Abstract
Some herbal medications induce acute kidney injury. The acute kidney injuries caused by herbal medications are mild and commonly treated by palliative care. A 51-years-old man who drank the juice squeezed from the raw tubers of Dioscorea quinqueloba (D. quinqueloba) was admitted with nausea, vomiting and chilling. He developed a seizure with decreased level of consciousness. He was diagnosed with acute kidney injury, which was cured by continuous venovenous hemodialfiltration. Non-detoxified D. quinqueloba can cause severe acute kidney injury with toxic encephalopathy. It is critical to inform possible adverse effects of the medicinal herbs and to implement more strict regulation of these products.
There has been a trend to consider herbal medicines as more natural and safe than western medicines.1 Herbal medicines have been widely used in western countries as well as in Asian countries.2 However, many people lack the proper knowledge of medicinal herbs and take them without specialist advice.3 Therefore, adverse effects associated with herbal materials are increasingly reported. Especially, kidney injury is one of the common adverse effects caused by herbal materials.4
Dioscorea species, known as yams, are an important tuber crop used as dietary component in tropical regions.5 Some of them are used in herbal medicines. However, taking yams without proper detoxification process can cause poisoning although the injury mechanism is unknown.6 For instance, even though Dioscorea quinqueloba (D. quinqueloba) is known to help relieve symptoms caused by atherosclerosis, myocardial infarction and asthma, it can induce acute kidney injury.7
We report a case of severe acute kidney injury with toxic encephalopathy caused by ingestion of D. quinqueloba. This case is noteworthy because it was a more critical than previously reported cases, and the patient needed more aggressive care than conservative care only.
A 51-years-old man visited the department of internal medicine complaining of vomiting, nausea, headache and weakness. He had no past medical history and family history of note. He has frequently taken medicinal herbs for his own health. Three days ago, he dug up tubers of D. quinqueloba and drank about 400 mL of juice made from the raw tubers (Fig. 1). His wife took only a small amount of it. The following morning, he felt nausea and was vomiting continuously. While his wife developed the same symptoms, her symptoms were relatively milder and disappeared shortly.
On admission, he was alert and his blood pressure was 130/90 mm Hg, respiration 20/min, pulse 80/min, and body temperature 37.8℃. The results of chest auscultation and physical examination were normal. His laboratory values also showed normal range. On the 2nd day, his creatinine (Cr) level was 2.9 mg/dL, and blood urea nitrogen (BUN) was 42.7 mg/dL. Kidney ultrasonography revealed both kidney of normal size and echogenicity.
On the 3rd day, his body temperature elevated to 39.0℃ and he developed a tonic-clonic type of seizure with decreased level of consciousness. However, brain perfusion computed tomography and cerebrospinal fluid tapping were normal. His blood gas analysis revealed pH 7.10, pCO2 24 mm Hg, pO2 69 mm Hg, and pO2 saturation 87.4%. His anion gap (AG) was 20.6, and he had a high AG metabolic acidosis. While his brain magnetic resonance diffusion imaging was normal, his electroencephalogram showed an abnormal feature of high significance with evidence of nonspecific and diffuse cerebral dysfunction (Fig. 2). We inserted an intubation tube and sedated the patient. He received emergency hemodialysis and then was transferred to the intensive care unit. On the 5th day, he had BUN 88.8 mg/dL and Cr 8.6 mg/dL. He was placed on continuous venovenous hemodiafiltration (CVVHDF). After the CVVHDF treatment, the levels of BUN level gradually decreased from 88.8 mg/dL to 39.4 mg/dL and Cr level decreased from 8.6 mg/dL to 2.4 mg/dL. As his level of consciousness continued to improve, he was discontinued with the CVVHDF and extubated on the 12th day. On the 13th day, he was transferred to a general ward for conservative care. On the 26th day, the level of BUN and Cr dropped to 8.4 mg/dL and 1.2 mg/dL, respectively, and he was discharged and regularly followed up (Table 1).
Herbs are widely used for health care in developed and developing countries.8,9 Many of them are classified as dietary supplements. Therefore, herbal materials are easily available and not under strict control of authorities. Furthermore, there is a widespread belief that these materials are harmless.10 However, most people have not been aware of the possible adverse effects as well as the proper handling and dosage amount. In recent years, various adverse effects related with herbal medicines have increasingly been reported.11
Dioscorea species are one of the widely well-known folklore medicinal herbs. Some countries use them for food and herbal medicine.12 However, It has been under-recognized and under-reported that non-detoxified Dioscorea spp. can induce acute kidney injury.7 Before taking them, the detoxification process is necessary to avoid any possible toxicity or adverse effects. Boiling, steaming and baking in fire are effective ways of detoxification.13 In vivo experiment, non-detoxified Dioscorea spp. can trigger chronic kidney injury via direct toxicity and pro-fibrotic in the kidney.14 However, the pathophysiology of acute kidney injury related with Dioscorea spp. is unknown.
In our case, the patient consumed the tuber of D. quinqueloba in a raw undiluted juice form without the detoxification process. The non-detoxified herb leads to severe acute kidney injury with seizure and toxic encephalopathy. The mechanism of toxic encephalopathy associated with Dioscorea spp. has not been reported. Nevertheless, Dioscorea spp. are rich in dioscorine and dioscine both of which can induce convulsive, local anesthetic, and anti-diuretic actions.6 Therefore, it can be inferred that the consumption of these undiluted components and reduced kidney function are related with developing toxic encephalopathy.
Although there have been reports of acute kidney injury associated with D. quinqueloba, the patients in the previously reported cases had diabetes, and their symptoms were mild and cured by palliative care only.7 In contrast, our patient had no evidence of underlying disease, but was in a life-threatening condition that needed a more aggressive care such as CVVHDF. This case reveals that an inappropriate use of D. quinqueloba can lead to severe acute kidney injury which requires aggressive treatments in healthy people. People should be informed about the possible adverse effects of non-detoxified herbs. Additionally, herbal medicines which can induce severe side effects need to be classified as prescription drugs and to be regulated more strictly.
Figures and Tables
Fig. 2
Electroencephalogram showed diffuse continuous slowing (theta or delta range) with maximum appearance at the frontal electrode.
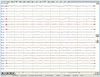
Table 1
Laboratory Results and Clinical Course during Hospital Stay

ACKNOWLEDGEMENTS
This research was supported by the 2014 scientific promotion program funded by Jeju National University.
References
3. Gabardi S, Munz K, Ulbricht C. A review of dietary supplement-induced renal dysfunction. Clin J Am Soc Nephrol. 2007; 2:757–765.

4. Isnard Bagnis C, Deray G, Baumelou A, Le Quintrec M, Vanherweghem JL. Herbs and the kidney. Am J Kidney Dis. 2004; 44:1–11.

5. Mengesha WA, Demissew S, Fay MF, Smith RJ, Nordal I, Wilkin P. Genetic diversity and species delimitation in the cultivated and wild Guinea yams (Dioscorea spp.) from Southwest Ethiopia as determined by AFLP (amplified fragment length polymorphism) markers. Genet Resour Crop Evol. 2013; 60:1365–1375.

6. Steenkamp V, Stewart MJ. Nephrotoxicity associated with exposure to plant toxins, with particular reference to Africa. Ther Drug Monit. 2005; 27:270–277.

7. Kim CS, Kim SM, Choi JS, Bae EH, Kim SW. Dioscorea quinqueloba induces acute kidney injury. Clin Toxicol (Phila). 2012; 50:80.

10. Yang CS, Lin CH, Chang SH, Hsu HC. Rapidly progressive fibrosing interstitial nephritis associated with Chinese herbal drugs. Am J Kidney Dis. 2000; 35:313–318.

12. Tchabi A, Burger S, Coyne D, Hountondji F, Lawouin L, Wiemken A, et al. Promiscuous arbuscular mycorrhizal symbiosis of yam (Dioscorea spp.), a key staple crop in West Africa. Mycorrhiza. 2009; 19:375–392.





 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download