Abstract
Purpose
To determine the effect of intraocular pressure (IOP) reduction of selective laser trabeculoplasty (SLT) on medically uncontrolled open-angle glaucoma (OAG) and the factors associated with the treatment result.
Methods
Forty-seven eyes of 47 OAG patients were enrolled for 180° SLT or 360° SLT, all under maximal tolerated medical therapy and with IOP above their target pressure. All patients were followed-up for at least 1 year after the procedure. Treatment success was defined as IOP reduction ≥20% from baseline at 12 months after SLT treatment without additional anti-glaucoma-tous intervention.
Results
The treatment success rate was 65.96%. Baseline IOP was 23.84 ± 4.52 mmHg in the success group and 21.44 ± 2.97 mmHg in the failure group (p = 0.035). Significant mean IOP reduction was observed at 6, 9, and 12 month follow-ups (p = 0.001 at 6 months; 0.041 at 9 months, and <0.001 at 12 months). The success rate did not vary significantly by sex (p = 0.362), age (p = 0.081), history of cataract surgery (p = 0.470), number of medications (p = 0.857), duration of medication (p = 0.613), or an-gular degree of SLT treatment (180° vs. 360°) (p = 0.137). There was a positive correlation between mean baseline IOP and mean reduction of IOP from baseline in the success group (p < 0.001, r = 0.861), while there was no such correlation in the failure group (p = 0.272, r = -2.921).
Go to : 
References
1. Latina MA, Park C. Selective targeting of trabecular meshwork cells: in vitro studies of pulsed and CW laser interactions. Exp Eye Res. 1995; 60:359–71.

2. Lai JS, Chua JK, Tham CC, Lam DS. Five-year follow up of se-lective laser trabeculoplasty in Chinese eyes. Clin Exp Ophthalmol. 2004; 32:368–72.

3. McIlraith I, Strasfeld M, Colev G, Hutnik CM. Selective laser tra-beculoplasty as initial and adjunctive treatment for open-angle glaucoma. J Glaucoma. 2006; 15:124–30.

4. Juzych MS, Chopra V, Banitt MR. . Comparison of long-term outcomes of selective laser trabeculoplasty versus argon laser tra-beculoplasty in open-angle glaucoma. Ophthalmology. 2004; 111:1853–9.

5. Song J, Lee PP, Epstein DL. . High failure rate associated with 180 selective laser trabeculoplasty. J Glaucoma. 2005; 14:400–8.

6. Ayala M, Chen E. Comparison of selective laser trabeculoplasty (SLT) in primary open angle glaucoma and pseudoexfoliation glaucoma. Clin Ophthalmol. 2011; 5:1469–73.

7. Stein JD, Challa P. Mechanisms of action and efficacy of argon la-ser trabeculoplasty and selective laser trabeculoplasty. Curr Opin Ophthalmol. 2007; 18:140–5.

8. Latina MA, Gulati V. Selective laser trabeculoplasty: stimulating the meshwork to mend its ways. Internati Int Ophthalmol Clin. 2004; 44:93–103.

9. Moon SJ, Choi ES, Park JI, Lee KH. Two-year follow-up of se-lective laser trabeculoplasty as initial and adjunctive treatment for ocular hypertension and open angle glaucoma. J Korean Ophthalmol Soc. 2010; 51:974–80.

10. Park JJ, Lee JW, Lee KW. Comparison of clinical outcomes of ar-gon laser versus selective laser trabeculoplasty in POAG. J Korean Ophthalmol Soc. 2008; 49:1491–500.

11. Park HJ, Park JW. Effect of prior cataract surgery on the clinical outcome of selective laser trabeculoplasty. J Korean Ophthalmol Soc. 2015; 56:911–6.

12. Jang YS, Kim JM, Lim TH. . Comparison of 180 and 360 se-lective laser trabeculoplasty. J Korean Ophthalmol Soc. 2012; 53:291–6.

13. Lee JW, Kim EJ, Lee TY, Lee KW. Comparison of efficacy and safety between superior 180 degree and inferior 180 degree se-lective laser trabeculoplasty. J Korean Ophthalmol Soc. 2012; 53:1642–8.

14. Lee JY, Lee YK, Moon JI, Park MH. Long-term outcomes and pre-dictive factors for success of selective laser trabeculoplasty. J Korean Ophthalmol Soc. 2014; 55:1347–54.

15. O’conor DJ, Caprioli J. Comparison of methods to detect glaucom-atous damage. Ophthalmology. 1993; 100:1498–503.
16. Suh W, Jun RM, Choi KR. Longitudinal analysis of retinal nerve fi-ber layer thickness with GDx-VCC in glaucoma suspect. J Korean Ophthalmol Soc. 2009; 50:235–41.

17. Kim DY, Singh A. Severe iritis and choroidal effusion following selective laser trabeculoplasty. Ophthalmic Surg Lasers Imaging. 2008; 39:409–11.

18. Song J. Complications of selective laser trabeculoplasty: a review. Clin Ophthalmol. 2016; 10:137–43.

19. Hodge WG, Damji KF, Rock W. . Baseline IOP predicts se-lective laser trabeculoplasty success at 1 year post-treatment: re-sults from a randomised clinical trial. Br J Ophthalmol. 2005; 89:1157–60.

20. Weinand FS, Althen F. Long-term clinical results of selective laser trabeculoplasty in the treatment of primary open angle glaucoma. Eur J Ophthalmol. 2006; 16:100–4.

21. Sayin N, Alkin Z, Ozkaya A. . Efficacy of selective laser trabe-culoplasty in medically uncontrolled glaucoma. ISRN Ophthalmol. 2013; 2013:975281.

22. Gracner T, Naji M, Hudovernik M. . Predictive factors of suc-cessful selective laser trabeculoplasty in open-angle glaucoma. Klin Monbl Augenheilkd. 2007; 224:922–6.
23. Busbee BG, Recchia FM, Kaiser R. . Bleb-associated endoph-thalmitis: clinical characteristics and visual outcomes. Ophthalmology. 2004; 111:1495–503 discussion 1503.
24. DeBry PW, Perkins TW, Heatley G. . Incidence of late-onset bleb-related complications following trabeculectomy with mitomycin. Arch Ophthalmol. 2002; 120:297–300.

25. Jampel HD, Musch DC, Gillespie BW. . Perioperative compli-cations of trabeculectomy in the collaborative initial glaucoma treatment study (CIGTS). Am J Ophthalmol. 2005; 140:16–22.

26. Gracner T. Intraocular pressure response to selective laser trabecu-loplasty in the treatment of primary open-angle glaucoma. Ophthalmologica. 2001; 215:267–70.

27. The Glaucoma Laser Trial (GLT). 2. Results of argon laser trabecu-loplasty versus topical medicines. The Glaucoma Laser Trial Research Group. Ophthalmology. 1990; 97:1403–13.
28. Reiss GR, Wilensky JT, Higginbotham EJ. Laser trabeculoplasty. Surv Ophthalmol. 1991; 35:407–28.

29. Ederer F, Gaasterland DA, Dally LG. . The Advanced Glaucoma Intervention Study (AGIS): 13. Comparison of treatment outcomes within race: 10-year results. Ophthalmology. 2004; 111:651–64.
30. Prasad N, Murthy S, Dagianis JJ, Latina MA. A comparison of the intervisit intraocular pressure fluctuation after 180 and 360 degrees of selective laser trabeculoplasty (SLT) as a primary therapy in pri-mary open angle glaucoma and ocular hypertension. J Glaucoma. 2009; 18:157–60.

31. Seymenoğ lu G, Baser EF. Efficacy of selective laser trabeculo-plasty in phakic and pseudophakic eyes. J Glaucoma. 2015; 24:105–10.
Go to : 
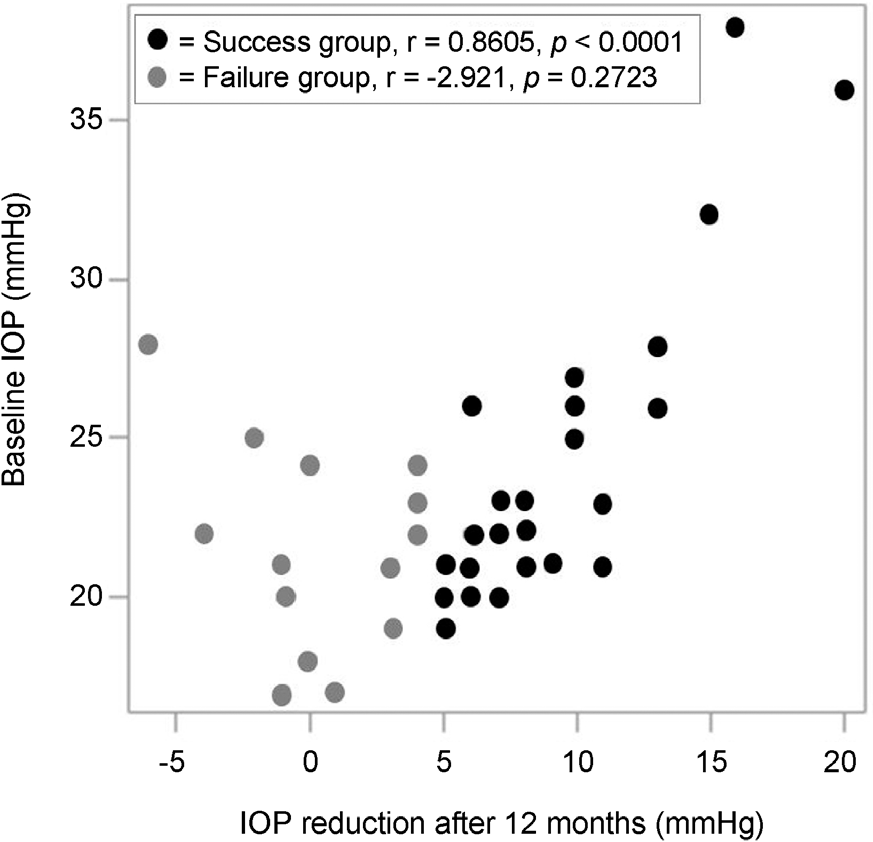 | Figure 1.Pearson correlation of baseline intraocular pressure (IOP) and IOP reduction after 12 months. IOP measurements obtained by Goldmann applanation tonometer. |
Table 1.
The general characteristics of 47 patients with medi-cally uncontrolled open-angle glaucoma
Table 2.
Comparison of baseline characteristics between success and failure group
| Characteristics | Success* (n = 31) | Failure (n = 16) | p-value† |
|---|---|---|---|
| Age (n, %) | 0.081 | ||
| >70 years old | 20 (76.92) | 6 (23.08) | |
| ≤70 years old | 11 (52.38) | 10 (47.62) | |
| Sex (n, %) | 0.362 | ||
| Male | 17 (60.71) | 11 (39.29) | |
| Female | 14 (73.68) | 5 (26.32) | |
| Lens status, phakic (n, %) | 0.470 | ||
| Pseudo-phakic | 11 (73.33) | 4 (26.67) | |
| Phackic | 20 (62.50) | 12 (37.50) | |
| Baseline IOP (mmHg) | 23.84 ± 4.52 | 21.44 ± 2.97 | 0.035 |
| Type of laser (n, %) | 0.137 | ||
| 180° SLT | 7 (50.00) | 7 (50.00) | |
| 360° SLT | 24 (72.73) | 9 (27.27) | |
| Mean duration of medication (n, %) | 0.613 | ||
| >4 years | 15 (62.50) | 9 (37.50) | |
| ≤4 years | 16 (69.57) | 7 (30.43) | |
| Number of medication (n, %) | 0.857 | ||
| 1 | 4 (57.14) | 3 (42.86) | |
| 2 | 16 (69.57) | 7 (30.43) | |
| 3 | 11 (64.71) | 6 (32.29) | |
| Comorbidities | |||
| Hypertension | 0.613 | ||
| Yes | 15 (62.50) | 9 (37.50) | |
| No | 16 (69.57) | 7 (30.43) | |
| Diabetic mellitus type 2 | 0.469 | ||
| Yes | 5 (55.56) | 4 (44.44) | |
| No | 26 (68.42) | 12 (31.58) | |
| BCVA (logMAR) | 0.19 ± 0.25 | 0.18 ± 0.19 | 0.900 |
| Refraction | |||
| Spherical power (diopters) | -1.29 ± 2.51 | -1.42 ± 2.37 | 0.900 |
| Cylindrical power (diopters) | -0.66 ± 0.74 | -1.11 ± 0.57 | 0.117 |
| Visual field | |||
| MD (dB) | -15.40 ± 6.86 | -16.71 ± 8.43 | 0.576 |
| PSD (dB) | 10.05 ± 2.82 | 10.05 ± 3.14 | 0.995 |
Values are presented as mean ± SD or n (%) unless otherwise indicated. IOP = intraocular pressure; SLT = selective laser trabeculoplasty; BCVA = best corrected visual acuity; MD = mean deviation; PSD = pat-tern standard deviation.
Table 3.
IOP reduction throughout the 12 months follow up period
| Variables | Success | Failure | p-value* |
|---|---|---|---|
| Baseline IOP (mmHg) | 23.84 ± 4.52 | 21.44 ± 2.97 | 0.062 |
| 1 week | 18.06 ± 3.87 | 17.75 ± 5.93 | 0.850 |
| 1 month | 16.58 ± 3.51 | 16.19 ± 1.94 | 0.624 |
| 3 months | 16.32 ± 4.34 | 17.19 ± 4.65 | 0.531 |
| 6 months | 15.52 ± 3.00 | 19.00 ± 3.65 | 0.001 |
| 9 months | 15.57 ± 2.83 | 19.62 ± 6.21 | 0.041 |
| 12 months | 14.84 ± 2.33 | 20.81 ± 4.82 | <0.001 |
Table 4.
Association between success and demographic variables for multivariate logistic regression




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download