Abstract
Objectives
To report the results and techniques of posterior vertebral column resections for fixed lumbosacral deformity.
Summary of Literature Review
Fixed lumbosacral deformity results in gross imbalance and progressive compensatory thoracolumbar deformity due to the absence of a mobile spine caudally.
Material and Methods
Twenty- five consecutive fixed lumbosacral deformity patients subjected to PVCR were reviewed after a minimum follow- up of 2 years. The offending vertebra was below the L4 in all cases. The etiological diagnoses were congenital scoliosis, congenital kyphoscoliosis, post-traumatic kyphosis and postinfectious kyphosis in 6, 3, 2 and 14 patients, respectively. The average age at the time of operation was 38 years, with a male:female ratio of 7:18. The indication for PVCR was fixed lumbosacral deformities that could not be brought to a reasonable balance on traction or forced side bending.
Results
On average 2.1, ranging from 1 to 5, vertebrae were removed, with 52 removed in all. The average fusion extent was 4.5 vertebrae, ranging from 2 to 8. A n anterior column reconstruction was carried out with an autogenous bone graft in all patients, with the additional insertion of titanium mesh in 12. The distal anchor went down to the L5, S1 and S2 in 4, 12 and 9 patients, respectively. A preoperative scoliosis of 3812 was corrected to 158 (60% correction), and a preoperative kyphosis of 3525 was corrected to - 511 (40% correction). A preoperative coronal imbalance of 2.0cm was improved to 0.9cm, and a preoperative sagittal imbalance of 9.3 cm was improved to 4.6 cm. The mean operation time and blood loss were 280 minutes and 2810ml, respectively. Following complications were encountered in 5 patients: 2 transient neurologies, 2 compression fractures at proximal adjacent vertebra and 1 pseudoarthrosis.
Conclusions
A posterior vertebral column resection is an effective procedure for the management of a fixed lumbosacral deformity. It provides satisfactory correction and improved functional outcomes. However, it is a technically demanding and exhausting procedure, with possible risks for complications
REFERENCES
1). Leong JC, Day GA, Luk KD, Freedman LS, Ho EK. Nine-year mean follow-up of one-stage anteroposterior excision of hemivertebrae in the lumbosacral spine. Spine. 1993; 18:2069–74.

2). Slabaugh PB, Winter RB, Lonstein JE, Moe JH. Lumbosacral hemivertebrae. A review of twenty-four patients, with excision in eight. Spine. 1980; 5:234–44.
3). Winter RB, Moe JH, Eilers VE. Congenital scoliosis. A study of 234 patients treated and untreated. J Bone Joint Surg [Am]. 1968; 50A:1–47.

5). Deviren V, Smith JA, Emami A, Hu SS, Bra dford DS. Management of fixed sagittal plane deformity: results of the transpedicular wedge resection osteotomy. Spine. 2001; 26:2036–43.
6). Bradford DS, Tribus CB. Vertebral column resection for the treatment of rigid coronal decompensation. Spine. 1997; 22:1590–9.

7). Suk SI, Kim JH, Lee SM, et al. Posterior vertebral colu mn resection for severe spinal deformities. J Kor Orthop Assoc. 2003; 38:72–78.
8). Suk SI, Kim JH, Kim WJ, et al. Treatment of fixed lumbosacral kyphosis by posterior vertebral column resection. J Kor Spine Surg. 1998; 5:307–313.
9). Fisk JR, Winter RB, Moe JH. The lumbosacral curve in idiopathic scoliosis. Its significance and management. J Bone Joint Surg [Am]. 1980; 62A:39–46.

11). Leatherman KD, Dickson RA. Two-stage corrective surgery for congenital deformities of the spine. J Bone Joint Surg [Br]. 1979; 61B:324–8.

12). Bradford DS, Boachie-Adjei O. One-stage anterior and posterior hemivertebral resection and arthrodesis for congenital scoliosis. J Bone Joint Surg [Am]. 1990; 72:536–40.

13). Smith-Peterson MN, Larson CB, Aufranc OE. Osteotomy of the spine for correction of flexion deformity in rheumatoid arthritis. J Bone Joint Surg [Am]. 1945; 27:1–11.
14). Heinig CF, Boyd BM. One stage vertebrectomy or eggshell procedure. orthopaedic transaction. J Bone Joint Surg [Am]. 1985; 9:130.
15). Thomasen E. Vertebral osteotomy for correction of k y p h osis in ankylosing spondylitis. Clin Orthop. 1985; 194:142–52.
16). Floman Y, Micheli LJ, Penny JN, Riseborough EJ, Hall JE. Combined anterior and posterior fusion in seven -ty-three spinally deformed patients: indications, results and complications. Clin Orthop. 1982; 164:110–22.
17). Kostuik JP, Maurais GR, Richardson WJ, Okajima Y. Combined single stage anterior and posterior osteotomy for correction of iatrogenic lumbar kyphosis. Spine. 1988; 13:257–66.
Fig. 1.
Case 6. 41-year-old female with lumbosacral scoliosis and L5 hemivertebra. (A) Preoperative anteroposterior radiograph shows lumbosacral scoliosis of 25° and proximal compensatory curve of 33°. (B) Preoperative lateral radiograph. (C) Preioerative tomograph shows L5 hemivertebra. (D) Postoperative anteroposterior radiograph. She was treated with posterior vertebral column resection of L5 with interbody cage. The lumbosacral scoliosis is corrected to 6° and proximal compensatory curve is corrected to 6°. The trunk is balanced post-operatively. (E) Postoperative lateral radiograph.
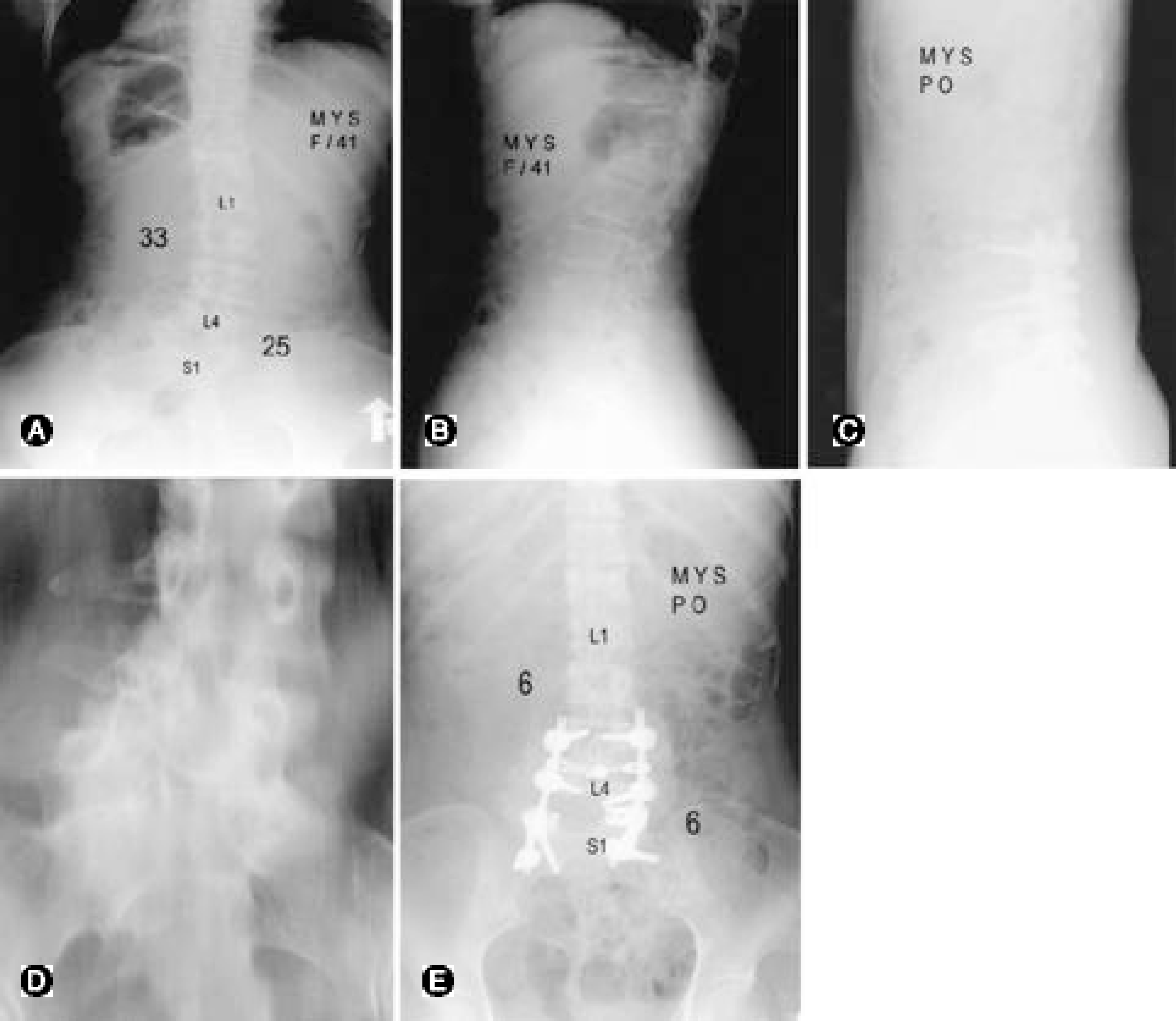
Fig. 2.
Case 25. 49-year-old female with post-infectious lumbosacral kyphosis.(A) Preoperative anteroposterior radi-ogra p hs.(B) Preoperative lateral radiograph shows lumbosacral kyphosis of 54° and sagittal imbalance of 10.5 cm.(C) Preoperative MRI shows neural compression at the apex of deformity.(D) Postoperative anteroposterior radiograph. (E) Postoperative lateral radiograph. She was treated with posterior vertebral column resection of L3,4,5 with interbody cage. The lumbosacral kyphosis is corrected to lordosis of 1°, and the trunk imbalance is corrected to 2.7 cm.
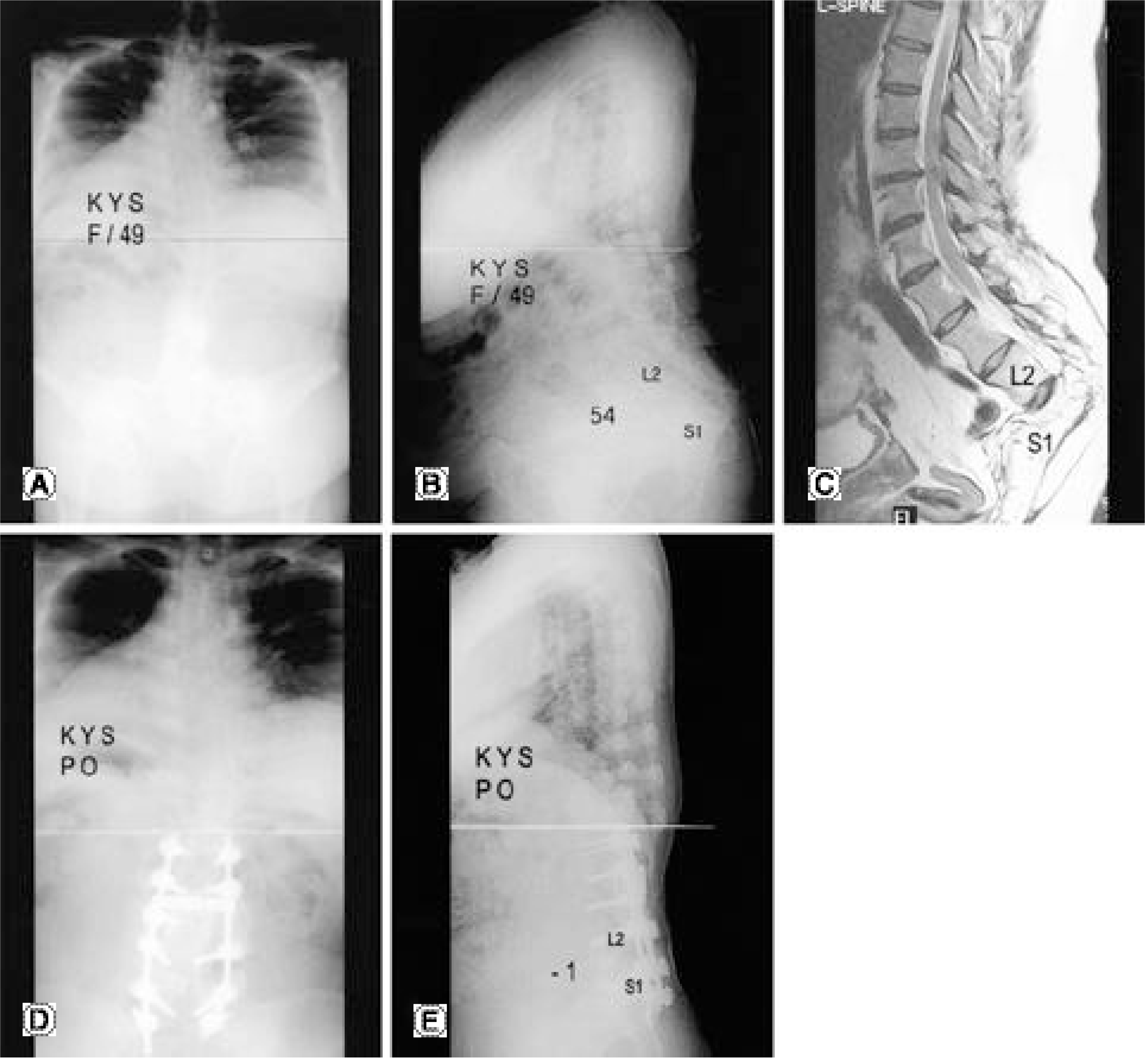
Table 1.
Patient characteristics and surgical outcome
| No | Sex | Age | Dx∗ | CP† | F/U(month) | Res. | No.of RV‡ | Ant.recons | Distal anchor | Cx∗∗ |
|---|---|---|---|---|---|---|---|---|---|---|
| 1 | M | 2.5 | CS | 76 | L4 | 1 | Chip bone | L5 | ||
| 2 | F | 34 | CS | P | 56 | L5 | 1 | Chip bone | S2 | |
| 3 | M | 9.9 | CS | 26 | L5 | 1 | Chip bone | S1 | ||
| 4 | M | 25 | CS | P | 26 | L56 | 2 | Mesh | S1 | |
| 5 | M | 8.9 | CS | 25 | L4 | 1 | Chip bone | L5 | ||
| 6 | F | 41 | CS | N, P | 24 | L5 | 1 | Mesh | S2 | |
| 7 | F | 35 | CKS | P | 52 | L5 | 1 | Chip bone | S2 | |
| 8 | F | 61 | CKS | N, P | 46 | L34 | 2 | Mesh | S2 | Comp fx |
| 9 | M | 16 | CKS | 28 | L4 | 1 | Mesh | L5 | ||
| 10 | F | 69 | PTK | P | 73 | L4 | 1 | Chip bone | S1 | |
| 11 | F | 61 | PTK | P | 29 | L4 | 1 | Chip bone | S1 | |
| 12 | F | 52 | PIK | N, P | 73 | L3 | 1 | Chip bone | L5 | |
| 13 | F | 36 | PIK | N | 71 | L1234 | 4 | Chip bone | S1 | TN |
| 14 | F | 37 | PIK | N, P | 70 | L1234 | 4 | Chip bone | S1 | |
| 15 | F | 44 | PIK | N, P | 69 | L234 | 3 | Chip bone | S1 | |
| 16 | M | 37 | PIK | P | 65 | L34 | 2 | Chip bone | S1 | |
| 17 | F | 38 | PIK | N, P | 65 | L12345 | 5 | Mesh | S2 | |
| 18 | F | 61 | PIK | N, P | 65 | L3 | 1 | Mesh | S1 | NU |
| 19 | F | 40 | PIK | P | 60 | L1234 | 4 | Mesh | S1 | |
| 20 | M | 61 | PIK | N, P | 58 | L5 | 1 | Mesh | S2 | TN |
| 21 | F | 40 | PIK | P | 57 | L345 | 3 | Mesh | S2 | |
| 22 | F | 60 | PIK | N, P | 49 | L45 | 2 | Mesh | S2 | Comp fx |
| 23 | F | 26 | PIK | P | 44 | L234 | 3 | Mesh | S1 | |
| 24 | F | 49 | PIK | N, P | 26 | L234 | 3 | Chip bone | S1 | |
| 25 | F | 49 | PIK | N, P | 25 | L345 | 3 | Mesh | S2 |
Table 2.
Coronal correction
| No | LS curve (°) | Compensatory curve (°) | Balance (cm) | |||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Pre | IMPO | Last | Net | Pre | IMPO | Last | Net | Pre | IMPO | Last | Net | |
| 1 | 26 | 4 | 3 | 23 | 8 | 1 | 2 | 6 | 1.0 | 0.2 | 0 | 1.0 |
| 2 | 37 | 16 | 18 | 19 | 40 | 15 | 23 | 17 | 3.5 | 1.6 | 2.3 | 1.2 |
| 3 | 40 | 14 | 16 | 24 | 7 | 4 | 4 | 3 | 1.5 | 0 | 0 | 1.5 |
| 4 | 29 | 8 | 10 | 19 | 40 | 14 | 15 | 25 | 3.5 | 1.2 | 1.2 | 2.3 |
| 5 | 35 | 12 | 12 | 23 | 8 | 6 | 3 | 5 | 0 | 0.2 | 0 | 0 |
| 6 | 25 | 6 | 6 | 19 | 33 | 8 | 6 | 27 | 1.2 | 0.5 | 0.6 | 0.6 |
| 7 | 37 | 18 | 18 | 19 | 47 | 30 | 33 | 14 | 6.0 | 2.8 | 3.0 | 3.0 |
| 8∗ | 56 | 21 | 25 | 31 | 26 | 7 | 6 | 20 | 0 | 0.2 | 1.2 | -1.2 |
| 9 | 57 | 30 | 28 | 29 | 28 | 8 | 14 | 14 | 1.0 | 0.1 | 0 | 1.0 |
| Pre = preoperative; IMPO = at 2 weeks after surgery; Last = at most recent follow-up; Net = Pre-Last. | ||||||||||||
Table 3.
Sagittal correction
| No | Regional kyphosis (°) | Thoracic kyphosis (°) | Lumbar lordosis (°) | Balance (cm) | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Pre | IMPO | Last | Net | Pre | IMPO | Last | Net | Pre | IMPO | Last | Net | Pre | IMPO | Last | Net | |
| 7 | 0 | -10 | -8 | 8 | 5 | 10 | 10 | 5 | -28 | -30 | -32 | 4 | 5.0 | 4.5 | 4.5 | 0.5 |
| 8∗ | 53 | -17 | -16 | 69 | 4 | 11 | 24 | 20 | 47 | -22 | -18 | 65 | 16.5 | 8.4 | 11.1 | 5.4 |
| 9 | 15 | -13 | -11 | 26 | 20 | 23 | 22 | 2 | -25 | -36 | -38 | 13 | 5.2 | 0.3 | 0 | 5.2 |
| 10 | 3 | -20 | -17 | 20 | 3 | 10 | 12 | 9 | -10 | -35 | -30 | 20 | 3.0 | 0.8 | 2.1 | 0.9 |
| 11 | 9 | -17 | -15 | 24 | 15 | 20 | 20 | 5 | -15 | -32 | -28 | 13 | 7.7 | 3.2 | 3.5 | 4.2 |
| 12 | 50 | 10 | 11 | 39 | -3 | 18 | 23 | 26 | 10 | -36 | -38 | 48 | 4.0 | 1.3 | 2.0 | 2.0 |
| 13 | 60 | 12 | 18 | 42 | -32 | -10 | -12 | 20 | 35 | -14 | -1 | 36 | 7.0 | 1.5 | 3.2 | 3.8 |
| 14 | 35 | -5 | -3 | 38 | -37 | -10 | -11 | 26 | 23 | -17 | -13 | 36 | 9.5 | 0.5 | 1.0 | 8.5 |
| 15 | 58 | -3 | -2 | 60 | -38 | -15 | -7 | 31 | 51 | -3 | 0 | 51 | 14.1 | 6.2 | 6.7 | 7.4 |
| 16 | 0 | -30 | -30 | 30 | -27 | -5 | 0 | 27 | -4 | -35 | -32 | 28 | 3.5 | -3.8 | 0.5 | 3.0 |
| 17 | 64 | -3 | -1 | 65 | -26 | 2 | 3 | 29 | 64 | -3 | -1 | 65 | 14.8 | 6.1 | 6.0 | 8.8 |
| 18† | 10 | 10 | 10 | 0 | -6 | 10 | 0 | 6 | -5 | -37 | -25 | 20 | 21.0 | 8.5 | 20.1 | 0.9 |
| 19 | 55 | -7 | -7 | 62 | -40 | -18 | 2 | 42 | 55 | -7 | -7 | 62 | 3.3 | -4.2 | -0.9 | 4.2 |
| 20 | 18 | 0 | 0 | 18 | 16 | 20 | 22 | 6 | -21 | -39 | -35 | 14 | 6.2 | 3.6 | 4.2 | 2.0 |
| 21 | 40 | -10 | -10 | 50 | -35 | -10 | -10 | 25 | 27 | -18 | -12 | 39 | 10.9 | 4.5 | 4.8 | 6.1 |
| 22∗ | 25 | -7 | -7 | 32 | -20 | 2 | -21 | -1 | 20 | -15 | 7 | 13 | 19.0 | 3.7 | 12.0 | 7.0 |
| 23 | 40 | -6 | -4 | 44 | -23 | 3 | 5 | 28 | 40 | -6 | -4 | 44 | 4.3 | 0 | 2.5 | 1.8 |
| 24 | 84 | 0 | 2 | 82 | -40 | 5 | 11 | 51 | 83 | -4 | -4 | 87 | 12.0 | 0 | 2.2 | 9.8 |
| 25 | 54 | -3 | -1 | 55 | -40 | -15 | -15 | 25 | 32 | -6 | -5 | 37 | 10.5 | 0.9 | 2.7 | 7.8 |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download