Abstract
Statement of problem
Flapless implant surgery using a soft tissue punch device requires a circumferential excision of the mucosa at the implant site. To date, Although there have been several reports on clinical outcomes of flapless implant surgeries, there are no published reports that address the appropriate size of the soft tissue punch for peri-implant tissue healing.
Purpose
In an attempt to help produce guidelines for the use of soft tissue punches, this animal study was undertaken to examine the effect of soft tissue punch size on the healing of peri-implant tissue in a canine mandible model.
Material and methods
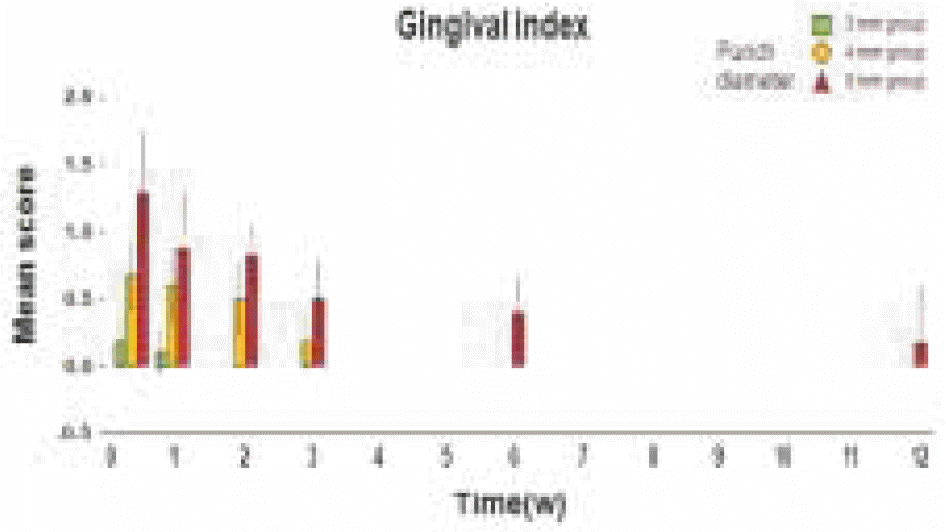
Bilateral, edentulated, flat alveolar ridges were created in the mandibles of six mongrel dogs. After a three month healing period, three fixtures (diameter, 4.0 mm) were placed on each side of the mandible using 3 mm, 4 mm, or 5 mm soft tissue punches. During subsequent healing periods, the peri-implant mucosa was evaluated using clinical, radiological, and histometric parameters, which included Gingival Index, bleeding on probing, probing pocket depth, marginal bone loss, and vertical dimension measurements of the peri-implant tissues.
Results
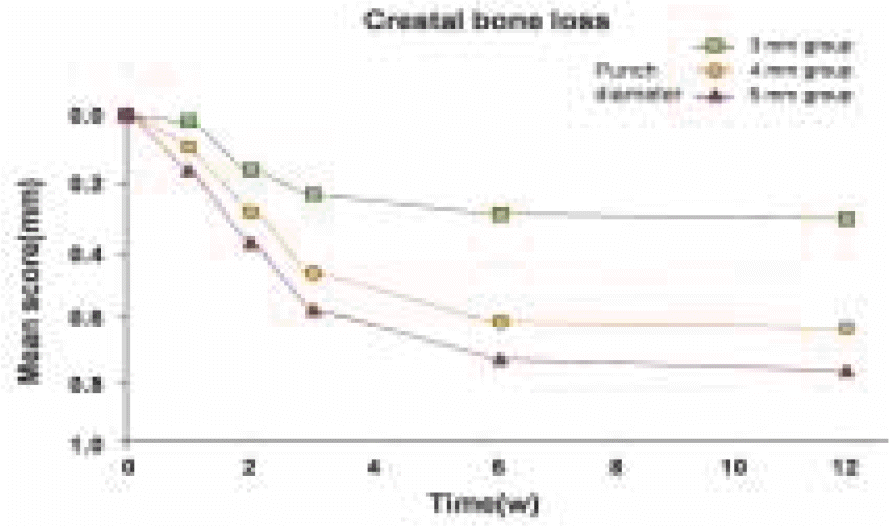
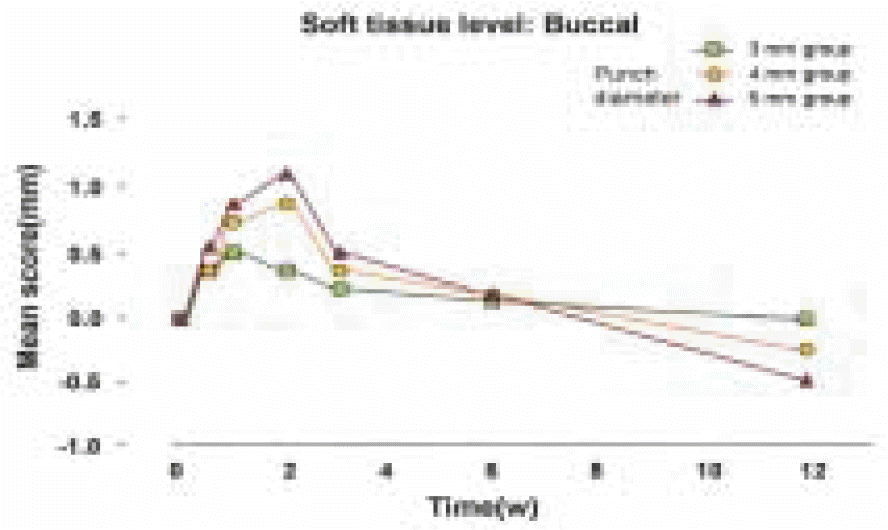
The results showed significant differences (P < 0.05) between the 3 mm, 4 mm and 5 mm tissue punch groups for the length of the junctional epithelium, probing depth, and marginal bone loss during healing periods after implant placement. When the mucosa was punched with a 3 mm tissue punch, the length of the junctional epithelium was shorter, the probing depth was shallower, and less crestal bone loss occurred than when using a tissue punch with a diameter ≥ 4 mm.
Conclusion
Within the limit of this study, the size of the soft tissue punch plays an important role in achieving optimal healing. Our findings support the use of tissue punch that 1 mm smaller than implant itself to obtain better peri-implant tissue healing around flapless implants. (J Korean Acad Prosthodont 2009;47:301-11)
Go to : 
REFERENCES
1.Belser UC., Buser D., Hess D., Schmid B., Bernard JP., Lang NP. Aesthetic implant restorations in partially edentulous patients—a critical appraisal. Periodontol 2000. 1998. 17:132–50.
2.Choquet V., Hermans M., Adriaenssens P., Daelemans P., Tarnow DP., Malevez C. Clinical and radiographic evaluation of the papilla level adjacent to single-tooth dental implants. A retrospective study in the maxillary anterior region. J Periodontol. 2001. 72:1364–71.

3.Grossberg DE. Interimplant papilla reconstruction: assessment of soft tissue changes and results of 12 consecutive cases. J Periodontol. 2001. 72:958–62.

4.Schroeder A., van der Zypen E., Stich H., Sutter F. The reactions of bone, connective tissue, and epithelium to endosteal implants with titanium-sprayed surfaces. J Maxillofac Surg. 1981. 9:15–25.

5.Buser D., Mericske-Stern R., Bernard JP., Behneke A., Behneke N., Hirt HP., Belser UC., Lang NP. Long-term evaluation of nonsubmerged ITI implants. Part 1: 8-year life table analysis of a prospective multi-center study with 2359 implants. Clin Oral Implants Res. 1997. 8:161–72.

6.Buser D., Mericske-Stern R., Dula K., Lang NP. Clinical experience with one-stage, nonsubmerged dental implants. Adv Dent Res. 1999. 13:153–61.

7.Buser D., Weber HP., Lang NP. Tissue integration of nonsubmerged implants. 1-year results of a prospective study with 100 ITI hollow-cylinder and hollow-screw implants. Clin Oral Implants Res. 1990. 1:33–40.
8.Weber HP., Buser D., Fiorellini JP., Williams RC. Radiographic evaluation of crestal bone levels adjacent to nonsubmerged titanium implants. Clin Oral Implants Res. 1992. 3:181–8.

9.Mericske-Stern R., SchaffnerT Steinlin., Marti P., Geering AH. Peri-implant mucosal aspects of ITI implants supporting overdentures. A five-year longitudinal study. Clin Oral Implants Res. 1994. 5:9–18.

10.Wismeyer D., van Waas MA., Vermeeren JI. Overdentures supported by ITI implants: a 6.5-year evaluation of patient satisfaction and prosthetic aftercare. Int J Oral Maxillofac Implants. 1995. 10:744–9.
11.Auty C., Siddiqui A. Punch technique for preservation of interdental papillae at nonsubmerged implant placement. Implant Dent. 1999. 8:160–6.

12.Salinas TJ. Soft tissue punch technique for aesthetic implant dentistry. Pract Periodontics Aesthet Dent. 1998. 10:434.
13.McGlumphy EA., Mendel DA., Holloway JA. Implant screw mechanics. Dent Clin North Am. 1998. 42:71–89.
14.Jemt T., Lekholm U., Gro ¨ndahl K. 3-year followup study of early single implant restorations ad modum Bra � nemark. Int J Periodontics Restorative Dent. 1990. 10:340–9.
15.Jemt T., Linde ´ n B., Lekholm U. Failures and complications in 127 consecutively placed fixed partial prostheses supported by Bra � nemark implants: from prosthetic treatment to first annual checkup. Int J Oral Maxillofac Implants. 1992. 7:40–4.
16.Saadoun AP. Single tooth implant restoration: surgical management for aesthetic results. Int J Dent Symp. 1995. 3:30–5.
17.Campelo LD., Camara JR. Flapless implant surgery: a 10-year clinical retrospective analysis. Int J Oral Maxillofac Implants. 2002. 17:271–6.
18.Zunino JH., Zunino D. Implant surgery: our experience in performing second stage surgery by a punch approach. J Oral Implantol. 1995. 21:148–9.
19.Kusek ER. Tissue-punch technique in nonattached tissue using the YSGG laser. Dent Today. 2009. 28(132):134–5.
20.Rocci A., Martignoni M., Gottlow J. Immediate loading in the maxilla using flapless surgery, implants placed in predetermined positions, and prefabricated provisional restorations: a retrospective 3-year clinical study. Clin Implant Dent Relat Res. 2003. 5:29–36.

21.Lorenzoni M., Pertl C., Zhang K., Wimmer G., Wegscheider WA. Immediate loading of single-tooth implants in the anterior maxilla. Preliminary results after one year. Clin Oral Implants Res. 2003. 14:180–7.

22.Andersen E., Haanaes HR., Knutsen BM. Immediate loading of single-tooth ITI implants in the anterior maxilla: a prospective 5-year pilot study. Clin Oral Implants Res. 2002. 13:281–7.

24.Arem AJ., Madden JW. Effects of stress on healing wounds: I. Intermittent noncyclical tension. J Surg Res. 1976. 20:93–102.

25.Burgess LP., Morin GV., Rand M., Vossoughi J., Hollinger JO. Wound healing. Relationship of wound closing tension to scar width in rats. Arch Otolaryngol Head Neck Surg. 1990. 116:798–802.

26.Meyer M., McGrouther DA. A study relating wound tension to scar morphology in the pre-sternal scar using Langers technique. Br J Plast Surg. 1991. 44:291–4.

27.Langer K. On the anatomy and physiology of the skin. II. Skin tension. Br J Plast Surg. 1978. 31:93–106.
29.Small PN., Tarnow DP. Gingival recession around implants: a 1-year longitudinal prospective study. Int J Oral Maxillofac Implants. 2000. 15:527–32.
30.Cardaropoli G., Lekholm U., Wennstro ¨m JL. Tissue alterations at implant-supported single-tooth replacements: a 1-year prospective clinical study. Clin Oral Implants Res. 2006. 17:165–71.

31.DeAngelo SJ., Kumar PS., Beck FM., Tatakis DN., Leblebicioglu B. Early soft tissue healing around one-stage dental implants: clinical and microbiologic parameters. J Periodontol. 2007. 78:1878–86.

32.Tal H., Dayan D. Spontaneous early exposure of submerged implants: II. Histopathology and histomorphome-try of non-perforated mucosa covering submerged implants. J Periodontol. 2000. 71:1224–30.

33.Tal H., Dayan D. Spontaneous early exposure of submerged implants: III. Histopathology of perforated mucosa covering submerged implants. J Periodontol. 2000. 71:1231–5.

34.Martins MC., Abi-Rached RS., Shibli JA., Araujo MW., Marcantonio E Jr. Experimental peri-implant tissue breakdown around different dental implant surfaces: clinical and radiographic evaluation in dogs. Int J Oral Maxillofac Implants. 2004. 19:839–48.
35.Haas R., Haimbo ¨ck W., Mailath G., Watzek G. The relationship of smoking on peri-implant tissue: a retrospective study. J Prosthet Dent. 1996. 76:592–6.

36.Abrahamsson I., Berglundh T., Lindhe J. The mucosal barrier following abutment dis/reconnection. An experimental study in dogs. J Clin Periodontol. 1997. 24:568–72.

37.Cochran DL., Hermann JS., Schenk RK., Higginbottom FL., Buser D. Biologic width around titanium implants. A histometric analysis of the implanto-gingival junction around unloaded and loaded nonsubmerged implants in the canine mandible. J Periodontol. 1997. 68:186–98.

38.Hansson HA., Albrektsson T., Bra � nemark PI. Structural aspects of the interface between tissue and titanium implants. J Prosthet Dent. 1983. 50:108–13.

39.Gould TR., Westbury L., Brunette DM. Ultrastructural study of the attachment of human gingiva to titanium in vivo. J Prosthet Dent. 1984. 52:418–20.
40.Hashimoto M., Akagawa Y., Nikai H., Tsuru H. Ultrastructure of the peri-implant junctional epithelium on single-crystal sapphire endosseous dental implant loaded with functional stress. J Oral Rehabil. 1989. 16:261–70.
41.Homans J. A textbook of surgery. Illinois: Charles C Thomas Publisher;1945. p. 1–30.
42.Sabiston DC., Lyerly HK. Textbook of surgery. The biological basis of modern surgical practice. WB Saunders Company;1997. p. 207–20.
43.Mathes SJ. Plastic surgery. Saunders Elsevier Company;2006. p. 209–34.
44.Pham AN., Fiorellini JP., Paquette D., Williams RC., Weber HP. Longitudinal radiographic study of crestal bone levels adjacent to nonsubmerged dental implants. J Oral Implantol. 1994. 20:26–34.
45.Hermann JS., Cochran DL., Nummikoski PV., Buser D. Crestal bone changes around titanium implants. A radiographic evaluation of unloaded nonsubmerged and submerged implants in the canine mandible. J Periodontol. 1997. 68:1117–30.

46.Naert I., Gizani S., van Steenberghe D. Bone behavior around sleeping and non-sleeping implants retaining a mandibular hinging overdenture. Clin Oral Implants Res. 1999. 10:149–54.
Go to : 
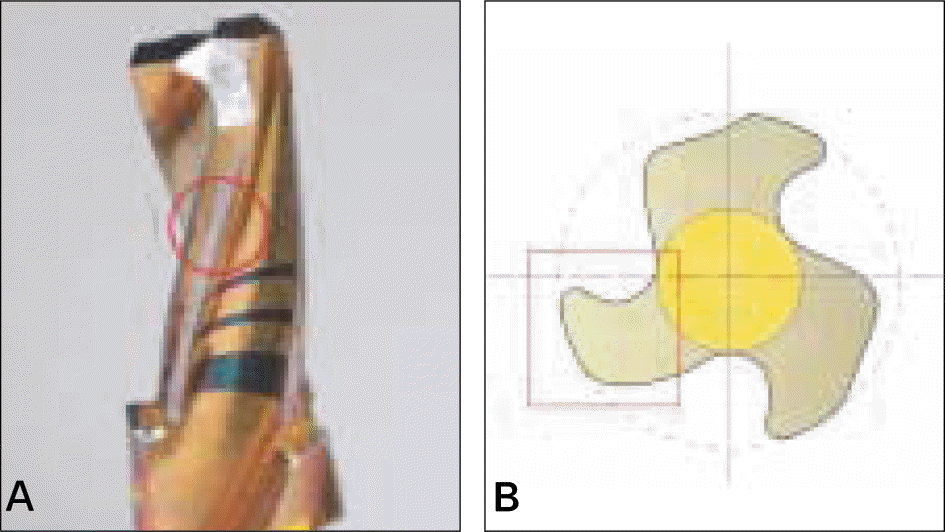 | Fig. 2.Clinical photograph of a drill that has only 0.5 mm cutting edge at terminal portion and a blunted edge at other portion (A) and diagram of cross section (B). |
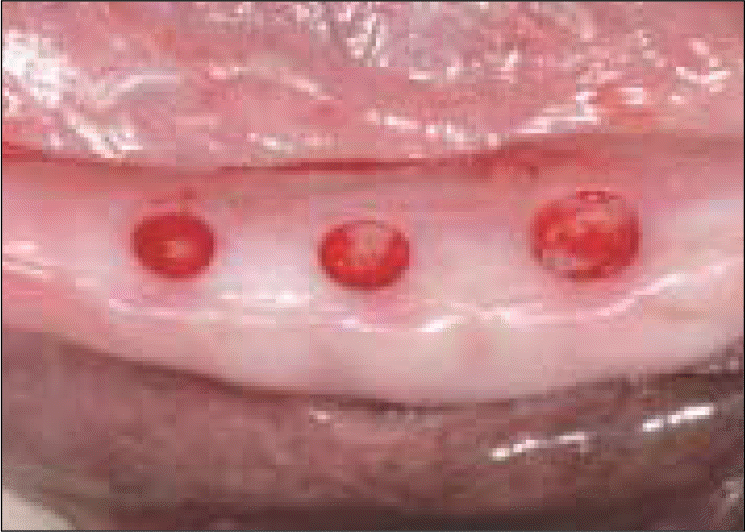 | Fig. 3.Clinical feature immediately after punching using 3 mm, 4 mm and 5 mm tissue punches. |
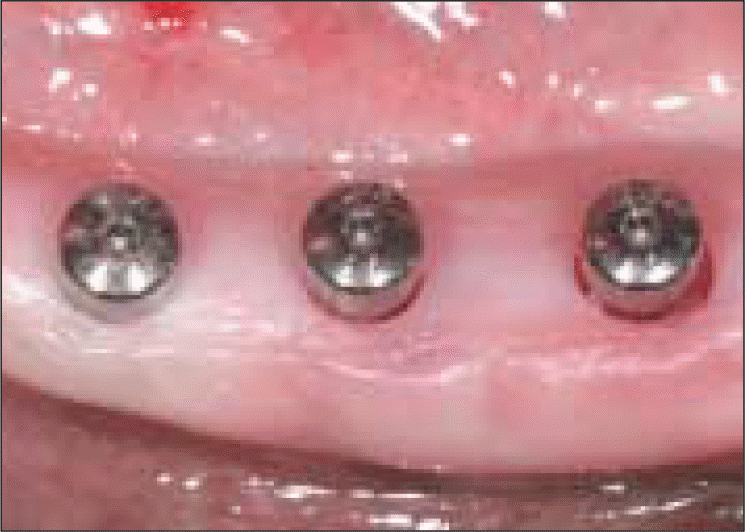 | Fig. 4.Clinical feature after placing a 4 mm fixture and a 4.5 mm permucosal healing abutment. |
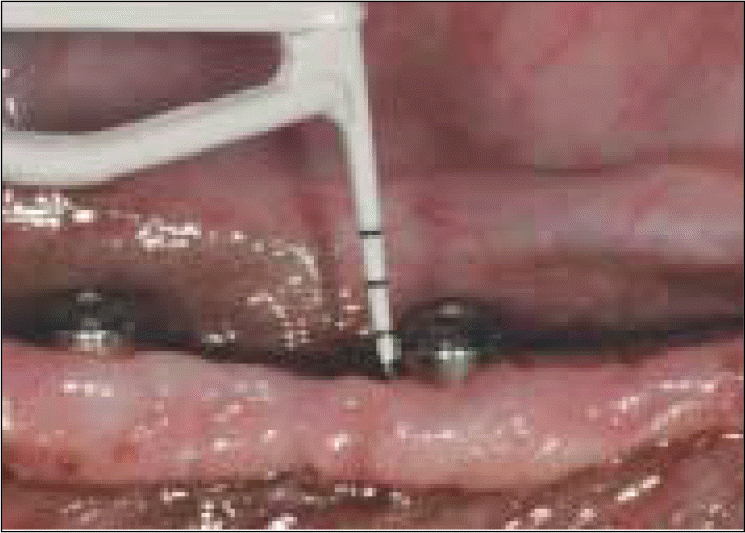 | Fig. 7.Clinical feature of measuring pocket depths using probes with a probing force of 0.2 N. |
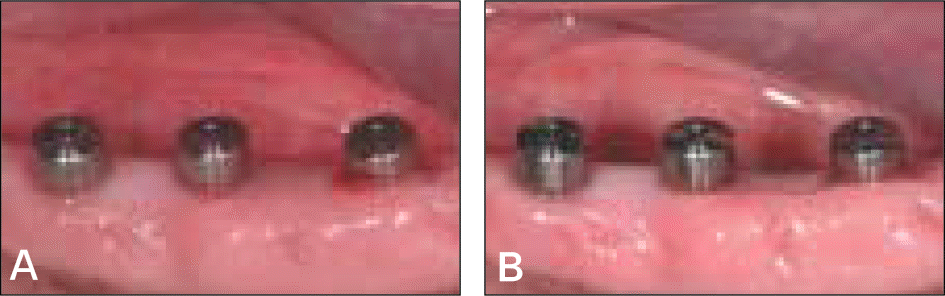
 | Fig. 12.Clinical photograph of the implants at 3 weeks (A) and 12 weeks (B) after implant placement. |
 | Fig. 14.Periapical radiographs taken at 3 weeks (A) and 12 weeks (B) after implant placement. Note that most early bone loss occurred around the implants during the first three weeks after implant placement, and more marginal bone loss occurred with the ≥ 4 mm tissue punch than with the 3 mm tissue punch. |
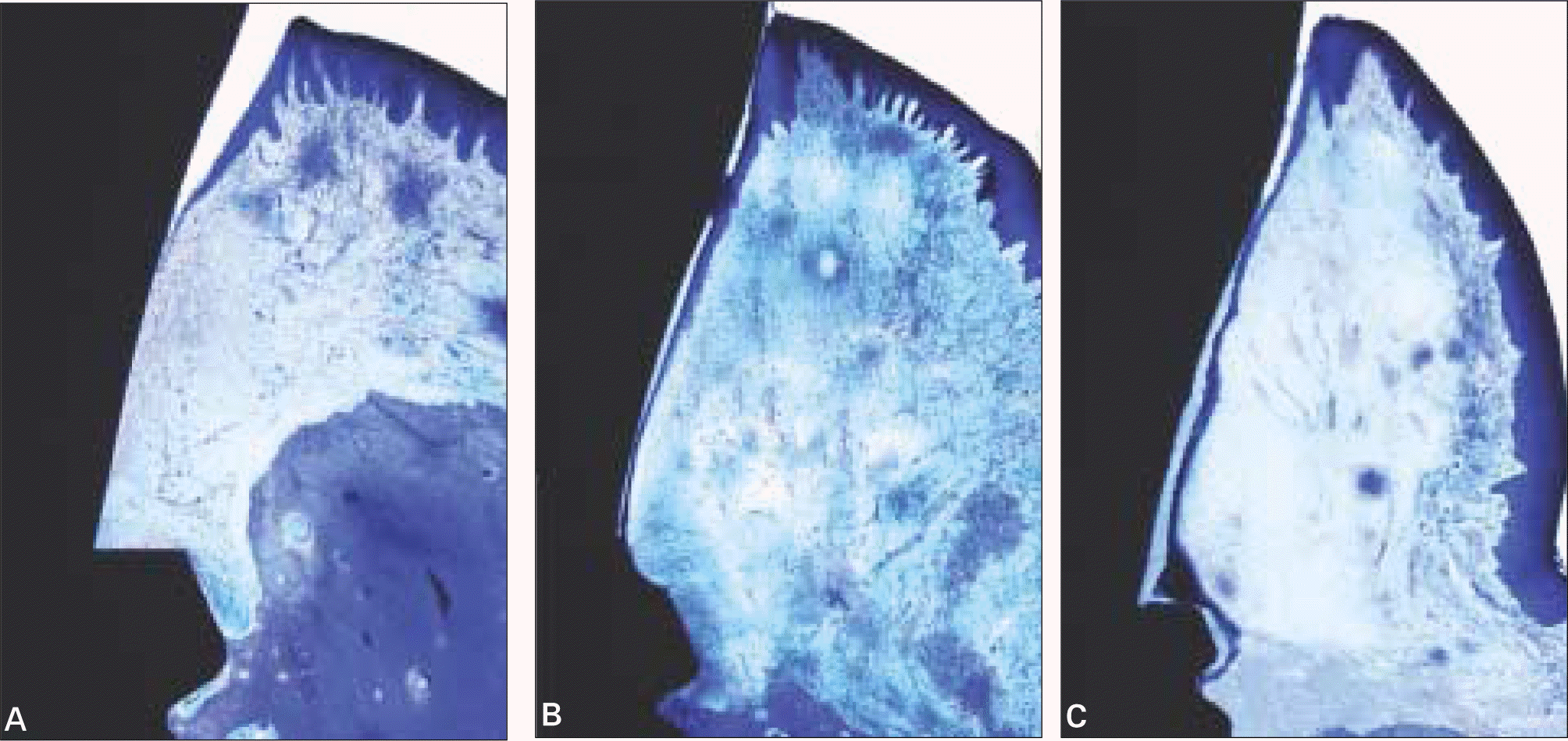 | Fig. 15.Magnified view of the specimens showing the peri-implant mucosa. (A) Implant placed with a 3 mm tissue punch. (B) Implant placed with a 4 mm tissue punch. (C) Implant placed with a 5 mm tissue punch. (Toluidine blue stain, × 12) |
Table I.
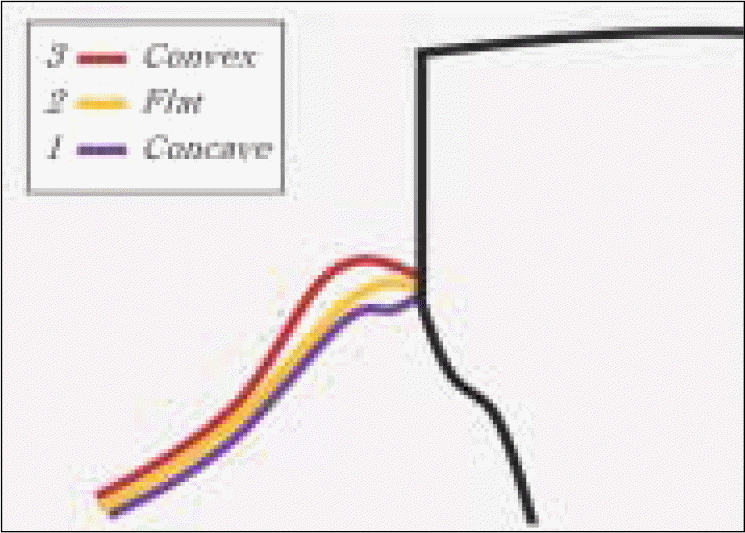
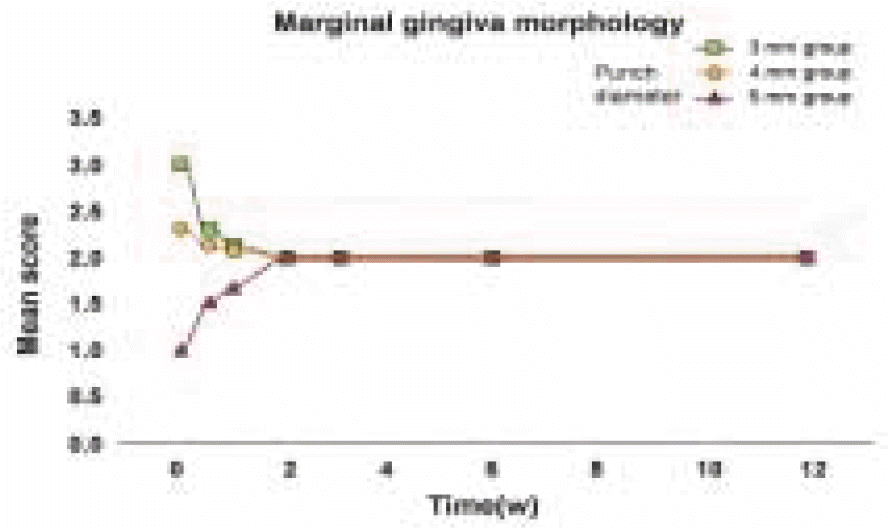
Marginal gingiva morphology
Table II.
Soft tissue level : Buccal
Table III.
Clinical and radiological parameters




 PDF
PDF ePub
ePub Citation
Citation Print
Print





 XML Download
XML Download