Abstract
Synovial fistula of the ankle joint is an uncommon complication from an ankle sprain. This may likely result in an unhealed wound around the ankle joint due to continuous leakage of joint fluid. However, in the event of an open wound on the lower leg, and not on the joint, it may be difficult to consider synovial fistula as a cause of the open wound. We experienced an interesting case with an unhealed open wound on the lower leg due to a synovial fistula of the ankle joint following an ankle sprain. We obtained good results after a treatment using a self-produced suction drainage device on the unhealed open wound.
Synovial fistula is an uncommon complication after trauma or surgery. Synovial fistula is well-recognized in knee surgery, particularly knee arthroscopic surgery,12) and some authors have reported synovial fistula as a complication after shoulder or wrist arthroscopy.34) However, little is known about synovial fistula of the ankle joint, and there is only one report on synovial fistula of the ankle joint in Korean literature.5)
Synovial fistula of the ankle joint can accompany a chronic open wound around lateral malleolus, and could be misdiagnosed as bursitis. However, when an open wound occurs on the lower leg, not around the joint, it is difficult to consider synovial fistula as a cause of the open wound, and deciding on an appropriate treatment method can be difficult.
We experienced the interesting case of a patient with an unhealed open wound on the lower leg due to a synovial fistula of the ankle joint following an ankle sprain. We obtained a good result after treatment using a self-produced suction drainage device on the unhealed open wound. The patient was informed that data regarding his case would be submitted for publication.
A 71-year-old male without underlying disease was referred to our hospital for evaluation of a chronically unhealed wound on the right mid-lower leg. The wound occurred after slipping two months ago and did not heal despite sutures three times at a local hospital. At the time of visiting our hospital, the wound was opened in the mid-portion and distal portion of the suture site and discharge was consistently drained (Fig. 1). No infectious signs such as swelling, redness, or heat sensation were observed around the open wound.
Radiographs of the tibia showed an osteolytic lesion in the midshaft of the tibia. The patient had a history of tibial shaft fracture and treatment using intramedullary nailing 30 years ago. We suspected chronic osteomyelitis and a three-phase bone scan was performed immediately. However, no osteomyelitis was observed and blood tests, including complete blood count, erythrocyte sedimentation rate, and C-reactive protein, were normal.
On more detailed history taking, the patient had a severe sprain of the right ankle, which had occurred three months ago, and a splint was applied for a month. Mild swelling was observed around the lateral malleolus of the right ankle joint. Arthrography and computed tomography arthrography were performed to confirm a synovial fistula of the ankle joint. Arthrography showed leakage of contrast media at the ankle joint and communication between the ankle joint and open wound (Fig. 2).
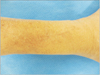
We diagnosed an unhealed wound due to a synovial fistula of the ankle joint and surgical treatment was performed. During surgery, clear fluid was observed and peroneal muscles were swollen because of leaked joint fluid (Fig. 3A). Wide debridement of swollen muscles was performed (Fig. 3B), and wound was sutured with insertion of a self-produced suction drainage device using syringe to prevent joint fluid filling (Fig. 4).
Postoperatively, a short leg splint was applied for four weeks and stitches with suction drainage device were removed at three weeks after surgery. At two-year after surgery, neither recurrence of the open wound nor synovial fistula was observed (Fig. 5).
This is an interesting case of development of an unhealed open wound after a laceration due to a synovial fistula of the ankle joint. Wound healing could be delayed in patients with poor vascularity, infection such as tuberculosis, or rheumatoid arthritis.6) A synovial fistula, a communication between a synovial or tenosynovial space and the skin, could also be a cause of delayed wound healing. It has been commonly reported in the knee following arthroscopy,12) and it is also known to occur in the shoulder after arthroscopy or rotator cuff repair.3) Development of a fistula occurs when excessive synovial fluid forces its way through the defect; the sinus track then allows joint fluid to squirt through the opening during joint motion and muscle contracture.7) However, information about synovial fistula of the ankle joint is limited, and, to the best of our knowledge, there is only one report on synovial fistula of the ankle joint following an ankle sprain in Korean literature.5)
Synovial fistula of the ankle joint could be misdiagnosed as bursitis, and misdiagnosis of a chronic open wound after surgery in association with a synovial fistula as bursitis is not uncommon. Therefore, suspicion of synovial fistula is important for proper diagnosis and treatment. However, when an open wound occurs on the lower leg, not around the joint, as in the current case, it is difficult to consider synovial fistula as a cause of the unhealed wound.
Magnetic resonance imaging (MRI) is an effective tool for diagnosis of a synovial fistula8); however, it is an indirect method for detection of a fistulous track with no fistula opening and is also an expensive method. The definitive diagnosis is visualizing the fistulous opening. Arthrography is a good tool for detection of a fistulous opening and is also very helpful in locating the fistulous track.9) It is also a simpler and less expensive method than MRI despite being more invasive. In the current case, arthrography was performed at the same time, and the communication between open wound and ankle joint as well as the fistulous opening was confirmed.
The general consensus regarding the method for treatment of a synovial fistula is immobilization and compression for one to two weeks.7) Surgical treatment is usually required for a fistula persisting beyond two weeks.7) Principle of surgical treatment is excision of the fistulous track and closure of the opening; however, a chronic, recurrent synovial fistula should require additional procedures, such as myofascial flap and periosteum augmentation.710) In the current case in which conservative treatment failed for two months, excision of the fistulous track and closure of the opening was essential; however, application of surgical trauma at the lateral malleolous area that does not have any external wound was a burden. Therefore, we used a self-produced suction drainage device using syringe for maintenance of negative pressure and obtained good results without recurrence at two years after surgery. However, we cannot assure closure of the fistula at the last follow-up because we did not perform direct closure of the opening and repeated arthrography. Furthermore, it is practically difficult to perform invasive test such as arthrography in patient without symptoms. We believe that the fistula could heal after using self-produced suction drainage device because high negative pressure enhance wound healing potential.11) Even if the fistula did not close after surgery, we believe that our treatment method has the meaning because of no recurrence at two years after surgery
The self-produced suction drainage device used in the current case has a similar function with Jackson-Pratt drain12) which is commonly called as hemovac drain. However, hemovac drain has low negative pressure because it was introduced by neurosurgeons and has been commonly used in brain surgery, breast surgery, and abdominal surgery.13) In these surgeries, high negative pressure is very dangerous because of occurrence of brain herniation, visceral wall necrosis, and perforation.13) Thus most closed vacuum drains have low negative pressure about 70~120 mmHg. In orthopedics, hemovac drain has been used to decrease local edema, lessen the potential for hematoma or seroma formation, and to aid in the efflux of infection although the evidence has not been firmly established.14) However, it is difficult to treat using conventional hemovac drain in case of wound with large continuous discharge and we have experienced several failures of treatment in these cases. Thus we used a self-produced suction drainage device using syringe for maintenance of negative pressure. Although there are no official data yet, our device has high negative pressure about 600~700 mmHg in preliminary experiment. However, data from official experiment and large clinical trial is needed to prove the function and usefulness of our device.
In the case of an unhealed wound that occurs at a non-joint location, it is difficult to suspect a synovial fistula as a cause of the unhealed wound. However, synovial fistula should be considered as a cause of the unhealed wound in patients with ankle sprain history and swelling in the ankle joint. In addition, application of continuous negative pressure could be a treatment method for a synovial fistula without direct surgical incision.
Figures and Tables
Figure 1
Preoperative photograph showed that the wound was opened in the mid-portion and distal portion of the suture site (arrows).
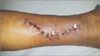
Figure 2
Arthrography showed leakage of contrast media in the ankle joint (A) and communication between open wound and ankle joint (B).
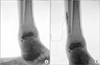
Figure 3
Intraoperative photographs showed clear fluid and swollen peroneal muscles (A) and debrided swollen muscles (B).

References
1. Díaz Heredia J, Ruiz Iban MA, Cuéllar Gutiérrez R, Ruiz Diaz R, Cebreiro Martinez del Val I, Turrion Merino L. Early postoperative transtibial articular fistula formation after anterior cruciate ligament reconstruction: a review of three cases. Arch Orthop Trauma Surg. 2014; 134:829–834.

2. Yiannakopoulos CK. Diagnosis and treatment of postarthroscopic synovial knee fistulae: a report of four cases and review of the literature. J Knee Surg. 2007; 20:34–38.

3. Richards RS, Curl LA, Moorman CT 3rd, Mallon WJ. Sterile synovio-cutaneous fistula: a potential complication of repair of large and massive rotator cuff tears. J Shoulder Elbow Surg. 2006; 15:436–439.

4. Shirley DS, Mullet H, Stanley JK. Extensor tendon sheath fistula formation as a complication of wrist arthroscopy. Arthroscopy. 2008; 24:1311–1312.

5. Lee WC, Kim JH, Song JK, Moon JS. Fistula of the ankle: a complication of ankle sprain. J Korean Foot Ankle Soc. 2002; 6:261–264.
6. Chen SH, Wang T, Lee CH. Tuberculous ankle versus pyogenic septic ankle arthritis: a retrospective comparison. Jpn J Infect Dis. 2011; 64:139–142.

7. Méndez-Fernández MA. Treatment of chronic recurrent synovial fistulae with myofascial flaps. Br J Plast Surg. 1993; 46:303–306.

8. Diduch DR, Lee GP, Barr M. Traumatic articular-bursal fistula in a collegiate football player. Arthroscopy. 2005; 21:1266.

9. Iveson JM, Hill AG, Wright V. Wrist cysts and fistulae. An arthrographic study of the rheumatoid wrist. Ann Rheum Dis. 1975; 34:388–394.

10. Hussein ElGhamry A. Peroneal tendofascial flap: a new fascial flap for Achilles tendon coverage, a preliminary report. Br J Plast Surg. 2003; 56:284–288.

11. Stannard JP, Volgas DA, Stewart R, McGwin G Jr, Alonso JE. Negative pressure wound therapy after severe open fractures: a prospective randomized study. J Orthop Trauma. 2009; 23:552–557.

12. Jackson FE, Pratt RA 3rd. Technical report: a silicone rubber suction drain for drainage of subdural hematomas. Surgery. 1971; 70:578–579.




 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download