Abstract
The remnant cystic duct or gallbladder neck calculus may rarely result in post-cholecystectomy Mirizzi syndrome. Various managements have been proposed for the treatment of post-cholecystectomy Mirizzi syndrome. Some previous cases of post-cholecystectomy Mirizzi syndrome have been managed with open cholecystectomy and endoscopically. We report a case of a laparoscopic stone removal of post-cholecystectomy Mirizzi syndrome that developed 7 months after laparoscopic cholecystectomy. To our knowledge, this is the first case of laparoscopic management of post-cholecystectomy Mirizzi syndrome. The mechanism, diagnosis and treatment of post-cholecystectomy Mirizzi syndrome are discussed.
Mirizzi syndrome results from the impacted gallstone in the cystic duct or gallbladder neck.1 Although Mirizzi's syndrome bears Mirizzi's name, he was not the first to describe it. It was described by Kehr in 1905 and Ruge in 1908 as partial obstruction secondary to longstanding impacted stone and inflammation.1 The reported incidence of Mirizzi syndrome is 0.7-1.4% of all patients undergoing cholecystectomy.2 A remnant cystic duct stone causing post-cholecystectomy Mirizzi syndrome is very rare. Conventionally, management of the Mirizzi syndrome has been surgical; the type of laparoscopic or open procedure depending on the type of Mirizzi syndrome. Laparoscopic treatment of Mirizzi syndrome depends on the ability to delineate structures within Calot's triangle, which can be somewhat difficult due to severe adhesion and large stone or fistula, if present.3 We describe the treatment of a case of a cystic duct remnant calculus causing Mirizzi syndrome. To our knowledge, this is the first case of laparoscopic management of post-cholecystectomy Mirizzi syndrome.
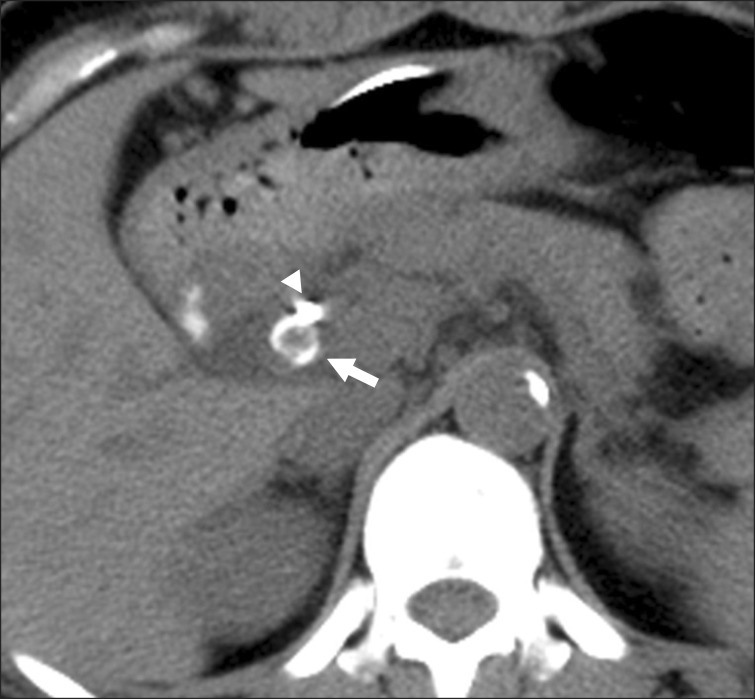
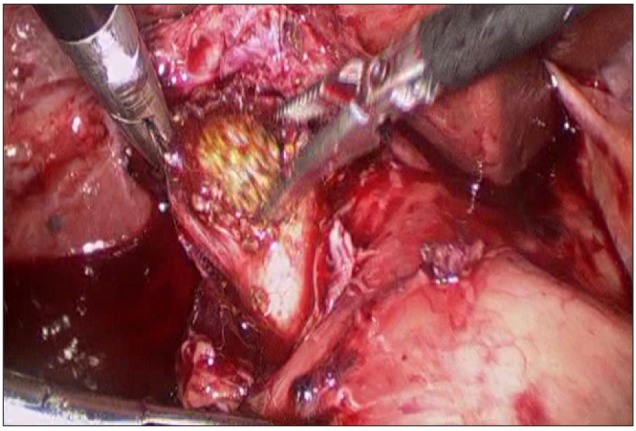
A 47-year-old woman presented recurrent epigatric pain, nausea and vomiting. There was no history of fever. She had undergone laparoscopic cholecystectomy for recurrent biliary pain 7 months before. At that time, preoperative ultrasonography (USG) had been performed only. On physical examination, the pulse rate was found to be 86 beats/min, temperature was 38.1℃, and blood pressure was 120/70 mmHg. She had an icteric sclera. Abdominal examination revealed that she was mild to moderate tender in the epigastrium, with no palpable mass. Laboratory studies revealed: alkaline phosphatase 817 IU/L (80-241), aspartate aminotransferase (AST) 188 IU/L (8-38), alanine aminotransferase (ALT) 232 IU/L (5-43), total bilirubin 4.3 mg/dl (0.2-1.2), direct bilirubin 2.9 mg/dl (0-0.4), serum albumin 3.5 g/dl (3.8-5.3), white blood cell 16.5×103/ul (4-10), hemoglobin 11.9 g/dl (12-16), polymorphonuclear neutrophils 91.4% (40-74), and prothrombin time of 0.96 INR (0.88-1.13). Regarding the raised bilirubin with altered liver function tests, imaging study such as USG and magnetic resonance cholangiopancreatography (MRCP) was performed to look for the cause of obstructive jaundice. On USG, intrahepatic bile ducts were dilated with dilatation of extrahepatic duct up to 1.1 cm. A 1.5 cm stone was seen in relation to the common bile duct. MRCP was performed for further characterization of the extrahepatic biliary tract anatomy. MRCP showed a long tortuous cystic lesion representing remnant cystic duct (Fig. 1). There was a 1.2 cm-length abrupt cut-off of the proximal cystic duct just after the cystic duct os, causing extrinsic compression of common hepatic duct level on an endoscopic retrograde cholangiopancreatography (ERCP) (Fig. 2). The cystic lesion, which showed dark signal intensity at all sequences, was highly suggestive of remnant cystic duct stone. The finding was compatible with a long tortuous remnant cystic duct with remnant duct stone causing extrinsic compression and obstruction of common duct, i.e. post-cholecystectomy Mirizzi syndrome. We could not ascertain definitely whether it was a case of residual or recurrent cystic duct stone, as no preoperative cholangiogram was done. However, in view of 7 months of asymptomatic period after cholecystectomy, we presumed residual stone as the cause of remnant cystic duct stone. ERCP was performed for a possible endoscopic therapeutic procedure, but failed. It confirmed the MRCP finding, there was no evidence of bilobillary fistula; type I Mirizzi syndrome. The ENBD was positioned into the proximal common hepatic duct (Fig. 2). The pre-enhanced CT showed a stone facing the endoscopic nasobiliary drainage (ENBD) tube (Fig. 3). Elective laparoscopic exploration of the remnant cystic duct and common bile duct was planned. Through the previous operation scar, 4 trochars were inserted. Fortunately, the adhesion was mild. We could get access to the common hepatic duct level. After removing the previous hemo-lock clips around the cystic duct, we tried to remove the stone, but failed. Therefore, we tried to incise the wall of the remnant cystic duct with a hook dissector, and we could remove the stone successfully (Fig. 4). After suturing the incised cystic duct with vicryl 3-0 interruptedly, operative cholangiography, via ENBD tube, was made. It did not show stenosis of the common bile duct and bile leakage (Fig. 5). A Jackson-Pratt drain was inserted into the subhepatic space. On postoperative 5 days, after clamping the ENBD tube, there was no post operative cystic duct bile leak. The patient made an uneventful recovery and has been symptom-free after 10 months of follow-up.
To avoid the common bile duct injury during laparoscopic cholecystectomy, it is recommended that dissection around Carlot's triangle should be kept close to the gallbladder, despite the potential risk of long cystic duct stump.4 The residual or recurrent impacted stone in the gallbladder neck or cystic duct may cause inflammatory reaction, resulting in common bile duct obstruction by extrinsic compression called Mirizzi syndrome.1 In this case, the short interval between laparoscopic cholecystectomy and readmission suggests that the calculus was retained rather than formed de novo. Post-cholecystectomy Mirizzi syndrome refers to a wide spectrum of conditions that often pose a diagnostic and therapeutic dilemma for the surgeon. Mc Sherry et al.5 in 1982 suggested a classification that includes type I, compression of the bile duct by a stone impacted in the cystic duct or Hartmann's pouch, and type II, characterized by cholecystobiliary fistula. Csendes et al.6 in 1989 subclassified cholecystobiliary fistula into three types according to the diameter of the fistula. A fistula occluding one-third of the duct is a Mirizzi type II, whereas occlusion of two-thirds of the duct or complete occlusion are classified as Mirizzi type III and IV, respectively.
Preoperative diagnosis is very important to avoid bile duct injury. Antoniou et al.7 reported that preoperative diagnosis of the Mirizzi syndrome seemed an important predicting factor of technical success. MRCP is the optimal method for evaluating the biliary anatomy, as it is non-invasive. Cystic duct stone causing extrinsic compression of the common duct can be very well seen in the axial MRCP images. ERCP has been the procedure of choice to confirm the diagnosis and to determine whether a fistula is present, and also has a therapeutic role, including stone retrieval and stent placement.8 At times, low inserting cystic duct may be mistaken for the common duct on ERCP, resulting in inadvertent placement of the stent into the adjacent duct than the intended one. Therefore, Wani et al.9 suggest that performing MRCP prior to ERCP is an important step to avoid a possible ERCP related complication.
The traditional treatment of Mirizzi syndrome is surgery. The surgical technique depends on the type of Mirizzi syndrome. Most authors agree that the surgery for type I Mirizz's syndrome involves a partial or total (open or laparoscopic) cholecystectomy, although some authors consider Mirizzi syndrome as a contraindication for laparoscopic cholecystectomy.7 The presence of common bile duct stones, fistula, or stricture at the site of impaction of the stone may necessitate a common bile duct exploration, and/or the insertion of a T-tube. However, endoscopic therapy has recently been used in the evaluation and treatment of patients with Mirizzi syndrome, mainly in types I and II.10 In the cases with type II-IV Mirizzi syndrome, who require more complex surgical techniques, T-tube insertion or bilioenteric anastomosis, especially Roux-en-Y hepaticojejunostomy following cholecystectomy, is a more preferable approach because of low morbidity and mortality rates.8
Some previous case reports of post-cholecystectomy Mirizzi syndrome were successfully treated via an open cholecystecomy and endoscopically.9 To our knowledge, this is the first case of laparoscopic management of post-cholecystectomy Mirizzi syndrome.
We conclude that the remnant cystic duct stone after cholecystectomy may cause post-cholecystectomy Mirizzi syndrome. Laparoscopic management is a safe and feasible alternative to open the surgery for post-cholecystectomy Mirizzi syndrome in the case of well selected patients.
References
1. Johnson LW, Sehon JK, Lee WC, et al. Mirizzi's syndrome: experience from a multi-institutional review. Am Surg. 2001; 67:11–14. PMID: 11206888.
3. Janes S, Berry L, Dijkstra B. Management of post cholecystectomy Mirizzi's syndrome. J Minim Access Surg. 2005; 1:34–36. PMID: 21234142.

4. Joo SH, Kim KH, Yun EJ, et al. Laparoscopic removal of a retained gallbladder with remnant cystic duct calculi. Korean J Hepatobiliary Pancreat Surg. 2006; 10:47–51.
5. McSherry CK, Ferstenberg H, Virship M. The Mirizzi syndrome: suggested classification and surgical therapy. Surg Gastroenterol. 1982; 1:219–225.
6. Csendes A, Díaz JC, Burdiles P, et al. Mirizzi syndrome and cholecystobiliary fistula: a unifying classification. Br J Surg. 1989; 76:1139–1143. PMID: 2597969.

7. Antoniou SA, Antoniou GA, Makridis C. Laparoscopic treatment of Mirizzi syndrome: a systematic review. Surg Endosc. 2010; 24:33–39. PMID: 19466486.

8. Yonetci N, Kutluana U, Yilmaz M, et al. The incidence of Mirizzi syndrome in patients undergoing endoscopic retrograde cholangiopancreatography. Hepatobiliary Pancreat Dis Int. 2008; 7:520–524. PMID: 18842500.
9. Wani NA, Khan NA, Shah AI, et al. Post-cholecystectomy Mirizzi's syndrome: magnetic resonance cholangiopancreatography demonstration. Saudi J Gastroenterol. 2010; 16:295–298. PMID: 20871198.

10. Mithani R, Schwesinger WH, Bingener J, et al. The Mirizzi syndrome: multidisciplinary management promotes optimal outcomes. J Gastrointest Surg. 2008; 12:1022–1028. PMID: 17874273.

Fig. 1
Coronal T2-weighted image shows a cystic duct stone representing as dark signal intensity round lesion (arrows) and shows remnant cystic duct appearing tubular hyperintense lesion (arrowhead).
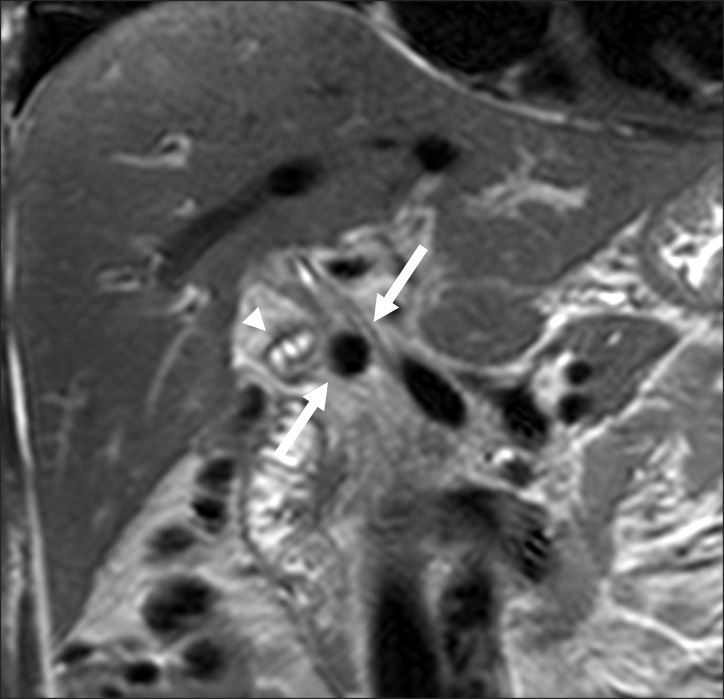
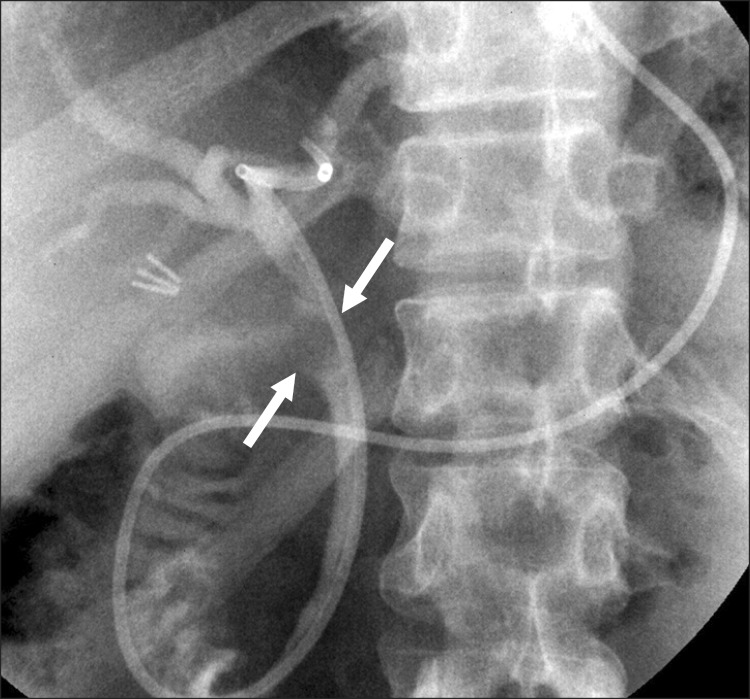
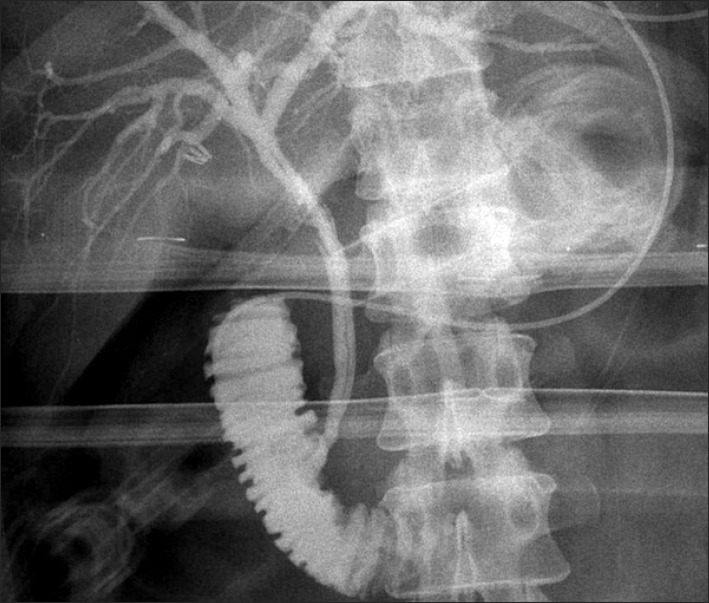
Fig. 2
An ovoid filling defect is noted in mid CBD level, which resulted in mild dilatation of above the common hepatic duct and intrahepatic bile ducts.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download