Abstract
Backgrounds/Aims
With recent advances in pancreatic surgery, pancreaticoduodenectomy (PD) has become increasingly safe. However, pancreatic leakage is still one of the leading postoperative complications. An accurate prediction model for pancreatic leakage after PD can be helpful for pancreas surgeons. The aim of this study was to provide a new model that was simple and useful with high accuracy for predicting pancreatic leakage after PD.
Methods
To predict the occurrence of pancreatic leakage, several factors were selected using bivariate analysis and univariate logistic regression analysis. The final model was developed using multivariable logistic regression analysis in the model construction data set.
Results
Overall, 41 of 100 patients had pancreatic leakage by the International Study Group on Pancreatic Fistula (ISGPF) criteria. Soft pancreatic parenchyma, small pancreatic duct diameter (≤3 mm), and combined resection of SMV and portal vein were independently predictive of pancreatic leakage. The risk score (R) for individual patients can be calculated by combining the 3 prognostic values with the regression test: R=0.5986+(0.5533×pancreatic parenchyma)+(0.5448×pancreatic duct diameter)+(0.8453×combined resection). The overall predictive accuracy of the model, as measured by the receiver operating characteristic (ROC) curve, was 0.728.
Go to : 
With recent advances in pancreatic surgery, pancreaticoduodenectomy (PD) in high-volume centers has become increasingly safe.1-4 However, the morbidity rate remains high, with complication rates remaining around 40%.1-4 In PD, pancreatic leakage is still one of the leading postoperative complications, often resulting in prolonged hospital stay and operative mortality.
In previous reports, some factors predictive of pancreatic leakage after PD, such as old age, anastomotic techniques, small pancreatic duct, and soft pancreatic texture, have been reported.5-10 However, no model has been developed to accurately predict pancreatic leakage after PD. An accurate prediction model for pancreatic leakage after PD can be helpful for pancreatic surgeons. Using the statistical methods that have been successful in predicting axillary node metastasis,11,12 we developed a method for predicting pancreatic leakage after PD. We chose the most objective definition of pancreatic leakage as defined by the International Study Group on Pancreatic Fistula (ISGPF).13
The aim of this study was to provide a new model that is simple and useful and has a high accuracy for predicting pancreatic leakage after PD.
Go to : 
Between January 2003 and June 2008, 140 patients with benign or malignant periampullary pathology underwent PDs at the Department of Surgery, Gangnam Severance Hospital, Yonsei University Health System, Seoul, Korea. Eleven patients were excluded because of incomplete clinicopathologic data or loss to follow up. As a result, 129 patients who underwent PD were retrospectively reviewed. This study was approved by the Institutional Review Board of Yonsei University for retrospective chart review and data collection.
In pylorus-preserving pancreaticoduodenectomy (PPPD), we removed the gallbladder, distal common bile duct, head of the pancreas, duodenum (except for the first portion), and 10-15 cm of the proximal jejunum. The proximal duodenum was carefully preserved 2-4 cm distal to the pylorus ring. The right gastric artery was divided along with the pyloric branch of the vagus nerve. Conventional PD was performed in the usual manner. All patients underwent dissection of the lymph nodes in the hepatoduodenal ligament, common hepatic artery, and celiac axis.
As a first step in reconstruction, the proximal jejunum was brought through the transverse mesocolon by the retrocolic route. Pancreaticojejunostomy was performed with a duct-to-mucosa anastomosis in all patients. The inner layer was a duct-to-mucosa with interrupted 5-0 prolene sutures and a short internal stent. The outer layer was a seromuscular envelope with interrupted 4-0 vicryl Lembert sutures. No pancreaticogastrostomies were performed. Hepaticojejunostomy was performed as end-to-side with single-layer interrupted sutures at 15 cm proximal to the pancreatojejunostomy. Duodenojejunostomy (or gastrojejunostomy) was constructed using a two-layer anastomosis by the antecolic route. A closed suction silicon drain (Jackson-Pratt, Baxter Health Care Corp.; Deerfield, IL) was placed in the patient from the right upper quadrant dorsal to the pancreatojejunal and the biliary anastomoses.
As a policy of our department, all patients received antacid drugs for stress ulcer prophylaxis, and octreotide (Sandostatin® 150 µg) was subcutaneously administered postoperatively for 7 days.
In all cases, the pancreatic duct diameter was measured after pancreatic transection by the operator. Fibrotic changes were assessed by trichrome staining. After staining, the texture of the pancreatic parenchyma was divided into two groups based upon the thickness of the fibrotic changes in the resection margin at a lower magnification (×40 magnification). Soft pancreatic parenchyma was characterized by the absence of fibrosis, or by a slightly thick layer of perilobular fibrosis (≤50 µm). Hard parenchyma was characterized by a layer of thick perilobular fibrosis of >50 µm.
A pancreatic fistula is defined by the output via an operative drain of drain fluid of any measurable volume on or after postoperative day 3, with an amylase content greater than 3 times the upper normal serum level (>300 IU/L) according to the ISGPF definition.13 All patients below this threshold were considered to have no fistula.
For model construction and validation, using 100 trials, the patients were randomly divided into 2 independent sets. The model set consisted of 100 patients. To predict occurrence of pancreatic leakage, several factors were selected using bivariate analysis and univariate logistic regression analysis; all measures of statistical significance were based on 0.05. The final model was developed using multivariable logistic regression analysis, and the calibration was assessed using the Akaika Information Criterion and c-statistics. Occurrence of pancreatic leakage was recorded as events and no leakage was recorded as non-events.
An independent validation set was used to validate the statistical model to predict pancreatic leakage. They included 19 men and 10 women, and their mean age was 57.8±12.7 years (range 28-81 years). The prevalence rate of pancreatic leakage was 44.8% (n=13). Validation was performed with calculation of the area under the receiver operating characteristic curves (AUC) after applying nomograms of the new model. For accuracy of the validation set, the same random sample selection method was carried out 5 times and generated 5 different validation sets, regardless of the independence of the model set. After verification of the similarity of the 5 sets, the original validation set including all patients was finally used. All the analyses used the SAS system 9.1.3 (SAS Institute Inc, Cary, North Carolina) AUC, and 95% confidence intervals (CI) were calculated using MedCalc (demo version).
Go to : 
A total of 100 patients who underwent PD or PPPD were selected for this study. The average age of patients was 61.1±11.5 years and consisted of 57 men and 43 women. Of the 100 patients, 31 underwent PD and 69 underwent PPPD. Pathologic diagnosis was pancreatic carcinoma in 31 patients, chronic pancreatitis in 2 patients, bile duct cancer in 38, ampulla of Vater cancer in 24, ampulla of Vater adenoma in 2 patients and duodenal carcinoma in 3. There were no the overall in-hospital mortality.
The average pancreatic duct diameter was 3.6±2.1 mm, 41 patients had normal pancreatic ducts (≤3 mm), and 59 had dilated pancreatic ducts (>3 mm). There were 24 patients (24%) with soft pancreatic texture and 76 patients (76%) with hard pancreatic texture.
Overall, 41 of 100 patients had pancreatic leakage by the ISGPF criteria13 for an overall incidence of 41%. 22 patients were grade A (22.0%), 18 were grade B (18.0%) and 2 were grade C (2.0%).
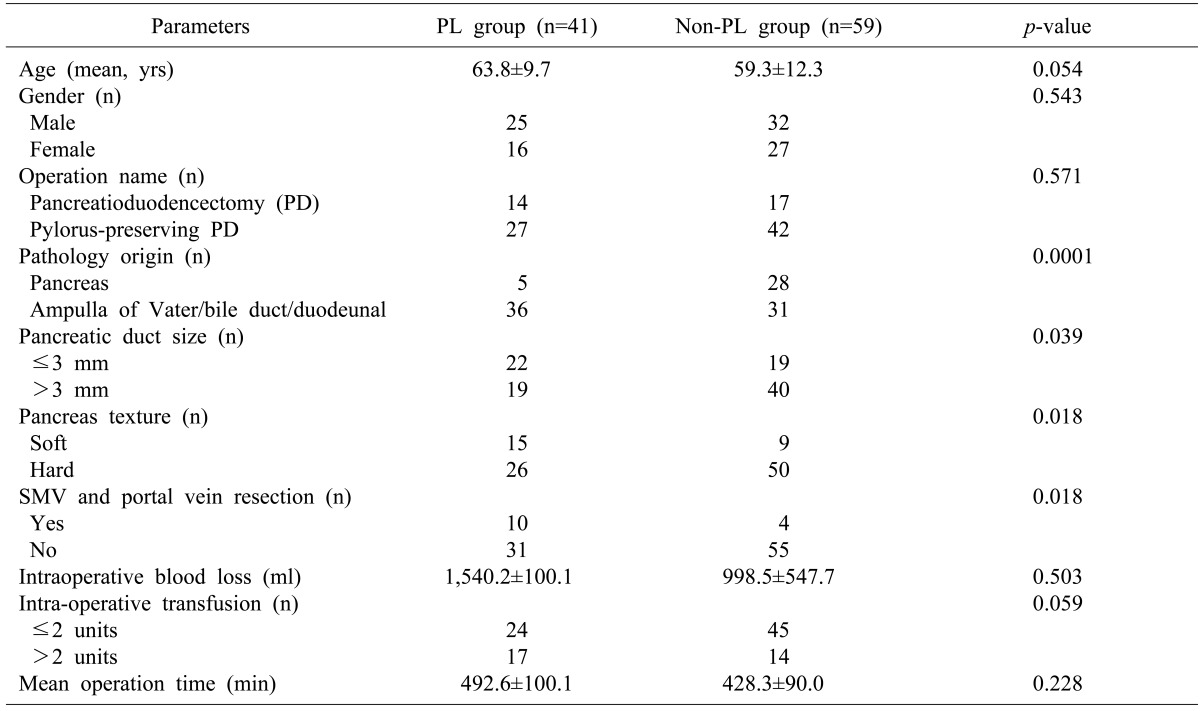
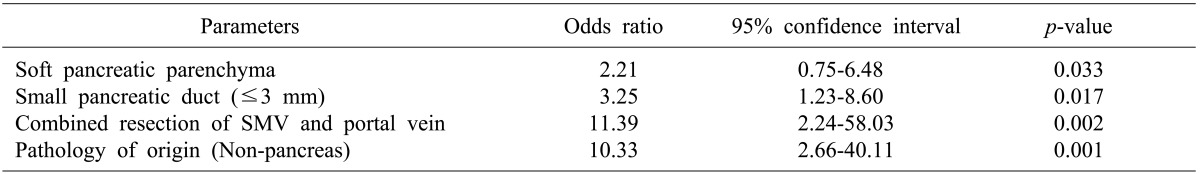
Pre- and intraoperative risk factors for pancreatic leakage were compared between patients with and without pancreatic leakage. The incidence of pancreatic leakage was significantly higher in the group with soft pancreatic parenchyma, small pancreatic duct diameter (≤3 mm), combined resection of the SMV and portal vein, and cancer of non pancreatic origin (bile duct, ampulla of Vater, duodenal) (Table 1). The candidate predictor variables were assessed using each univariate logistic analysis. In the multivariate analysis, soft pancreatic parenchyma, small pancreatic duct diameter (≤3 mm), pathology of non-pancreatic origin and combined resection of the SMV and portal vein were identified as independent factors for pancreatic leakage after PD (Table 2).
Soft pancreatic parenchyma increased the risk of pancreatic leakage by 3.02 times, small pancreatic duct diameter (≤3 mm) by 2.97 times, and combined resection of the SMV and portal vein by 5.42 times.
The risk score (R) for individual patients can be calculated by combining the 3 prognostic values with the regression test: R=0.5986+(0.5533×pancreatic parenchyma) +(0.5448×pancreatic duct diameter)+(0.8453×combined resection). The pancreatic parenchyma was coded as 0 for hard and 1 for soft. The pancreatic duct diameter was classified as 0 for large (>3 mm) and 1 for small (≤3 mm). Combined resection was coded as 0 for non resection of the SMV/portal vein and 1 for combined resection of the SMV and portal vein.
For example, for a hypothetical patient with a pancreatic duct diameter of 2 mm with soft pancreatic parenchyma and who did not have resection of the SMV, the risk score would be as follows: R=0.5986+(0.5533×1)+(0.5448×1)+(0.8453×0)=1.6967.
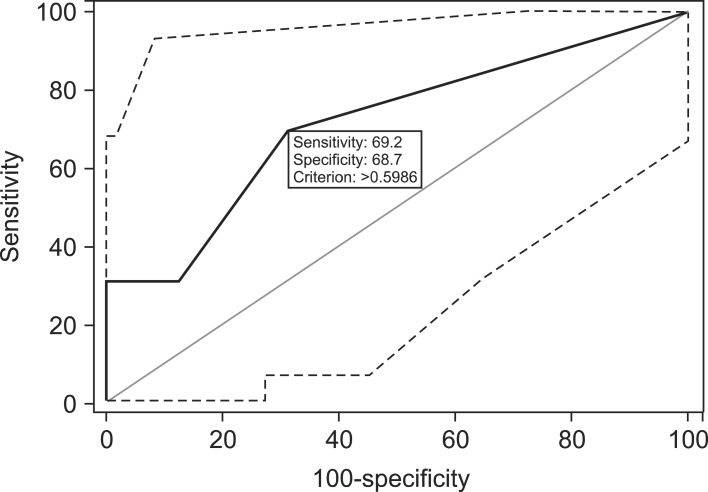
The overall predictive accuracy of the model as measured by the ROC curve was 0.728 (95% CI: 0.630 to 0.812).
To validate the model, we plotted the probabilities predicted by the observed proportions in 29 patients who underwent PD. C-statistics can be regarded as an extension of the AUC. The AUC for prediction of pancreatic leakage by the model was 0.714 (95% CI 0.517 to 0.865) (Fig. 1).
Go to : 
After PD, pancreatic leakage may occur in 5%-30% of patients. This wide range of occurrence in different studies could be partially explained by differences in the definition of pancreatic leakage.10,14-19 The variance obviously precludes accurate comparisons of surgical techniques and outcomes. To overcome this problem, the International Study Group of Pancreatic Surgery on Pancreatic fistula (ISGPF) suggested a universal and applicable definition of pancreatic leakage in 2005.13 The ISGPF definition of pancreatic leakage is very strict and objective criteria, which is why we chose it for this study.
Pancreatic leakage is a leading postoperative complication of PD, often resulting in prolonged hospital stay and operative mortality. Thus, it is important to be able to predict which patients are more likely to develop pancreatic leakage after PD. In previous reports, some factors predictive of pancreatic leakage after PD, including old age, anastomotic techniques, small pancreatic duct, and soft pancreatic texture, have been reported.5-10 We have shown that pancreatic duct size, texture of the remnant pancreatic parenchyma, and combined resection of the SMV were significantly associated with the risk of pancreatic leakage in the multivariate analysis. Although these predictive factors have been recognized, we think that they may not be independently but interdependently related to pancreatic leakage after PD.
In this study, we developed methods for predicting pancreatic leakage after PD. The model is a calculator program using pancreatic duct size, texture of the remnant pancreatic parenchyma, and concomitant surgery. The c-static for prediction of pancreatic leakage by our model was 0.728 (95% CI 0.630-0.812). The model was also validated in an independent set of patients and the c-static for prediction of pancreatic leakage was 0.714 (95% CI 0.517-0.865). Generally, an AUC>0.7 is considered a useful test result; we think that our model is an objective method for predicting pancreatic leakage after PD. Our model utilizes readily available clinical information and allows quick calculations to be made. It is a predictive instrument that can accurately identify high-risk patients for pancreatic leakage and could be used as a tool in the decision-making process.
There are some limitations of our model. First, it does no present varying degrees of clinical severity. In fact, grade A leakage is not significant because it may be clinically silent. Therefore, this model alone cannot predict the true clinical impact on patients. Second, our model is imperfect. It included sample sizes of less than 200 patients and had decreased predictive accuracy when applied to subjects. This failure may be due to the limited sample size. Large-scale evaluation of patients would provide a revised value of the parameter estimator. Finally, a potential weakness of our data is that all patients underwent the same pancreatic anastomosis technique performed by a single surgeon. Therefore, other pancreaticojejunostomy anastomosis techniques, such as pancreaticogastrostomy, dunking anastomosis, and pancreaticojejunal invagination were not included in our model. However, there is still no clear evidence for or against any type of anastomosis.
Nonetheless, the advantage of this model is that it is based on multivariable analysis, and is objective and the variables of pancreatic duct diameter, texture of pancreatic parenchyma, and combined resection of the SMV and portal vein are easily available. Before the model can be widely accepted, it will need to be validated by other investigators in independent groups of patients undergoing PD.
Although continued refinement and improvement of the model is needed, the present model may be useful for pancreatic surgeons in the prediction of pancreatic leakage after PD. We hope that other institutions will use our model using their databases, which will likely contain different patient characteristics, to validate its accuracy and to refine its ability.
Go to : 
References
1. Cameron JL, Pitt HA, Yeo CJ, et al. One hundred and forty-five consecutive pancreaticoduodenectomies without mortality. Ann Surg. 1993; 217:430–435. PMID: 8098202.

2. Gouma DJ, van Geenen RC, van Gulik TM, et al. Rates of complications and death after pancreaticoduodenectomy: risk factors and the impact of hospital volume. Ann Surg. 2000; 232:786–795. PMID: 11088073.

3. Trede M, Schwall G, Saeger HD. Survival after pancreatoduodenectomy. 118 consecutive resections without an operative mortality. Ann Surg. 1990; 211:447–458. PMID: 2322039.
4. Yeo CJ, Cameron JL, Sohn TA, et al. Six hundred fifty consecutive pancreaticoduodenectomies in the 1990s: pathology, complications, and outcomes. Ann Surg. 1997; 226:248–257. PMID: 9339931.
5. de Castro SM, Busch OR, van Gulik TM, et al. Incidence and management of pancreatic leakage after pancreatoduodenectomy. Br J Surg. 2005; 92:1117–1123. PMID: 15931656.

6. Hosotani R, Doi R, Imamura M. Duct-to-mucosa pancreaticojejunostomy reduces the risk of pancreatic leakage after pancreatoduodenectomy. World J Surg. 2002; 26:99–104. PMID: 11898041.

7. Lin JW, Cameron JL, Yeo CJ, et al. Risk factors and outcomes in postpancreaticoduodenectomy pancreaticocutaneous fistula. J Gastrointest Surg. 2004; 8:951–959. PMID: 15585382.

8. Miedema BW, Sarr MG, van Heerden JA, et al. Complications following pancreaticoduodenectomy. Current management. Arch Surg. 1992; 127:945–949. PMID: 1353671.
9. van Berge Henegouwen MI, De Wit LT, Van Gulik TM, et al. Incidence, risk factors, and treatment of pancreatic leakage after pancreaticoduodenectomy: drainage versus resection of the pancreatic remnant. J Am Coll Surg. 1997; 185:18–24. PMID: 9208956.

10. Yeo CJ, Cameron JL, Maher MM, et al. A prospective randomized trial of pancreaticogastrostomy versus pancreaticojejunostomy after pancreaticoduodenectomy. Ann Surg. 1995; 222:580–588. PMID: 7574936.

11. Katz A, Smith BL, Golshan M, et al. Nomogram for the prediction of having four or more involved nodes for sentinel lymph node-positive breast cancer. J Clin Oncol. 2008; 26:2093–2098. PMID: 18445838.

12. Soni NK, Carmalt HL, Gillett DJ, et al. Evaluation of a breast cancer nomogram for prediction of non-sentinel lymph node positivity. Eur J Surg Oncol. 2005; 31:958–964. PMID: 15979270.

13. Bassi C, Dervenis C, Butturini G, et al. International Study Group on Pancreatic Fistula Definition. Postoperative pancreatic fistula: an international study group (ISGPF) definition. Surgery. 2005; 138:8–13. PMID: 16003309.

14. Choi JJ, Choi H, Shin DS, et al. Risk factors for the pancreatic leakage after pancreaticoduodenectomy. Korean J Hepatobiliary Pancreat Surg. 2005; 9:225–232.
15. Büchler MW, Friess H, Wagner M, et al. Pancreatic fistula after pancreatic head resection. Br J Surg. 2000; 87:883–889. PMID: 10931023.

16. Conlon KC, Labow D, Leung D, et al. Prospective randomized clinical trial of the value of intraperitoneal drainage after pancreatic resection. Ann Surg. 2001; 234:487–493. PMID: 11573042.

17. Lowy AM, Lee JE, Pisters PW, et al. Prospective, randomized trial of octreotide to prevent pancreatic fistula after pancreaticoduodenectomy for malignant disease. Ann Surg. 1997; 226:632–641. PMID: 9389397.

18. Pederzoli P, Bassi C, Falconi M, et al. Italian Study Group. Efficacy of octreotide in the prevention of complications of elective pancreatic surgery. Br J Surg. 1994; 81:265–269. PMID: 8156354.
19. Suzuki Y, Kuroda Y, Morita A, et al. Fibrin glue sealing for the prevention of pancreatic fistulas following distal pancreatectomy. Arch Surg. 1995; 130:952–955. PMID: 7661678.

Go to : 




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download