Abstract
Nail changes are common side effects of taxane chemotherapeutic agents. Docetaxel (Taxotere®) is known to cause a great incidence of nail change. Various types of nail changes have previously been reported as a result of treatment with taxanes. We describe 2 cases of severe nail changes induced by docetaxel. The patients had previously been diagnosed with breast cancer and advanced gastric cancer, respectively. During the course of treatment with docetaxel, nail changes became apparent in both patients. Initially, they complained of nail bed purpura. Subungual hematomas with hemopurulent discharge were later observed in several fingers. Drainage of the hemopurulent material occurred spontaneously in our cases, leading to onycholysis. Following drainage, the pain in the nail with subungual hemoprulent material was relieved immediately and spontaneous healing of the patients' nails was noticed after few months. Subungual hemorrhage and suppuration therefore are considered causes of onycholysis and the pain in these patients. Although systemic or topical antibiotics were not used to treat these patients, antibiotics may be also worthwhile to hasten the drainage of the subungual hematomas and suppuration in patients for quick relief of pain.
Docetaxel (Taxotere®) is a semi-synthetic, taxane chemotherapeutic agent used widely in the treatment of various cancers including ovarian, breast and lung cancer.1-3 Taxanes are usually administered intravenously once every 3 weeks, but weekly administration is also common. The most common dose-limiting toxicity is known as myelosuppression.1,2 Other side effects include asthenia/fatigue, alopecia, cutaneous reactions, stomatitis, hypersensitivity reactions and a fluid-retention syndrome.1,2 Cutaneous reactions such as erythematous pruritic maculopapular rash, dry skin, palmoplantar erythrodysesthesia and desquamation may occur in as many as 50-70% of patients.4 The incidence of patients developing nail changes ranges from 0% to 44%.5 Here we report 2 cases in which severe nail changes developed in patients while using docetaxel once every 3-weeks.
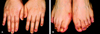
The first patient was a 43-year-old female who was previously diagnosed with breast cancer in 1994. The patient subsequently underwent radical mastectomy of her left breast. She received 6 cycles of first-line chemotherapy with cyclophosphamide, methotrexate and 5-fluorouracil (5-FU) followed by radiotherapy, which resulted in complete remission of the disease. In 2002, a metastasis on her right rib was found in a whole body bone scan. She received pamidronate injections without any improvement. The patient then began receiving chemotherapy with docetaxel. After a cumulative dose of 240mg/m2, she developed nail changes as a prominent adverse side effect. Initially, nail bed purpura appeared on several fingernails. Then subungual hema-tomas with hemopurulent discharge were also observed. Drainage of the hemopurulent discharge occurred spontaneously without any treatment, leading to onycholysis. Four months after the patient began docetaxel treatments, we observed the following changes in the nails of all the digits in both hands and feet: dyschromasia, dystrophy, onycholysis, hemorrhages, and subungual hematomas (Fig. 1A and Fig. 1B). A fungus study revealed no evidence of onychomycosis.
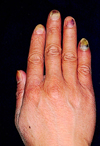
The second patient was a 50-year-old male who was diagnosed with advanced gastric cancer in 2002. The patient underwent radical total gastrectomy with esophago-jejunostomy followed by post-operative adjuvant chemotherapy of 5-FU and carboplatin. Following 12 cycles of 5-FU and carboplatin infusion, a change of regimen was recommended due to poor clinical response. The patient then began four months of chemotherapy with docetaxel. After 4 cycles of docetaxel treatment, he developed bilateral finger paresthesia and painful subungual hematomas with suppuration. The drainage of subungual hemopurulent material occurred spontaneously. Upon drainage completion, pain subsided without antibiotic treatment. The damage to the patient's nails subsequently lead to onycholysis. Nail changes in all the digits in both hands and both 1st toes observed in the dermatology clinic included onycholysis, hemorrhage, nail bed discoloration and subungual hematomas with suppuration (Fig. 2). A gram stain of the hemopurulent material showed numerous white blood cells. Although many Streptococcus, Staphylococcus, Morganella morganii and Acinebacter baumannii were cultured from the purulent material from this patient, an absence of periungual inflammation along with spontaneous improvement following drainage was observed.
Nail changes are a relatively common side effect of systemic chemotherapy. Taxanes such as docetaxel and paclitaxel appear to cause nail changes more frequently than other chemotherapeutic agents. Nail changes related to docetaxel treatment include nail bed purpura, onycholysis, nail pigmentation, splinter hemorrhage, subungual abscess, Beau's line, acute paronychia and hemorrhagic onycholysis.4-12 'Hemorrhagic onycholysis' refers to the combination of subungual discharge of hemopurulent material and subsequent onycholysis.8 Such nail changes during docetaxel treatment are usually not severe, but subungual hematomas and hemorrhagic onycholysis can occur, leading to an impaired quality of life or to a discontinuation of chemotherapy. Direct nail bed toxicity or inhibition of nail bed angiogenesis related to taxane-mediated effects are suggested to be possible mechanisms leading to onycholysis.9,10 Considering that pain was reduced following spontaneous drainage of the subungual hemopurulent material, pressure effect due to hemorrhage seems to be the more direct cause for pain in these patients. A neurogenic mechanism for nail change was also suggested by the absence of nail changes in the denervated hands.13,14 Nail changes occur after several cycles of docetaxel chemotherapy with a tendency to resolve gradually over a few weeks, despite continued treatment.8 Currently, there are no known preventive measures for the nail changes.4 As these nail changes are prone to bacterial infection in the case of an immunosuppressed state induced by chemotherapy, some recommend a topical antiseptic treatment.13 Severe paronychia or subungual abscess due to a secondary infection should be treated with systemic antibiotics.14 Although we did not use any antibiotics for these patients, it may be also worthwhile to use topical or systemic antibiotics to hasten the drainage of the subungual hematomas and suppuration in patients for quick relief of pain. Therefore, it is important for the clinician to recognize nail changes early in order to manage them properly and to prevent the unnecessary discontinuation of chemotherapy.
Figures and Tables
References
1. Chevallier B, Fumoleau P, Kerbrat P, Dieras V, Roche H, Krakowski I, et al. Docetaxel is a major cytotoxic drug for the treatment of advanced breast cancer: a phase II trial of the Clinical Screening Cooperative Group of the European Organization for Research and Treatment of Cancer. J Clin Oncol. 1995. 13:314–322.
2. Francis P, Schneider J, Hann L, Balmaceda C, Barakat R, Phillips M, et al. Phase II trial of docetaxel in patients with platinum-refractory advanced ovarian cancer. J Clin Oncol. 1994. 12:2301–2308.
3. Fossella FV, Lee JS, Murphy WK, Lippman SM, Calayag M, Pang A, et al. Phase II study of docetaxel for recurrent or metastatic non-small-cell lung cancer. J Clin Oncol. 1994. 12:1238–1244.
4. Pavithran K, Doval DC. Nail changes due to docetaxel. Br J Dermatol. 2002. 146:709–710.
5. Minisini AM, Tosti A, Sobrero AF, Mansutti M, Piraccini BM, Sacco C, et al. Taxane-induced nail changes: incidence, clinical presentation and outcome. Ann Oncol. 2003. 14:333–337.
6. Correia O, Azevedo C, Pinto Ferreira E, Braga Cruz F, Polonia J. Nail changes secondary to docetaxel (Taxotere). Dermatology. 1999. 198:288–290.
7. Rafi L, Friedrich M, Tilgen W, Reichrath J. Severe nail changes due to Docetaxel treatment. Eur J Dermatol. 2003. 13:610–611.
8. Nicolopoulos J, Howard A. Docetaxel-induced nail dystrophy. Australas J Dermatol. 2002. 43:293–296.
9. Flory SM, Solimando DA Jr, Webster GF, Dunton CJ, Neufeld JM, Haffey MB. Onycholysis associated with weekly administration of paclitaxel. Ann Pharmacother. 1999. 33:584–586.
10. Vanhooteghem O, Andre J, Vindevoghel A, Vandenbossche L, Vandeveire A, Song M. Docetaxel-induced subungual hemorrhage. Dermatology. 1997. 194:419–420.
11. Ghetti E, Piraccini BM, Tosti A. Onycholysis and subungual haemorrhages secondary to systemic chemotherapy (paclitaxel). J Eur Acad Dermatol Venereol. 2003. 17:459–460.
12. Vanhooteghem O, Richert B, Vindevoghel A, Vandenbossche L, Vandeveire A, de la Brassinne M. Subungal abscesses: a new ungual side-effect related to docetaxel therapy. Br J Dermatol. 2000. 143:462–463.
13. Wasner G, Hilpert F, Schattschneider J, Binder A, Pfisterer J, Baron R. Docetaxel-induced nail changes--a neurogenic mechanism: a case report. J Neurooncol. 2002. 58:167–174.
14. Wasner G, Hilpert F, Baron R, Pfisterer J. Clinical picture: nail changes secondary to docetaxel. Lancet. 2001. 357:910.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download