Abstract
An intracapsular and pericapsular infection of the temporomandibular joint (TMJ) is rare. The invasion of bacteria into the joint space can occur through several routes. Among them, hematogenous spread is most common. This report describes three cases of abscess formation in the TMJ (intracapsular and pericapsular infection). The patients were treated with supportive care and surgical intervention (incision and drainage) under hospitalization, and their symptoms had improved. Pain of the TMJ is a typical symptom of temporomandibular joint disorders (TMD). On the other hand, an infection of the TMJ can also cause pain on the affected side, and can be misdiagnosed as routine TMD. Therefore, the possibility of an infection of the TMJ cavity should be considered when treating TMD.
Go to : 
References
2. Goldschmidt MJ, Butterfield KJ, Goracy ES, Goldberg MH. Streptococcal infection of the temporomandibular joint of hematogenous origin: a case report and contemporary therapy. J Oral Maxillofac Surg. 2002; 60:1347–53.

3. Borenstein DG, Simon GL. Hemophilus influenzae septic arthritis in adults. A report of four cases and a review of the literature. Medicine (Baltimore). 1986; 65:191–201.
4. Schurman DJ, Mirra J, Ding A, Nagel DA. Experimental E. coli arthritis in the rabbit. A model of infectious and post-infectious inflammatory synovitis. J Rheumatol. 1977; 4:118–28.
5. Bounds GA, Hopkins R, Sugar A. Septic arthritis of the temporomandibular joint–a problematic diagnosis. Br J Oral Maxillofac Surg. 1987; 25:61–7.

8. Hekkenberg RJ, Piedade L, Mock D, Baker G, Freeman JL. Septic arthritis of the temporomandibular joint. Otolaryngol Head Neck Surg. 1999; 120:780–2.

9. Murakami K, Matsumoto K, Iizuka T. Suppurative arthritis of the temporomandibular joint. Report of a case with special reference to arthroscopic observations. J Maxillofac Surg. 1984; 12:41–5.
10. Goodman WS, Strelzow VV. Infections of the temporomandibular joint. J Otolaryngol. 1979; 8:250–4.
11. Henry CH, Hughes CV, Gérard HC, Hudson AP, Wolford LM. Reactive arthritis: preliminary microbiologic analysis of the human temporomandibular joint. J Oral Maxillofac Surg. 2000; 58:1137–42.

12. Kim SJ, Park YH, Hong SP, Cho BO, Park JW, Kim SG. The presence of bacteria in the synovial fluid of the temporomandibular joint and clinical significance: preliminary study. J Oral Maxillofac Surg. 2003; 61:1156–61.

13. Hincapie JW, Tobon D, Diaz-Reyes GA. Septic arthritis of the temporomandibular joint. Otolaryngol Head Neck Surg. 1999; 121:836–7.

16. Piecuch J, Lieblich S. Anatomy and pathology of the temporomandibular joint. Peterson U, editor. Principles of Oral and Maxillofacial Surgery. 3. Philadelphia: JB Lippincott;1992. p. 1867–71.
Go to : 
 | Fig. 1.A. Clinical findings in Case 1. Hypoocclusion with ipsilateral posterior open bite. B. Computed tomography (CT) findings in Case 1. Coronal CTscan reveals intracapsular abscess formation in left temporomandibular joint with widened joint cavity (arrow). C. Treatment of Case 1. D. CT findings of postoperation in Case 1. One month follow-up CT-scan reveals a normal joint cavity. Hyung-Mo Kim et al: Infection of the temporomandibular joint: a report of three cases. J Korean Assoc Oral Maxillofac Surg 2011
|
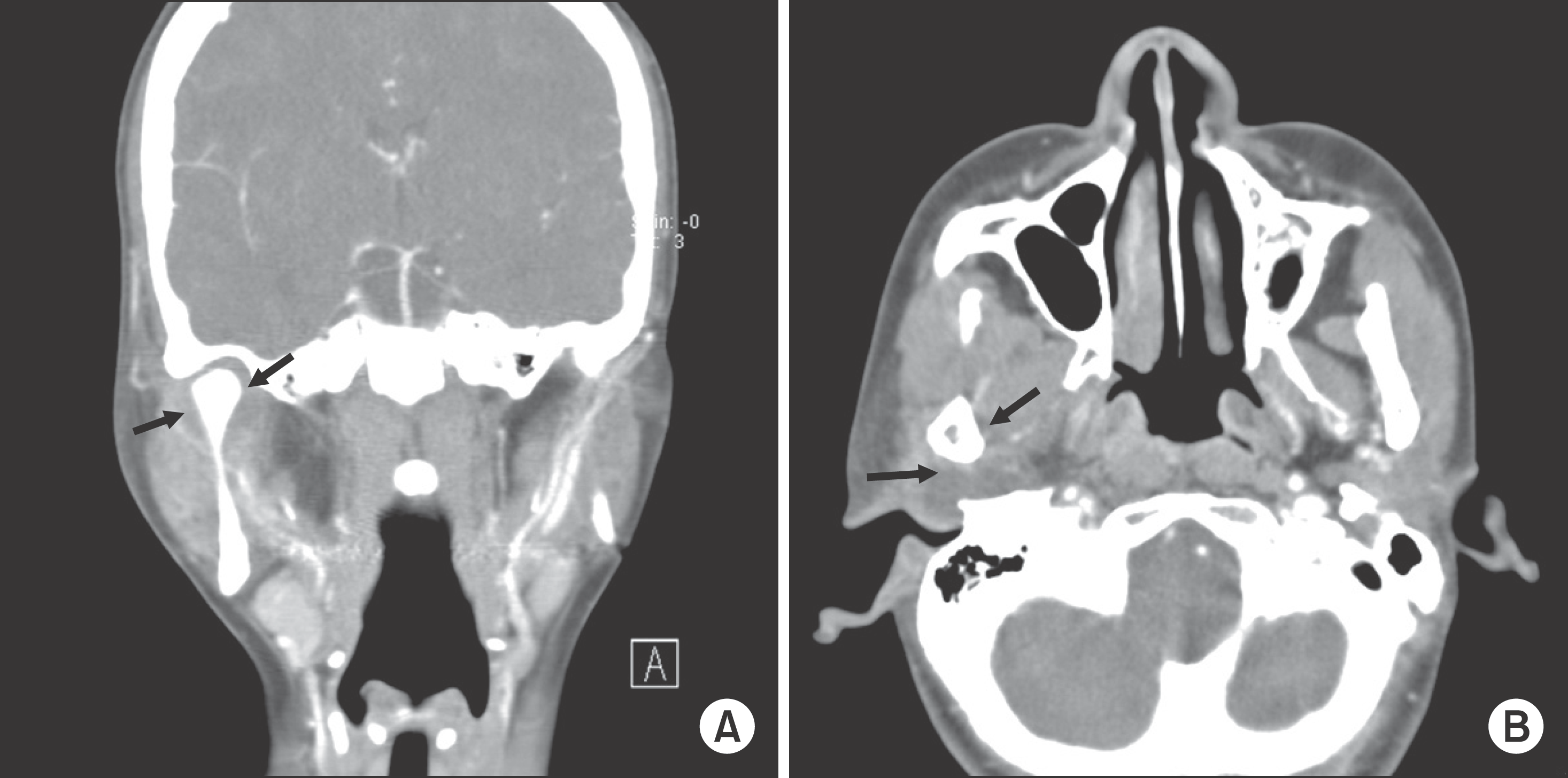
 | Fig. 2.A, B. Computed tomography (CT) findings of Case 2. Diffuse inflammation and multifocal small abscess cavity around right temporomandibular joint (arrows). C. CT findings of postoperation in Case 2. Normal joint cavity was seen (1 month later). Hyung-Mo Kim et al: Infection of the temporomandibular joint: a report of three cases. J Korean Assoc Oral Maxillofac Surg 2011
|




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download