Abstract
Background
With prolonged life expectancies, mental illness has emerged as a disabling disorder among people with HIV.
Materials and Methods
This study was conducted to assess the prevalence of depression and its risk factors among Korean patients with HIV infections. Eighty-two HIV-infected patients completed structured questionnaires including the Beck Depression Inventory and the State-Trait Anxiety Inventory. Subjects with depression were compared to those without depression in terms of demographics, comorbidities, CD4 T-cell count, RNA copy numbers, highly active antiretroviral therapy (HAART) regimens, and adherence.
Results
The estimated depression rate was 21% (17 of 82 subjects). Comorbidities (47% vs. 20%, P = 0.01) and unemployment (65% vs. 31%, P = 0.02) were risk factors for depression. Depressive patients were more likely to be anxious (71% vs. 29%, P < 0.01), to frequently miss clinical appointments each year (P = 0.04), and to have higher cumulative time lost to follow-up per month (P <0.01) compared to non-depressive patients. Only three depressive patients were referred to neuropsychologists.
Conclusions
More than 20% of the Korean HIV patients in this study suffered from depression associated with poor adherence. Considering the low level of recognition of depression by clinicians, risk factor-based active assessment is recommended to manage depression properly in HIV-infected patients.
In the era of highly active antiretroviral therapy (HAART), patients with human immunodeficiency virus (HIV) are experiencing longer life spans with delayed HIV disease progression. With prolonged life expectancies, the issue of mental illness has surfaced in relation to quality of life. Specifically, although there is significant variation based on study samples, geographic areas, and methods of measurement, depression is the most common mental illness in patients with HIV, affecting up to 50% of these patients [1-4]. However, data on Asian countries have been insufficient.
Depression has been linked to poor adherence, resulting in faster progression to acquired immune deficiency syndrome (AIDS) and higher mortality rates among HIV-infected patients [5, 6]. Adherence is recognized as an important factor in treatment for patients with HIV, with many studies showing that consistently high levels of adherence are necessary for reliable viral suppression and prevention of resistance [7, 8]. Depression-related poor adherence has also been reported for diverse other medical conditions including diabetes, cardiovascular diseases, malignancy, and renal failure [9, 10].
In this study, we assessed the prevalence of depression and its risk factors in Korean HIV-infected patients, along with the clinical impacts of depression on adherence and treatment outcomes.
Between September 2009 and February 2010, 82 Korean HIV-infected patients were recruited to the study from two university hospitals. Two trained monitors collected demographic, clinical, laboratory, and pharmacological data using structured case report forms that gathered information on age, sex, marital status, employment status, comorbidities, route of HIV transmission, opportunistic diseases, HAART regimens, duration of HAART treatment, and adherence to treatment. Unemployment was defined as a situation in which a subject of working age could not obtain a job but would like to be in full-time employment. Temporary employment was regarded as unemployment, while housewives were considered employed. Adherence to clinic visits was evaluated by reviews of electronic medical records that revealed the number of missed clinical appointments (per year) and the cumulative loss of time to follow-up (days per month). HAART was classified into three regimens: the boosted protease inhibitor (PI)-based regimen, the unboosted protease inhibitor (PI)-based regimen, and the non-nucleoside reverse transcriptase inhibitor (NNRTI)-based regimen. CD4 T-cell counts and HIV-1 RNA loads were serially recorded, with values noted at the time of HIV diagnosis, at the time of study entry (baseline), and 6 months (± 2 weeks) later.
The primary endpoint of the current study was to estimate the prevalence of depression and accompanying anxiety disorders among HIV-infected patients. In addition, subjects with depression were compared to those without depression with respect to demographics, comorbidities, CD4 T-cell count, RNA copy numbers, HAART regimen, and adherence.
This study was approved by the ethics committee of each involved institution (Korea University Guro Hospital and Inha University Hospital) and was conducted in accordance with the Declaration of Helsinki and Good Clinical Practice guidelines. All subjects provided written informed consent prior to enrollment.
Depression was measured using the Beck Depression Inventory (BDI), a 21-question multiple-choice self-report inventory. The BDI is one of the most commonly used instruments in research and practice to measure the presence and severity of depression [11,12]. We used cutoff scores as recommended by Han et al., which were based on data from a Korean sample, with scores of ≥21 indicating depression [12]. Anxiety symptoms were evaluated with the State-Trait Anxiety Inventory (STAI) developed by Spielberger et al. in 1970, which has been translated and standardized for use in Korea [13]. The STAI consists of two self-evaluation scales designed to separately assess state anxiety and trait anxiety. The state anxiety scale evaluates transitory state anxiety, in which unpleasant feelings, tension, and intensity vary according to the situation. The trait anxiety scale assesses a long-term personality characteristic. In this study, the state anxiety scale was evaluated and clinically significant levels of state anxiety were defined as scores ≥ 50. All patients filled out the questionnaires independently.
We conducted descriptive analyses and comparisons to examine the demographic and clinical characteristics of depressive patients. Data processing and evaluation were performed using SPSS 12.0 (SPSS Inc., Chicago, IL, USA). For categorical variables, analysis was performed using either the chi-square test or Fisher's exact test. Continuous variables were compared using the Student's t-test or Mann-Whitney U-test, as appropriate. All P-values were two-tailed, and P < 0.05 was considered to be statistically significant.
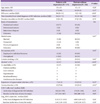
Among the 82 participants, the depression rate was 21% (17 of 82) with a median BDI score of 29 (26-31). The prevalence of anxiety disorders was 38% (31 among 82 subjects), and anxiety was more frequent in depressive patients compared to non-depressive patients (71% vs. 29%, P < 0.01) (Table 1). Comorbidities (47% vs. 20%, P = 0.01) and unemployment (65% vs. 31%, P = 0.02) were risk factors for depression. Regarding route of HIV transmission, non-depressive patients were more reluctant to disclose that information than depressive patients (52% vs. 18%). There were no significant differences in age, sex, smoking, alcohol, marital status, opportunistic infections, years since HIV diagnosis, duration of HAART treatment, CD4 T-cell count, and RNA copy numbers between depressive and non-depressive HIV patients.
Fourteen (82%) depressive and 51 (79%) non-depressive patients were treated with HAART (Table 2). While boosted protease inhibitor (PI)-based regimens (64%) were predominant among the depressive patients, NNRTI-based regimens were not prescribed for any of these patients. In comparison, boosted PI (39%), unboosted PI (24%), and non-nucleoside reverse transcriptase inhibitor (NNRTI)-based regimens (37%) were more evenly administered to non-depressive patients (P = 0.03). As for the clinical outcomes of HAART, virological (P = 0.74) and immunological (P = 0.67) responses were similar between depressive and non-depressive patients 24 weeks after entry into the study (Table 2). Although statistically insignificant, the rate of virological failure (viral load >50 copies/mL) was higher in depressive patients than in non-depressive patients (21% vs. 8%, P = 0.15). Moreover, depressive patients were more likely to miss clinical appointments (P = 0.04) compared with the non-depressive patients, with longer cumulative follow-up times (P < 0.01) (Table 2). Among the 17 depressive patients in the study, only three were referred to neuropsychologists and received anti-depressive agents.
In this study, the prevalence of depression in HIV-infected patients was 21%, comparable to previous reports for HIV-infected patients, which observed prevalence typically ranging from 20% to 36% [14]. The estimated rate of depression among HIV-infected patients was higher than that among the general population. A recent review indicates that the point prevalence of depression in the general Korean population ranges from 7.6% to 16.9% and increases with age [15]. In the present study, compared to non-depressive patients, depressive patients were more likely to have anxiety symptoms including fear, worry, insomnia, impaired concentration and memory, diminished appetite, ruminations, compulsive rituals, and avoidance of situations, thereby impairing quality of life.
Although depressive disorders are common among HIV-infected patients, they are frequently undetected. Clinicians may hesitate to ask patients about depression, while patients are reluctant to express their emotional stresses for fear of experiencing prejudice. In our sample, only three of 17 depressive patients were referred to a neuropsychiatric clinic and received antidepressants. Knowledge of predictive factors might assist clinicians to identify depressive patients; early recognition and management of depression may improve adherence to treatment regimens as well as quality of life. Some risk factors have previously been reported for depression in HIV-infected patients, including female gender, older age, unemployment, poor social support, and low CD4 T-cell count [2, 16-18]. However, according to a meta-analysis by Ciesla et al. [19], depression does not appear to be correlated with sexual orientation or stage of disease. Likewise, in the present study, CD4 T-cell count and RNA copy numbers were not associated with depression, whereas unemployment and underlying comorbidities were the risk factors for depression.
With respect to the type of HAART regimens used, while non-depressive patients were prescribed three kinds of regimen evenly, depressive patients were not prescribed NNRTI-based regimens. Clinicians might prefer to prescribe PI-based regimens after considering patients' characteristics due to concern for neuropsychiatric adverse events from NNRTIs. There was a chance that depressive patients did not report intolerability to their physicians despite poor adherence to PI-based regimens. Poor adherence has been shown to be related to the emergence of antiviral resistance, AIDS progression, and mortality [5, 7, 8].
This study has some limitations. First, it was cross-sectional in design. Second, the sample size was small and a matched HIV-negative control group was not included. Third, routes of HIV transmission were not identified in a large number of cases. More than 50% of non-depressive subjects refused to disclose transmission routes. Finally, other risk factors such as family history, substance abuse, and level of education were not included. In fact, however, all of the study subjects denied substance abuse, and none of those in this study reported becoming infected through intravenous drug use.
In conclusion, we found that the prevalence of depression was relatively high in HIV-infected patients and that the condition was associated with poor adherence. Considering the low recognition level of depression by clinicians, risk factor-based active assessments are recommended for the proper management of depression in HIV-infected patients.
Figures and Tables
Table 1
Clinical and epidemiological characteristics of depressive and non-depressive HIV-infected patients
Acknowledgements
This research was supported by the Korean Society for AIDS and a grant by the Chronic Infectious Disease Cohort (4800-4859-304) from the Korea Centers for Disease Control and Prevention.
References
1. Berger-Greenstein JA, Cuevas CA, Brady SM, Trezza G, Richardson MA, Keane TM. Major depression in patients with HIV/AIDS and substance abuse. AIDS Patient Care STDS. 2007. 21:942–955.

2. Kaharuza FM, Bunnell R, Moss S, Purcell DW, Bikaako-Kajura W, Wamai N, Downing R, Solberg P, Coutinho A, Mermin J. Depression and CD4 cell count among persons with HIV infection in Uganda. AIDS Behav. 2006. 10:4 Suppl. S105–S111.

3. Kelly B, Raphael B, Judd F, Perdices M, Kernutt G, Burrows GD, Burnett PC, Dunne M. Psychiatric disorder in HIV infection. Aust N Z J Psychiatry. 1998. 32:441–453.

4. Nakasujja N, Skolasky RL, Musisi S, Allebeck P, Robertson K, Ronald A, Katabira E, Clifford DB, Sacktor N. Depression symptoms and cognitive function among individuals with advanced HIV infection initiating HAART in Uganda. BMC Psychiatry. 2010. 10:44.

5. García de Olalla P, Knobel H, Carmona A, Guelar A, López-Colomés JL, Caylà JA. Impact of adherence and highly active antiretroviral therapy on survival in HIV-infected patients. J Acquir Immune Defic Syndr. 2002. 30:105–110.

6. Gonzalez JS, Batchelder AW, Psaros C, Safren SA. Depression and HIV/AIDS treatment nonadherence: a review and meta-analysis. J Acquir Immune Defic Syndr. 2011. 58:181–187.

7. Bangsberg DR. Less than 95% adherence to nonnucleoside reverse-transcriptase inhibitor therapy can lead to viral suppression. Clin Infect Dis. 2006. 43:939–941.

8. Bangsberg DR, Hecht FM, Charlebois ED, Zolopa AR, Holodniy M, Sheiner L, Bamberger JD, Chesney MA, Moss A. Adherence to protease inhibitors, HIV-1 viral load, and development of drug resistance in an indigent population. AIDS. 2000. 14:357–366.

9. DiMatteo MR, Lepper HS, Croghan TW. Depression is a risk factor for noncompliance with medical treatment: meta-analysis of the effects of anxiety and depression on patient adherence. Arch Intern Med. 2000. 160:2101–2107.

10. Osborn CY, Egede LE. The relationship between depressive symptoms and medication nonadherence in type 2 diabetes: the role of social support. Gen Hosp Psychiatry. 2012. 34:249–253.

11. Beck AT, Ward CH, Mendelson M, Mock J, Erbaugh J. An inventory for measuring depression. Arch Gen Psychiatry. 1961. 4:561–571.

12. Hahn HM, Yum TH, Shin YW, Kim KH, Yoon DJ, Chung KJ. A standardization study of beck depression inventory in Korea. J Korean Neuropsychiatric Assoc. 1986. 25:487–502.
13. Hahn DW, Lee CH, Chon KK. Korean adaptation of Spielberger's STAI (K-STAI). Korean J Health Psychol. 1996. 1:1–14.
15. Park JH, Kim KW. A review of the epidemiology of depression in Korea. J Korean Med Assoc. 2011. 54:362–369.

16. Adewuya AO, Afolabi MO, Ola BA, Ogundele OA, Ajibare AO, Oladipo BF, Fakande I. Relationship between depression and quality of life in persons with HIV infection in Nigeria. Int J Psychiatry Med. 2008. 38:43–51.

17. Judd F, Komiti A, Chua P, Mijch A, Hoy J, Grech P, Street A, Lloyd J, Williams B. Nature of depression in patients with HIV/AIDS. Aust N Z J Psychiatry. 2005. 39:826–832.





 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download