Abstract
Purpose
To report relatively long-term clinical results of lateral supramalleolar adipofascial flap for children who injured soft tissue on the dorsum of the foot and ankle, a condition that readily gives rise to contracture and deformity in that area.
Materials and Methods
This report presents the authors' experience with eleven patients treated with this flap. The patients' ages ranged from three to nine years; three of the patients were male and eight were female. The major cause of the soft-tissue defects involved acute crushing injury from a traffic accident. The flap and the adjoining raw area were covered with a full-thickness skin graft after 5-7 days postoperatively, and the donor site at the lateral aspect of the leg was closed primarily without grafting. A skin graft was taken from the groin area, which was closed primarily.
Results
All flaps survived, and there were no major complications. No patients showed contracture at the recipient site or deformity of the foot and ankle. Compared with the other flaps, this adipofascial flap was thinner, produced less bulkiness at the recipient site, and caused only minor aesthetic sequelae at the donor site. None of the patients in this study complained of contracture and limitation of motion of the metatarso-phalangeal joint, which might be disturbed by wearing shoes or walking.
Figures and Tables
Figure 1
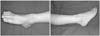
Posttraumatic soft-tissue defect of a 3-year-old girl, with exposure of the medial cuneiform, the first tarsometatarsal joint, the tibialis anterior tendon and the extensor hallucis tendon, and loss of the dorsalis pedis artery and the superficial peroneal nerve.
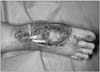
Figure 2
Wound was prepared to be covered with the flap. Big toe and ankle were fixated with K-wire temporally.
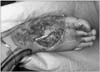
Figure 3
Design of the lateral supramalleolar adipofascial flap, with its vascular supply from the perforating branch of the peroneal artery. The adipofascial flap was obtained from the same territory as the lateral supramalleolar flap.
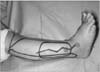
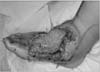
Figure 5
The adipofascial flap was elevated and ready to transfer. The overlying skin and superficial peroneal nerve were preserved.
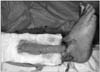
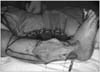
Figure 6
The flap was brought to lateral dorsal side of the foot. Supreficial peroneal nerve and perforating branch of the peroneal artery were observed.
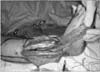
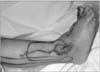
Figure 7
The donor site was closed primarily. The flap was transferred through subcutaneous tunnel to cover the defect. The distal area of the donor site was loosely sutured not to choke a pedicle of the flap.
References
1. Gibstein LA, Abramson DL, Sampson CE, Pribaz JJ. Musculofascial flaps based on the dorsalis pedis vascular pedicle for coverage of the foot and ankle. Ann Plast Surg. 1996. 37:152–157.

2. Choi SJ, Yuh YD, Lee CJ, Cho WH, Chang HC. Reconstruction of foot and ankle soft tissue defect by lateral supramalleolar flap. J Korean Orthop Assoc. 1995. 30:1725–1732.
4. Chiang YC, Jeng SF, Yeh MC, Liu YT, Chen HT, Wei FC. Free tissue transfer for leg reconstruction in children. Br J Plast Surg. 1997. 50:335–342.

5. Lee YH, Rah SK, Choi SJ, Chung MS, Baek GH. Distally based lateral supramalleolar adipofascial flap for reconstruction of the dorsum of the foot and ankle. Plast Reconstr Surg. 2004. 114:1478–1485.

6. Masquelet AC, Beveridge J, Romana C, Gerber C. The lateral supramalleolar flap. Plast Reconstr Surg. 1988. 81:74–81.

7. Valenti P, Masquelet AC, Romana C, Nordin JY. Technical refinement of the lateral supramalleolar flap. Br J Plast Surg. 1991. 44:459–462.

8. Cocchiarella L, Andersson G. American Medical Association. Guides to the evaluation of permanent impairment. 2000. 5th. Chicago: AMA press;536–598.
9. Boone DC, Azen SP. Normal range of motion of joints in male subjects. J Bone Joint Surg Am. 1979. 61:756–759.

10. el-Khatib H. Island adipofascial flap for resurfacing of the Achilles tendon. Plast Reconstr Surg. 1996. 98:1034–1038.

11. Biswas G, Lohani I, Chari PS. The sandwich temporoparietal free fascial flap for tendon gliding. Plast Reconstr Surg. 2001. 108:1639–1645.

12. Fotopoulos P, Holmer P, Leicht P, Elberg JJ. Dorsal hand coverage with free serratus fascia flap. J Reconstr Microsurg. 2003. 19:555–559.

14. Jin YT, Cao HP, Chang TS. Clinical application of the free scapular fascial flap. Ann Plast Surg. 1989. 23:170–177.

15. Meland NB, Weimar R. Microsurgical reconstruction: experience with free fascia flaps. Ann Plast Surg. 1991. 27:1–8.

16. Walton RL, Matory WE Jr, Petry JJ. The posterior calf fascial free flap. Plast Reconstr Surg. 1985. 76:914–926.

17. Lai CS, Lin SD, Yang CC, Chou CK. Adipofascial turn-over flap for reconstruction of the dorsum of the foot. Br J Plast Surg. 1991. 44:170–174.

18. Lin SD, Lai CS, Chiu YT, Lin TM. The lateral calcaneal artery adipofascial flap. Br J Plast Surg. 1996. 49:52–57.





 PDF
PDF ePub
ePub Citation
Citation Print
Print




 XML Download
XML Download