Abstract
This paper reports two cases of schwannomas arising from the oral cavity. One is an intraoral ancient schwannoma located at the left cheek, which evolved over a period of 13 years. The tumor was a well-demarcated buccal mass, which was located in the left lower first premolar area, with an obliterated the buccal vestibule, leaving the overlying mucosa intact. The second case was a central intraosseous schwannoma located from the left lower 1st molar periapical area to the left 3rd molar periapical area. Pathologically, the first mass was composed of the spindle shaped tumor cells with wavy nuclei beneath the fibroconnective tissue of the gingiva but second case mass was not. Occasional nuclear pleomorphism was observed but mitosis or necrosis was absent. There were Antoni A and B areas along with strong, diffuse staining with the S-100 protein. Ancient schwannomas were diagnosed. Schwannoma is a slow-growing benign tumor, and an ancient schwannoma that shows cellular atypism is a variant of a schwannoma caused by purely degenerative changes. To date, only limited cases of ancient schwannomas in the oral cavity have been reported.
References
1. Martins MD, Anunciato de Jesus L, Fernandes KP, Bussadori SK, Taghloubi SA, Martins MA. Intraoral schwannoma: case report and literature review. Indian J Dent Res. 2009; 20:121–5.

2. Yang SW, Lin CY. Schwannoma of the upper lip: case report and literature review. Am J Otolaryngol. 2003; 24:351–4.

3. Grabowski L. A rare case of schwannoma of the tongue. Otolaryngol Pol. 2008; 62:191–4.
4. Marx RE, Stern D. Oral and maxillofacial pathology: a rationale for treatment. 1st ed.Carol Stream: Quintessence Publishing;2003. p. 408–11.
5. Eversole LR, Howell RM. Ancient neurilemmoma of the oral cavity. Oral Surg Oral Med Oral Pathol. 1971; 32:440–3.

6. Marks RK, Carr RF, Kreller AJ 3rd. Ancient neurilemoma of the floor of the mouth: report of a case. J Oral Surg. 1976; 34:731–5.
7. McCoy JM, Mincer HH, Turner JE. Intraoral ancient neurilemoma (ancient schwannoma). Report of a case with histologic and electron microscopic studies. Oral Surg Oral Med Oral Pathol. 1983; 56:174–84.
8. Dayan D, Buchner A, Hirschberg A. Ancient neurilemmoma (Schwannoma) of the oral cavity. J Craniomaxillofac Surg. 1989; 17:280–2.

9. Nakayama H, Gobara R, Shimamoto F, Kajihara H. Ancient schwannoma of the oral floor and ventricular portion of the tongue: a case report and review of the literature. Jpn J Clin Oncol. 1996; 26:185–8.

10. Ledesma C, Portilla J, Hernandez F, Garces M, Hernandez JC. Paraglandular ancient schwannoma. Med Oral. 1999; 4:398–402.
11. Kim TW, Go CH, Song BU, Yang CM. A case of ancient schwannoma of the lingual nerve. Korean J Otolaryngol-Head Neck Surg. 2000; 43:559–61. .(Korean).
12. Chen CY, Wang WC, Chen CH, Chen YK, Lin LM. Ancient schwannoma of the floor of the mouth –A case report and review. Oral Oncol Extra. 2006; 42:281–5.
13. Subhashraj K, Balanand S, Pajaniammalle S. Ancient schwannoma arising from mental nerve. A case report and review. Med Oral Patol Oral Cir Bucal. 2009; 14:E12–4.
14. Amirchaghmaghi M, Salehinejad J, Basirat M, Delavarian Z, Javadzade A, Forouzanfar A. Gingival ancient schwannoma: Review of literature and a case report. J Applied Sci. 2010; 10:3137–40.
15. Bilici S, Akpınar M, Yiğit O, Günver F. Ancient schwannoma of the tongue: a case report. Kulak Burun Bogaz Ihtis Derg. 2011; 21:234–6.
16. Humber CC, Copete MA, Hohn FI. Ancient schwannoma of upper lip: case report with distinct histologic features and review of the literature. J Oral Maxillofac Surg. 2011; 69:e118–22.

17. Karaca CT, Habesoglu TE, Naiboglu B, Habesoglu M, Oysu C, Egeli E, et al. Schwannoma of the tongue in a child. Am J Otolaryngol. 2010; 31:46–8.

18. López-Carriches C, Baca-Pérez-Bryan R, Montalvo-Montero S. Schwannoma located in the palate: clinical case and literature review. Med Oral Patol Oral Cir Bucal. 2009; 14:e465–8.
19. Gallego L, Junquera L, Rodríguez-Recio C, Fresno MF. Intraosseous mandibular schwannoma mimicking an odontogenic keratocyst, with a postsurgical pathological fracture. J Laryngol Otol. 2009; 123:560–2.

20. Flickinger FW, Lozano RL, Yuh WT, Sachs MA. Neurilemoma of the tongue: MR findings. J Comput Assist Tomogr. 1989; 13:886–8.
21. Weiss SW, Goldblum JR. Benign tumors of peripheral nerves. Weiss SW, Goldblum JR, editors. Enzinger and Weiss's Soft Tissue Tumors. 5th ed.Philadelphia: Mosby;2008. p. 825–902.
Fig. 1.
Axial (A) and coronal (B) computed tomography of Case 1 reveals an ill defined lesion at the left mandibular body (arrows). Na Rae Kim et al: Ancient schwannoma in oral cavity: a report of two cases. J Korean Assoc Oral Maxillofac Surg 2011
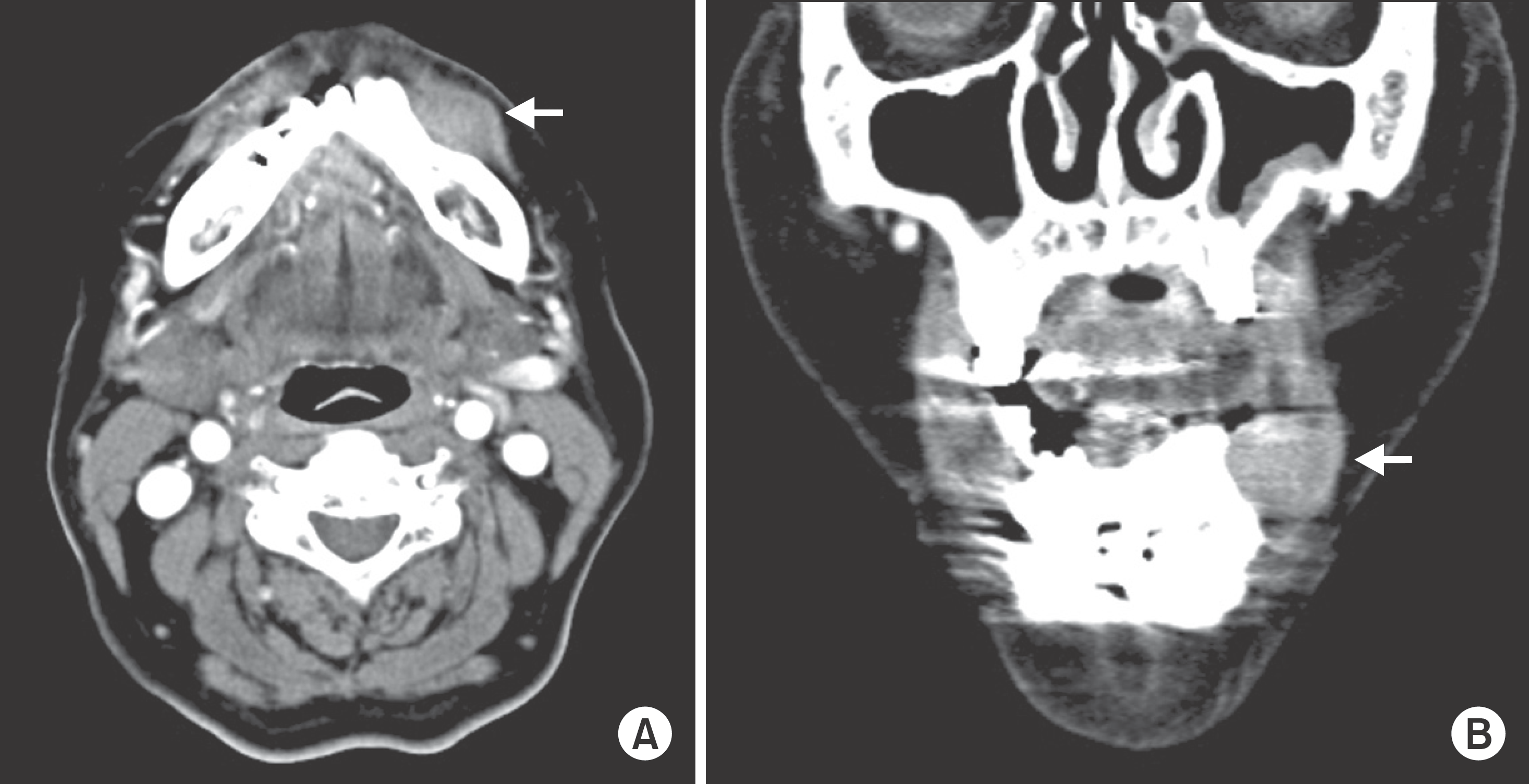
Fig. 2.
The well circumscribed protruding mass over the first premolar area near the mental foramen is seen in Case 1. Na Rae Kim et al: Ancient schwannoma in oral cavity: a report of two cases. J Korean Assoc Oral Maxillofac Surg 2011
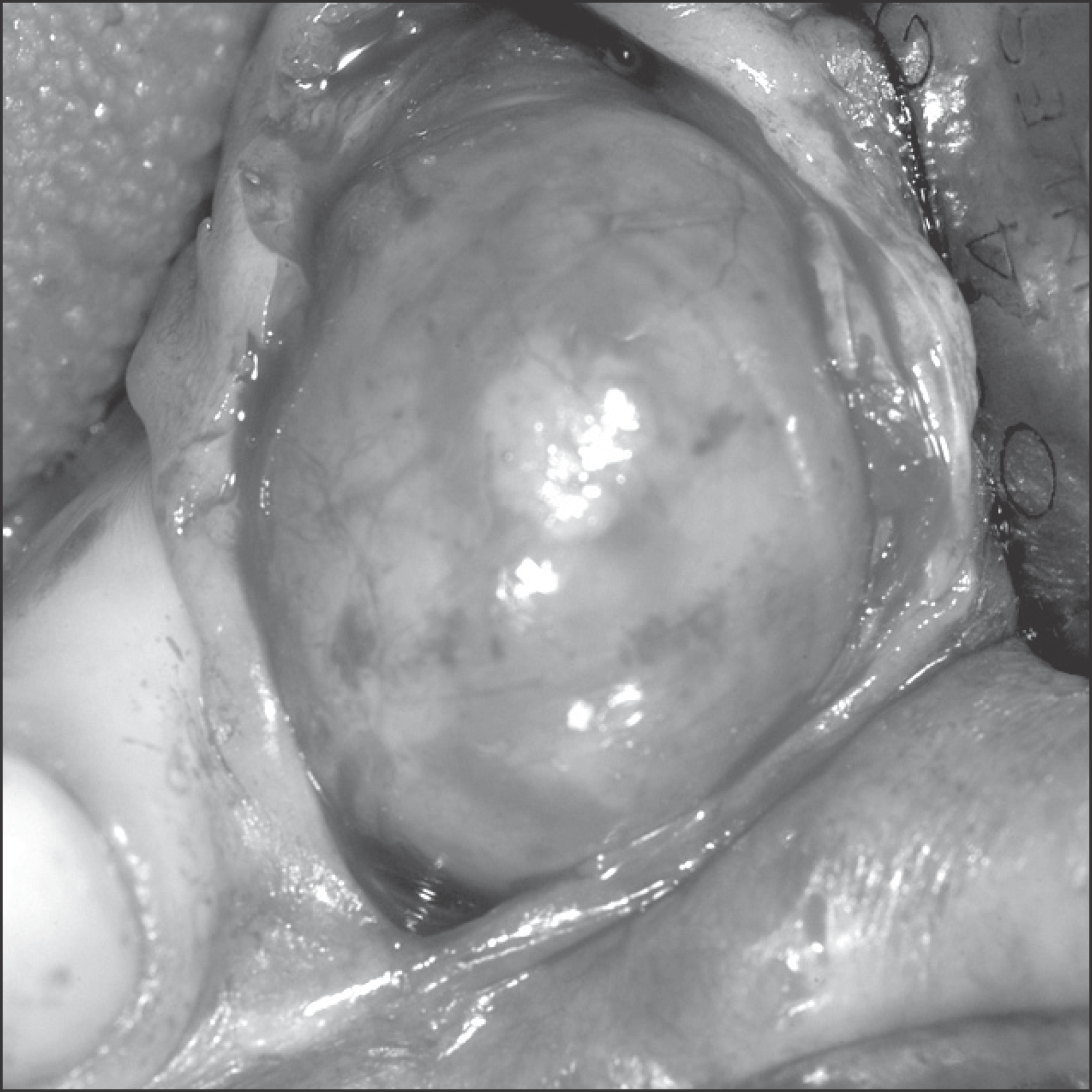
Fig. 3.
A. The relatively well marginated mass consists of spindle shaped tumor cells with buckling nuclei (H & E staining, ×40). B. The mass comprises the Antoni A area with the nuclear palisading patterns forming occasional Verocay bodies (arrow). Note the paucicellular myxoid Antoni B area (left upper portion, H & E staining, ×200). Na Rae Kim et al: Ancient schwannoma in oral cavity: a report of two cases. J Korean Assoc Oral Maxillofac Surg 2011
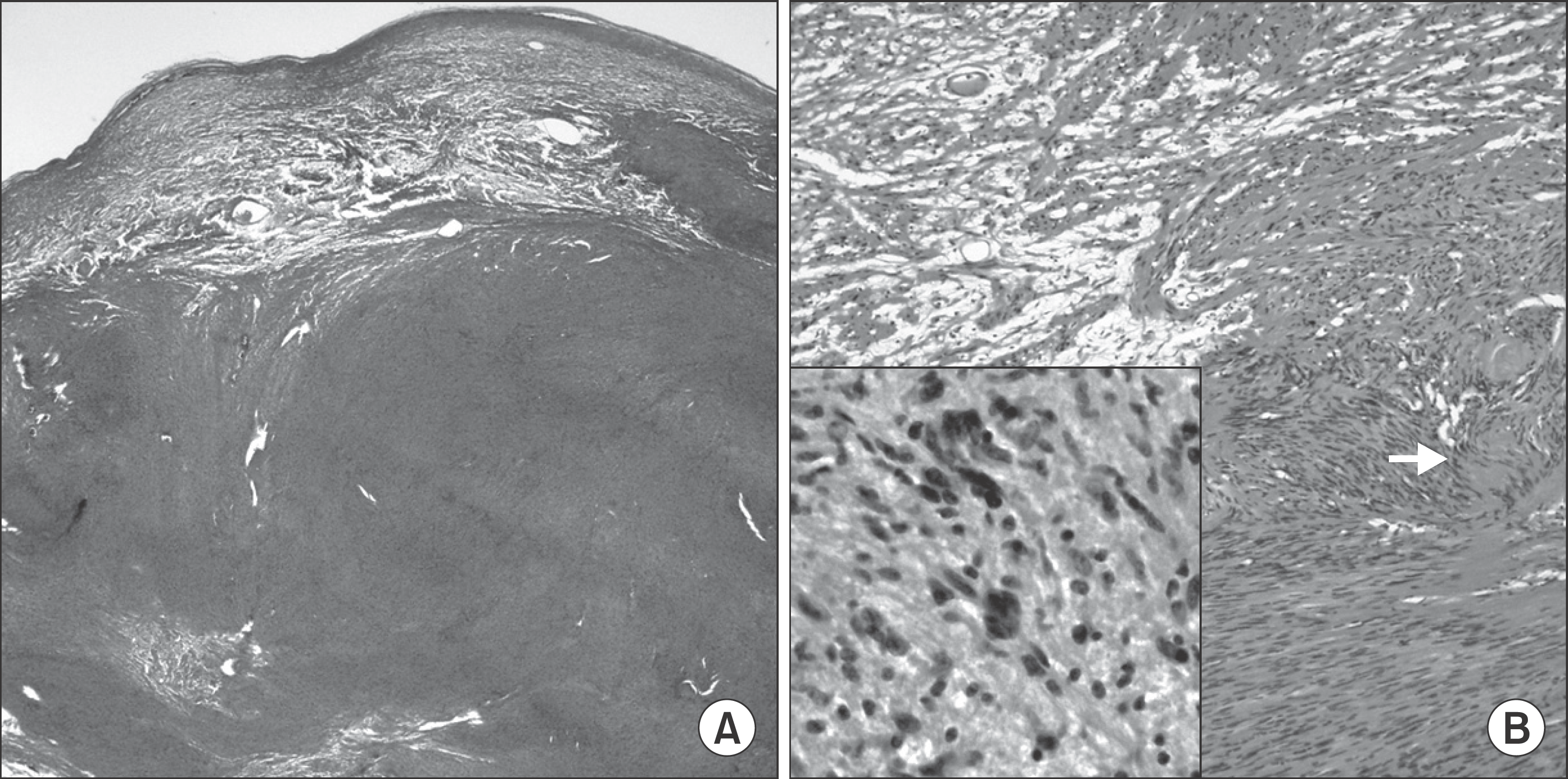
Fig. 4.
Panoramic view of Case 2 showed well-defined homogeneous low density about 3.0×1.5×2.0 cm-sized cystic mass which is including inferior alveolar nerve in left mandible body. Left lower 1st molar distal root and 2nd molar root were resorption state. Na Rae Kim et al: Ancient schwannoma in oral cavity: a report of two cases. J Korean Assoc Oral Maxillofac Surg 2011
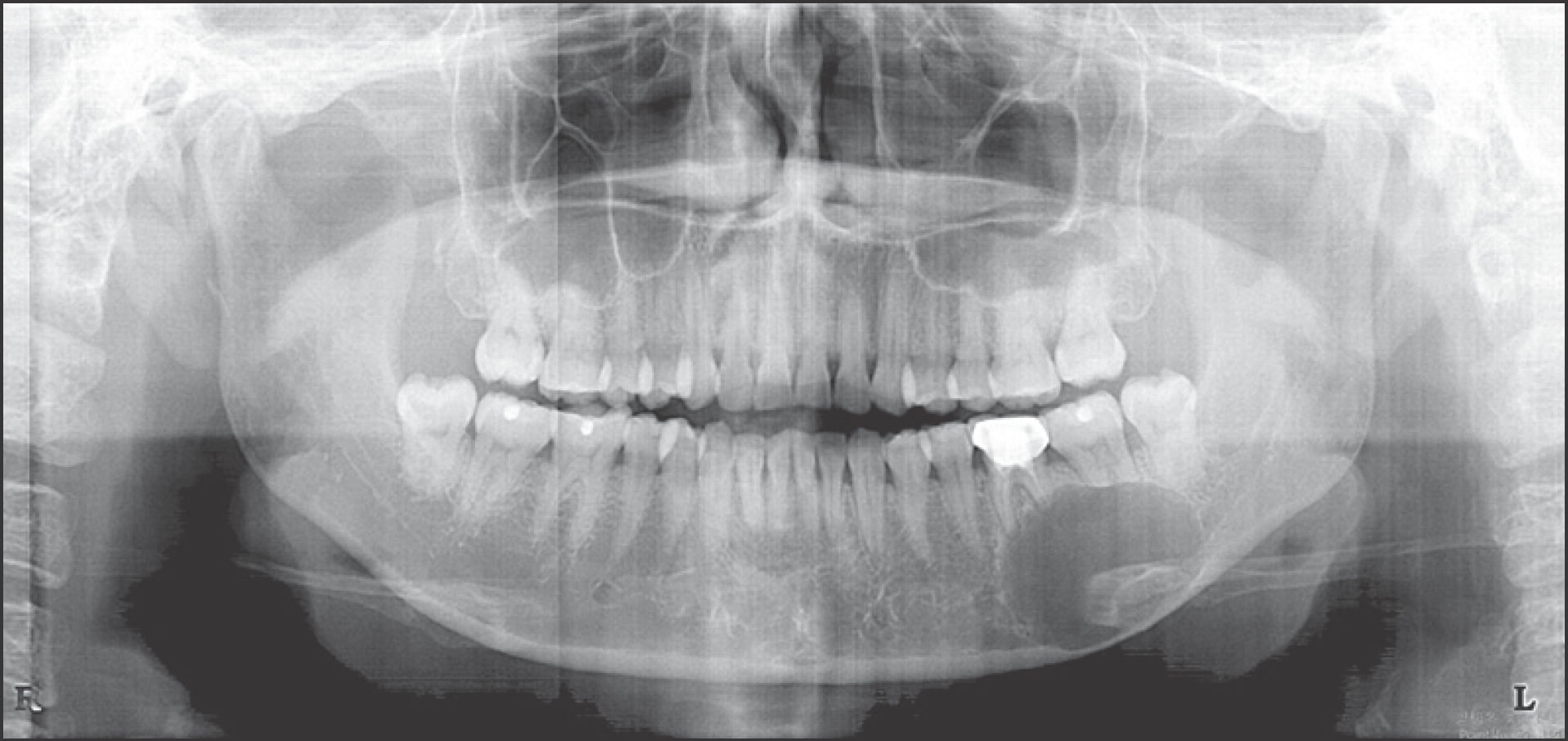
Fig. 5.
A well-defined homogenous low density cystic mass in left mandible body. Definite root resorptions of molars were seen in left mandible. Na Rae Kim et al: Ancient schwannoma in oral cavity: a report of two cases. J Korean Assoc Oral Maxillofac Surg 2011
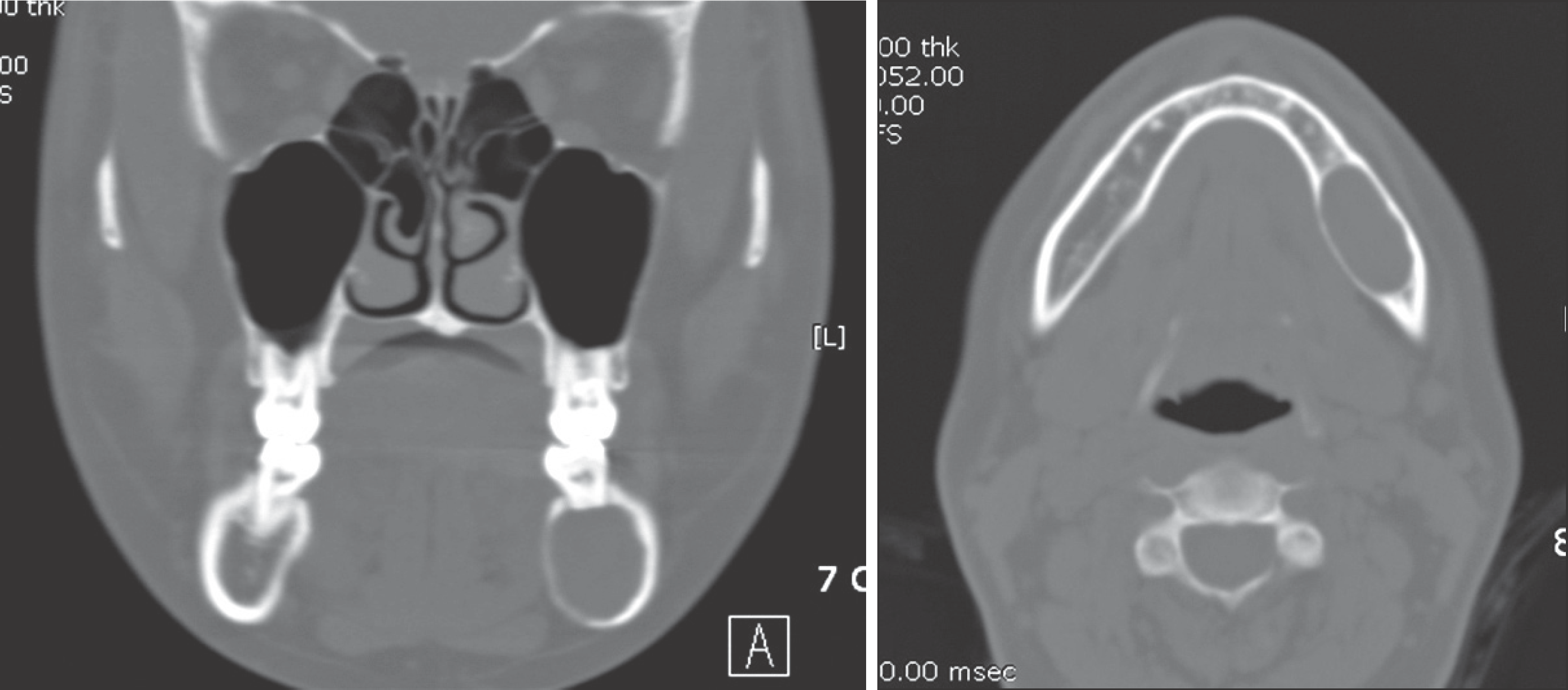
Fig. 6.
The biopsied specimen is composed of spindle cells with twisted nuclei (H & E staining, ×100). Na Rae Kim et al: Ancient schwannoma in oral cavity: a report of two cases. J Korean Assoc Oral Maxillofac Surg 2011Na Rae Kim et al: Ancient schwannoma in oral cavity: a report of two cases. J Korean Assoc Oral Maxillofac Surg 2011

Table 1.
Summary of the intraoral ancient schwannomas including the presented two cases




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download