within 1 week of the study; (3) previous hypersensitivity reaction to bee venom in the 5 years before the study. Patients who applied topical medications, including topical corticosteroids, were included in the study, but they were not allowed to apply them during the course of the study.
Statistical analysis was performed using SAS ver. 9.3 (Statistical Analysis System, Cary, NC, USA). T-test was used for continuous data and a Wilcoxon rank sum test for categorical data. The principle of last observation carried forward was used in both analyses, using the score recorded just prior to the missing scores in cases of missing post-treatment values. The data were analyzed for the group adhering to the study with an "intention-to-treat" application model (full analysis set, FAS) for analysis of data for clinical trials. Test results that produced p-values <0.05 were regarded as statistically significant.
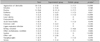
Of the 136 patients who were initially enrolled, 22 who violated FAS criteria were excluded from the statistical analysis for not visiting the hospital at least once after application of the emollient. The remaining 114 individuals who were evaluated at least once in addition to the baseline evaluation were included in statistical analysis. No statistically significant differences were present in number of early withdrawals between the experimental and vehicle groups. No statistically significant differences were noted at baseline between the two groups based on age, sex, TEWL, EASI score, or VAS score for pruritus (Table 1).
The decreases in EASI scores during the study period are shown in Table 2 and Fig. 1A. The EASI score of the experimental group was significantly decreased from 9.29±3.71 at baseline. The percent decrease of EASI score was –25.16%±3.91% (p=0.023) at visit 2 and –34.69%±4.55% (p=0.022) at visit 3, which were significantly larger compared to the values for the vehicle group (–13.47%± 3.27% at visit 2 and –19.66%±4.64% at visit 3).
The changes in TEWL value are shown in Table 2 and Fig. 1B. From 27.87±13.5 at baseline, the TEWL value measured on the right forearm of the experimental group changed by 6.15%±8.65% (p=0.427) and 6.97%±7.25% (p=0.571) when measured during visit 2 and visit 3, respectively. The decreases in TEWL value were not statistically significantly different between the experimental group and the vehicle group.
The changes in VAS score for pruritus are shown in Table 2 and Fig. 1C. The VAS score for pruritus was significantly decreased in the experimental group at visit 3. From 5.53±1.82 at baseline, decreases of –0.95±0.25 (p=0.179) at visit 2 and –1.50±0.31 (p=0.03) at visit 3 were observed, compared to the vehicle group, which showed –0.48±0.24 and –0.55±0.30 decreases at visit 2 and visit 3, respectively.
The results of the IGA are shown in Fig. 2. A Wilcoxon rank sum test was used to identify the differences between the treated and untreated groups. No statistically significant difference was noted between the experimental and vehicle groups at visit 2 (p=0.1086) or visit 3 (p=0.4228).
All of the reported adverse drug reactions are shown in Table 3. Irritation (5), pruritus (13), erythema (4), urticaria (3), and disease exacerbation (10) were commonly reported as adverse cutaneous drug reactions. All of the reported adverse reactions were classified as mild, which did not impair daily activity and did not require any treatment. Of the 71 patients who applied emollient containing bee venom, 25 (35.2%) experienced adverse drug reactions. Of the 65 patients who applied the vehicle, 15 (23.1%) experienced adverse drug reactions. There were no statistically significant differences in the incidence of adverse drug reactions between the experimental and vehicle groups (p=0.135, Fisher's exact test). Incidences of all reported adverse drug reactions showed no statistically significant difference between two groups.
In the present study, we demonstrated the efficacy and safety of emollient containing bee venom for the treatment of AD. To our knowledge, this is the first clinical study demonstrating the efficacy of bee venom on human skin. The experimental group showed a significant improvement in EASI score and VAS score for pruritus. However, the TEWL and IGA values did not differ from those in the vehicle group. This may be due to the hydrating effect of silk protein. Silk protein is an ingredient registered in the international cosmetic ingredient dictionary and is widely used in cosmetics for its excellent moisture-binding properties. In this study, silk protein was used as a vehicle and applied identically in both the experimental group and the vehicle group. The moisturizing effect of silk protein might have improved the skin barrier function and, therefore, lessened the differences in TEWL and IGA between the two groups of patients.
The rationale for barrier repair therapy in AD goes beyond trapping moisture and preventing xerosis14. Restoration of the normal skin barrier function by emollient use can down-regulate inflammation and reduce the symptoms and flares of AD15. Additionally, regular use of emollient may also reduce the need for topical corticosteroid by 50%16. Consequently, regular use of emollient is important in AD management.
From an immunologic point of view, in the acute phase of AD, recruited monocytes produce proinflammatory cytokines, such as TNF-α and IL-1β, which are important in regulating T cell activation and in stimulating the acute phase reaction, supporting the recruitment, proliferation, and survival of leukocytes in the skin6. There have been reports suggesting that TNF-α and IL-1β play important roles in eczema development with increasing skin irritability and pruritus517.
Among the colonized microbial organisms in AD patient's skin, S. aureus is cultured from 90% of eczematous lesions and also resides in normal-appearing skin in AD patients18. Colonization by S. aureus not only increases the risk of infection, but also exacerbates skin inflammation through secretion of toxins with superantigenic properties, resulting in activation of T cells and other immune system components. Staphylococcal superantigens induce mast cell degranulation and specific IgE antibody production that leads to T cell proliferation and increases in IL-31, which induces pruritus. Thus, S. aureus contribute to pruritus and to the inflammatory changes in AD skin315.
Recently, much attention has been focused on discovering substances used in traditional medicine and evaluating their efficacy and safety. Bee venom has been used in China, Japan, and Korea for the treatment of various inflammatory disorders, including arthritis. Bee venom is a complex mixture of at least 18 pharmacologically active components, including melittin, apamin, adolapin, phospholipase A2, and mast cell deregulating peptide11. Among these compounds, melittin is the principal toxin and the major active peptide, contributing 52% of the dry weight of bee venom19. Bee venom, especially the melittin component, has been widely researched and has been shown to exert various effects. Han et al.20 reported an anti-inflammatory effect of bee venom in rats. In another study, it was shown that pre-treatment with bee venom significantly inhibited compound 48/80-induced scratching in rats. Bee venom was shown to have an anti-inflammatory effect and suppressed AD-related pruritus by reducing degranulation of mast cells and expression of pro-inflammatory cytokines. Bee venom or melittin has been suggested to inhibit the DNA binding activity of NF-κB through inhibition of IκB phosphorylation and p50 translocation. It is possible that bee venom binds directly to p50 and inhibits NF-κB activation9. Moreover, several studies have clearly demonstrated the broad antibiotic effects of bee venom, especially with respect to anti-staphylococcal potency1121.
Considering the anti-inflammatory effects of bee venom and the characteristics of AD, an emollient containing bee venom was expected to have advantages over other emollients in treating AD. Our study showed the beneficial effect of an emollient containing bee venom on AD, resulting in significant decreases in EASI score and pruritus. Bee venom not only prevented proinflammatory cytokine production, but also reduced pruritus and prevented keratinocyte damage from scratching, which may reduce the inflammatory cytokines released from keratinocytes. These anti-inflammatory and pruritus-reducing properties of bee venom are effective as maintenance therapy for AD. Furthermore, the antibiotic effect of bee venom may improve skin eczema and pruritus by eradicating S. aureus. With respect to safety, one study previously showed that bee venom applied topically to the skin does not induce any irritation or toxicity in rabbits22. Another study showed that topically applied bee venom does not induce any cutaneous sensitization or anayphlactic reaction in mice23. Our study found no significant differences in the incidences of adverse reactions caused by bee venom on human skin and demonstrated its safety.
In conclusion, this double-blinded, randomized, controlled, multicenter study suggests that an emollient containing bee venom may be an efficient and safe option for patients with AD, resulting in improvements in disease severity and pruritus.
Figures and Tables
 | Fig. 1Comparison of the outcomes at visit 2 and visit 3, assessed as change from baseline: (A) The percent decrease in eczema area severity index (EASI) score. (B) The percent decrease in transepidermal water loss (TEWL). (C) Decrease in visual analogue scale (VAS) score for pruritus. *Statistically significant decrease compared to vehicle group. |
Table 1
Demographic characteristics and baseline data of the experimental and vehicle groups (n=114)

Table 2
Efficacy assessment at visit 2 and visit 3

Table 3
Adverse drug reactions
References
1. Boguniewicz M, Leung DY. Atopic dermatitis: a disease of altered skin barrier and immune dysregulation. Immunol Rev. 2011; 242:233–246.

2. Wakao S, Kuroda Y, Ogura F, Shigemoto T, Dezawa M. Regenerative effects of mesenchymal stem cells: contribution of muse cells, a novel pluripotent stem cell type that resides in mesenchymal cells. Cells. 2012; 1:1045–1060.

3. Boguniewicz M, Leung DY. Recent insights into atopic dermatitis and implications for management of infectious complications. J Allergy Clin Immunol. 2010; 125:4–13.

4. Angelova-Fischer I, Neufang G, Jung K, Fischer TW, Zillikens D. A randomized, investigator-blinded efficacy assessment study of stand-alone emollient use in mild to moderately severe atopic dermatitis flares. J Eur Acad Dermatol Venereol. 2014; 28:Suppl 3. 9–15.

5. Kim KH, Lee WR, An HJ, Kim JY, Chung H, Han SM, et al. Bee venom ameliorates compound 48/80-induced atopic dermatitis-related symptoms. Int J Clin Exp Pathol. 2013; 6:2896–2903.
6. Homey B, Steinhoff M, Ruzicka T, Leung DY. Cytokines and chemokines orchestrate atopic skin inflammation. J Allergy Clin Immunol. 2006; 118:178–189.

7. Zollner TM, Wichelhaus TA, Hartung A, Von Mallinckrodt C, Wagner TO, Brade V, et al. Colonization with superantigen-producing Staphylococcus aureus is associated with increased severity of atopic dermatitis. Clin Exp Allergy. 2000; 30:994–1000.

8. Breuer K, HAussler S, Kapp A, Werfel T. Staphylococcus aureus: colonizing features and influence of an antibacterial treatment in adults with atopic dermatitis. Br J Dermatol. 2002; 147:55–61.

9. Park HJ, Lee SH, Son DJ, Oh KW, Kim KH, Song HS, et al. Antiarthritic effect of bee venom: inhibition of inflammation mediator generation by suppression of NF-kappaB through interaction with the p50 subunit. Arthritis Rheum. 2004; 50:3504–3515.

10. Han S, Yeo J, Baek H, Lin SM, Meyer S, Molan P. Postantibiotic effect of purified melittin from honeybee (Apis mellifera) venom against Escherichia coli and Staphylococcus aureus. J Asian Nat Prod Res. 2009; 11:796–804.

11. Al-Ani I, Zimmermann S, Reichling J, Wink M. Pharmacological synergism of bee venom and melittin with antibiotics and plant secondary metabolites against multi-drug resistant microbial pathogens. Phytomedicine. 2015; 22:245–255.

12. Noh S, Jung JY, Park WS, Koh HJ, Lee KH. The steroid-sparing effect of an emollient APDDR-0801 in patients with atopic dermatitis. Korean J Dermatol. 2011; 49:227–233.
13. Park J, Lee KH, Kim JW, Ro YS, Park CW, Park WS, et al. The therapeutic efficacy of the moisturizer APDDR-0801 for patients with atopic dermatitis. Korean J Dermatol. 2010; 48:93–100.
14. Taïeb A. Hypothesis: from epidermal barrier dysfunction to atopic disorders. Contact Dermatitis. 1999; 41:177–180.

15. Elias PM. Therapeutic implications of a barrier-based pathogenesis of atopic dermatitis. Ann Dermatol. 2010; 22:245–254.

16. Park SB, Im M, Lee Y, Lee JH, Lim J, Park YH, et al. Effect of emollients containing vegetable-derived lactobacillus in the treatment of atopic dermatitis symptoms: split-body clinical trial. Ann Dermatol. 2014; 26:150–155.

17. Junghans V, Gutgesell C, Jung T, Neumann C. Epidermal cytokines IL-1beta, TNF-alpha, and IL-12 in patients with atopic dermatitis: response to application of house dust mite antigens. J Invest Dermatol. 1998; 111:1184–1188.

18. Cho SH, Strickland I, Boguniewicz M, Leung DY. Fibronectin and fibrinogen contribute to the enhanced binding of Staphylococcus aureus to atopic skin. J Allergy Clin Immunol. 2001; 108:269–274.

19. Zhou J, Zhao J, Zhang S, Shen J, Qi Y, Xue X, et al. Quantification of melittin and apamin in bee venom lyophilized powder from Apis mellifera by liquid chromatography-diode array detector-tandem mass spectrometry. Anal Biochem. 2010; 404:171–178.

20. Han S, Lee K, Yeo J, Kim W, Park K. Biological effects of treatment of an animal skin wound with honeybee (Apis mellifera. L) venom. J Plast Reconstr Aesthet Surg. 2011; 64:e67–e72.
21. Kim BY, Lee KS, Zou FM, Wan H, Choi YS, Yoon HJ, et al. Antimicrobial activity of a honeybee (Apis cerana) venom Kazal-type serine protease inhibitor. Toxicon. 2013; 76:110–117.

22. Han SM, Lee KG, Yeo JH. Dermal and ocular irritation studies of honeybee (Apis mellifera L.) venom. Korean J Pharmacogn. 2011; 42:76–81.
23. Bae JH, You SR, Kang MK, Lim GH, Lee WS. Final report: Cutaneous sensitization test of bee venom using guinea pig. Korean Res Inst Chem Technol Saf Res Cent. 2010; G09195:1–38.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download