Abstract
Purpose
To document the clinical features of disc hemorrhage in patients with branch retinal vein occlusion (BRVO) and normal tension glaucoma (NTG), and to evaluate the relationship between BRVO and NTG with disc hemorrhages.
Methods
From July 2001 to May 2006, sixteen patients with both NTG and BRVO in different eyes were successively collected from outpatient population of Seoul National University Hospital in this observational case series. The frequency and location of disc hemorrhages, history of associated systemic diseases, and the order of the time of diagnosis between NTG and BRVO were studied.
Results
All patients had unilateral BRVO, and their mean age was 63.3±10.6 years. Disc hemorrhages were detected in eight patients (50%) during the mean follow-up of 26.8 months (range, 3-96 months). Six patients (75%) had disc hemorrhages in the non-BRVO eyes and two patients (25%) in BRVO eyes. Five hemorrhages (62.5%) were located at inferior-temporal quadrant of the optic disc. History of systemic hypertension was identified in 12 patients (75.0%). In 11 patients (68.8%), NTG was diagnosed at the same time as BRVO.
A small, isolated, often splinter-shaped hemorrhage may be present on the optic disc in some eyes, especially those with open-angle glaucoma.1-4 Disc hemorrhages in glaucoma are considered to be a sign of imminent retinal nerve fiber defects and a potential risk factor of associated visual field deterioration.5 They are more prevalent in normal tension glaucoma (NTG) than in other types of glaucoma.3,5 These findings raise the possibility of a vascular causative factor in this disease. The pathogenesis of disc hemorrhage is not yet fully understood. Which vessels do disc hemorrhages originate from, e.g., arterioles, venules or capillaries? Why they are located at the border of the optic disc with a predilection for superior-temporal and inferior-temporal regions?
Also, the pathogenesis of open angle glaucoma is not fully known. Primary open angle glaucoma (POAG) and NTG appear to represent a continuum of open angle glaucoma in which the mechanism of glaucomatous optic neuropathy shifts from predominantly elevated intraocular pressure (IOP) in the former to additional IOP independent factors, i.e. a vascular ischemic effect in the latter, with considerable overlap of causative factors.6
In the literature, there is an interesting report that there is a close association of open angle glaucoma with disc hemorrhage and retinal vein occlusion.7 Some associations have been recognized between ocular hypertension or POAG and retinal vein occlusion, especially central retinal vein occlusion (CRVO).8-11 However, branch retinal vein occlusion (BRVO) does not seem to be related to increased intraocular pressure or POAG.12-14
There has been no report dealing with NTG with disc hemorrhage in BRVO patients except one case report which described four cases of NTG with disc hemorrhage combined with BRVO in the contralateral eye.15 In the present study, we report on a consecutive case series of patients with both BRVO and NTG in different eyes, and document the clinical features of disc hemorrhage in those patients and the relationship between NTG with disc hemorrhages and BRVO.
The study was in adherence to the tenets of the Declaration of Helsinki and was approved by our Institutional Review Board. From July 2001 to May 2006, patients with both NTG and BRVO who met the eligibility criteria stated below were successively collected from outpatient glaucoma clinic population of Seoul National University Hospital and medical records were reviewed. Patients who met both of following two eligibility criteria were recruited: (1) presence of BRVO in one eye, as diagnosed by retina specialists at our hospital; and (2) presence of NTG in the fellow eye or both eyes. Patients with hemicentral retinal vein occlusion, central retinal vein occlusion, bilateral branch retinal vein occlusions, optic neuritis, anterior ischemic optic neuropathy, diabetic retinopathy, or any other retinal vascular disorder capable of causing retinal hemorrhages were excluded from the study.
All subjects underwent a comprehensive ophthalmologic examination, including measurement of best corrected visual acuity, intraocular pressure measurement by a Goldmann applanation tonometry (Haag-Streit AG, Liebefeld, Switzerland), slit-lamp biomicroscopy, gonioscopy, and fundus examination using a 78D lens. Fluorescein angiography, color disc photography and red-free retinal nerve fiber layer (RNFL) photography (CF-60UVi, Canon Inc., Utsunomiya, Japan) were acquired. Visual field examinations were done using the C30-2 program in the Humphrey Visual Field Analyzer (model 750, Zeiss Inc., San Leandro, CA). Routine medical histories included associated systemic diseases such as diabetes and systemic hypertension, systemic medications, and family histories. Every 3 months, measurement of visual acuity and intraocular pressure, and dilated fundus examination, especially for searching disc hemorrhages, were done.
Patients were regarded as having BRVO if a fundus examination showed flame-shaped or dot-like hemorrhages in the distribution of occluded branch retinal vein with an apex of the obstructed tributary system located at an arteriovenous crossing. In addition, patients were regarded as having BRVO if the retinal hemorrhages had resolved and new vessels or collateral vessels, that suggest a previous vascular occlusive attack, appeared. NTG was diagnosed when the following criteria were fulfilled: (1) a wedge-shaped or diffuse retinal nerve fiber layer (RNFL) defect in an RNFL photograph, (2) an intraocular pressure consistently lower than 21 mmHg without medication over at least five consecutive measurements, (3) an open angle by gonioscopy, and (4) absence of secondary causes for glaucomatous optic neuropathy. In eyes with BRVO, RNFL defects at the quadrant affected by BRVO were excluded from the diagnosis of NTG. Disc hemorrhage was defined as an isolated hemorrhage on the optic disc tissue or in the peripapillary retina reaching the disc rim and those located at the same quadrants involved by BRVO were also excluded form the study. Cup-to-disc (C/D) ratio was defined as the ratio between the vertical diameter of the optic cup and that of the optic disc measured though the center of the optic disc.
We documented the retinal quadrants segmentally involved by BRVO, the frequency and location of disc hemorrhages, and the order of the time of detections between NTG and BRVO in the patients. In addition, we compared intraocular pressure, C/D ratio, visual field indices (mean deviation and pattern standard deviation) between BRVO eyes without NTG and contralateral non-BRVO eyes with NTG. Statistical analysis was performed using the Mann-Whitney test in MedCalc version 9.0 (MedCalc Software, Mariakerke, Belgium). P values of <0.05 were considered statistically significant.
Twenty one patients were collected during the recruiting period of 59 months. However, among those, five patients were excluded from the study because of diabetic retinopathy (two patients), bilateral BRVO (two patients), and combined branch retinal artery occlusion (one patient), and the remaining sixteen patients were included in this study. Table 1 summarizes their clinical characteristics. Their mean age±standard deviation was 63.3±10.6 (range, 36-75) years. There were seven men and nine women. Twelve patients had unilateral BRVO and unilateral NTG in different eyes. The other four patients had unilateral BRVO and bilateral NTG. Patients were followed up for an average of 26.8 (range 3-96) months. Twelve patients (75.0%) had histories of systemic hypertension and two patients (12.5%) had histories of diabetes. All patients in the study were Korean.
The sites of all retinal vein occlusion were at the arteriovenous crossings in all patients. The most frequent quadrants of retina of the segmentally involved BRVO was the inferior-temporal (37.5%) and superior-temporal quadrants (43.7%). During the follow-up period, disc hemorrhages were detected in eight patients (50.0%). Six (75%) of these patients had disc hemorrhages in the non-BRVO eyes with NTG (Fig. 1) and two patients (25%) had disc hemorrhages in the eyes with BRVO, which were in the opposite hemispheres each other (Fig. 2). All disc hemorrhages were located at the temporal side, especially the inferior-temporal quadrant (Table 2).
No significant differences were observed in the intraocular pressure, C/D ratio, and visual field indices between BRVO eyes without NTG and contralateral non-BRVO eyes with NTG (Table 3). In 11 patients (68.8%), NTG was diagnosed when BRVO was detected. In four patients (25.0%), BRVO was diagnosed first and NTG later during the follow-up (range, 2-15 years). In only one patient (6.3%), NTG was diagnosed first and BRVO later during a follow-up of 6 years.
The present study documented that the incidence of disc hemorrhages was 50% in patients with both NTG and BRVO during the mean follow-up period of 2.2 years: 25% of these were in the BRVO eyes and 75% were in the contralateral non-BRVO eyes with NTG. Because disc hemorrhages last for about 8 days to 12 weeks after initial bleedings16 and the patients are actually not seen frequently enough to detect each and every hemorrhage occurring in these eyes, the incidence of disc hemorrhage in glaucoma patients varies from study to study. Therefore, it is difficult to compare the incidence of disc hemorrhage among different studies and it may be a matter of chance that one happens to see the patient when there is a disc hemorrhage. At initial examination, only one patient revealed a disc hemorrhage in non-BRVO eye. During the follow up of every 3 months, seven patients revealed splint or flame shaped hemorrhages on the optic disc.
Several population-based surveys reported that the overall prevalence rates of disc hemorrhages were from 0.9% to 1.4%.17-19 In addition to the prevalence rates, the cumulative incidences of disc hemorrhages were reported. In a study, a cumulative incidence of disc hemorrhages in patients with NTG was 35.3% during a mean follow-up period of 7.3±2.5 years.20 Although direct comparison of our results with that of previous study is difficult as stated above, the incidence of disc hemorrhages in our study was higher (50%) in the face of shorter mean follow up period (2.2 years) compared with that of the previous report (7.3 years). This finding may correspond with previous studies which reported that disc hemorrhages, retinal vein occlusion (RVO), and open angle glaucoma occur in the same patient.7,21,22 Sonnsjo and Krakau proposed that disc hemorrhage and RVO may be the same phenomenon of one disease process, and that observed differences are attributable to the size of affected vessels.7,22 As the pathogeneses of CRVO and BRVO are totally different, their findings, based on studies in which CRVO and BRVO patients were grouped together, may be mostly not relevant to results for BRVO, as in this study. Also, their studies regarded both POAG and NTG as open angle glaucoma. On the other hand, our study included only NTG which is known to be the most prevalent subtype of glaucoma among Koreans.23
As expected from the findings of several pervious studies that reported the frequency of disc hemorrhages in glaucoma patients,19,20 all disc hemorrhages were found in the inferior-temporal and superior-temporal regions. Patients had a more frequent history of systemic hypertension compared with those in patients only with glaucoma. Also, this result was similar to our expectation which was based on the result of previous study about the risk factors of BRVO.13
With regard to the pathogenesis of disc hemorrhage, a question arises whether disc hemorrhages have their origin in the arterioles, venules, or the capillaries of the peripapillary radial network on the surface of the peripapillary retina.24 NTG may be due to arterial insufficiency in the optic nerve head which is supplied by the posterior ciliary arteries.3 Because BRVO almost always occurs at arteriovenous crossings,25,26 underlying arterial disease may play a causative role. Our results show a high incidence of disc hemorrhage in patients with both NTG and BRVO, leading us to think that some cases of NTG, which have higher frequency of disc hemorrhage than other type of glaucoma, may share a common vascular pathophysiology with BRVO. However, we do not show that the actual prevalence of NTG in our clinic population with BRVO is higher than that seen in the general population, and our study has several important limitations, mostly stemming from its small sample size and lack of any control group. It is also limited because the patients included were hospital-based cases and of Korean ethnicity. Thus, it may be difficult to generalize the results of this study. To confirm our findings, it should be investigated by well designed case-control studies that BRVO is more prevalent in NTG patients than normal population.
To diagnose and confirm NTG in all patients, we used a red-free RNFL photography rather than a standard automated perimetry, which may be affected by the segmentally distributed retinal hemorrhages or retinal ischemia that develop during the course of BRVO. RNFL defects were also identified at 50% of the quadrants affected by BRVO and these defects were excluded in the diagnosis of NTG. These eyes showed a characteristic retinal appearance of chronic phase BRVO, i.e., collateral vessels and new vessels. It appears that the ischemic effect due to BRVO may induce retinal nerve fiber layer defects and deformities of optic disc at the corresponding sites. Therefore, there was no significant difference in IOP, C/D ratio, and visual field indices in comparison of 12 eyes with BRVO without NTG and 16 contralateral non-BRVO eyes with NTG (Table 3). BRVO was diagnosed by retina specialists at our hospital, and patients with BRVO were referred to us for the evaluation of suspicious change in the optic nerve head found at the time of diagnosis or during the work-up period for BRVO. In most patients, NTG was diagnosed concurrently at the detection time of BRVO. Even when the medical records of four patients in whom BRVO was detected firstly were reviewed, the findings attributable to glaucomatous optic neuropathy were already present at the detection of BRVO. Since NTG is a chronically progressing disease, these findings imply that patients had NTG before BRVO, and correspond with the results of earlier studies.27
We propose that some cases of NTG, which have higher frequency of disc hemorrhage than other type of glaucoma, may share a common vascular pathophysiology with BRVO. However, to confirm our conclusion, well designed case-control studies should be performed since our study is a case series without any control. Because NTG has no alarming symptoms until far advanced, BRVO may be the first encountered sign of NTG, like disc hemorrhages. Therefore, the optic disc of both eyes should be carefully examined to detect disc hemorrhages or other early glaucomatous changes together with RNFL photography during the evaluation of unilateral BRVO.
Figures and Tables
Fig. 1
Retinal nerve fiber layer (RNFL) photographs of a 67 year-old female patient (Case 10). (A) Right eye shows a small wedge shape RNFL defect (arrowheads) with a disc hemorrhage (white arrow) at 11 o'clock of disc. (B) Left eye shows features of chronic phase branch retinal vein occlusion (BRVO), i.e., vascular sheathing, epiretinal membrane, and collateral vessels that note a previous event of BRVO at superior nasal quadrant of retina.
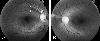
Fig. 2
Retinal nerve fiber layer (RNFL) photographs and fluorescein angiogram of a 73 year-old male patient (Case 1). (A) Right eye shows a small, splint hemorrhage at 7 o'clock of disc (white arrow), and vascular sheathing and retinal hemorrhages at superior temporal quadrant. Fluorescein angiography of right eye (inset picture), taken 3 months prior to RNFL photographies, shows a venous filling delay at superior temporal quadrant. (B) Left eye shows diffuse thinning of RNFL.
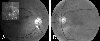
Table 1
Clinical characteristics of sixteen cases recruited in this study

BRVO=branch retinal vein occlusion, NTG=normal tension glaucoma, DH=disc hemorrhage, IOP=intraocular pressure, CDR=cup-to-disc ratio, DM=diabetes mellitus, HTN=systemic hypertension, R=right eye, L=left eye, B=both eyes, ST=superior-temporal, IT=inferior-temporal, IN=inferior-nasal, SN=superior-nasal.
References
1. Susanna R, Drance SM, Douglas GR. Disc hemorrhage in patients with elevated intraocular pressure. Occurrence with and without field changes. Arch Ophthalmol. 1979. 97:284–285.
2. Bengtsson B, Holmin C, Krakau CE. Disc haemorrhage and glaucoma. Acta Ophthalmol (Copenh). 1981. 59:1–14.
3. Kitazawa Y, Shirato S, Yamamoto T. Optic disc hemorrhage in low-tension glaucoma. Ohthalmology. 1986. 93:853–857.
4. Diehl DLC, Quigley HA, Miller NR, et al. Prevalence and significance of disc hemorrhage in a longitudinal study of glaucoma. Arch Ophthalmol. 1990. 108:545–550.
5. Ishida K, Yamamoto T, Sugiyama K, et al. Disk hemorrhage is a significantly negative prognostic factor in normal-tension glaucoma. Am J Ophthalmol. 2000. 129:707–714.
6. Allingham RR. Allingham RR, Damji K, Freedman S, editors. Chronic open-angle glaucoma and normaltension glaucoma. Shield's textbook of glaucoma. 2005. 5th ed. Philadelphia: Lippincott Williams & Wilkins;chap. 11.
7. Sonnsjo B, Krakau CE. Arguments for a vascular glaucoma etiology. Acta Ophthalmol (Copenh). 1993. 71:433–444.
8. Soni KG, Woodhouse DF. Retinal vascular occlusion as a presenting feature of glaucoma simplex. Br J Ophthalmol. 1971. 55:192–195.
9. Frucht J, Shapiro A, Merin S. Intraocular pressure in retinal vein occlusion. Br J Ophthalmol. 1984. 68:26–28.
10. Beaumont PE, Kang HK. Cup-to-disc ratio, intraocular pressure, and primary open-angle glaucoma in retinal venous occlusion. Ophthalmology. 2002. 109:282–286.
11. Hayreh SS, Zimmerman MB, Beri M, et al. Intraocular pressure abnormalities associated with central and hemicentral retinal vein occlusion. Ophthalmology. 2004. 111:133–141.
12. Luntz MH, Scjenker HI. Retinal vascular accidents in glaucoma and ocular hypertension. Surv Ophthalmol. 1980. 25:163–167.
13. Risk factors for branch retinal vein occlusion. Am J Ophthalmol. 1993. 116:286–296.
14. Klein BE, Meuer SM, Knudtson MD, et al. The relationship of optic disc cupping to retinal vein occlusion: The beaver dam eye study. Am J Ophthalmol. 2006. 141:859–862.
15. Kim SJ, Park KH. Four cases of normal-tension glaucoma with disk hemorrhage combined with branch retinal vein occlusion in the contralateral eye. Am J Ophthalmol. 2004. 137:357–359.
16. Heijl A. Frequent disk photography and computerized perimetry in eyes with optic disk haemorrhage. Acta Ophthalmol. 1986. 64:274–281.
17. Klein BE, Klein R, Sponsel WE, et al. Prevalence of glaucoma. The Beaver Dam Eye Study. Ophthalmology. 1992. 99:1499–1504.
18. Healey PR, Mitchell P, Smith W, et al. Optic disc hemorrhages in a population with and without signs of glaucoma. Ophthalmology. 1998. 105:216–223.
19. Yamamoto T, Iwase A, Kawase K, et al. Optic disc hemorrhages detected in a large-scale eye screening project. J Glaucoma. 2004. 13:356–360.
20. Hendrickx KH, van den Enden A, Rasker MT, Hoyng PF. Cumulative incidence of patients with disc hemorrhages in glaucoma and the effect of therapy. Ophthalmology. 1994. 101:1165–1172.
21. Rubinstein K, Jones EB. Retinal vein occlusion: long-term prospects, 10 years follow-up on 143 patients. Br J Ophthalmol. 1976. 60:148–150.
22. Sonnsjo B. Similarities between disc haemorrhages and thrombosis of the retinal veins. Int Ophthalmol. 1992. 16:235–238.
23. Lee JB, Cho YS, Choe YJ, Hong YJ. The prevalence of glaucoma in Korean adults. J Korean Ophthalmol Soc. 1993. 34:65–69.
24. Alterman M, Henkind P. Radial peripapillary capillaries of the retina:II. Possible role in Bjerrum scotoma. Br J Ophthalmol. 1968. 52:26–31.
25. Duker JS, Brown GC. Anterior location of the crossing artery in branch retinal vein occlusion. Arch Ophthalmol. 1989. 107:998–1000.
26. Zhao J, Sastry SM, Sperduto RD, et al. Arteriovenous crossing patterns in branch retinal vein occlusion. The Eye Disease Case-Control Study Group. Ophthalmology. 1993. 100:423–428.
27. Lindblom B. Open angle glaucoma and non-central retinal vein occlusion--the chicken or the egg? Acta Ophthalmol Scand. 1998. 76:329–333.




 PDF
PDF ePub
ePub Citation
Citation Print
Print




 XML Download
XML Download