Dear Editor,
IgG4-related disease (RD) is a systemic immune-mediated syndrome characterized by mass-forming lesions in one or more exocrine glands or other extranodal sites caused by lymphoplasmacytic infiltrates and sclerosis. Certain autoimmune diseases and inflammatory disorders, such as rheumatoid arthritis, Hashimoto's thyroiditis, and Sjögren's syndrome, have been shown to be associated with lymphoma [1]. Although little is known about lymphomagenesis with regard to IgG4-RD, a few articles about orbital malignant lymphoma associated with IgG4-RD have been published [234]. However, most of these articles are related to ocular adnexal lymphoma in the lacrimal gland. We describe herein the first case of incipient mucosa-associated lymphoid tissue (MALT) lymphoma arising in a case of IgG4-related sclerosing orbital inflammation surrounding the optic nerve.
A 53-year-old male visited Severance Hospital for evaluation of bilateral proptosis and periorbital eyelid swelling for 3 months. The patient had a history of chronic sinusitis, pitting edema in the extremities, and intermittent dyspnea when walking and laying down. The patient did not complain of either diplopia or ocular pain. An ophthalmic examination revealed that visual acuity, pupillary reaction, intraocular pressure, and fundus were within normal limits; proptosis was bilaterally confirmed as 21.5 mm by Hertel exophthalmometry. Initial orbital computed tomography showed diffuse thickening of the extraocular muscles and a retrobulbar dense infiltration along the optic nerve, which was more severe in the right eye than in the left eye (Fig. 1A-1C).
As we suspected the lesion to be bilateral, idiopathic, orbital inflammation, we began oral steroid treatment. After treatment with 40 mg oral prednisolone daily, periorbital swelling of the eyelids and other sites markedly subsided. However, whenever the prednisolone dose was tapered to 15 mg or less per day, intermittent ocular pain and eyelid swelling redeveloped and became aggravated. The patient became resistant to even high doses of prednisolone, showing systemic complications of steroids including Cushing's disease and secondary diabetes. Fifteen months after steroid treatment, orbital computed tomography showed an enlarged, lobulated mass in the bilateral retrobulbar area and diffuse, bilateral enlargement of the infraorbital nerve, superior rectus muscles, and lacrimal glands with bilateral paranasal sinusitis (Fig. 1D-1F).
To confirm these histological results and avoid further steroid treatment, we performed debulking of the inflamed orbital mass by orbital fat and bony decompression with biopsy of the lobulated lesion along the optic nerve via canthofornix incision. Although it is challenging to establish overall criteria that are applicable across all organs, recently proposed diagnostic criteria defined IgG4-RD in patients with (1) organ enlargement, mass or nodular lesions, or organ dysfunction; (2) a serum IgG4 concentration >135 mg/dL; and (3) histopathological findings >10 IgG4 cells per high power field and an IgG4+/IgG+ cell ratio >40% [5]. Histologically, the orbital fat in the present case was massively infiltrated with IgG4+ plasma cells. The biopsied lobulated lesion revealed perifollicular (germinal center) infiltration of CD20+ and CD3− monocytoid B-cells associated with IgG4+ plasma cell infiltrates, consistent with incipient marginal zone B-cell lymphoma of MALT (Fig. 1J-1L). In addition, the tissue IgG4+/IgG+ plasma cell ratio was 62%; the number of IgG4+ cells/HPF was 124; serum IgG4 level was 766.2 mg/dL; and the serum IgG4/IgG ratio was 22.5%. These findings are compatible with a definitive diagnosis of IgG4-related orbital disease. Histology of the lymph nodes showed reactive follicular hyperplasia, and a renal biopsy showed acute interstitial nephritis with massive IgG4+ plasma cell and eosinophil infiltration. The patient received a total dose of 27 Gy (1.8 Gy per fraction for 15 fractions) orbital radiotherapy over 3 weeks and also was administered 60 mg of oral steroids and azathioprine. After radiotherapy and steroid treatment following debulking surgery, the retrobulbar orbital mass markedly decreased, the generalized edema resolved, and most serologic tests were within normal limits (Fig. 1G-1I).
Autoimmune diseases and chronic inflammation have been found to be associated with lymphoma [1]. Recent studies suggest that IgG4+ plasma cells might be involved in the pathogenesis of MALT lymphoma [234]. Igawa et al. [3] have suggested that some IgG4-producing lymphomas may be derived from pre-existing IgG4-RD. In addition, Yamamoto et al. [4] observed malignant transformation of lymphocytes in two of 106 patients with extranodal IgG4-RD over an average observation period of 3.1 years. We present incipient MALT lymphoma arising in a case of IgG4-related sclerosing orbital inflammation surrounding the optic nerve. In cases of orbital inflammation with systemic symptoms, especially steroid-dependent and relapsed cases, we must rule out IgG4-RD via biopsy and confirm whether the inflammation has systemic involvement. When complications due to steroid administration become intolerable and the abatement of symptoms is insufficient despite high-dose administration, surgical debulking with adjuvant radiotherapy and use of corticosteroids and immunosuppressants can be effective for remission.
Figures and Tables
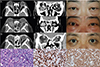 | Fig. 1(A,B) Initial computed tomography (CT) shows diffuse thickening of the extraocular muscles and a dense retrobulbar infiltration around the optic nerve that is more severe in the right eye than the left eye. (C) Bilateral periorbital swelling is shown. (D,E) Preoperative CT shows an increase in the size of the lobulated mass in the bilateral orbit and retrobulbar area and diffuse enlargement of the bilateral infraorbital nerve and bilateral superior rectus muscles. Additionally, a slight increase in the size of the bilateral lacrimal glands and bilateral paranasal sinusitis are shown. (F) Signs of inflammation, such as conjunctival injection, caruncle injection and swelling, proptosis, and periorbital swelling are apparent. (G,H) Three months after debulking surgery, CT shows a much decreased size of the retrobulbar mass, thickening of the extraocular muscles, and improvement in the dense retrobulbar infiltration. Moreover, the increased volume of the orbital cavity, owing to medial and inferior orbital wall decompression surgery, is shown. (I) Proptosis and periorbital swelling show improvement and there are no signs of inflammation. (J) Hematoxylin and eosin staining reveals monomorphous small-to-medium-size lymphoid cells and plasma cells without significant atypia (×100). (K) Immunohistochemical staining reveals mild perifollicular expansion of CD20+ B-cells (×100). (L) Immunostaining of IgG4 shows many IgG4-positive plasma cells with a high ratio of IgG4-positive plasma cells: IgG-positive plasma cells (~60%) (×200). |
References
1. van den Brand M, van Krieken JH. Recognizing nodal marginal zone lymphoma: recent advances and pitfalls. A systematic review. Haematologica. 2013; 98:1003–1013.
2. Lee MJ, Kim N, Choe JY, et al. Clinicopathological analysis of ocular adnexal extranodal marginal zone B-cell lymphoma with IgG4-positive cells. PLoS One. 2015; 10:e0131458.
3. Igawa T, Hayashi T, Ishiguro K, et al. IgG4-producing lymphoma arising in a patient with IgG4-related disease. Med Mol Morphol. 2016; 49:243–249.
4. Yamamoto M, Takahashi H, Tabeya T, et al. Risk of malignancies in IgG4-related disease. Mod Rheumatol. 2012; 22:414–418.
5. Umehara H, Okazaki K, Masaki Y, et al. Comprehensive diagnostic criteria for IgG4-related disease (IgG4-RD), 2011. Mod Rheumatol. 2012; 22:21–30.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download