INTRODUCTION
The term notalgia paresthetica (NP), derived from the Greek word 'notos' meaning 'back', was first introduced by Astwazaturow1 in 1934. It refers to an isolated mononeuropathy with chronic localized itch or paresthesia usually involving the skin over or near the scapula. There are no specific skin manifestations except for lesions, which are thought to be secondary to chronic scratching and rubbing. We describe here a case of NP in a 55-year-old woman. This is the first case report in Korea.
CASE REPORT
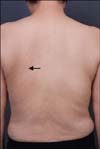
A 55-year-old woman visited our hospital complaining of tingling pain around the left inferior angle of the scapula. The patient reported pruritus, which had been ongoing for the last seven years, with a tingling pain that had developed four months ago. No other clinically relevant past medical history was described. Before visiting our clinic, the patient had undergone comprehensive neurological examinations at different hospitals including magnetic resonance imaging of the spine none of which revealed any significant abnormalities. We could not find any specific skin lesions except excoriation marks and vague hyperpigmentation (Fig. 1). A skin biopsy was performed on the back. Histopathologically, only epidermal thinning with slight pigmentary incontinence was detected (Fig. 2). S-100 protein immunostaining showed negative results. The patient was diagnosed as a case of NP based on her typical clinical features. She was treated with 600 mg of gabapentin daily, as well as capsaicin cream. Unfortunately, the response was deemed unsatisfactory.
DISCUSSION
NP is a neurocutaneous disorder that mainly affects mature and older adult subjects, and it is two-fold more frequent in women than in men2. The etiology of NP remains unknown although it is thought to be a neuropathic itch caused by sensory nerve entrapment involving the posterior rami of the T2 to T6 nerve root and is associated mainly with degenerative changes in the vertebrae. In a study of 12 cases2, the nine patients scanned using X-rays were found to have spinal disorders, including osteoarthritic lesions such as kyphosis, kyphoscoliosis, and vertebral hyperostosis. NP is usually diagnosed based on functional symptoms. Pruritus is the most common symptom and is intermittent, often paroxysmal, and of variable intensity. It can be accompanied by paresthesias such as pain, abnormal heating, burning or cold sensations, tingling sensations, numbness, and even foreign body sensations. This leads to chronic scratching and rubbing of the affected area that results in a secondary well-circumscribed hyperpigmented patch in the symptomatic area, resembling clinically macular amyloidosis2. Secondary to the functional signs, the diagnosis of NP can be made based on the specific area of the symptoms, i.e. T2 to T6 dermatomes, which correspond to the subscapular paravertebral region2. In most cases, NP is unilateral with either side being similarly affected. However, it is sometimes found to be bilateral or with an interscapular focus. Clinically, it is essential to rule out other pruritic disorders of the back such as pigmented contact dermatitis, patchy parapsoriasis, and neurodermatitis. The disorder most difficult to differentiate is early cutaneous amyloidosis, which localizes on the back even at the initial stage2. In such cases, the diagnosis is based on the course of the disease and the appearance of cutaneous lesions in other locations.
Our histological findings such as postinflammatory melanosis, which demonstrates as basal hyperpigmentation and pigmentary incontinence, were not much different from those previously reported2,3. In certain cases, dermal amyloidosis is described. This is suggested to be the result of irritation since prolonged friction can degenerate keratinocytes and subsequently degrade keratin into amyloid. Epidermal proliferation, as seen in lichen simplex chronicus, can be usually expected in the area of the lesion where pruritus and chronic rubbing persist. However, the opposite, i.e. epidermal thinning, was demonstrated in our patient. One possible explanation for this may be the prolonged use of over-the counter topical corticosteroids on the itching site. This may also have led to the attenuated hyperpigmentation at the symptomatic site.
Springall et al.4 previously described an increase in sensory epidermal innervation in the affected skin areas of NP, which could contribute to the symptoms. They found that frozen sections from the affected areas had a significant increase in the number of intradermal protein gene product 9.5-immunoreactive nerve fibers as compared to unaffected areas from the same patients and normal controls. In a later study, Inaloz et al.5 demonstrated the significant increase in number of dermal nerves using the neural marker S-100. However, S-100 protein staining did not show neural proliferation in our case.
No definite treatments have been established for NP with most of those reported to date being anecdotal. Topical capsaicin is the most widely used medication among dermatologists. Transcutaneous electrical nerve stimulation, treatment with gabapentin, oxcarbazepine, and botulinum toxin, and exposure to narrow-band ultraviolet-B radiation have recently shown promising results6. However, in most cases, various treatment efforts have been disappointing. Our patient was also treated with a moderate dose of gabapentin and topical capsaicin; however, she did not show a satisfactory response. Non-dermatologic, non-invasive therapies for NP with associated spinal disease can also include spinal manipulation, physical therapy, massage, cervical traction, cervical muscle strengthening, and therapy with oral nonsteroidal anti-inflammatory drugs and muscle relaxants7. Collaborative multidisciplinary approaches by dermatologists, radiologists, orthopedic surgeons, and neurologists may be indicated for successful management of this condition.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download