Abstract
A wedge-shaped anterior hairline extension is a very rare skin manifestation usually associated with congenital anomalies including a Tessier number 10 cleft. Other associated conditions are the Tessier number 9 cleft, the Fraser syndrome, and the Manitoba oculotrichoanal syndrome (MOTA syndrome). The Tessier number 10 cleft features include a coloboma of the middle third of the upper eyelid, and an eyebrow divided into two portions. The medial eyebrow portion may be absent and the lateral portion is angulated vertically, joining the hairline of the scalp. This creates a wedge-shaped anterior hairline extension. Herein we report on a case of a wedge-shaped anterior hairline extension associated with the Tessier number 10 cleft.
The Tessier number 10 cleft is one of the rarest defects in the Tessier classification, characterized by a coloboma of the middle third of the upper eyelid, disruption of the middle eyebrow segment, and ipsilateral projection of the fronto-temopral hairline1. The exact rate of occurrence of atypical clefts including the number 10 cleft is unknown, but is estimated at 1.4~4.9 cases per 100,000 live births2,3. To the best of our knowledge, no case of the Tessier number 10 cleft has been reported in the domestic literature. Differential diagnoses include a Tessier number 9 cleft, Fraser syndrome, and Manitoba oculotrichoanal syndrome (MOTA syndrome); all of these can include a wedge-shaped anterior hairline extension. Because most patients with such congenital anomalies visit plastic or ophthalmologic clinics, dermatologists seldom experience such cases. Herein we report on a case of a wedge-shaped anterior hairline extension associated with the Tessier number 10 cleft.
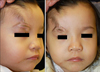
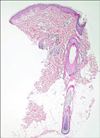
A 3-year-old girl presented with a wedge-shaped anterior hairline extension on the right forehead. This lesion had been present at birth and became larger in size in proportion to the infant's growth. The patient was born at the gestational age of 38 weeks. Her birth weight was 3,890 g. At that time, she had a coloboma of the middle third of the right upper eyelid. The defect of the eyelid was diagnosed as a Tessier number 10 cleft after visiting the department of plastic surgery. Ophthalmologic examination revealed she had normal visual acuity and a clear cornea. Pediatric evaluation indicated that her intelligence and development were normal, and that there were no abnormalities in her internal organs including the heart, kidney, vertebrae, and anorectal system. There was no family history of congenital anomalies, and her parents had normal appearance. She was an only child. Her mother stated that no medications had been taken during the pregnancy. The antenatal ultrasonography was reported to be normal. The Tessier number 10 cleft was reconstructed using semicircular rotational flap and Z-plasty at the age of 23 months. She was referred to the department of dermatology for the evaluation and treatment of the remaining aberrant hairline extension. There was a localized, wedge-shaped, skin-colored, and hairy patch in the temporal region pointing to the coloboma (Fig. 1). Histologic examination of the lesion from the forehead showed the increasing terminal hair follicles (Fig. 2). We planned to treat the aberrant hairline extension using laser devices such as intense pulsed light (IPL) or long-pulsed Nd:YAG laser.
Because of the rarity of craniofacial clefts, their classification is difficult. In 1976, Paul Tessier proposed a classification of craniofacial clefts using the orbit as a central hallmark that is now widely accepted4,5. Fifteen cleft locations (numbers 0~14) have been classified using the orbit as a central landmark.
The Tessier number 10 cleft is a rare congenital anomaly. Features include a coloboma of the middle third of the upper eyelid, an eyebrow divided into two portions, and a wedge-shaped anterior hairline extension. It may also be accompanied by other ocular anomalies, including orbital hypertelorism, symblepharon and corneal opacification. In the majority of reported patients, the cleft is limited to the soft tissue, with computed tomography (CT) images revealing an absence of bony clefts1. However, a central superior orbital cleft may sometimes be present, with the gap occupied by a fronto-orbital encephalocele4. CT imaging was not clinically indicated in our patient.
The etiology of craniofacial clefting is believed to be multifactorial. Genetics seems to play a minor role (other than for the Treacher Collins syndrome), with most craniofacial clefts, including the Tessier number 10 cleft, occurring sporadically4,6. A number of environmental factors have been associated with cleft development, including radiation, influenza A2, toxoplasmosis, maternal metabolic abnormalities (phenylketonuria), and drugs (such as isotretinoin, anticonvulsants, antimetabolic agents, alkylating agents, steroids, and tranquilizers)4. Amniotic bands are considered to be a likely cause of the cleft if the cleft is associated with the presence of a constriction ring. The patient in this case study was born following a normal pregnancy, with antenatal ultrasonography reported to be normal. There was no family history of congenital anomalies, and her mother denied taking medication during pregnancy. We believed our case to be an example of sporadic occurrence with no identified cause.
In addition to a Tessier number 10 cleft, a wedge-shaped anterior hairline extension is also associated with other congenital anomalies, including a Tessier number 9 cleft, Fraser syndrome and MOTA syndrome4,7,8. Unlike the Tessier number 10 cleft involving the middle third of the upper eyelid, Tessier number 9 clefts occur at the superolateral orbit, creating abnormalities of the lateral third of the upper eyelid and eyebrow. The lateral canthus is distorted and the superolateral orbital bone deficiency generates a lateral displacement of the globe. The temporal hairline projects anteriorly.
Fraser syndrome, an autosomal recessive condition characterized by the constellation of cryptophthalmos, syndactyly, laryngeal and oral clefting, genitourinary malformation, ambiguous genitalia, and mental retardation, is caused by mutations in the FRAS1 gene8,9. The phenotype overlap of Fraser syndrome, Tessier number 10 cleft, and MOTA syndrome, include ocular abnormalities, a wedge-shaped anterior hairline, and a notched nose. Unlike Fraser syndrome patients, the patient in this case did not have mental retardation, syndactyly or abnormal genitalia.
MOTA syndrome was initially described by Marles et al.7 in Aboriginal patients of the Island Lake region of Northern Manitoba, Canada. MOTA syndrome is so rare that only ten cases have been reported until now9-11. The pattern of inheritance is not clear but is thought to have an autosomal recessive basis. Molecular genetic testing is not available because the causative gene has not yet been isolated7. Recently, Slavotinek et al.11 reported that MOTA syndrome is caused by mutations in the FREM1 gene. Characteristic findings include eyelid colobomas, cryptopthalmos and anopthalmia/micropthalmia, an aberrant hairline, a bifid or broad nasal tip, and gastrointestinal anomalies such as omphalocele and anal stenosis11. Unlike MOTA syndrome, our patient did not have gastrointestinal anomalies or a family history of congenital anomaly. In addition, no case of MOTA syndrome occurring in the Asian region has been reported. However, because the omphalocele and anal anomalies are not a perquisite for diagnosis1, we could not exclude MOTA syndrome completely.
There is considerable phenotypic overlap between patients with MOTA syndrome and patients with the Tessier number 10 cleft. Yeung et al.1 suggested that Tessier number 10 clefts and MOTA syndrome result from a common defect in craniofacial development due to genetic factors, environmental insult, or a combination of genetic and environmental factors. Tessier's classification provides a purely anatomic description of the malformation and does not make reference to underlying etiologic mechanisms1. In other words, Tessier number 10 is a term commonly used by plastic surgeons, whereas MOTA syndrome is a term commonly used by geneticists. We suggest that, although the rarity of both entities makes the study difficult, further studies are necessary to establish the definite diagnosis of MOTA syndrome.
Eyelid colobomas are also seen in other syndromes, including Goldenhar syndrome (oculoauriculovertebral dysplasia), and Treacher Collins syndrome (mandibulofacial dysostosis)7,8,10. To the best of our knowledge, no Goldenhar or Treacher Collins syndrome patients have been reported with an accompanying wedge-shaped anterior hairline extension.
The treatment of a Tessier number 10 cleft mainly involves a combination of various surgical techniques, and a strategy must be created for each case. The basic principle in management is to reconstruct a cosmetically acceptable upper eyelid to provide corneal coverage. The concurrent aberrant wedge-shaped anterior hairline extension or absent eyebrow are also cosmetic concerns. Histologic examination of our patient showed that the aberrant hairline extension lesion consisted of terminal hair follicles and was not combined with nevus lesions. Therefore, the removal of the aberrant hairs can be accomplished using lasers, including a ruby laser, alexandrite laser, long pulsed Nd:Yag laser and IPL12. However, in cases involving both an aberrant hairline extension and absent eyebrow, a transposition flap using an aberrant hairline lesion can be used to reconstruct the absent eyebrow4. Thus, the eyebrow defect must be evaluated before removal of the aberrant hairline. In the present case, the patient's eyebrow defect had been previously repaired with plastic surgery, and no further management was required. Therefore, we devised a plan to treat the aberrant hairline extension using laser devices such as IPL or long-pulsed Nd:YAG laser.
Herein we describe an interesting and rare case presenting a wedge-shaped anterior hairline extension associated with a Tessier number 10 cleft. It is expected that dermatologists are aware that anterior hairline extension is usually associated with various congenital anomalies.
Figures and Tables
References
1. Yeung A, Amor D, Savarirayan R. Familial upper eyelid coloboma with ipsilateral anterior hairline abnormality: two new reports of MOTA syndrome. Am J Med Genet A. 2009. 149A:767–769.

2. Kawamoto HK Jr. The kaleidoscopic world of rare craniofacial clefts: order out of chaos (Tessier classification). Clin Plast Surg. 1976. 3:529–572.
3. Kawamoto HK Jr. McCarthey JG, editor. Rare craniofacial clefts. Plastic surgery. 4th ed. Philadelphia: WB Saunders;2922–2973.
4. Fan X, Shao C, Fu Y, Zhou H, Lin M, Zhu H. Surgical management and outcome of tessier number 10 clefts. Ophthalmology. 2008. 115:2290–2294.

5. Tessier P. Anatomical classification facial, cranio-facial and latero-facial clefts. J Maxillofac Surg. 1976. 4:69–92.
6. Langevin CJ, Gage E, Papay F. Siemionow MZ, Eisenmann-Klein M, editors. Craniofacial clefts and craniofacial syndromes. Plastic and reconstructive surgery. 2010. London: Springer-Verlag;253–264.

7. Marles SL, Greenberg CR, Persaud TV, Shuckett EP, Chudley AE. New familial syndrome of unilateral upper eyelid coloboma, aberrant anterior hairline pattern, and anal anomalies in Manitoba Indians. Am J Med Genet. 1992. 42:793–799.

8. Li C, Slavotinek A, Chudley AE. Pagon RA, Bird TD, Dolan CR, Stephens K, Adam MP, editors. Manitoba oculotrichoanal syndrome. GeneReviews. 1993. Seattle (WA): University of Washington.
9. Eskander BS, Shehata BM. Fraser syndrome: a new case report with review of the literature. Fetal Pediatr Pathol. 2008. 27:99–104.

10. Li C, Marles SL, Greenberg CR, Chodirker BN, van de Kamp J, Slavotinek A, et al. Manitoba oculotrichoanal (MOTA) syndrome: report of eight new cases. Am J Med Genet A. 2007. 143A:853–857.





 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download