Abstract
Purpose
To unveil the etiology, pathogenic mechanism and the clinical significance of the corneal iron line through various clinical aspects of the corneal iron line.
Methods
This study included 45 eyes of 39 patients who visited the Department of Ophthalmology in Chungnam National University Hospital between April 2011 and March 2014. Anterior segment of the eye was photographed during the diagnostic process. The medical history of the patient was investigated and corneal topography was performed to discover the relationship between the position of the corneal iron line and the curvature of the corneal surface.
Results
The corneal iron line was identified in various corneal diseases such as herpetic stromal keratitis and; corneal ulcer. The average age of patients was 57.8 years. Corneal topography was performed in 12 patients and a connection was found between the curvature of the corneal surface and the position of corneal iron line at 75%. During the research period, corneal disease progressed and associated corneal iron line became clearer in 2 eyes. However, there was no repositioning or new appearance in different areas. The corneal iron line was not associated with visual acuity and the shape varied in accordance with the accompanying corneal disorder. The location where the tears repeatedly accumulate was associated with corneal surface irregularity, and the corneal iron line was confirmed where the cornea was depressed or around the uplifted surface.
Conclusions
Based on the occurrence location and the shape of the corneal iron line, we could understand that the occurrence of corneal iron line is associated with the past and current corneal surface irregularities, which verified the validity of the tear pooling hypothesis. Therefore, this result can aid in establishing the diagnosis and treatment plan when the corneal iron line is discovered during clinical practice.
Go to : 
References
2. Hudson AC. A note on certain peculiar pigmentary markings in the cornea. R Lond Ophthalmic Hosp Rep. 1911; 18:198–202.
3. Norn M. Hudson-Stähli's iron line in the cornea. Occurrence in 1968 and in 1988. Acta Ophthalmol (Copenh). 1990; 68:339–40.
4. Ferry AP. A “new” iron line of the superficial cornea. Occurrence in patients with filtering blebs. Arch Ophthalmol. 1968; 79:142–5.
5. Seiler T, Holschbach A. Central corneal iron deposit after photo-refractive keratectomy. Ger J Ophthalmol. 1993; 2:143–5.
6. Steinberg EB, Wilson LA, Waring GO 3rd, et al. Stellate iron lines in the corneal epithelium after radial keratotomy. Am J Ophthalmol. 1984; 98:416–21.

7. Assil KK, Quantock AJ, Barrett AM, Schanzlin DJ. Corneal iron lines associated with the intrastromal corneal ring. Am J Ophthalmol. 1993; 116:350–6.

8. Farkas RH, Chowers I, Hackam AS, et al. Increased expression of iron-regulating genes in monkey and human glaucoma. Invest Ophthalmol Vis Sci. 2004; 45:1410–7.

9. Zigler JS Jr, Huang QL, Du XY. Oxidative modification of lens crystallins by H2O2 and chelated iron. Free Radic Biol Med. 1989; 7:499–505.
10. Hahn P, Milam AH, Dunaief JL. Maculas affected by age-related macular degeneration contain increased chelatable iron in the abdominall pigment epithelium and Bruch's membrane. Arch Ophthalmol. 2003; 121:1099–105.
11. Iwamoto T, DeVoe G. Electron microscopical study of the Fleisher ring. Arch Ophthalmol. 1976; 94:1579–84.
13. Collin HB. Prevalence of the Hudson-Stähli line of the cornea. Am J Optom Physiol Opt. 1979; 56:94–7.

14. Rose GE, Lavin MJ. The Hudson-Stahli line. I: an epidemiological study. Eye (Lond). 1987; 1(Pt 4):466–70.

15. Rao SK, Ananth VS, Padmanabhan P. Corneal topography and Schirmer testing in eyes with the Hudson-Stahli line. Eye (Lond). 2002; 16:267–70.

17. Norn MS. Hudson-Stähli's line of cornea. II. Aetiological studies. Acta Ophthalmol (Copenh). 1968; 46:119–28.
18. Rose GE, Lavin MJ. The Hudson-Stähli Line. III: Observations on morphology, a critical review of aetiology and a unified theory for the formation of iron lines of the corneal epithelium. Eye (Lond). 1987; 1(Pt 4):475–9.
19. Thoft RA, Friend J. The X, Y, Z hypothesis of corneal epithelial maintenance. Invest Ophthalmol Vis Sci. 1983; 24:1442–3.
Go to : 
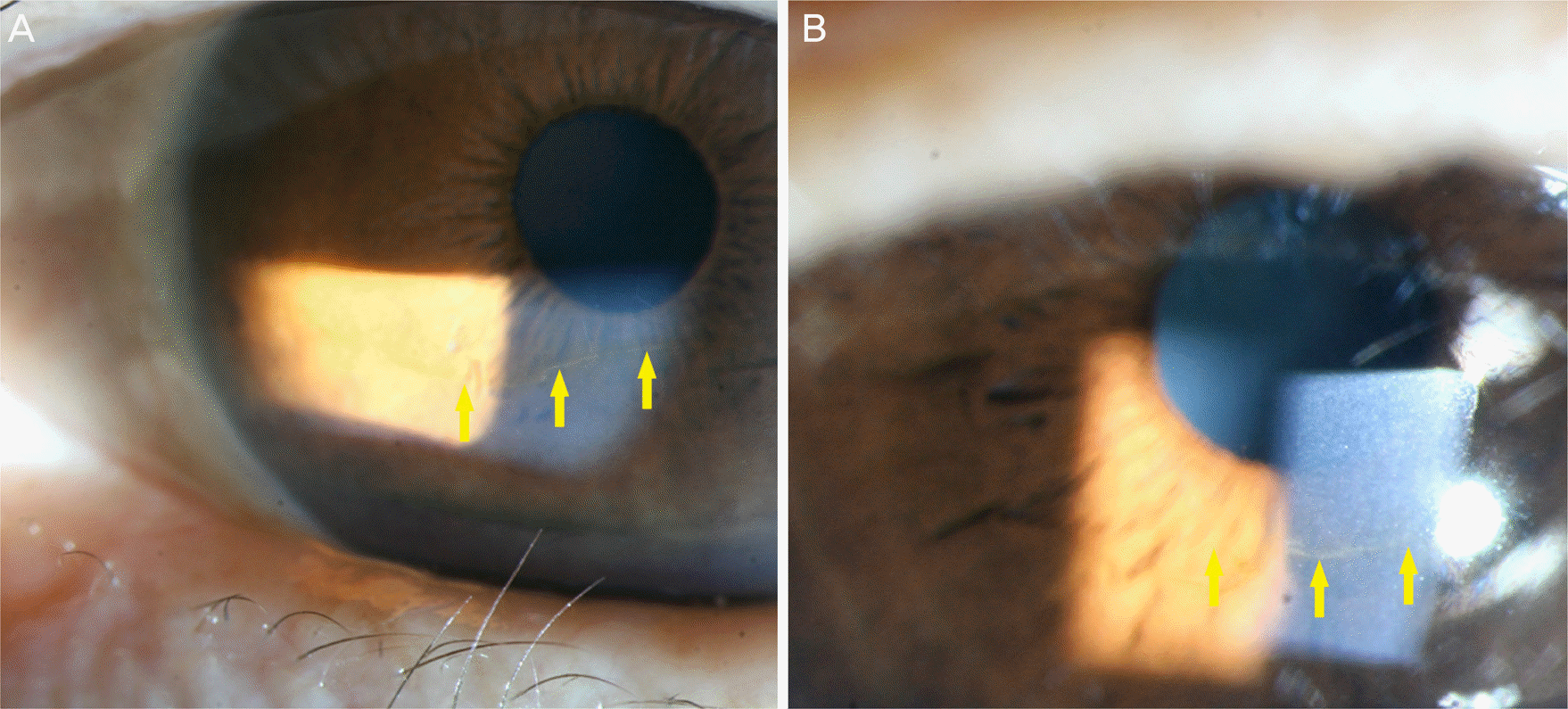 | Figure 1.Hudson-Stähli line. A 76-year-old female diagnosed with conjunctivochalasis. (A) The yellow horizontal iron line is formed in the lower third of the cornea where the closed eyelids meet (arrows). (B) Corneal surface is even and the yellow arrows indicate the iron line identified under the direct illumination. |
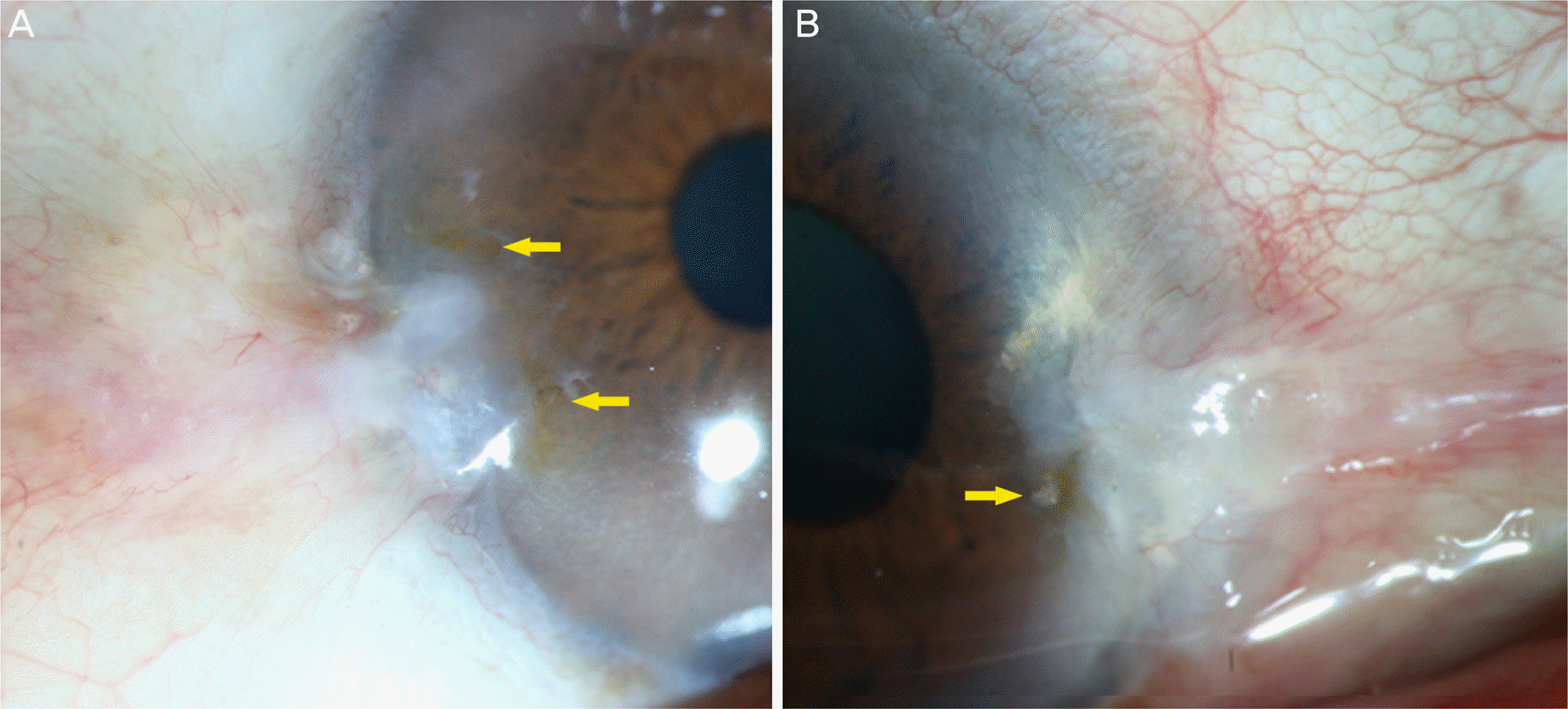 | Figure 2.Stocker's line (slit-lamp photo). (A) A 64-year-old male diagnosed with pteygium. Pterygium has invaded the cornea for about 1 mm. The yellow arrows point the thick brown line formed adjacent to the pterygium head. (B) Another 64-year-old female diagnosed with pteygium and dry eye syndrome. The dark brown corneal iron line is formed at the bottom of the pterygium (yellow arrow). |
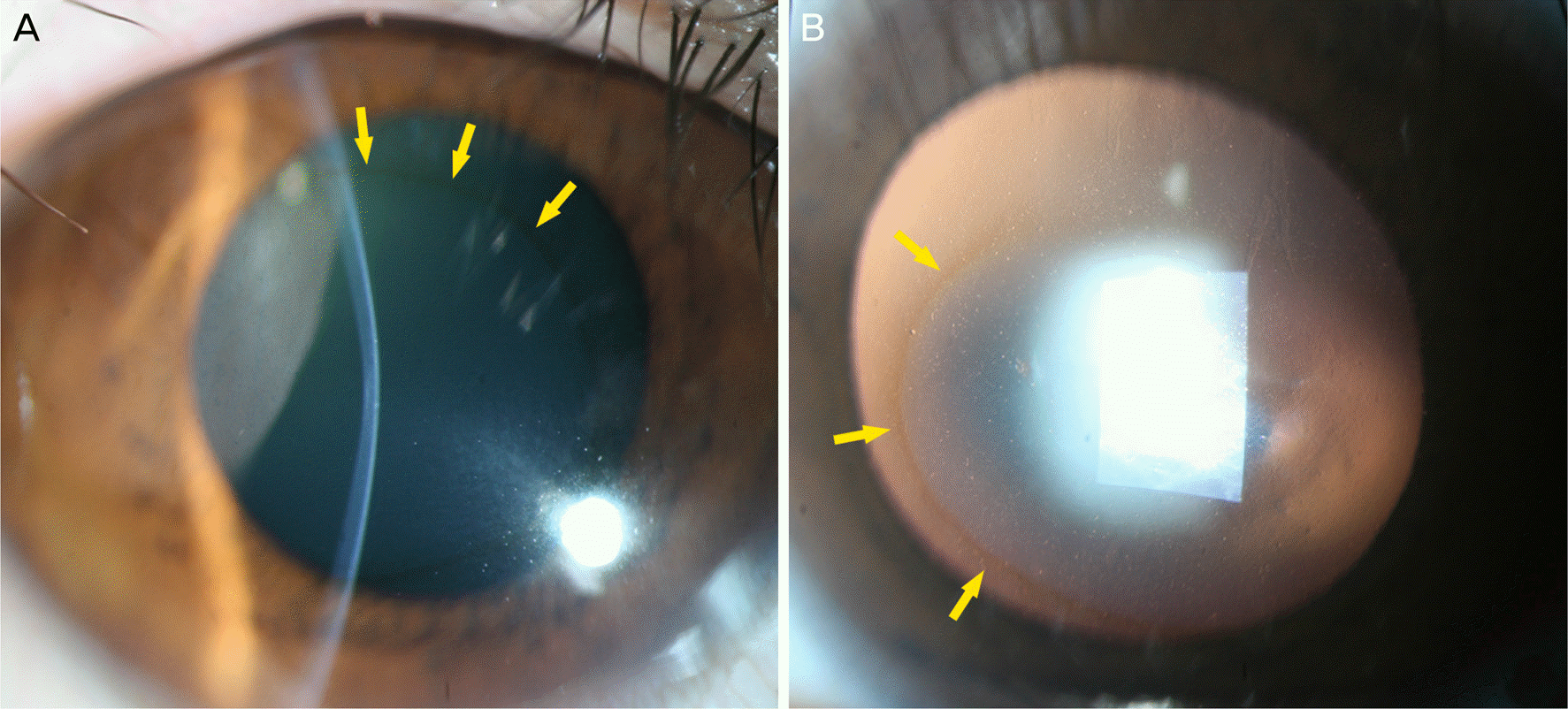 | Figure 3.Fleischer's ring. (A) The round corneal iron line is identified at the conical base of keratoconus under the direct illumination (yellow arrows). The center of the cornea becomes thinner and it has been protruded. (B) Dark brown corneal iron line is visible in the retroillumination. The yellow arrows indicate the corneal iron line more prominent in the lower part of the cornea than the upper part of the cornea. |
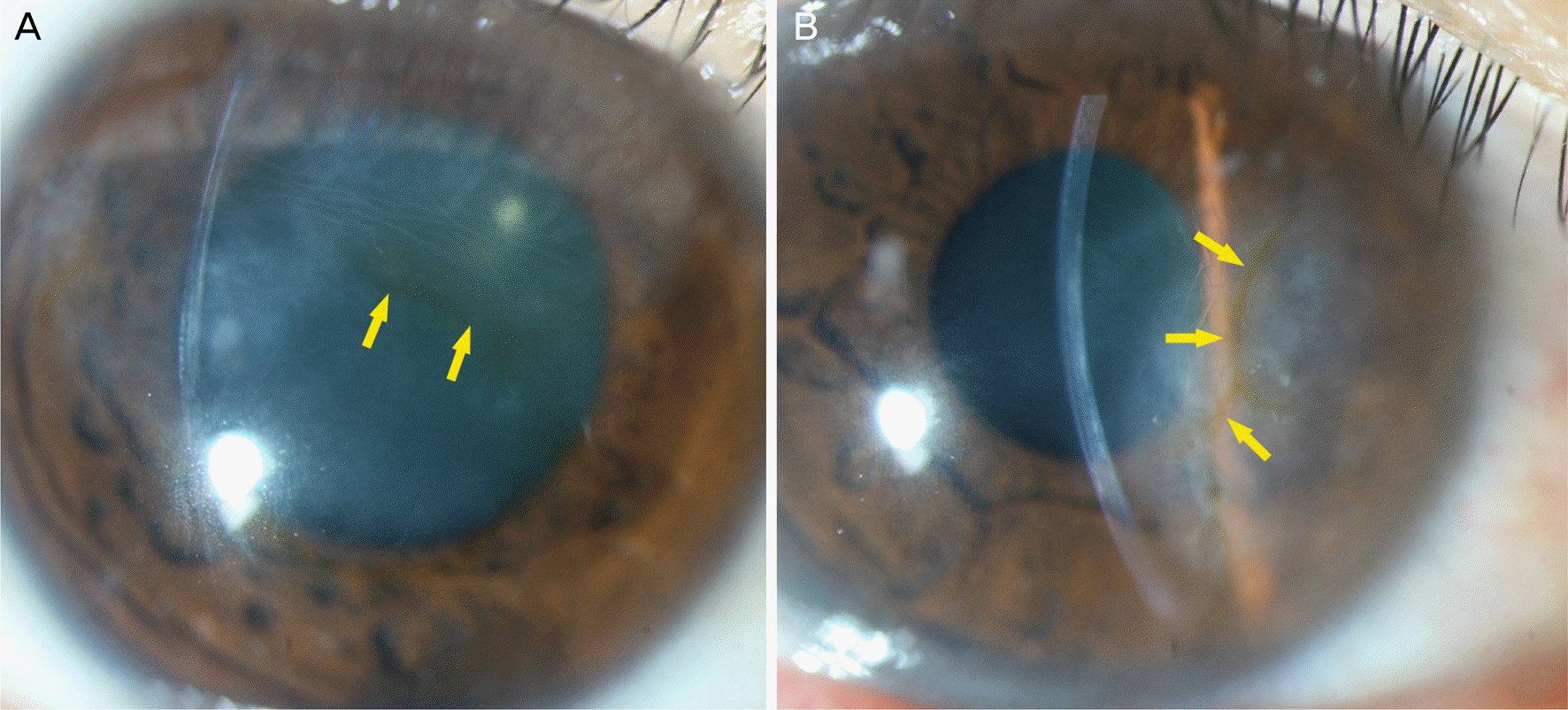 | Figure 4.Herpetic stromal keratitis. (A) A 41-year-old male diagnosed with herpetic stromal keratitis 4 years ago. Slit-lamp photograph shows severe corneal opacity and stromal edema which are accompanied with Descemet membrane folds. Wide distribution of the cornea pigmentation are formed on the bottom of corneal edema (yellow arrows). (B) A 49-year-old male. The initial diagnosis was herpetic stromal keratitis 9 years ago. The yellow arrows marks the thin brown corneal iron line formed within the corneal opacity. |
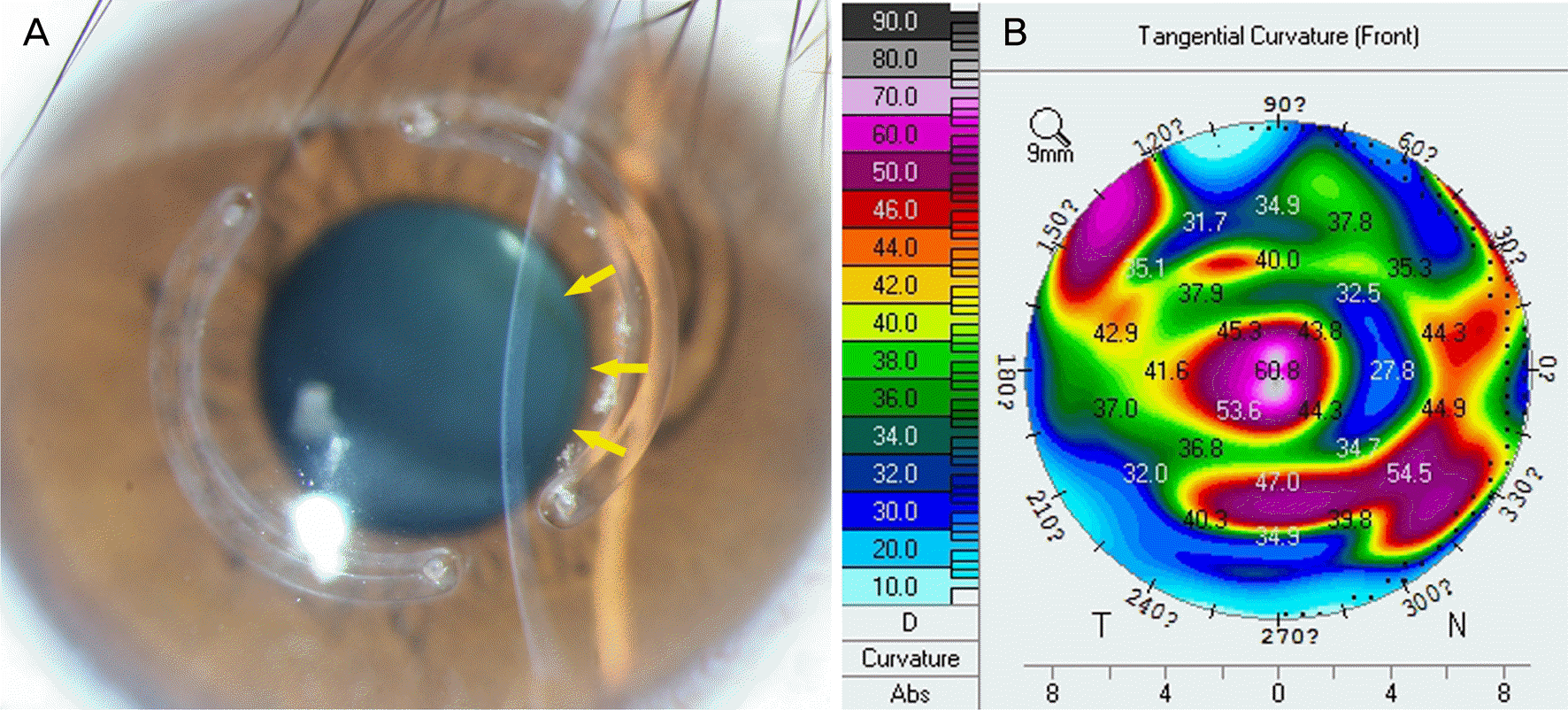 | Figure 5.Corneal iron line which is formed after intrastromal ring insertion. (A) It appears white stromal haze around the inserted ring (slit-lamp photo). The center of the cornea becomes thinner and the faint yellow corneal iron line which is similar to Fleischer's ring of keratoconus is seen from the inner part of the intrastromal ring (yellow arrows). (B) Corresponding corneal curvature in corneal topograph is also significantly lower than the surrounding. N = nasal; T = temporal. |
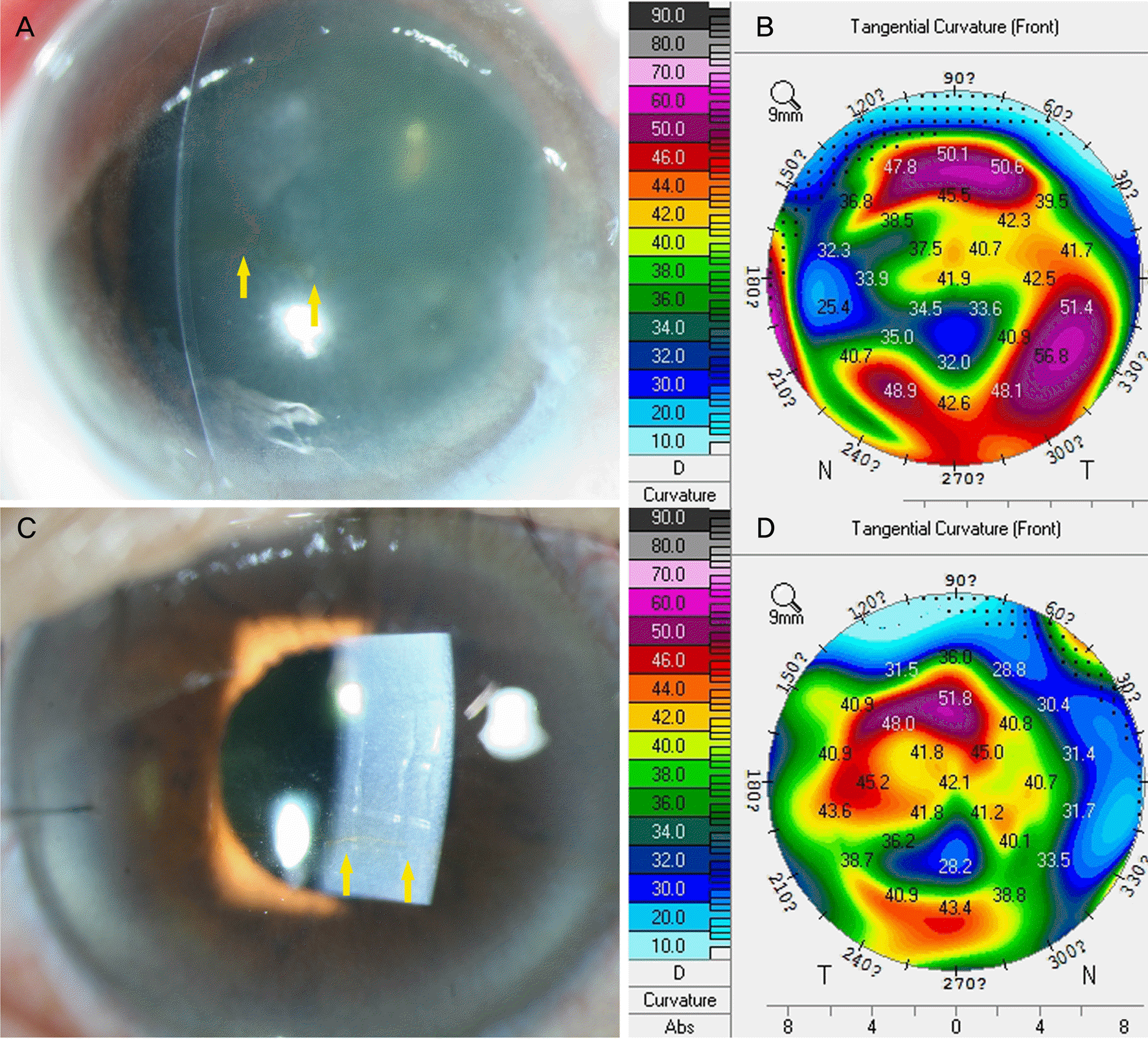 | Figure 6.Chemical burn (slit-lamp photo). (A) A 58-year-old male was working at a building site and got cement into his eyes. Widely distributed yellow iron line is seen in the relatively recessed area in between the corneal edema and opacity (yellow arrows). (B) Corresponding topography of photo A. (C) A 67-year-old female diagnosed with blast-related ocular trauma 26 years ago. The slight corneal opacity and Descemet membrane folds are seen in the direct illumination. The yellow iron line is marked by the yellow arrows and formed in parallel to the corneal center. (D) Corresponding topography of photo C. N = nasal; T = temporal. |
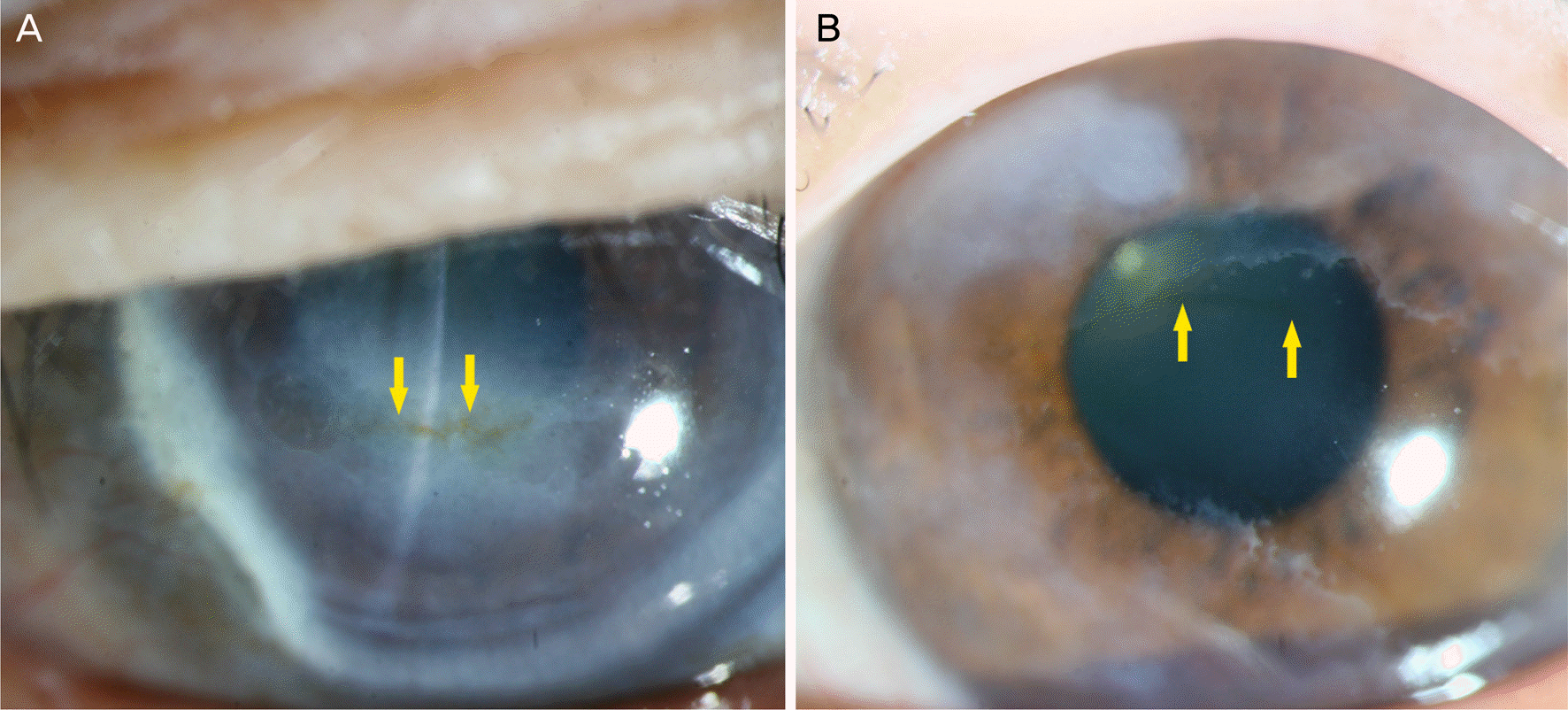 | Figure 7.Corneal iron lines with corneal degeneration. (A) Terrien marginal degeneration (slit-lamp photo). The temporal limbus and the central cornea become thinner and there is a severe opacity. Dark brown cornea iron line is formed in the central cornea (yellow arrows). (B) Salzmann nodular degeneration. Relatively protruded and grayish nodule is seen in the upper and lower edges of the cornea. The yellow arrows indicate corneal iron line formed around the nodule. |
Table 1.
Clinical features of eyes with corneal iron lines and fellow eyes
| Causes | Age (years) | Sex (male:female) | Number of cases (n, %) | Eyes with iron line BCVA (log MAR) | Fellow eyes BCVA (log MAR) | Correlation with front tangential curvature* | Progression |
|---|---|---|---|---|---|---|---|
| Herpetic stromal keratitis | 51.5 | 6:4 | 10 (25.6) | 0.67 | 0.29 | 1/1 (100%) | 1/10 (10%) |
| Hudson-Stähli line | 73.3 | 3:4 | 7 (17.9) | 0.07 | 0.09 | 0/2 (0%) | 0/7 (0%) |
| Cornea opacity after ulcer | 54.3 | 3:3 | 6 (15.3) | 0.60 | 0.16 | 3/3 (100%) | 0/6 (0%) |
| Keratoconus | 33.3 | 4:0 | 4 (10.3) | 0.70 | 0.18 | 3/4 (75%) | 0/4 (0%) |
| Pterygium | 66.3 | 2:1 | 3 (7.7) | 0.06 | 0.12 | 0/0 (0%) | 0/3 (0%) |
| Unclassified | 60.2 | 5:4 | 9 (23.1) | 0.77 | 0.60 | 1/2 (50%) | 1/9 (11%) |
| Total | 57.8 | 23:16 | 39 (100) | 9/12 (75%) | 2/39 (5%) |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download