Abstract
Purpose
To investigate the accuracy of intraocular lens power calculations using simulated keratometry (simK) of dual Scheimpflug analyzer and 5 types of formulas in cataract patients.
Methods
The keratometry (K), axial length (AXL) and anterior chamber depth (ACD) were measured using ultrasound biometry (USB) combined with auto-keratometry (Auto-K), parital coherence interferometry (PCI; IOL master®) and dual Scheimpflug analyzer (DSA; Galilei®) in 39 eyes of 39 patients. Predicted refraction was calculated using Auto-K, mean K of PCI, and simK and total corneal power (TCP) of DSA in the Sanders-Retzlaff-Kraff (SRK-T) formula. The SRK-II, SRK-T, Holladay II, Haigis, and Hoffer-Q formula were used to calculate predicted refraction with the simK of DSA and AXL of USB. Manifest refraction, mean numerical error (MNE) and mean absolute error were evaluated 1, 3 and 6 months after cataract surgery.
Results
TCP of DSA was lower compared with other keratometric values (p < 0.05). The MNE was not different among Auto-K, mean K and simK. The MNE using TCP was larger compared with Auto-K, mean K and simK at 1 month after surgery (p < 0.05). There was a difference in MNE between simK and TCP of DSA at 6 months after surgery (p < 0.05). The MNE of SRK-T formula was the smallest in the intraocular lens (IOL) power calculation using the simK of DSA.
References
1. Wang JK, Hu CY, Chang SW. Intraocular lens power calculation using the IOLMaster and various formulas in eyes with long axial length. J Cataract Refract Surg. 2008; 34:262–7.

2. Preussner PR, Olsen T, Hoffmann P, Findl O. Intraocular lens calculation accuracy limits in normal eyes. J Cataract Refract Surg. 2008; 34:802–8.
3. Drexler W, Findl O, Menapace R, et al. Partial coherence interferometry: a novel approach to biometry in cataract surgery. Am J Ophthalmol. 1998; 126:524–34.

4. Olsen T. Sources of error in intraocular lens power calculation. J Cataract Refract Surg. 1992; 18:125–9.

5. Lam AK, Chan R, Pang PC. The repeatability and accuracy of axial length and anterior chamber depth measurements from the IOLMaster. Ophthalmic Physiol Opt. 2001; 21:477–83.
6. Findl O, Drexler W, Menapace R, et al. High precision biometry of pseudophakic eyes using partial coherence interferometry. J Cataract Refract Surg. 1998; 24:1087–93.

7. Haigis W, Lege B, Miller N, Schneider B. Comparison of immersion ultrasound biometry and partial coherence interferometry for intraocular lens calculation according to Haigis. Graefes Arch Clin Exp Ophthalmol. 2000; 238:765–73.

8. Holladay JT. Standardizing constants for ultrasonic biometry, keratometry, and intraocular lens power calculations. J Cataract Refract Surg. 1997; 23:1356–70.

9. Saad E, Shammas MC, Shammas HJ. Scheimpflug corneal power measurements for intraocular lens power calculation in cataract surgery. Am J Ophthalmol. 2013; 156:460–7.e2.

10. Savini G, Barboni P, Carbonelli M, Hoffer KJ. Comparison of methods to measure cornealpower for intraocular lens power calculation using a rotating Scheimpflug camera. J Cataract Refract Surg. 2013; 39:598–604.
11. Saiki M, Negishi K, Kato N, et al. Ray tracing software for intraocular lens power calculation after corneal excimer laser surgery. Jpn J Ophthalmol. 2014; 58:276–81.

12. Savini G, Barboni P, Carbonelli M, Hoffer KJ. Accuracy of Scheimpflug corneal power measurements for intraocular lens power calculation. J Cataract Refract Surg. 2009; 35:1193–7.

13. Minami K, Kataoka Y, Matsunaga J, et al. Ray-tracing intraocular lens power calculation using anterior segment optical coherence tomography measurements. J Cataract Refract Surg. 2012; 38:1758–63.

14. Shammas HJ, Hoffer KJ, Shammas MC. Scheimpflug photography keratometry readings for routine intraocular lens power calculation. J Cataract Refract Surg. 2009; 35:330–4.

15. Savini G, Barboni P, Carbonelli M, Hoffer KJ. Accuracy of a dual Scheimpflug analyzer and a corneal topography system for intraocular lens power calculation in unoperated eyes. J Cataract Refract Surg. 2011; 37:72–6.

16. Shirayama M, Wang L, Koch DD, Weikert MP. Comparison of accuracy of intraocular lens calculations using automated keratometry, a Placido-based corneal topographer, and a combined Placido-based and dual Scheimpflug corneal topographer. Cornea. 2010; 29:1136–8.
17. Zaldivar R, Shultz MC, Davidorf JM, Holladay JT. Intraocular lens power calculations in patients with extreme myopia. J Cataract Refract Surg. 2000; 26:668–74.

19. Rose LT, Moshegov CN. Comparison of the Zeiss IOLMaster and applanation A-scan ultrasound: biometry for intraocular lens calculation. Clin Experiment Ophthalmol. 2003; 31:121–4.

20. Németh J, Fekete O, Pesztenlehrer N. Optical and ultrasound measurement of axial length and anterior chamber depth for intraocular lens power calculation. J Cataract Refract Surg. 2003; 29:85–8.

21. Utine CA, Altin F, Cakir H, Perente I. Comparison of anterior chamber depth measurements taken with the Pentacam, Orbscan IIz and IOLMaster in myopic and emmetropic eyes. Acta Ophthalmol. 2009; 87:386–91.

22. Reddy AR, Pande MV, Finn P, El-Gogary H. Comparative estimation of anterior chamber depth by ultrasonography, Orbscan II, and IOLMaster. J Cataract Refract Surg. 2004; 30:1268–71.

23. Jonna G, Channa P. Updated practical intraocular lens power calculation after refractive surgery. Curr Opin Ophthalmol. 2013; 24:275–80.

Figure 1.
Mean K according to biometry. (A) TCP is low er com pared to auto-keratometry (Auto-K), PCI and simK (p < 0.001 for all, paired t-test). (B) TCP is correlated with PCI (r = 0.653, p < 0.001, Pearson correlation analysis). K = keratometry; PCI = partial coherence interferometry; simK = simulated keratometry; TCP = total corneal power. *Statistically significant.
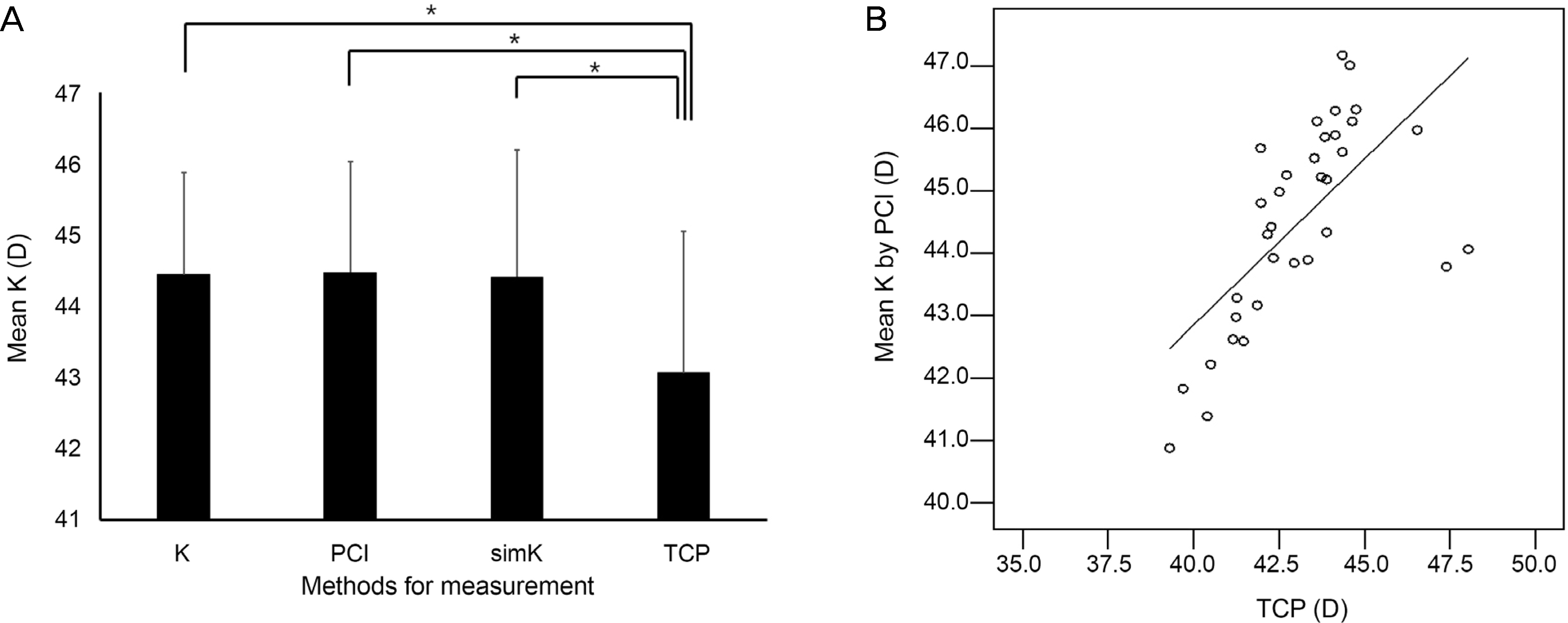
Figure 2.
Correlation between AXL measured by USB and PCI and Bland-Altman plot of axial length between USB and PCI. (A) Axial length measured by USB was well correlated with PCI (r = 0.965, p < 0.001, Pearson correlation analysis). (B) 95% limits of agreement for axial length difference (USB-PCI) is −0.45 to 0.37. PCI = partial coherence interferometry; AXL = axial lengths; USB = ultrasound biometry; SD = standard deviation.
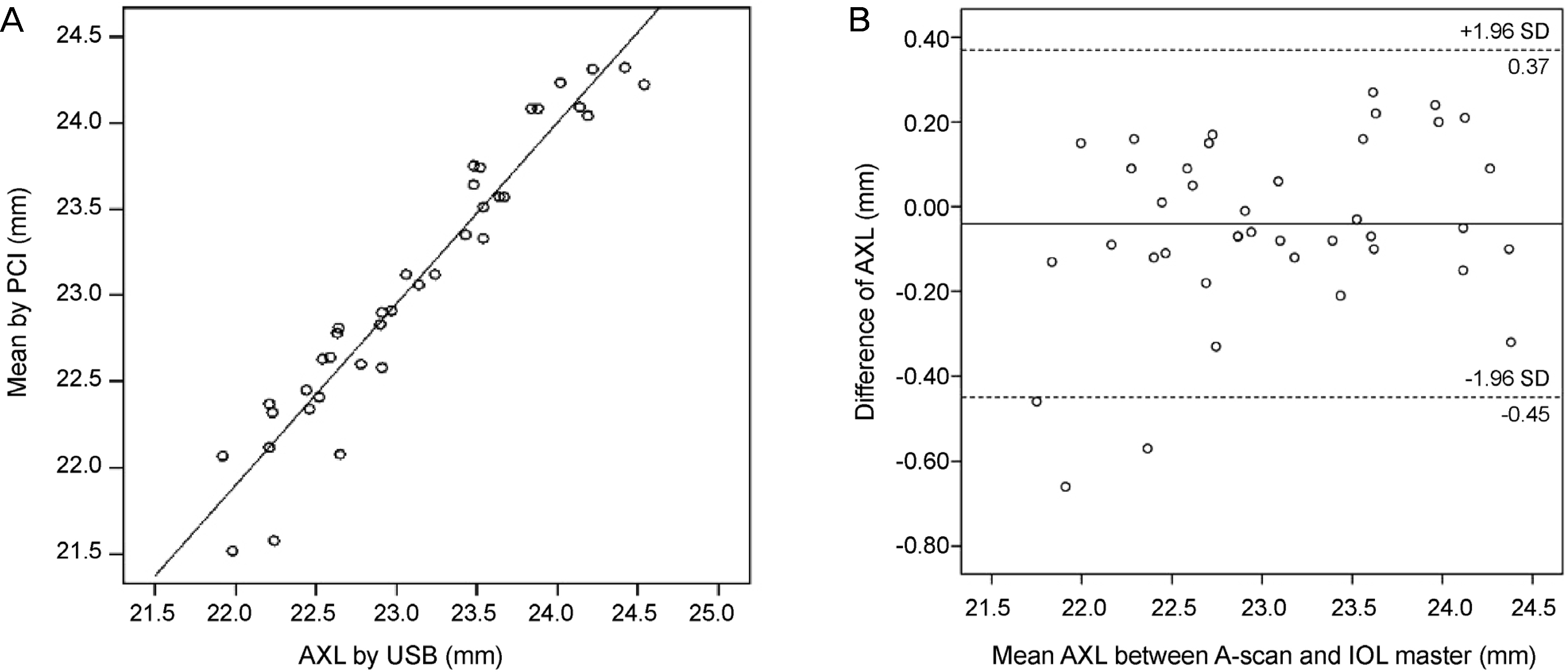
Figure 3.
Correlation and Bland-Altman plot of ACD between USB and PCI or DSA. (A) ACD measured by PCI was well correlated with USB (r = 0.811, p < 0.001, Pearson correlation analysis). (B) ACD measured by DSA was well correlated with USB (r = 0.982, p < 0.001, Pearson correlation analysis). (C) 95% limits of agreement for ACD difference (USB-PCI) was −0.57 to 0.59. (D) 95% limits of agreement for ACD difference (USB-DSA) was −0.18 to 0.16. ACD = anterior chamber depth; USB = ultrasound biometry; PCI = partial coherence interferometry; DSA = dual Scheimpflug analyzer; SD = standard deviation.
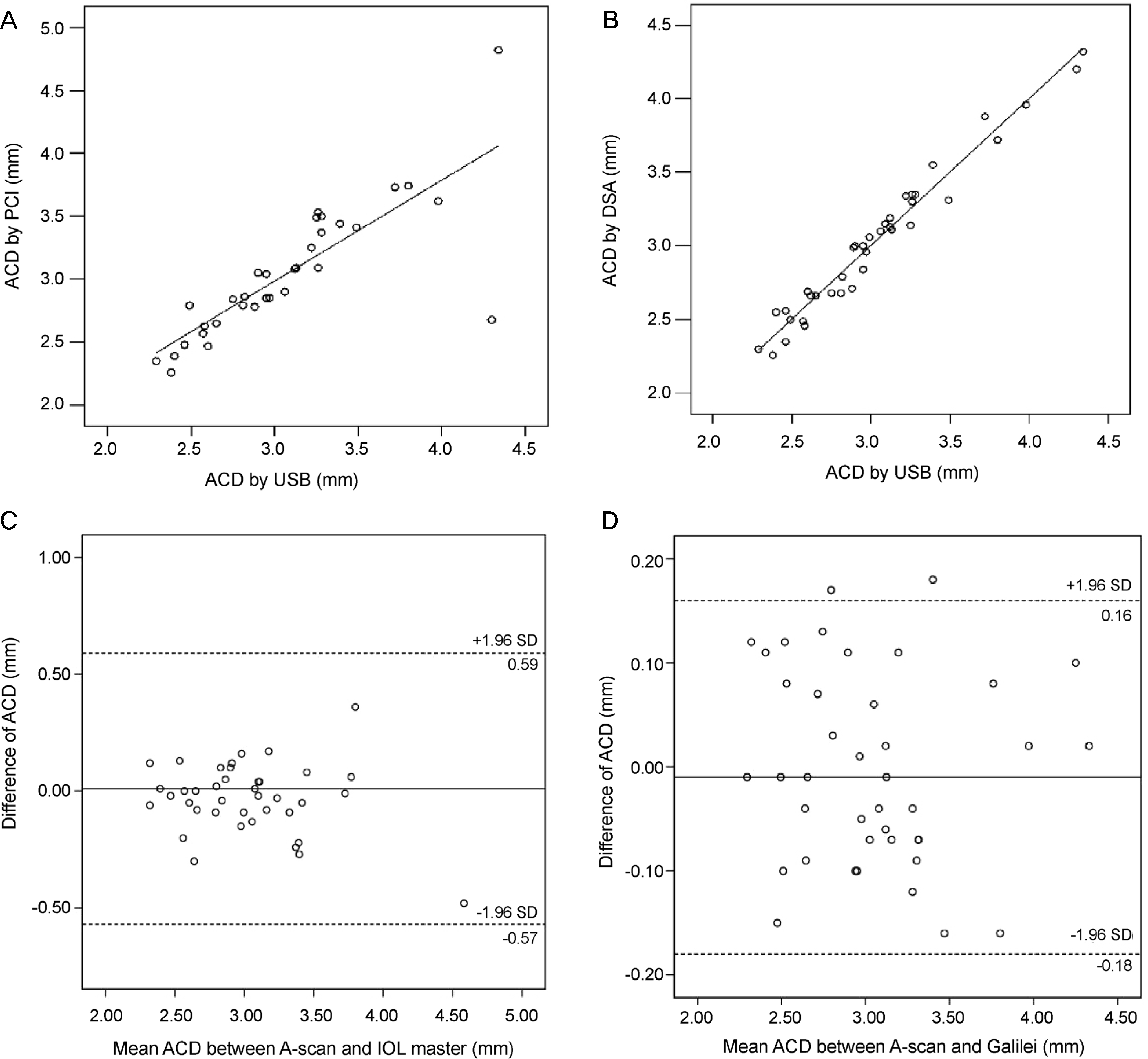
Figure 4.
Predicted refraction according to biometry or formula. (A) Predicted refraction is not different between PCI and Auto-K combined with USB or between PCI and DSA. Predicted refraction is different between USB and DSA (p=0.045, paired t-test). Predicted refraction calculated using TCP is higher compared with other methods (p = 0.003 for all, paired t-test). (B) Predicted refraction is different between formulas (p < 0.05, paired t-test). PCI = partial coherence interferometry; Auto-K = auto-keratometry; USB = ultrasound biometry; DSA = dual Scheimpflug analyzer; simK = simulated keratometry; TCP = total corneal power; SRK = Sanders-Retzlaff-Kraff. *Statistically significant.
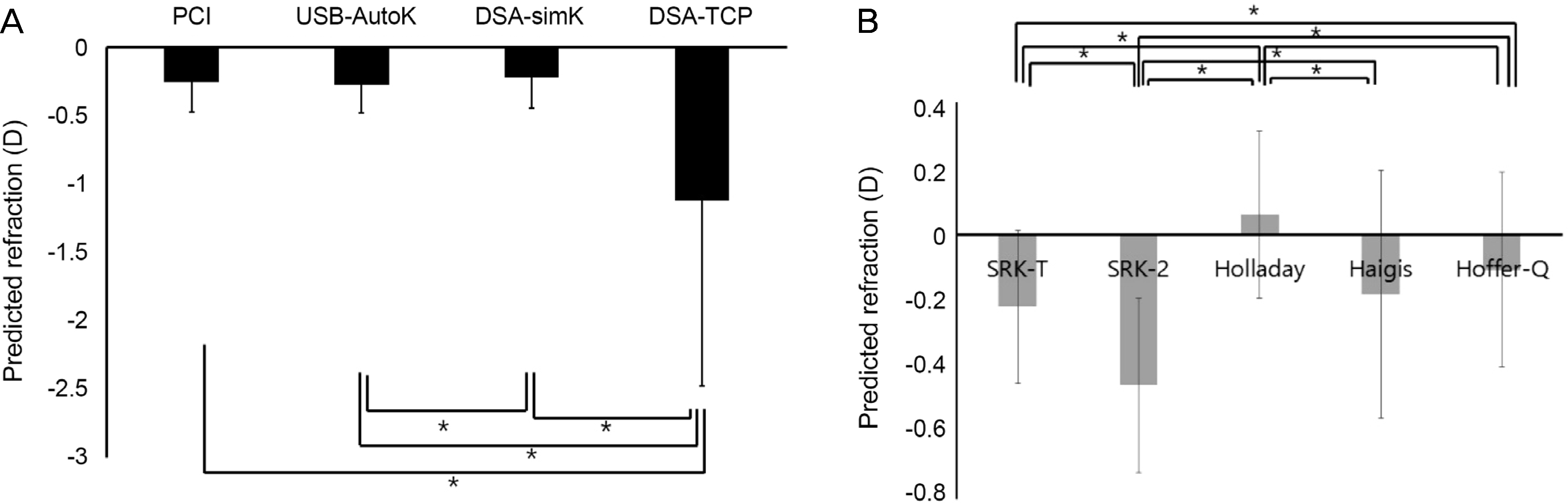
Figure 5.
Change in MRSE overtime. There is no significant change over time (Wilcoxon rank test). MRSE = manifest refraction spherical equivalent.
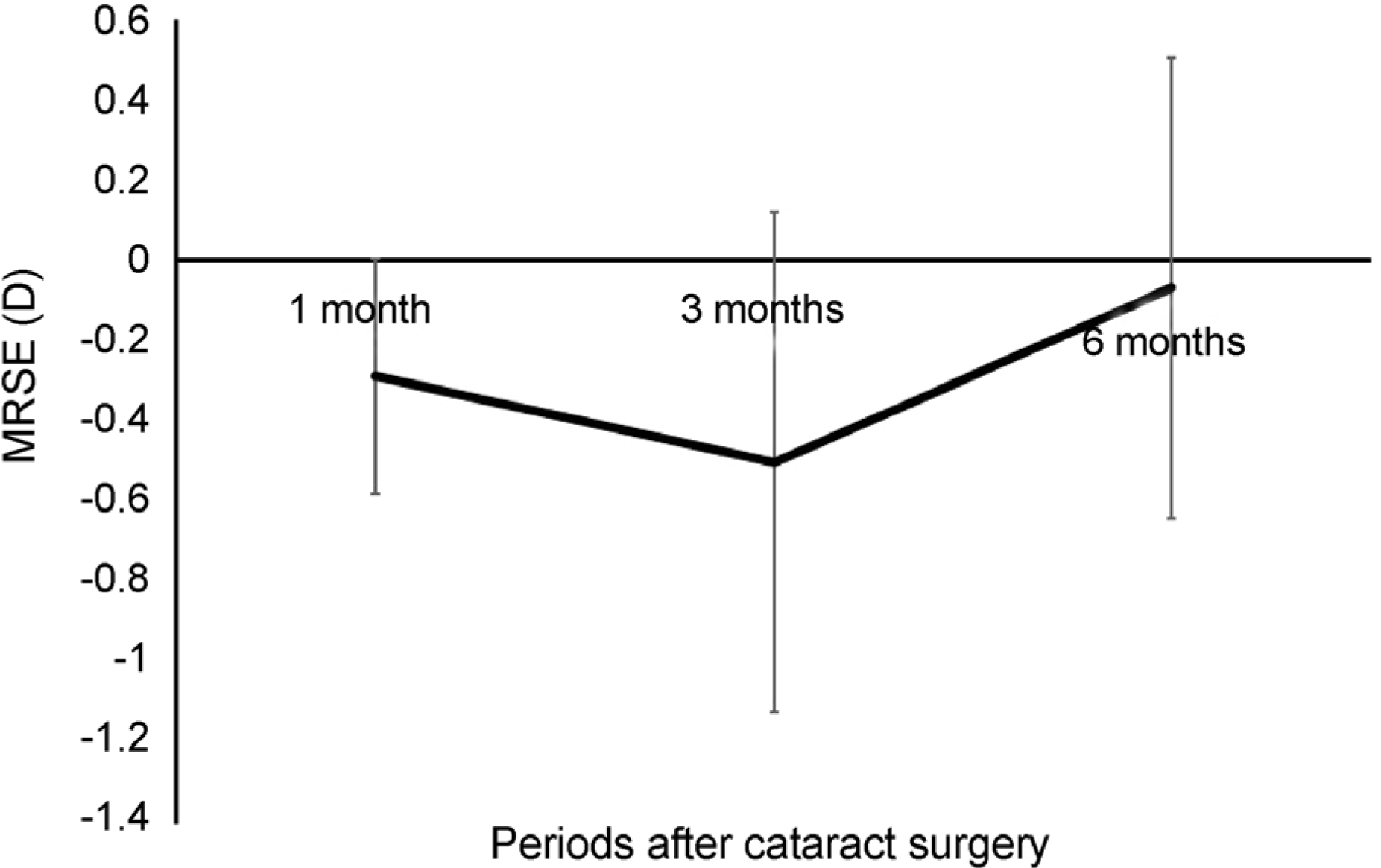
Figure 6.
MNE according to biometry overtime. MNE is not different between PCI, Auto-K combined with USB and DSA 1 month and 3 months after surgery. However, MNE calculated with DSA-simK is lower compared to USB (p = 0.046, Wilcoxon rank test). MNE using TCP is higher compared to other methods 1 month after surgery (p = 0.023, 0.013 and 0.009), and higher compared to DSA-simK 3 months and 6 months after surgery (p = 0.042 and 0.039). MNE = mean numerical error; PCI = partial coherence interferometry; Auto-K = auto-keratometry; USB = ultrasound biometry; DSA = dual Scheimpflug analyzer; simK = simulated keratometry; TCP = total corneal power. *Statistically significant.
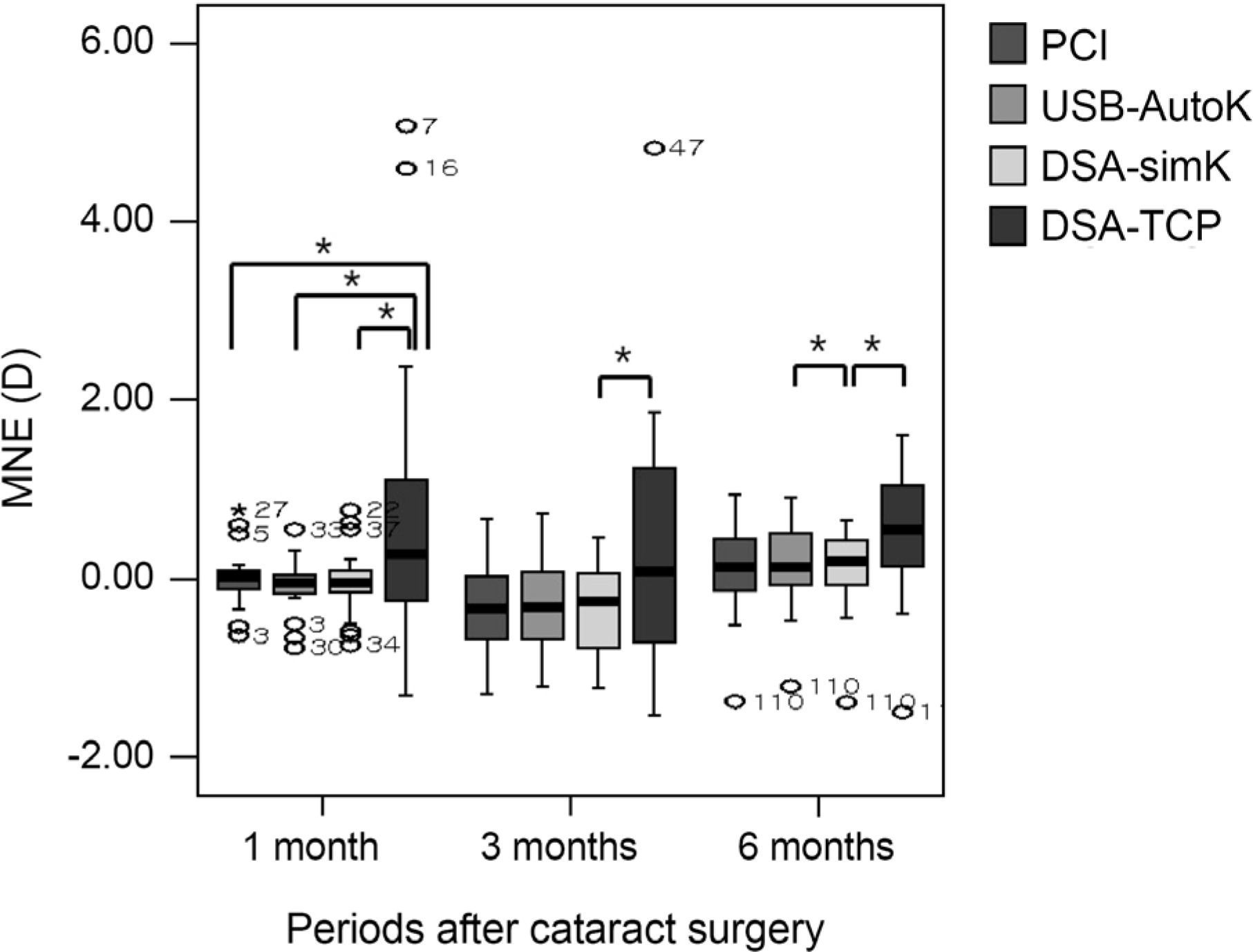
Figure 7.
MNE according to formula overtime. MNE by SRK-T is lower compared with SRK-2, Holladay or Hoffer-Q formula 1 month after surgery (p = 0.006, < 0.001, and 0.001, respectively, Wilcoxon rank test). MNE by Haigis formula was lower compared with SRK-2, Holladay or Hoffer-Q form ula 1 month after surgery (p < 0.001 for all). SRK-2 and Haigis are lower compared with Holladay formula 1 month after surgery (p < 0.001 for both, respectively). MNE by SRK-T is lower compared with SRK-2, Holladay or Hoffer-Q formula 6 month after surgery (p = 0.014, 0.001, and 0.018, respectively). MNE by Haigis formula is lower compared with SRK-2, Holladay or Hoffer-Q formula 6 month after surgery (p = 0.012, < 0.001 and 0.001, respectively). SRK-2 and Haigis are lower compared with Holladay formula (p < 0.001 and 0.003, respectively). MNE = mean numerical error; SRK-T = Sanders-Retzlaff-Kraff theoretical formula.
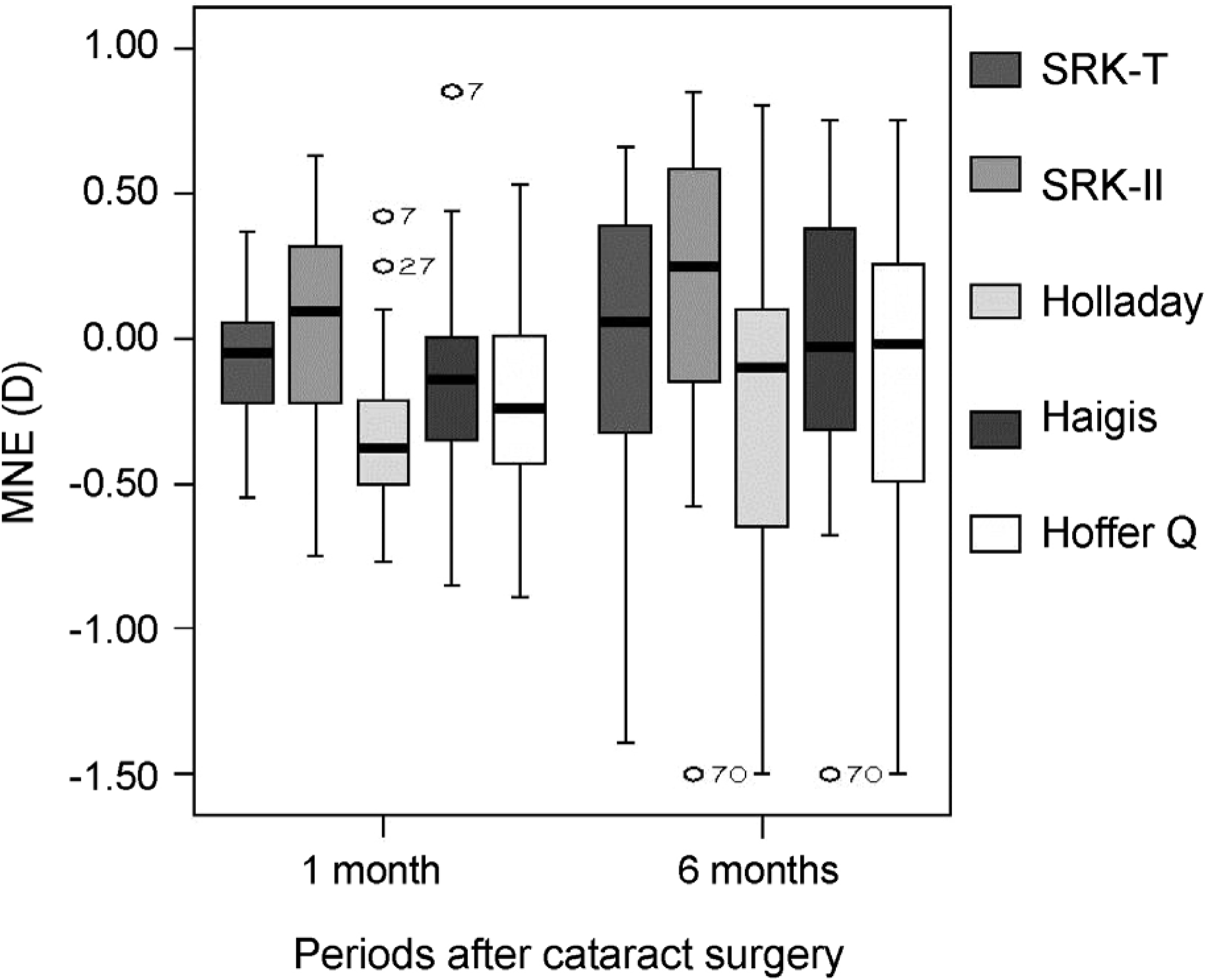
Table 1.
Demographics and biometry measurements by PCI, USB, and DSA
| PCI | USB-Auto K | DSA-simK | DSA-TCP | p-value | |
|---|---|---|---|---|---|
| AXL (mm) | 23.04 ± 0.79 | 23.08 ± 0.72 | − | − | 0.289 |
| ACD (mm) | 3.02 ± 0.48 | 3.03 ± 0.49 | 3.04 ± 0.50 | − | 0.822 |
| Mean K (diopter) | 44.51 ± 1.59 | 44.38 ± 1.52 | 44.42 ± 1.53 | 43.07 ± 1.98* | <0.001† |
Table 2.
Comparison of prediction error and proportion ratio among PCI, USB, and DSA
| PCI | USB | DSA-simK | DSA-TCP | p-value | |
|---|---|---|---|---|---|
| 1 month after surgery | |||||
| MNE (D) | −0.01 ± 0.25 | −0.06 ± 0.26 | −0.06 ± 0.30 | 0.46 ± 1.28 | 0.001* |
| MAE (D) | 0.14 ± 0.18 | 0.17 ± 0.20 | 0.22 ± 0.22 | 0.93 ± 1.01 | |
| No. of MAE < 0.5 D (%) | 36 (90.0%) | 34 (85.0%) | 32 (80.0%) | 21 (52.5%) | 0.000† |
| No. of MAE < 1.0 D (%) | 39 (100.0%) | 39 (100.0%) | 39 (100.0%) | 27 (67.5%) | 0.000† |
| 6 months after surgery | |||||
| MNE (D) | 0.04 ± 0.59 | 0.07 ± 0.56 | −0.02 ± 0.53 | 0.29 ± 0.79 | 0.471 |
| MAE (D) | 0.40 ± 0.34 | 0.42 ± 0.31 | 0.38 ± 0.31 | 0.63 ± 0.55 | |
| No. of MAE <0.5 D (%) | 12 (63.2%) | 13 (68.4%) | 14 (78.9%) | 7 (43.8%) | 0.181 |
| No. of MAE <1.0 D (%) | 17 (89.5%) | 18 (94.7%) | 18 (94.7%) | 12 (75.0%) | 0.212 |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download