Abstract
Purpose
To analyze the clinical and radiological results of whole lumbosacral fusion, and to identify whether an extension of the fusion level is required.
Materials and Methods
A retrospective review was carried out on 40 patients who had undergone whole lumbosacral fusion. The adjacent segment changes were evaluated by the radiological findings including intervertebral space narrowing, traction spur, endplate sclerosis and vacuum phenomenon. The clinical results were evaluated using a visual analogue scale (VAS) and Oswestry disability index (ODI).
Results
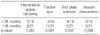
The mean age was 63.8 years and the mean follow-up period was 41.7 months. At the last follow-up, adjacent segment changes were observed in 12 cases of intervertebral space narrowing, 15 cases of traction spur, 20 cases of endplate sclerosis and 8 cases of vacuum phenomenon. In the clinical results, the VAS was improved to 4.0 points from 7.6 points, and the ODI improved to 43.9% from 86.0%. There were no revision cases due to adjacent segment problems.
Conclusion
Whole lumbosacral fusion in spinal stenosis with degenerative lumbar scoliosis was concomitant with some adjacent segment problems, but presented favorable outcomes. For the prevention of junctional problem, caution should be taken when extending the fusion level to the proximal level in whole lumbosacral fusion.
Figures and Tables
Fig. 1
69-year-old female patient. (A) Preoperative X-ray showed degenerative changes with mild scoliosis. (B) At postoperative 42 months, the X-ray showed no additional adjacent segmental changes compared with the preoperative state and bony union was well done.
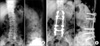
Fig. 2
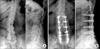
53-year-old female patient. (A) Preoperative X-ray showed degenerative lumbar disease with scoliosis. (B) At postoperative 39 months, the X-ray was showed intervertebral space narrowing, a traction spur, end plate sclerosis and vacuum phenomenon of the adjacent segment. However, the patient was satisfied with the result of the operation and did not complain of low back pain or radiating pain.
References
2. Booth KC, Bridwell KH, Eisenberg BA, Baldus CR, Lenke LG. Minimum 5-year results of degenerative spondylolisthesis treated with decompression and instrumented posterior fusion. Spine. 1999. 24:1721–1727.

3. Cho JL, Choi SW, Lee JM, Park YS. The changes of adjacent segments after long segment posterolateral fusion: comparative study of 3 year versus over the 7 year follow-up patients. J Korean Ortho Assoc. 2005. 40:38–43.

4. Cho JL, Park YS, Han JH, Lee CH, Roh WI. The Changes of adjacent segments after spinal fusion. J Korean Spine Surg. 1998. 5:239–246.
5. Etebar S, Carhill DW. Risk factors for adjacent-segment failure following lumbar fixation with rigid instrumentation for degenerative instability. J Neurosurg. 1999. 90:Suppl 2. S163–S169.

6. Fairbank JC, Couper J, Davies JB, O'Brien JP. The Oswestry low back pain disability questionnaire. Physiotheraphy. 1980. 66:271–273.
7. Farcy JP, Schwab FJ. Management of flat back and related kyphotic decompensation syndromes. Spine. 1997. 22:2452–2457.
8. Gelb DE, Lenke LG, Bridwell KH, Blanke K, McEnery KW. An analysis of sagittal spinal alignment in 100 asymptomatic middle and older aged volunteers. Spine. 1995. 20:1351–1358.

9. Guigui P, Lambert P, Lassale B, Deburge A. Long-term outcome at adjacent levels of lumbar arthrodesis. Rev Chir Orthop Reparatrice Appar Mot. 1997. 83:685–696.
10. Ha KY, Kim KW, Park SJ, Lee YH. Changes of the adjacent-unfused mobile segment after instrumental lumbar fusion. J Korean Spine Surg. 1998. 5:205–214.
12. Lenke LG, Bridwell KH, Bullis D, Betz RR, Baldus C, Schoenecker PL. Results of in situ fusion for isthmic spondylolisthesis. J Spinal Disord. 1992. 5:433–442.

13. Shufflebarger H, Suk SI, Mardjetko S. Debate: determining the upper instrumented vertebra in the management of adult degenerative scoliosis: stopping at T10 versus L1. Spine. 2006. 31:Suppl 19. S185–S194.
14. Stauffer RN, Coventry MB. Posterolateral lumbar-spine fusion. Analysis of Mayo clinic series. J Bone Joint Surg Am. 1972. 54:1195–1204.
15. Thompson WA, Gristina AG, Healy WA Jr. Lumbosacral spine fusion. A method of bilateral posterolateral fusion combined with a Hibbs fusion. J Bone Joint Surg Am. 1974. 56:1643–1647.
16. Weinhoffter SL, Guyer RD, Herbert M, Griffith SL. Intradiscal pressure measurements above an instrumented fusion: a cadaveric study. Spine. 1995. 20:526–531.




 PDF
PDF ePub
ePub Citation
Citation Print
Print




 XML Download
XML Download