1. Lin J, Gu Y. Preliminary investigation of nonsurgical treatment of severe skeletal Class III malocclusion in the permanent dentition. Angle Orthod. 2003. 73:401–410.
2. Guyer EC, Ellis EE 3rd, McNamara JA Jr, Behrents RG. Components of Class III malocclusion in juveniles and adolescents. Angle Orthod. 1986. 56:7–30.
3. Dietrich UC. Morphological variability of skeletal Class 3 relationships as revealed by cephalometric analysis. Rep Congr Eur Orthod Soc. 1970. 131–143.
4. Duan YZ, Yang ZH, Leng J. Effects of face mask/Class III elastic therapy on severe skeletal crossbite. J Modern Stomatol. 2003. 17:251–252.
5. Gu Y, Rabie AB, Hägg U. Treatment effects of simple fixed appliance and reverse headgear in correction of anterior crossbites. Am J Orthod Dentofacial Orthop. 2000. 117:691–699.

6. Uner O, Yüksel S, Uçüncü N. Long-term evaluation after chincap treatment. Eur J Orthod. 1995. 17:135–141.

7. Cha KS. Skeletal changes of maxillary protraction in patients exhibiting skeletal class III malocclusion: a comparison of three skeletal maturation groups. Angle Orthod. 2003. 73:26–35.
8. Tollaro I, Baccetti T, Franchi L. Craniofacial changes induced by early functional treatment of Class III malocclusion. Am J Orthod Dentofacial Orthop. 1996. 109:310–318.

9. Lin J, Gu Y. Lower second molar extraction in correction of severe skeletal Class III malocclusion. Angle Orthod. 2006. 76:217–225.
10. Sato S. Case report: developmental characterization of skeletal Class III malocclusion. Angle Orthod. 1994. 64:105–111.
11. Lew KK. Soft tissue profile changes following orthodontic treatment of Chinese adults with Class III malocclusion. Int J Adult Orthodon Orthognath Surg. 1990. 5:59–65.
12. Demir A, Uysal T, Sari Z, Basciftci FA. Effects of camouflage treatment on dentofacial structures in Class II division 1 mandibular retrognathic patients. Eur J Orthod. 2005. 27:524–531.

13. Nalbantgil D, Arun T, Sayinsu K, Fulya I. Skeletal, dental and soft-tissue changes induced by the Jasper Jumper appliance in late adolescence. Angle Orthod. 2005. 75:426–436.
14. Ning F, Duan Y, Huo N. Camouflage treatment in skeletal Class III cases combined with severe crowding by extraction of four premolars. Orthod Waves. 2009. 68:80–87.

15. Rabie AB, Wong RW, Min GU. Treatment in borderline Class III malocclusion: orthodontic camouflage (extraction) versus orthognathic surgery. Open Dent J. 2008. 2:38–48.

16. Cassidy DW Jr, Herbosa EG, Rotskoff KS, Johnston LE Jr. A comparison of surgery and orthodontics in "borderline" adults with Class II, division 1 malocclusions. Am J Orthod Dentofacial Orthop. 1993. 104:455–470.

17. Kerr WJ, Miller S, Dawber JE. Class III malocclusion: surgery or orthodontics? Br J Orthod. 1992. 19:21–24.

18. Zeng XL, Lin JX, Huang JF. Skeletal crossbite: surgery or orthodontics? West China J Stomatol. 1985. 3:233–237.
19. Stellzig-Eisenhauer A, Lux CJ, Schuster G. Treatment decision in adult patients with Class III malocclusion: orthodontic therapy or orthognathic surgery? Am J Orthod Dentofacial Orthop. 2002. 122:27–37.

20. Pellegrino G. Italian board of orthodontics: case N. 2 adult malocclusion. Prog Orthod. 2005. 6:102–112.
21. Fukui T, Tsuruta M. Invisible treatment of a Class III female adult patient with severe crowding and cross-bite. J Orthod. 2002. 29:267–275.

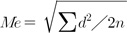 , where d represents the difference between two registrations and n is the number of duplicate registrations. The method error determined was 0.3 mm for linear measurement and 0.4° for angular measurement, which were both statistically insignificant (p ≥ 0.05).
, where d represents the difference between two registrations and n is the number of duplicate registrations. The method error determined was 0.3 mm for linear measurement and 0.4° for angular measurement, which were both statistically insignificant (p ≥ 0.05).



 PDF
PDF ePub
ePub Citation
Citation Print
Print





 XML Download
XML Download