Abstract
Medically refractory ventricular tachycardia (VT) storm can be controlled with radiofrequency catheter ablation (RFCA), however, it may be difficult to control in some patients with hemodynamic overload. We experienced a patient with intractable VT storm controlled by hemodynamic unloading. The patient had mid-septal hypertrophic cardiomyopathy with an implantable cardioverter defibrillator (ICD) back-up. Because of the severe mid-septal hypertrophy, his left ventricle (LV) had an hourglass-like morphology and showed apical ballooning; the focus of VT was at the border of apical ballooning. Although we performed VT ablation because of electrical storm with multiple ICD shocks, VT recurred 1 hour after procedure. As the post-RFCA monomorphic VT was refractory to anti-tachycardia pacing or ICD shock, we reduced the hemodynamic overload of LV with β-blockade, hydration, and sedation. VT spontaneously stopped 1.5 hours later and the patient has remained free of VT for 24 months with β-blockade alone. In patients with VT storm refractory to antiarrhythmic drugs or RFCA, the mechanism of mechano-electrical feedback should be considered and hemodynamic unloading may be an essential component of treatment.
Locally-enhanced circumferential strain can be a trigger for ventricular arrhythmias, and mechano-electrical feedback may enhance susceptibility to electrical storm (ES). We report a patient with hypertrophic cardiomyopathy (HCM) who presented with repetitive monomorphic ventricular tachycardia (VT), related to severe mid-septal hypertrophy and apical ballooning.
A 61-year-old male was referred to us because of frequent implantable cardioverter defibrillator (ICD) shocks. Five months earlier, he underwent ICD implantation due to sustained monomorphic VT associated with HCM (Fig. 1A-D) and had been taking amiodarone. 12-lead ECG localized the focus of VT on left ventricular (LV) apical posterior wall (Fig. 1E). Because of recurrent VT and ICD discharges despite intravenous amiodarone and β-blocker, we decided radiofrequency catheter ablation (RFCA). In electrophysiology laboratory, left ventriculography revealed an hourglass shaped LV with apical ballooning (Fig. 2A and B). The VT focus was ablated with a 3.5-mm open-irrigation-tip catheter (NaviStar Thermo-Cool, Biosense Webster, Diamond Bar, CA, USA) after 3D-electroanatomic mapping (CARTO XP, Biosense Webster, Diamond Bar, CA, USA) (Fig. 2C, D and E). The earliest activation site of VT was located at the border of apical ballooning, and VT was terminated during radiofrequency (RF) energy delivery (Stockert generator, Biosense Webster Inc., Diamond Bar, CA, USA, 30 to 50 W, 30 mL/min) at the site showing double potential (Fig. 3) and the earliest activation on CARTO image (Fig. 2E). VT could not be inducible by ventricular stimulation test after RFCA. Unfortunately, however, the identical VT recurred within 1 hour after procedure. This VT did not respond to anti-tachycardia pacing at all, ICD shocks terminated it transiently, but VT was re-initiateded repeatedly. We thought that the potential mechanism of this VT storm was a hemodynamic overload in LV apex distal to severe mid-septal hypertrophy by reduced diastolic filling period and preload during VT and hypotension. Therefore, the patient was managed with sufficient hydration, IV β-blockade, and deep sedation. Finally, VT subsided after 30 minutes of treatment. We maintained β-blocker (Carvedilol 25 mg), but stopped amiodarone 3-month after the procedure. There was no more VT episode during 24-months follow-up.
In patients with ES, mechanical factors should be considered. Myocardial strain strongly influences the repolarization properties and can trigger VT by ventricular mechanoelectrical feedback.1 Mechano-sensitive ion channels or cytoskeletal proteins and the activation of stretch-activated signal transduction pathways may contribute to the trigger and maintenance of VT.2 Generally, the potential mechanism of ventricular tachy-arrhytmias in patients with HCM involvestriggered activity or localized reentry at the area of severely localized myocardial hypertrophy with myofibrillar disarray or fibrosis. In this specific patient, monomorphic VT was reproducibly induced by programmed stimulation, suggesting reentry mechanism before RFCA. On the other hand, however, post-RFCA ES could not be terminated by anti-tachycardia pacing and easily reinitiated immediately after electrical cardioversion, suggesting triggered activity. Therefore, it is highly likely that hemodynamic preload-induced triggered activity on the pre-existing reentrant substrate was the mechanism of VT involved in this patient, although we did not measure LV apical pressure before and after RFCA. Of course, sedation, β-blocker, and hydration together might have contributed to the reduction of triggered activity by slowing-down heart rate, lengthening the diastolic filling period, and reducing apical hemodynamic load or sympathetic over-activity. Although there are several reports of successful RF catheter ablation of VT in patients with HCM and apical aneurysm,3 surgical unloading of mechanical stress should be considered in patients with severe LV mid-septal obstruction.4
In conclusion, we report herein a case of ES in a patient with HCM related to mechanical overload due to severe mid-septal hypertrophy and apical ballooning. It may be helpful to consider mechano-electrical factors in patients with ES that is refractory to medical therapy or catheter ablation. Imaging studies may play an important role in the detection of such mechanical factors.
Figures and Tables
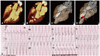 | Fig. 1(A and B) Cardiac CT images of left ventricle (LV) during systole and diastole. (C and D) 3D reconstructed CT images show LV cavity obstruction during systole because of significant mid-septal hypertrophy. (E) 12-lead ECG during ventricular tachycardia (VT) on admission, suggesting LV apical posterior wall origin of VT. CT, computed tomography. |
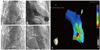 | Fig. 2(A and B) Left ventriculograms of LAO 35° (B) and RAO 35° views. Due to severe mid-septal hypertrophy, the LV had an hourglass-like morphology showing apical ballooning. (C and D) Catheter positions of ablation site (marked with asterisk) in LAO 35° (C) and RAO 35° views (D) match to the margin of apical ballooning due to significant mid-septal hypertrophy. (E) Electroanatomical activation map revealed that the earliest activation site of VT was located at the apical posteroseptum of the LV at the border of apical ballooning. LAO, left anterior oblique view; RAO, right anterior oblique view; VT, ventricular tachycardia. |
ACKNOWLEDGEMENTS
This work was supported by a grant (A085136) from the Korea Health 21 R&D Project, Ministry of Health and Welfare and a grant (2010-0010537) from the Basic Science Research Program run by the National Research Foundation of Korea (NRF) which is funded by the Ministry of Education, Science and Technology of the Republic of Korea.
References
1. Jeyaraj D, Wilson LD, Zhong J, Flask C, Saffitz JE, Deschênes I, et al. Mechanoelectrical feedback as novel mechanism of cardiac electrical remodeling. Circulation. 2007. 115:3145–3155.

2. Sadoshima J, Izumo S. The cellular and molecular response of cardiac myocytes to mechanical stress. Annu Rev Physiol. 1997. 59:551–571.





 PDF
PDF ePub
ePub Citation
Citation Print
Print



 XML Download
XML Download