Abstract
Purpose
The purpose of this study is to investigate the functional and radiologic results of treatment of the old with intertrochanteric fractures by implementation of the proximal femoral nail antirotation (PFNA) with Valgus reduction.
Materials and Methods
A retrospective review of patients (over 65 years old) with intertrochanteric fractures undergoing PFNA, during the period March 2008 to August 2012 at Chungbuk National University Hospital, with follow-up for at least 12 months, was conducted. Fifty-one patients were identified. The mean observation period was 15.6 months and the mean age of patients was 78.6 years old. In this study, AO foundation and Orthopaedic Trauma Association (AO/OTA) classification of initial fractures, post operative neck shaft angle, location of the blade tip (Cleveland index), tip-apex distance (TAD), incidence of complication, Wayne-County reduction, and Koval walking ability were analyzed.
Results
Satisfactory reduced status was achieved by significant (p<0.05) valgus reduction in 49 out of 51 cases and the mean period for radiologic bony union was 15.3 weeks. The mean blade sliding distance was 3.5 mm and the mean TAD was 18.7 mm; however, the blade location did not affect the results. No complications, including surgical site infection, delayed union, nonunion, rotational angulation, and cutting out of the blade tip were found. Thirty-one patients out of 42 who maintained their pre-fracture ambulatory ability, 11 patients (out of 42) remained ambulatory but became more dependent on assistive devices.
Figures and Tables
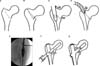 | Figure 1(A) First, the leg must be pulled on a fracture table until the gap between proximal and distal fragment can be identified. (B) Illustration shows that the fracture line is involved to the greater trochanter tip, which will be the nail entry point. (C) Illustration shows the varus angulated neck-shaft angle which results from insertion of the nail without sufficient reaming of the medial entry point. (D) Illustration shows reaming of the medial cortex of the entry point with medial direction force on the reamer. (E) Intraoperative image shows reaming of the medial entry point by towel clip assistance applying medial direction force. (F) Illustration shows hitting the blade several times when adequate tip-apex distance is attained for compression of the fracture line, as indicated by arrows. (G) Illustration shows the compressed fracture site after blade locking with valgus neck-shaft angle. |
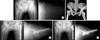 | Figure 2(A) Preoperative radiograph shows an unstable intertrochanteric fracture (AO type A2.3) of the femur and varus angulated states in a 78-year-old female. Pre-injury neck shaft angle in this patient was 129 degrees. The contralateral side shows mal-united states of the previous intertrochanteric fracture. (B) Preoperative 3-dimensional reconstructive computed tomography shows a posteromedial comminuted unstable intertrochanteric fracture of the femur. (C) Immediate postoperative radiograph shows a valgus reduced state compared to the pre-injury neck-shaft angle of the femur. (D) Radiograph 16 months after the operation shows complete union of the femur fracture with a 6 mm screw sliding and maintained valgus state. |
References
1. Rubin PJ, Leyvraz PF, Aubaniac JM, Argenson JN, Estève P, de Roguin B. The morphology of the proximal femur. A three-dimensional radiographic analysis. J Bone Joint Surg Br. 1992; 74:28–32.

2. Kaufer H, Matthews LS, Sonstegard D. Stable fixation of intertrochanteric fractures. J Bone Joint Surg Am. 1974; 56:899–907.

3. Choi NY, Nah KH, Song HS, Seo SI, Choi JK, Han SK. Treatment of the intertrochanteric fractures of the femur in elderly patients: comparision of Wayne-County reduction and anatomical reduction. J Korean Fract Soc. 2004; 17:301–307.

4. Baumgaertner MR, Curtin SL, Lindskog DM, Keggi JM. The value of the tip-apex distance in predicting failure of fixation of peritrochanteric fractures of the hip. J Bone Joint Surg Am. 1995; 77:1058–1064.

5. Cleveland M, Bosworth DM, Thompson FR, Wilson HJ Jr, Ishizuka T. A ten-year analysis of intertrochanteric fractures of the femur. J Bone Joint Surg Am. 1959; 41:1399–1408.

6. Koval KJ, Skovron ML, Aharonoff GB, Meadows SE, Zuckerman JD. Ambulatory ability after hip fracture. A prospective study in geriatric patients. Clin Orthop Relat Res. 1995; 310:150–159.
7. Hornby R, Evans JG, Vardon V. Operative or conservative treatment for trochanteric fractures of the femur. A randomised epidemiological trial in elderly patients. J Bone Joint Surg Br. 1989; 71:619–623.

8. Aune AK, Ekeland A, Odegaard B, Grøgaard B, Alho A. Gamma nail vs compression screw for trochanteric femoral fractures. 15 reoperations in a prospective, randomized study of 378 patients. Acta Orthop Scand. 1994; 65:127–130.

9. Harrington P, Nihal A, Singhania AK, Howell FR. Intramedullary hip screw versus sliding hip screw for unstable intertrochanteric femoral fractures in the elderly. Injury. 2002; 33:23–28.

10. Simmermacher RK, Bosch AM, Van der Werken C. The AO/ASIF-proximal femoral nail (PFN): a new device for the treatment of unstable proximal femoral fractures. Injury. 1999; 30:327–332.

11. Kweon SH, Chun CH, Yang JH, Park JY, Bae KH. Complications of femoral peritrochanteric fractures treated with the gamma nail. J Korean Fract Soc. 2009; 22:85–90.

12. Stern R, Lübbeke A, Suva D, Miozzari H, Hoffmeyer P. Prospective randomised study comparing screw versus helical blade in the treatment of low-energy trochanteric fractures. Int Orthop. 2011; 35:1855–1861.

13. Sung YB, Jo SI. Results of the proximal femoral nail-antirotation (PFNA) in patients with an unstable pertrochanteric fracture. J Korean Hip Soc. 2011; 23:39–46.

14. Rho JY, Kim SB, Heo YM, Cho SJ, Chae DS, Lee WS. Proximal femoral nail antirotation versus compression hip screw with trochanter stabilizing plate for unstable intertrochanteric hip fractures. J Korean Fract Soc. 2010; 23:161–166.

15. Takigami I, Matsumoto K, Ohara A, et al. Treatment of trochanteric fractures with the PFNA (proximal femoral nail antirotation) nail system - report of early results. Bull NYU Hosp Jt Dis. 2008; 66:276–279.
16. Mereddy P, Kamath S, Ramakrishnan M, Malik H, Donnachie N. The AO/ASIF proximal femoral nail antirotation (PFNA): a new design for the treatment of unstable proximal femoral fractures. Injury. 2009; 40:428–432.

17. Chang SA, Cho YH, Byun YS, Han JH, Park JY, Lee CY. The treatment of trochanteric femoral fracture withusing proximal femoral nail antirotation (PFNA). J Korean Hip Soc. 2009; 21:252–256.
18. Dimon JH, Hughston JC. Unstable intertrochanteric fractures of the hip. J Bone Joint Surg Am. 1967; 49:440–450.

19. Sarmiento A. Unstable intertrochanteric fractures of the femur. Clin Orthop Relat Res. 1973; 92:77–85.

20. Laskin RS, Gruber MA, Zimmerman AJ. Intertrochanteric fractures of the hip in the elderly: a retrospective analysis of 236 cases. Clin Orthop Relat Res. 1979; 141:188–195.




 PDF
PDF ePub
ePub Citation
Citation Print
Print




 XML Download
XML Download