Dear Editor,
Chronic infantile neurological cutaneous articular (CINCA) syndrome is a rare inflammatory disease that consists of a triad of neonatal onset cutaneous symptoms, meningitis, and joint manifestations with recurrent fever and inflammation [1]. We report a patient with acute-on-chronic ocular inflammation associated with intraocular pressure surge together with imaging findings.
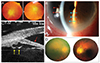
A 45-year-old Chinese man was referred to the eye clinic for dry eye evaluation, with suspicion of Sjogren's syndrome in 2004. Ophthalmological findings were unremarkable except for blurred optic disc margins (Fig. 1A). Further work-up was prompted by a compatible history of neonatal onset urticarial rash, periodic fever, joint deformities, and sensorineural hearing loss. Genetic tests showed heterozygous missense mutation in exon 3 of the CIAS1 gene, diagnostic of CINCA syndrome.
The patient presented again in February 2013 with right eye redness and decreased visual acuity (VA) for 2 days. Intraocular pressure was 44 mmHg and VA 3 / 60. The anterior chamber was deep and irides were flat, without obvious pupil block (e.g., iris bombé or seclusio pupillae). Gonioscopy of his right eye revealed no angle structures 360°, with no peripheral anterior synechiae, neovascularisation, or double-hump sign. His left eye showed 270° Shaffer grade 0, inferior 90° grade 1, and no double hump sign. There were bilateral cataracts, which was more severe on the right. He was treated as 'acute angle closure attack' of the right eye, and received intravenous acetazolamide, pilocarpine, and steroid eye-drops, resulting in rapid intraocular pressure normalization. He later underwent bilateral laser iridotomy and argon laser iridoplasty, after which post-laser gonioscopy revealed persistent angle closure with Shaffer grading 0 to 1. Further follow-ups showed peripheral corneal stromal opacification, mild bilateral intermittent anterior chamber activity with cells and flare, and chemosis (Fig. 1B). Ultrasound biomicroscopy confirmed invisibility of the scleral spur with flat irides, no anterior rotation of the ciliary body, and incidental findings of small iridociliary cysts in the right eye 9 o'clock and the left eye 6 o'clock positions (Fig. 1C). He then received right eye phacoemulsification, intraocular lens implantation, and posterior subtenon triamcinolone injection 4 mg. Best corrected VA improved to 0.3, and both fundi showed pale optic discs with blurry margins surrounded by ghost vessels (Fig. 1D). He was maintained on daily oral prednisolone 5 mg and loteprednol etabonate 0.5% eye-drops, and there was no recurrence of hypertensive episodes 22 months after the operation, although the postoperative gonioscopic appearance remained the same.
A wide variety of ocular disturbances have been described in association with CINCA syndrome, with poor correlation between ocular and systemic severity. Dollfus et al. [2] conducted the largest review of cases to date, with anterior uveitis, episodic redness, and corneal involvement being the most common anterior segment abnormalities. Among posterior segment changes, pseudopapilloedema, optic disc elevation, and optic atrophy predominate (83%). VA was moderately to severely affected in 27% of the cases in that study. Other sporadic cases describe ocular changes such as keratitis and corneal infiltrates [34]. Our patient had features of uveitis, but his closed angle was more likely due to congenital structural malformations rather than recurrent inflammatory changes, as evidenced by flat irides without peripheral anterior synechiae or pupillary block. To our knowledge, this is the first documented case of CINCA syndrome with acute ocular hypertension. Ultrasound biomicroscopy findings were atypical of primary angle closure. We postulate that the hypertensive episode was due to a compromised angle anatomy perpetuated by inflammation. Regular surveillance of visual function is mandatory for preserving vision in such patients.




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download