Abstract
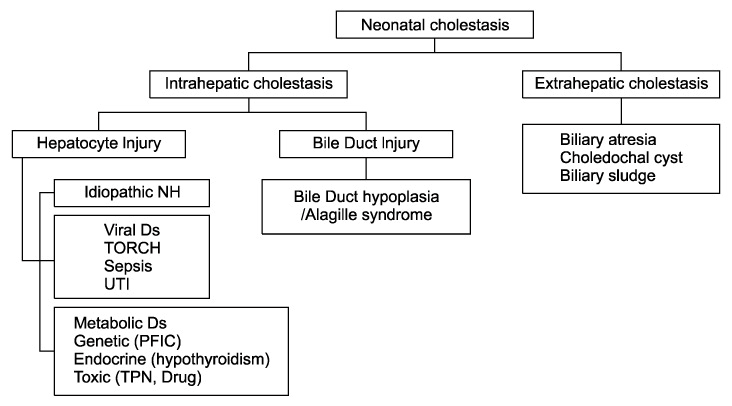
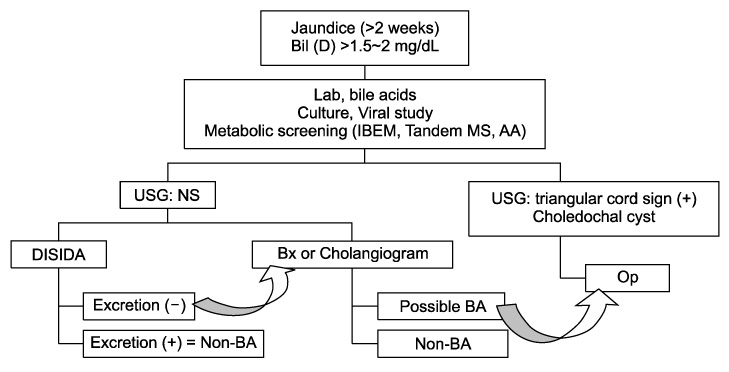
The persistence of jaundice beyond the first 2 weeks of life require further investigation and this can be determined if the conjugated bilirubin levels are greater than 1.5 mg/dL or greater than 20% of the total bilirubin level. There is a diverse differential diagnosis for the cause of neonatal cholestasis due to hepatobiliary disease including biliary atresia, which eventually leads to liver cirrhosis if uncorrected before 60~80 days of life. Long-established initial studies include abdominal ultrasonography, hepatobiliary scintigraphy and liver biopsy, but better diagnostic methods are needed. Promising new options are described including MRCP (magnetic resonance cholangiography), ERCP (endoscopic retrograde cholangiography), and PCC (percutaneous cholecysto-cholangiography). Though no single test can differentiate biliary atresia from other neonatal cholestasis with confidence, a combination of diagnostic methods is usually consistently beneficial. By excluding biliary atresia as early as possible, the risk of unnecessary explolaparotomy with intraoperative cholangiography is decreased. Further evaluation would be required for the diagnosis of neonatal cholestasis after excluding biliary atresia.
Go to : 
REFERENCES
1. Choe BH, Bezerra JA, Balistreri WF. Transplantation for cholestatic liver disease in the pediatric patient. In: Busuttil RW, Klintmalm GB, editors. Transplantation of the Liver. 2nd ed. Philadelphia: Elsevier Saunders; 2005. pp. 303-321.
2. Danks DM, Campbell PE, Smith AL, Rogers J. Prognosis of babies with neonatal hepatitis. Arch Dis Child. 1977; 52:368–372.

3. Mowat AP, Psacharopoulos HT, Williams R. Extrahepatic biliary atresia versus neonatal hepatitis. Review of 137 prospectively investigated infants. Arch Dis Child. 1976; 51:763–770.

4. Tazawa Y, Kobayashi K, Abukawa D, Nagata I, Maisawa S, Sumazaki R, et al. Clinical heterogeneity of neonatal intrahepatic cholestasis caused by citrin deficiency: case reports from 16 patients. Mol Genet Metab. 2004; 83:213–219.

5. Ko JS, Song JH, Park SS, Seo JK. Neonatal intrahepatic cholestasis caused by citrin deficiency in Korean infants. J Korean Med Sci. 2007; 22:952–956.

6. Alagille D, Estrada A, Hadchouel M, Gautier M, Odievre M, Dommergues JP. Syndromic paucity of interlobular bile ducts (Alagille syndrome or arteriohepatic dysplasia): review of 80 cases. J Pediatr. 1987; 110:195–200.

7. Deprettere A, Portmann B, Mowat AP. Syndromic paucity of the intrahepatic bile ducts: diagnostic difficulty; severe morbidity throughout early childhood. J Pediatr Gastroenterol Nutr. 1987; 6:865–871.
8. Oda T, Elkahloun AG, Pike BL, Okajima K, Krantz ID, Genin A, et al. Mutations in the human Jagged1 gene are responsible for Alagille syndrome. Nat Genet. 1997; 16:235–242.

9. Bates MD, Bucuvalas JC, Alonso MH, Ryckman FC. Biliary atresia: pathogenesis and treatment. Semin Liver Dis. 1998; 18:281–293.

10. Mieli-Vergani G, Howard ER, Portman B, Mowat AP. Late referral for biliary atresia--missed opportunities for effective surgery. Lancet. 1989; 1:421–423.
11. Grosfeld JL, Fitzgerald JF, Predaina R, West KW, Vane DW, Rescorla FJ. The efficacy of hepatoportoenterostomy in biliary atresia. Surgery. 1989; 106:692–700.
12. Volpert D, White F, Finegold MJ, Molleston J, Debaun M, Perlmutter DH. Outcome of early hepatic portoenterostomy for biliary atresia. J Pediatr Gastroenterol Nutr. 2001; 32:265–269.

13. Schoen BT, Lee H, Sullivan K, Ricketts RR. The Kasai portoenterostomy: when is it too late? J Pediatr Surg. 2001; 36:97–99.

14. Carceller A, Blanchard H, Alvarez F, St-Vil D, Bensoussan AL, Di Lorenzo M. Past and future of biliary atresia. J Pediatr Surg. 2000; 35:717–720.

15. Dolgin SE. Answered and unanswered controversies in the surgical management of extra hepatic biliary atresia. Pediatr Transplant. 2004; 8:628–631.

16. Maller ES. Liver function tests. In: Altschuler SM, Liacouras CA, editors. Clinical pediatric gastroenterology. 1st ed. Philadelphia: Churchill Livingstone; 1998. pp. 575-578.
17. Park WH, Choi SO, Lee HJ, Kim SP, Zeon SK, Lee SL. A new diagnostic approach to biliary atresia with emphasis on the ultrasonographic triangular cord sign: comparison of ultrasonography, hepatobiliary scintigraphy, and liver needle biopsy in the evaluation of infantile cholestasis. J Pediatr Surg. 1997; 32:1555–1559.

18. Park WH, Choi SO, Lee HJ. The ultrasonographic \'triangular cord\' coupled with gallbladder images in the diagnostic prediction of biliary atresia from infantile intrahepatic cholestasis. J Pediatr Surg. 1999; 34:1706–1710.

19. Park WH, Choi SO, Lee HJ. Technical innovation for noninvasive and early diagnosis of biliary atresia: the ultrasonographic \"triangular cord\" sign. J Hepatobiliary Pancreat Surg. 2001; 8:337–341.

20. Lee HJ, Lee SM, Park WH, Choi SO. Objective criteria of triangular cord sign in biliary atresia on US scans. Radiology. 2003; 229:395–400.

21. Kanegawa K, Akasaka Y, Kitamura E, Nishiyama S, Muraji T, Nishijima E, et al. Sonographic diagnosis of biliary atresia in pediatric patients using the \"triangular cord\" sign versus gallbladder length and contraction. AJR Am J Roentgenol. 2003; 181:1387–1390.

22. Tan Kendrick AP, Phua KB, Ooi BC, Subramaniam R, Tan CE, Goh AS. Making the diagnosis of biliary atresia using the triangular cord sign and gallbladder length. Pediatr Radiol. 2000; 30:69–73.

23. Kim JM, Choe BH, Jang YC, Oh KW, Cho MH, Lee KH, et al. Diagnostic limitation and usefulness of (99m)Tc-DISIDA hepatobiliary scanning on neonatal cholestasis. Korean J Pediatr. 2006; 49:737–744.
24. Norton KI, Glass RB, Kogan D, Lee JS, Emre S, Shneider BL. MR cholangiography in the evaluation of neonatal cholestasis: initial results. Radiology. 2002; 222:687–691.

25. Ryeom HK, Choe BH, Kim JY, Kwon S, Ko CW, Kim HM, et al. Biliary atresia: feasibility of mangafodipir trisodium-enhanced MR cholangiography for evaluation. Radiology. 2005; 235:250–258.

26. Ohnuma N, Takahashi T, Tanabe M, Yoshida H, Iwai J. The role of ERCP in biliary atresia. Gastrointest Endosc. 1997; 45:365–370.

27. Petersen C, Meier PN, Schneider A, Turowski C, Pfister ED, Manns MP, et al. Endoscopic retrograde cholangiopancreaticography prior to explorative laparotomy avoids unnecessary surgery in patients suspected for biliary atresia. J Hepatol. 2009; 51:1055–1060.

28. Shanmugam NP, Harrison PM, Devlin J, Peddu P, Knisely AS, Davenport M, et al. Selective use of endoscopic retrograde cholangiopancreatography in the diagnosis of biliary atresia in infants younger than 100 days. J Pediatr Gastroenterol Nutr. 2009; 49:435–441.

29. Hadzic N, Harrison PM. Selective rather than routine approach to endosopic retrograde cholangio-pancreatography in diagnosis of biliary atresia. J Hepatol. 2010; 52:777.

30. Shin KM, Ryeom HK, Choe BH, Kim KC, Kim JY, Lee JM, et al. Ultrasound-guided Percutaneous Cholecysto-Cholangiography for the Exclusion of Biliary Atresia in Infants. J Korean Radiol Soc. 2006; 55:177–182.

31. Nwomeh BC, Caniano DA, Hogan M. Definitive exclusion of biliary atresia in infants with cholestatic jaundice: the role of percutaneous cholecysto-cholangiography. Pediatr Surg Int. 2007; 23:845–849.

32. Lee SY, Kim GC, Jang YJ, Kim HJ, Ryeom HK, Choe BH, et al. The efficacy of ultrasound-guided percutaneous cholecysto-cholangiography for the early exclusion and type determination of biliary atresia. Radiology. 2011; (forthcoming).
33. Yamamoto H, Yoshida M, Ikeda S, Terakura H, Sera Y. Laparoscopic cholecystcholangiography in a patient with biliary atresia. Surg Laparosc Endosc. 1994; 4:370–372.

34. Hay SA, Soliman HE, Sherif HM, Abdelrahman AH, Kabesh AA, Hamza AF. Neonatal jaundice: the role of laparoscopy. J Pediatr Surg. 2000; 35:1706–1709.

35. Balistreri WF. Pediatric hepatology. A half-century of progress. Clin Liver Dis. 2000; 4:191–210.
36. Finegold MJ. Common diagnostic problems in pediatric liver pathology. Clin Liver Dis. 2002; 6:421–454.

37. Kahn E. Paucity of interlobular bile ducts. Arteriohepatic dysplasia and nonsyndromic duct paucity. Perspect Pediatr Pathol. 1991; 14:168–215.
38. Choe BH, Kim KM, Kwon S, Lee KS, Koo JH, Lee HM, et al. The pattern of differentially expressed genes in biliary atresia. J Korean Med Sci. 2003; 18:392–396.

Go to : 




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download