Abstract
To evaluate the safety and efficacy of the computed tomography coronary angiography (CTCA) for evaluation of acute chest pain in real world population, we prospectively enrolled 296 patients with acute chest pain at emergency department (ED) from November 2005 to February 2007. The patients were grouped based on the clinical information and CTCA result. The patients with a low risk profile and no significant coronary stenosis (>50%) in CTCA were discharged immediately (Group 1, n=103). On the other hand, the patients with an intermediate risk profile without significant stenosis were observed in ED for 24 hr (Group 2, n=104). The patients with significant stenosis underwent further coronary evaluation and management accordingly (Group 3, n=89). While no false negative case was found in Group 1, seven cases (6.73%) were found in Group 2, mostly during the observation period. In Group 3, there were 54 (60.67%) cases of acute coronary syndrome including 10 myocardial infarctions. The overall accuracy of CTCA for acute coronary syndrome was 88.5% (sensitivity), 85.1% (specificity), 60.7% (positive predictive value) and 96.6% (negative predictive value). In conclusion, clinical decision based on CTCA is safe and effective for low risk patients. Further validation is needed in patients with intermediate risk profile.
The evaluation of acute chest pain is a challenging task for physicians who work in emergency departments (EDs). Although complex diagnostic algorithms that combine multiple diagnostic modalities were developed to minimize error (1-3), a high portion (2-6%) of acute coronary syndrome (ACS) patients are being mistakenly discharged from EDs (4-6). This is related to adverse clinical outcomes (4) and responsible for the largest portion of malpractice suits (7).
The recent development of computed tomography coronary angiography (CTCA) provides a high spatial and temporal resolution images non-invasively (8). It provides comprehensive information about the patency of coronary artery, the integrity of great vessels and the lungs (triple rule out) (9, 10). In many comparative studies, targeting a non-ED based population, CTCA already showed its high diagnostic accuracy and high negative predictive value (8).
The application to the patients with an acute chest pain in ED environment is also being actively evaluated. Some recent studies had shown that CTCA is reliable for ruling out an ACS in low risk group. However, previous studies are mostly small observational studies and/or have a narrow spectrum of target population (11-17).
We tried to evaluate the safety and efficacy of the CTCA-based approach for the patients with acute chest pain in real world ED situation.
This study was performed at the urban teaching hospital with more than 44 thousand visits per year (2007) in ED. A total of 1,125 adult patients who visited the ED with acute chest pain was screened from November 2005 to February 2007. Initial clinical evaluation included history taking, physical examination, chest radiography, electrocardiogram (ECG), cardiac biomarker and creatinine level. The patients with high risk clinical profile were excluded after initial evaluation. High risk clinical profile was defined to the following criteria: 1) ST-segment elevation or new onset LBBB, 2) Increased level of serum troponin or CK-MB, 3) Typical chest pain with ischemic ST-T change (ST segment depression >1 mm or T-wave inversion >3 mm), 4) Overt congestive heart failure, recurrent ventricular arrhythmia, 5) Ongoing or recurrent angina at rest or minimal effort, and 6) Proven significant coronary artery disease.
After exclusion of these high risk patients, we determined whether each patient has intermediate or low risk profile. Intermediate risk profile was defined as having any of the following characteristics: 1) Atypical chest pain with any possible ischemic ECG change (mainly ST-segment depression or T-wave inversion), 2) Typical chest pain with normal ECG. And all patients who do not have possible ischemic ECG change nor typical chest pain were considered to have low risk profile.
The cases with definite evidence of non-coronary etiology of chest pain (e.g., newly diagnosed pneumothorax, overt herpes zoster or evident history of acute chest trauma) or which are not eligible for the test (significant arrhythmia, uncontrollable heart rate, contraindication to beta-blocker or hypersensitivity to radiocontrast agent) were also excluded.
Initial evaluation, enrollment and data collection were performed prospectively by trained emergency physician. The data also were reviewed by a cardiologist every week.
The patients with low to intermediate clinical profile and without other exclusion criteria underwent CTCA evaluation with 16 or 64-channel multi-detector computed tomography (MDCT) with ECG gating capability. Heart rate was controlled under 65 bpm with metoprolol. Scan results were analyzed by a radiologist specialized in cardiovascular imaging. CTCA criterion of significant stenosis was defined as more than 50% diameter stenosis of any major coronary arteries.
The patients were classified into three groups according to their clinical characteristics and CTCA reading (Fig. 1): 1) Group I (Immediate discharge group)-No significant coronary stenosis in the CTCA with low risk profile, 2) Group II (ED observation group)-No significant coronary stenosis in the CTCA with intermediate risk profile, 3) Group III (Further work up group)-Any CTCA evidence of significant coronary stenosis with low to intermediate risk profile.
The patients in Group I were immediately discharged from ED with a short-term out-patient department (OPD) follow-up arrangement. The patients in Group II were observed in ED chest pain unit with serial ECG and cardiac biomarker assay. During the observation period, if a patient had recurrent chest pain or dynamic ST-T change or rising cardiac biomarker level, he was admitted and had coronary angiography. When a patient showed no above-mentioned sign and ACS still could not be ruled out, patients underwent further diagnostic test such as treadmill test (TMT) or myocardial single photon emission computed tomography (SPECT). The patients in Group III underwent the coronary angiography in most cases. However, in the cases with intermediate coronary lesions in CTCA, the myocardial SPECT or TMT was also considered.
The follow-up evaluation was done by a cardiologist at outpatient department within one week for all patients discharged from ED. On the follow-up visit, the cardiologist reviewed every detail about ED evaluation and clinical courses after the discharge. If there was any doubt about patient's diagnosis, additional diagnostic modalities were followed accordingly. Any occurrence of major adverse cardiovascular events (MACE), which is defined as death, myocardial infarction, unplanned coronary revascularization, and repeat ED visits or hospitalization for unstable angina, were also monitored during one month of clinical follow-up. After this period, the cardiologist determined whether the patient had ACS or not.
The statistical analysis was performed with the use of STATA 10 software package (StataCorp LP, College Station, TX, USA). We calculated sensitivity, specificity, and positive and negative predictive values of MDCT findings for diagnosis of ACS in whole study group and each clinical risk group. Categorical variables were analyzed with chi-square test. Continuous variables were analyzed with ANOVA. A P value <0.05 was considered significant.
From November 2005 to February 2007, a total of 1,125 patients visited our ED with chief complaint of acute chest pain. High risk patients (n=271), evident non-cardiac etiology of chest pain (n=358) and patients having contraindication for CTCA (n=195) were excluded. As a result, 301 patients were initially enrolled in the registry and underwent CTCA scan. Five (1.7%) cases were excluded from the final analysis according to the poor image quality of CTCA (Fig. 1).
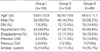
Of the 296 enrolled patients, 103 (34.8%) were classified as Group I, 104 (35.1%) classified as Group II, and 89 (30.0%), as Group III. Table 1 shows the demographic information of enrolled patients. There was little difference in the baseline characteristics between the three groups except mean age which was significantly higher in Group III.
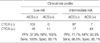
The prevalence of ACS was 20.6%. Diagnostic accuracy of CTCA for ACS was 88.5% (sensitivity), 85.1% (specificity), 60.7% (positive predictive value) and 96.6% (negative predictive value). However, according to the risk profile, the positive and negative predictive values were 37.9% and 100% in the low risk profile group, while 71.7% and 93.3% in intermediate risk profile group (Table 2).
Table 3 shows the result of clinical follow-up for each group. None of the Group I patients had MACE during follow-up period. In some cases additional tests were performed during follow-up period, but no ACS case was found in this group. Among Group II patients, seven (6.73%) were finally categorized as ACS, although there was no case of myocardial infarction or mortality (Table 4). Six of the seven were identified during the ED observation period and were admitted directly from ED. Among the six was a case of 65 yr old male who was diagnosed with microvascular angina. He had reproducible ischemic symptom and ECG change during a treadmill test which was performed during his ED observation period. He was admitted and his invasive coronary angiography showed no significant stenosis. Although he had no definite lesion found, he was considered as one of the seven false negative cases. The one missed ACS case was about a 73 yr old female who was discharged from ED after 24 hr observation period and had recurrent exertional chest pain at home. She was admitted and had coronary angiography (CAG) which showed 75% stenosis at the left circumflex artery. However there was no evidence that she suffered myocardial infarction. Neither myocardial infarction nor mortality case was missed in Group II.
In Group III (n=89), 53 patients (59.6%) had coronary angiography of which 43 patients (48.3%) showed significant stenosis and 33 (37.1%) were treated with interventions including PCI or CABG. Of the 53 patients examined by coronary angiography, 10 (18.9%) patients were diagnosed as myocardial infarction. There was no mortality.
Previous non ED-based studies of 64-channel MDCT reported very high diagnostic accuracy of CTCA (8). Both sensitivity and specificity were about 95% and negative predictive value was about 99% (8). In two meta-analyses, 64-channel MDCT showed sensitivity and specificity of 92% and 95% respectively for segment analysis. For patient analysis, both sensitivity and specificity reached 100% (18, 19). These excellent results of CTCA diagnosis, however, may not be applicable in patients with acute chest pain in ED. In recent small studies, 64 channel MDCT showed rather low discriminatory power compared to the previous non-ED based studies (Table 5) (13, 14, 16, 17). And the American College of Cardiology Foundation guideline 2006 mentioned that the clinical application of CTCA for acute chest pain can only be considered "appropriate" when its application is limited to patients with intermediate pre-test probability without ECG and serial biomarker change (20).
Our intention in this study was testing the clinical applicability of CTCA in the real world ED situation. We had to exclude high risk patients from the study population because application of CTCA to diagnose or exclude an ACS for the population is considered to be neither safe nor efficient. And we also excluded patients whose diagnoses were overtly evident at the beginning of clinical evaluation.
The remaining 'low to intermediate risk' patients group underwent rapid diagnostic evaluation by CTCA. Conventional stress tests require 4 to 8 hr of pre-test observation period and impose cardiovascular loading to patients which can be potential danger to them occasionally. In contrast, we could obtain CTCA image right after the brief initial clinical evaluation without causing the potentially undesirable cardiovascular loading. And immediate discharge from ED was safe in low risk profile group which was also reported to be safe in one previous study (21). In terms of time and effort to evaluate the patients with acute chest pain at ED, the CTCA-based algorithm we applied in this study can be considered more efficient than conventional approaches based on the stress tests. And it was also safe at least for low risk patients. However, there was seven false negative cases found in the intermediate risk group even though six out of the seven were successfully identified during observation period. It signifies the importance of clinical risk profiling. Until further technical advancement is to be made, judicious selection of patients and proper period of observation will remain important for most clinicians.
In terms of 'cost-effectiveness' there is possibility that CTCA may lead additional healthcare cost when used as a primary evaluation tool for acute chest pain. Otero and Rybicki evaluated cost-effectiveness of CTCA, stress echocardiography and myocardial SPECT for 10,000 simulated patients using reported imaging test characteristics, prevalence and risk of coronary heart disease, and medicare reimbursement schedules (22). They reported that the clinical application of CTCA may significantly reduced the overall observation period, negative CAG rate and total healthcare cost (22). However, injudicious use of CTCA can result in increased healthcare cost and develop undesirable health effect, such as radiation exposure, anaphylaxis and nephropathy that can also increase overall cost.
This study has some limitations. This study was conducted in a single, tertiary referral hospital. And more than 70% of initially screened patients were excluded. The results of this study could be applicable only for the "CTCA eligible" patients with "low to intermediate clinical risk profile". It is impossible to compare the result of this study with that of previous studies involving other popular diagnostic methods (e.g., myocardial SPECT, TMT), as this study is a single arm observational study. And the aspect of cost-effectiveness was not assessed in this study.
Figures and Tables
Fig. 1
Study protocol of CTCA based approach for acute chest pain patients. This flowchart shows CTCA based approach for patients with acute chest pain in our ED. Every patient without contraindication who visited our ED had CTCA and managed according to clinical risk profile and result of CTCA analysis.
CTCA, computed tomography coronary angiography; ED, emergency department.

Table 4
Seven false negative cases of Group II

*He had reproducible exertion-related dynamic ST-T change with chest pain without coronary lesion; †The Lesion was located at the distal part of the coronary artery.
LAD, Left anterior descending coronary artery; LCx, Left circumflex coronary artery; RCA, Right coronary artery; PCI, Percutaneous coronary intervention.
References
1. Lau J, Ioannidis JP, Balk EM, Milch C, Terrin N, Chew PW, Salem D. Diagnosing acute cardiac ischemia in the emergency department: a systematic review of the accuracy and clinical effect of current technologies. Ann Emerg Med. 2001. 37:453–460.

2. Selker HP, Zalenski RJ, Antman EM, Aufderheide TP, Bernard SA, Bonow RO, Gibler WB, Hagen MD, Johnson P, Lau J, McNutt RA, Ornato J, Schwartz JS, Scott JD, Tunick PA, Weaver WD. An evaluation of technologies for identifying acute cardiac ischemia in the emergency department: a report from a National Heart Attack Alert Program Working Group. Ann Emerg Med. 1997. 29:13–87.

3. Zalenski RJ, Selker HP, Cannon CP, Farin HM, Gibler WB, Goldberg RJ, Lambrew CT, Ornato JP, Rydman RJ, Steele P. National Heart Attack Alert Program position paper: chest pain centers and programs for the evaluation of acute cardiac ischemia. Ann Emerg Med. 2000. 35:462–471.

4. Pope JH, Aufderheide TP, Ruthazer R, Woolard RH, Feldman JA, Beshansky JR, Griffith JL, Selker HP. Missed diagnoses of acute car diac ischemia in the emergency department. N Engl J Med. 2000. 342:1163–1170.
5. Christenson J, Innes G, McKnight D, Boychuk B, Grafstein E, Thompson CR, Rosenberg F, Anis AH, Gin K, Tilley J, Wong H, Singer J. Safety and efficiency of emergency department assessment of chest discomfort. Canadian Med Ass J. 2004. 170:1803–1807.

6. Collinson PO, Premachandram S, Hashemi K. Prospective audit of incidence of prognostically important myocardial damage in patients discharged from emergency department. BMJ. 2000. 320:1702–1705.
7. Vukmir RB. Medical malpractice: managing the risk. Med Law. 2004. 23:495–513.
8. Budoff MJ, Achenbach S, Blumenthal RS, Carr JJ, Goldin JG, Greenland P, Guerci AD, Lima JA, Rader DJ, Rubin GD, Shaw LJ, Wiegers SE. Intervention AHACoCIa. Intervention AHACoCRa. American Heart Association Committee on Cardiac Imaging CoCC. Assessment of coronary artery disease by cardiac computed tomography: a scientific statement from the American Heart Association Committee on Cardiovascular Imaging and Intervention, Council on Cardiovascular Radiology and Intervention, and Committee on Cardiac Imaging, Council on Clinical Cardiology. Circulation. 2006. 114:1761–1791.
9. Schussler JM, Smith ER. Sixty-four-slice computed tomographic coronary angiography: will the "triple rule out" change chest pain evaluation in the ED? Am J Emerg Med. 2007. 25:367–375.

10. Gaspar T, Halon DA, Lewis BS, Adawi S, Schliamser JE, Rubinshtein R, Flugelman MY, Peled N. Diagnosis of coronary in-stent restenosis with multidetector row spiral computed tomography. J Am Coll Cardiol. 2005. 46:1573–1579.

11. White CS, Kuo D, Kelemen M, Jain V, Musk A, Zaidi E, Read K, Sliker C, Prasad R. Chest pain evaluation in the emergency department: can MDCT provide a comprehensive evaluation? AJR Am J Roentgenol. 2005. 185:533–540.

12. Ghersin E, Litmanovich D, Dragu R, Rispler S, Lessick J, Ofer A, Brook OR, Gruberg L, Beyar R, Engel A. 16-MDCT coronary angiography versus invasive coronary angiography in acute chest pain syndrome: a blinded prospective study. AJR Am J Roentgenol. 2006. 186:177–184.

13. Hoffmann U, Pena AJ, Moselewski F, Ferencik M, Abbara S, Cury RC, Chae CU, Nagurney JT. MDCT in early triage of patients with acute chest pain. AJR Am J Roentgenol. 2006. 187:1240–1247.

14. Hoffmann U, Nagurney JT, Moselewski F, Pena A, Ferencik M, Chae CU, Cury RC, Butler J, Abbara S, Brown DF, Manini A, Nichols JH, Achenbach S, Brady TJ. Coronary multidetector computed tomography in the assessment of patients with acute chest pain. Circulation. 2006. 114:2251–2260.

15. Olivetti L, Mazza G, Volpi D, Costa F, Ferrari O, Pirelli S. Multislice CT in emergency room management of patients with chest pain and medium-low probability of acute coronary syndrome. Radiol Med. 2006. 111:1054–1063.

16. Gallagher MJ, Ross MA, Raff GL, Goldstein JA, O'Neill WW, O'Neill B. The diagnostic accuracy of 64-slice computed tomography coronary angiography compared with stress nuclear imaging in emergency department low-risk chest pain patients. Ann Emerg Med. 2007. 49:125–136.

17. Rubinshtein R, Halon DA, Gaspar T, Jaffe R, Karkabi B, Flugelman MY, Kogan A, Shapira R, Peled N, Lewis BS. Usefulness of 64-slice cardiac computed tomographic angiography for diagnosing acute coronary syndromes and predicting clinical outcome in emergency department patients with chest pain of uncertain origin. Circulation. 2007. 115:1762–1768.

18. Schuijf JD, Bax JJ, Shaw LJ, de Roos A, Lamb HJ, van der Wall EE, Wijns W. Meta-analysis of comparative diagnostic performance of magnetic resonance imaging and multislice computed tomography for noninvasive coronary angiography. Am Heart J. 2006. 151:404–411.

19. Stein PD, Beemath A, Kayali F, Skaf E, Sanchez J, Olson RE. Multidetector computed tomography for the diagnosis of coronary artery disease: a systematic review. Am J Med. 2006. 119:203–216.

20. Hendel RC, Patel MR, Kramer CM, Poon M, Hendel RC, Carr JC, Gerstad NA, Gillam LD, Hodgson JM, Kim RJ, Kramer CM, Lesser JR, Martin ET, Messer JV, Redberg RF, Rubin GD, Rumsfeld JS, Taylor AJ, Weigold WG, Woodard PK, Brindis RG, Hendel RC, Douglas PS, Peterson ED, Wolk MJ, Allen JM, Patel MR. Group ACoCFQSDCACW. Radiology ACo. Tomography SoCC. Resonance SfCM. Cardiology ASoN. Imaging NASfC. Interventions SfCAa. Radiology SoI. ACCF/ACR/SCCT/SCMR/ASNC/NASCI/SCAI/SIR 2006 appropriateness criteria for cardiac computed tomography and cardiac magnetic resonance imaging: a report of the American College of Cardiology Foundation Quality Strategic Directions Committee Appropriateness Criteria Working Group, American College of Radiology, Society of Cardiovascular Computed Tomography, Society for Cardiovascular Magnetic Resonance, American Society of Nuclear Cardiology, North American Society for Cardiac Imaging, Society for Cardiovascular Angiography and Interventions, and Society of Interventional Radiology. J Am Coll Cardiol. 2006. 48:1475–1497.




 PDF
PDF ePub
ePub Citation
Citation Print
Print





 XML Download
XML Download