See the article "".
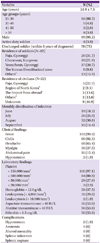
Kwak et al. [1] published an article entitled "Clinical Characteristics of Vivax Malaria and Analysis of Recurred Patients" in Infection and Chemotherapy in March 2013. This well-written report detailed the clinical characteristics of patients residing in a malaria-endemic area of Korea. However, a limited number of areas in Korea are considered malaria-endemic [2, 3, 4]. Vivax malaria also occurs outside northern Gyeonggi province, particularly as a relapse after Plasmodium protozoa infection [5]. Therefore, physicians outside this province should not dismiss malaria, particularly during the transmission season. In Korea, epidemiologic characteristics may differ between patients residing outside and inside northern Gyeonggi province. Therefore, the data presented by Kwak et al. [1] may not represent the typical clinical characteristics of vivax malaria in Korea. As a result, we performed this study to document the epidemiological characteristics of patients diagnosed with vivax malaria outside of northern Gyeonggi province. We retrospectively reviewed the medical records of patients at 2 university-affiliated hospitals located in non-endemic areas who had been diagnosed with vivax malaria using a peripheral blood smear between January 2001 and December 2012. A total of 104 patients were enrolled in our study. The mean patient age was 24.9 ± 7.5 years (range, 21-55 years), and 99 (95.2%) were male. Vivax malaria cases were most common in August (30.8%, 32/104) and July (25%, 26/104). The mean time between symptom onset and hospital visit was 9.0 ± 5.8 days (range, 0-40 days). Four patients (3.8%) were active service soldiers and 78 (75%) had been discharged from military service within 5 years of their diagnosis. These discharged soldiers developed symptoms an average of 6.4 months (range, 0-40 months) after discharge. All soldiers included in this study served in the malaria-endemic northern parts of Gyeonggi province in Korea (Fig. 1). No discharged soldiers had served in Jeolla province. Fever and chills were presented in 103 (99.0%) and 96 patients (92.3%), respectively. A total of 68 patients (65.4%) reported an accompanying headache. Of common vivax malaria complications, only hypotension was present in 2 patients (1.9%). A total of 101 patients (97.1%) had thrombocytopenia (< 150,000 cells/mm3); among them, 29 (27.9%) presented with moderate to severe cases (< 50,000 cells/mm3). Anemia (hemoglobin < 12 g/dL) was present in 39 patients (37.5%), and 56 patients (53.8%) had abnormal liver function tests (Table 1). During the study period, 4 patients (3.8%) experienced recurrent vivax malaria episodes. Most of our study patients were discharged soldiers, and the majority of these developed malaria within the 12 months after military discharge (93.6%, 73/78). In addition, most cases (97.1%, 101/104) occurred between May and October, peaking in July and August, similar to peaks reported by the majority of previous studies [1, 6]. The mean patient age was lower than in the endemic area reported by Kwak et al. [1], and almost all of our study patients were male.
In conclusion, most of the malaria cases occurred outside the northern part of Gyeonggi province; patients were mostly discharged soldiers in their mid-twenties; and the clinical characteristics, laboratory findings, recurrent rates, and complications associated with malaria were similar to those reported in an endemic area.
Figures and Tables
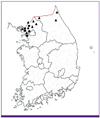 | Figure 1Distribution of study patient residences. Triangles indicate residences of patients in this study, and circles indicate residences of patients from the study by Kwak et al [1]. |
Acknowledgements
This study was supported in part by a 2013 Soongsan Fellowship from Wonkwang University.
References
1. Kwak YG, Lee HK, Kim M, Um TH, Cho CR. Clinical characteristics of vivax malaria and analysis of recurred patients. Infect Chemother. 2013; 45:69–75.

2. Yeom JS, Park JW. Status of vivax malaria after re-emergence in South Korea. Infect Chemother. 2008; 40:191–198.

3. Park JW, Klein TA, Lee HC, Pacha LA, Ryu SH, Yeom JS, Moon SH, Kim TS, Chai JY, Oh MD, Choe KW. Vivax malaria: a continuing health threat to the Republic of Korea. Am J Trop Med Hyg. 2003; 69:159–167.





 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download