Abstract
Microfracture as a reparative strategy is the treatment of choice for an osteochondral lesion of talus. Although the results of microfracture are generally excellent, at least 30% of patients who received microfracture have acute or chronic ankle pain with several or unknown causes. The most important factor for unsatisfactory outcome after microfracture is the size of the lesion. For failed osteochondral lesion of talus, the second options are autologous osteochondral graft, autologous chondrocyte implantation, or re-microfracture. In this article, we present the autologous chondrocyte implantation as a second procedure for failed microfracture and compare its clinical outcome with other methods based on a literature review.
Go to : 
REFERENCES
1.Berndt AL., Harty M. Transchondral fractures (osteochondritis dissecans) of the talus. J Bone Joint Surg Am. 1959. 41:988–1020.

2.Lee KT., Young KW., Lee YK., Park SY., Jang MS. Results in conservative treatment of osteochondral lesion of talus. J Korean Foot Ankle Soc. 2008. 12:145–9.
3.Anderson IF., Crichton KJ., Grattan-Smith T., Cooper RA., Brazier D. Osteochondral fractures of the dome of the talus. J Bone Joint Surg Am. 1989. 71:1143–52.

4.Lee KB., Bai LB., Yoon TR., Jung ST., Seon JK. Second-look ar-throscopic findings and clinical outcomes after microfracture for osteochondral lesions of the talus. Am J Sports Med. 2009. 37(Suppl 1):63S-70S.

5.Gobbi A., Francisco RA., Lubowitz JH., Allegra F., Canata G. Osteochondral lesions of the talus: randomized controlled trial comparing chondroplasty, microfracture, and osteochondral autograft transplantation. Arthroscopy. 2006. 22:1085–92.

6.Choi WJ., Park KK., Kim BS., Lee JW. Osteochondral lesion of the talus: is there a critical defect size for poor outcome? Am J Sports Med. 2009. 37:1974–80.
7.Savva N., Jabur M., Davies M., Saxby T. Osteochondral lesions of the talus: results of repeat arthroscopic debridement. Foot Ankle Int. 2007. 28:669–73.

8.Georgiannos D., Bisbinas I., Badekas A. Osteochondral transplantation of autologous graft for the treatment of osteochondral lesions of talus: 5- to 7-year follow-up. Knee Surg Sports Trau-matol Arthrosc. Published onlin October 19. 2014. DOI: doi: 10.1007/s00167-014-3389-3.
9.McGahan PJ., Pinney SJ. Current concept review: osteochondral lesions of the talus. Foot Ankle Int. 2010. 31:90–101.

10.Robinson P., White LM. Soft-tissue and osseous impingement syndromes of the ankle: role of imaging in diagnosis and man-agement. Radiographics. 2002. 22:1457–69. discussion 1470-1.

11.Hannon CP., Smyth NA., Murawski CD., Savage-Elliott I., Deyer TW., Calder JD, et al. Osteochondral lesions of the talus: aspects of current management. Bone Joint J. 2014. 96-B:164–71.
12.Loveday D., Clifton R., Robinson A. Interventions for treating osteochondral defects of the talus in adults. Cochrane Database Syst Rev. 2010. 8:CD008104.

13.Ogilvie-Harris DJ., Sarrosa EA. Arthroscopic treatment after previous failed open surgery for osteochondritis dissecans of the talus. Arthroscopy. 1999. 15:809–12.

14.Dragoni M., Bonasia DE., Amendola A. Osteochondral talar allograft for large osteochondral defects: technique tip. Foot Ankle Int. 2011. 32:910–6.

15.Yoon HS., Park YJ., Lee M., Choi WJ., Lee JW. Osteochondral autologous transplantation is superior to repeat arthroscopy for the treatment of osteochondral lesions of the talus after failed primary arthroscopic treatment. Am J Sports Med. 2014. 42:1896–903.

16.Lee KT., Kim JS., Young KW., Lee YK., Park YU., Kim YH, et al. The use of fibrin matrix-mixed gel-type autologous chondrocyte implantation in the treatment for osteochondral lesions of the talus. Knee Surg Sports Traumatol Arthrosc. 2013. 21:1251–60.

17.Kim YS., Park EH., Kim YC., Koh YG., Lee JW. Factors associated with the clinical outcomes of the osteochondral autograft transfer system in osteochondral lesions of the talus: second-look arthroscopic evaluation. Am J Sports Med. 2012. 40:2709–19.
18.Giannini S., Buda R., Ruffilli A., Cavallo M., Pagliazzi G., Bulzamini MC, et al. Arthroscopic autologous chondrocyte implantation in the ankle joint. Knee Surg Sports Traumatol Arthrosc. 2014. 22:1311–9.

Go to : 
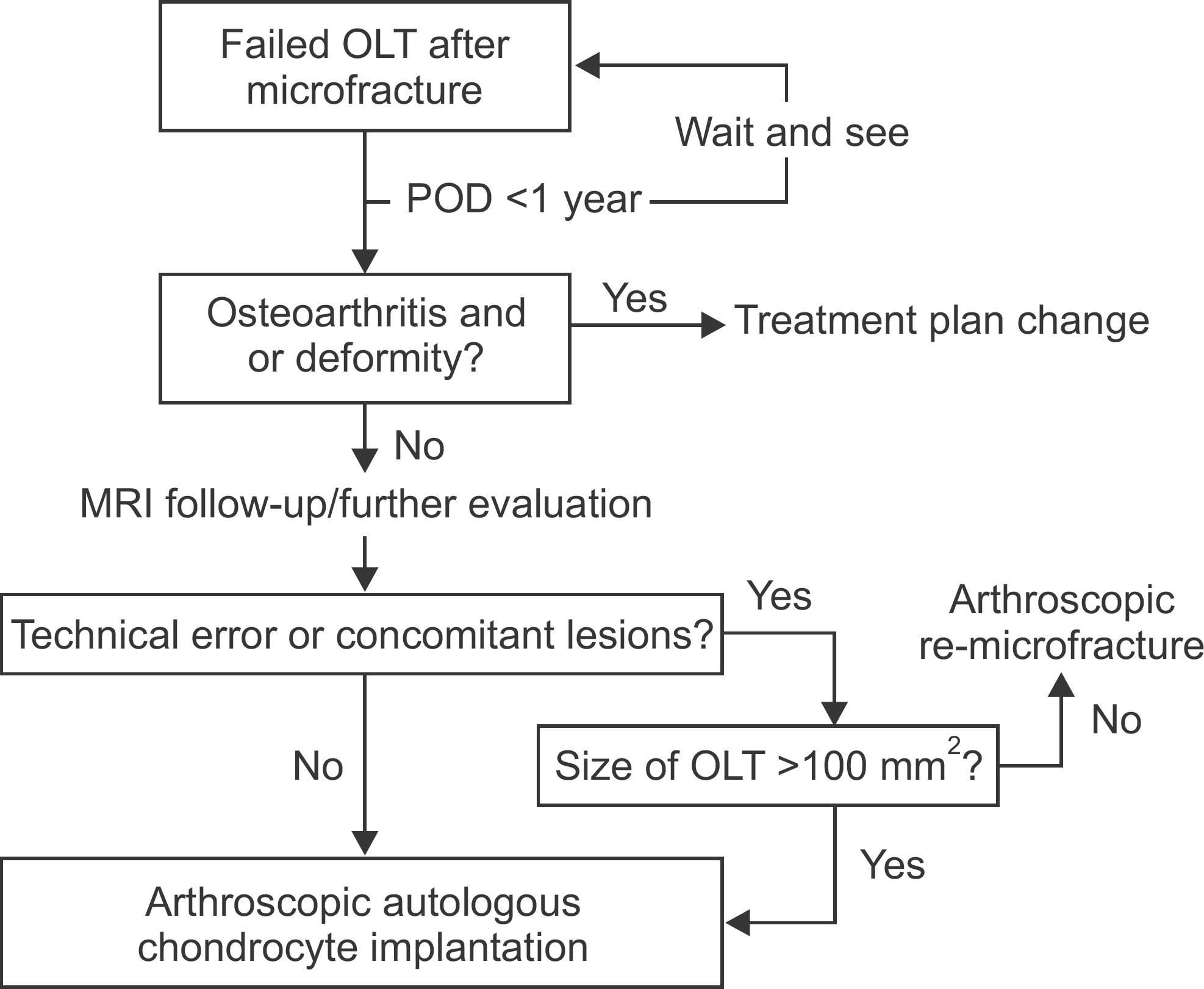 | Figure 1.Our flowchart for treatment of failed osteochondral lesion of talus. OLT: osteochondral lesion of talus, POD: postoperative days, MRI: magnetic resonance image. |
Table 1.
Simple Comparative Data between Several Procedures for Failed Osteochondral Lesion of Talus




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download