Abstract
Purpose
We compared the outcomes of laser iridotomy and primary phacoemulsification when treating acute angle-closure glaucoma.
Methods
This study was conducted with 61 patients diagnosed with acute angle closure glaucoma from January, 2005 to January, 2015. The patients received either laser iridotomy or primary phacoemulsification. The age and gender of each patient, differences of intraocular pressure (IOP) before and after treatment, visual acuity, need for IOP lowering agents and complications were analyzed retrospectively at 1-day, 1-month, 6-month and 12-month after the treatment. Patients who received laser iridotomy with phacoemulsification or trabeculectomy were excluded from this study. Additionally, we included only cases in which treatments were given within 3 days after the onset of symptom.
Results
Among the 61 patients, 45 patients received laser iridotomy and 16 patients received primary phacoemulsification. One day after the treatment the laser iridotomy group showed better outcome in their visual acuity (log MAR 0.62 ± 0.51; p = 0.048). At 6-month postoperatively, the primary phacoemulsification group showed better visual acuity (log MAR 0.07 ± 0.15; p = 0.013). However, at 12-month postoperatively, the visual acuities were not significantly different between the 2 groups. Regarding IOP, at postoperative 1-month, the group of primary phacoemulsification shows significantly lower IOP (9.5 ± 1.3 mm Hg), compared with the group of laser iridotomy. A significant difference was observed in the number of IOP lowering agents that patients at 12 month after the treatment. There were no severe complications in either group.
Conclusions
Following the initial treatment of acute angle-closure glaucoma, the primary phacoemulsification showed no significant differences in postoperative visual acuity, IOP and complications compared to the outcomes of laser iridotomy. Additionally, the need for IOP lowering agents was less in the primary phacoemulsification groups at 1 year after the operation.
Go to : 
REFERENCES
1). Choong YF, Irfan S, Menage MJ. Acute angle closure glaucoma: an evaluation of a protocol for acute treatment. Eye (Lond). 1999; 13((Pt 5)):613–6.

2). Tello C, Tran HV, Liebmann J, Ritch R. Angle closure: classification, concepts, and the role of ultrasound biomicroscopy in diagnosis and treatment. Semin Ophthalmol. 2002; 17:69–78.

4). Aung T, Ang LP, Chan SP, Chew PT. Acute primary angle-closure: long-term intraocular pressure outcome in Asian eyes. Am J Ophthalmol. 2001; 131:7–12.

5). Jacobi PC, Dietlein TS, Lüke C, et al. Primary phacoemulsification and intraocular lens implantation for acute angle-closure glaucoma. Ophthalmology. 2002; 109:1597–603.
6). Kim YW, Kim SD, Kim JD. Influence of lens factor and effect of selected cataract extraction on acute angle-closure glaucoma. J Korean Ophthalmol Soc. 2005; 46:1144–50.
7). Yoon JY, Hong JY, Kim CY. Cataract surgery in patients with acute primary angle-closure glaucoma. Korean J Ophthalmol. 2003; 17:122–6.

8). Lee KS, Kim SK, Kim EK, Kim TI. Comparison of intraocular pressure measured by non-contact tonometer, rebound tonometer, tono-pen, and Goldmann applanation tonometer. J Korean Ophthalmol Soc. 2014; 55:47–53.

9). Ritch R, Lowe RF. Angle-closure glaucoma: therapeutic overview. Ritch R, Shields MB, Krupin T, editors. The Glaucomas. 2nd ed.St Louis: Mosby;1996. chap. 74.
10). Kee HS, Kim SJ, Yang KJ. Clinical study on primary acute angle closure glaucoma. J Korean Ophthalmol Soc. 1995; 36:499–504.
11). An JW, On KK, Kim JD. Biometric measurements in acute angle closure glaucoma. J Korean Ophthalmol Soc. 1993; 34:648–53.
12). Lai JS, Tham CC, Chan JC. The clinical outcomes of cataract extraction by phacoemulsification in eyes with primary angle-closure glaucoma (PACG) and co-existing cataract: a prospective case series. J Glaucoma. 2006; 15:47–52.

13). Khokhar S, Sindhu N, Pangtey MS. Phacoemulsification in filtered chronic angle closure glaucoma eyes. Clin Experiment Ophthalmol. 2002; 30:256–60.

14). Kim YY, Jung HR. Clarifying the nomenclature for primary angle-closure glaucoma. Surv Ophthalmol. 1997; 42:125–36.

15). Lam DS, Leung DY, Tham CC, et al. Randomized trial of early phacoemulsification versus peripheral iridotomy to prevent intraocular pressure rise after acute primary angle closure. Ophthalmology. 2008; 115:1134–40.

16). Husain R, Gazzard G, Aung T, et al. Initial management of acute primary angle closure: a randomized trial comparing phacoemulsification with laser peripheral iridotomy. Ophthalmology. 2012; 119:2274–81.
Go to : 
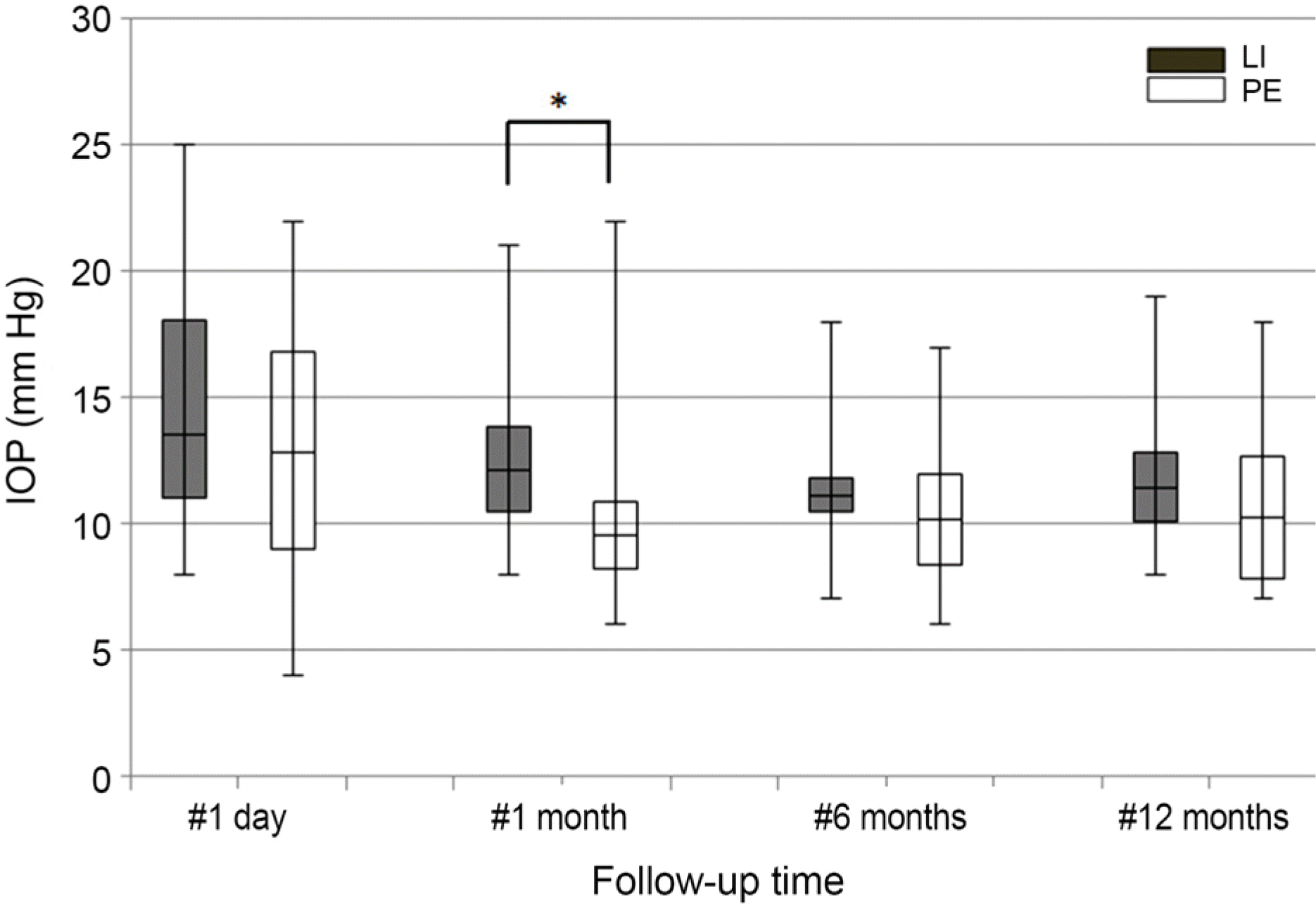 | Figure 1.Intraocular pressure after laser iridotomy and phacoemulsification. At postoperative 1 month, the group of primary phacoemulsification shows significantly lower intraocular pressure compared with the group of laser iridotomy (p = 0.032), but there's no other significance difference statistically between two groups (by Mann-Whitney U-test). IOP = intraocular pressure; LI = laser iridotomy; PE= phacoemulsification. * p<0.05. |
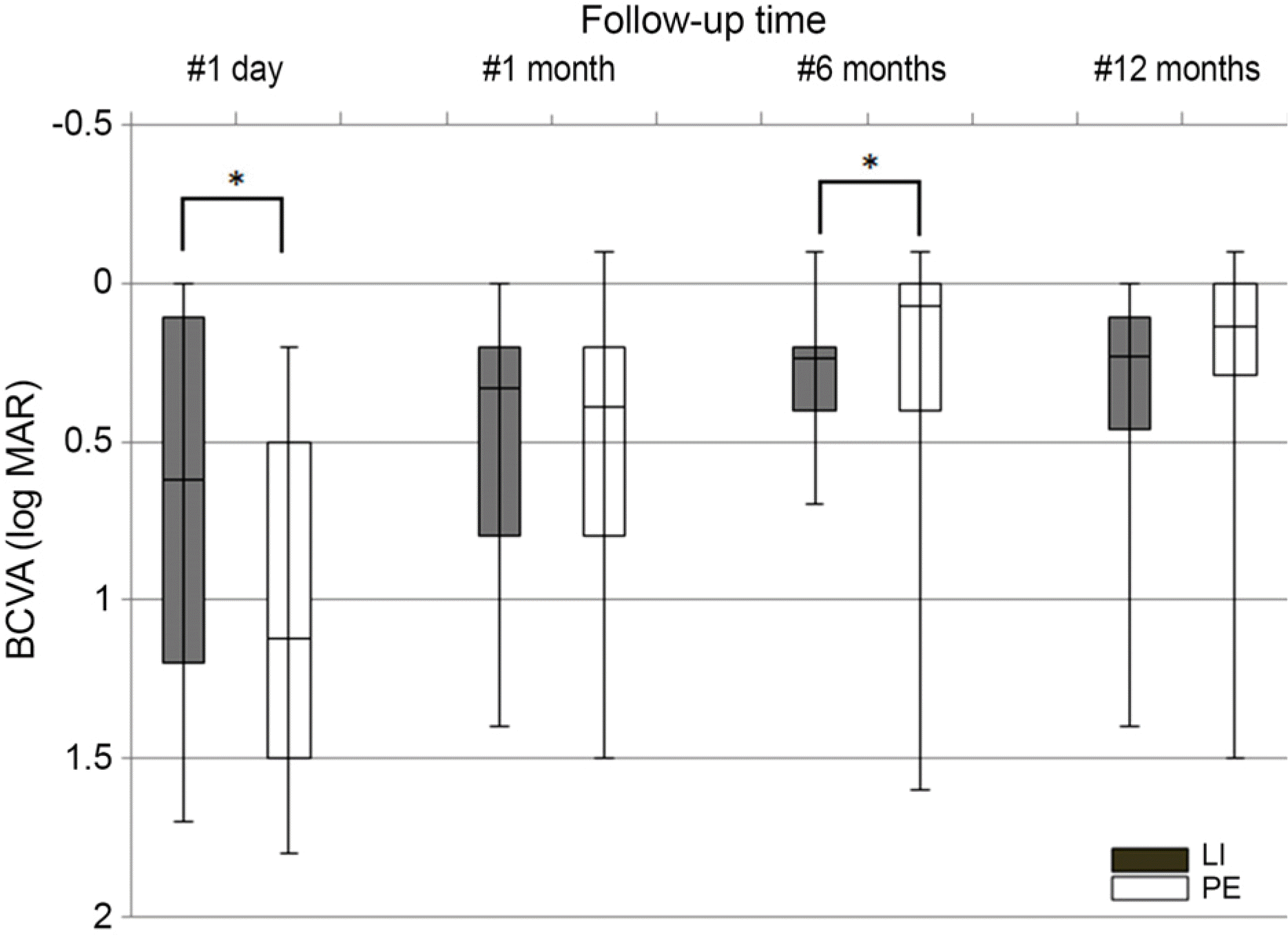 | Figure 2.BCVA after laser iridotomy and phacoemulsification. On the day after the operation, laser iridotomy group had the better outcome in their vision (log MAR) 0.62 ± 0.51 (p = 0.048), At 6 months after operation, primary phacoemulsification group has the better vision (log MAR) 0.07 ± 0.15 (p = 0.013), respectively. But other period, the vision outcomes between two groups show no significance difference (by Mann-Whitney U-test). BCVA = best corrected visual acuity; LI = laser iridotomy; 1.4 mmHg PE= phacoemulsification. *p<0.05. |
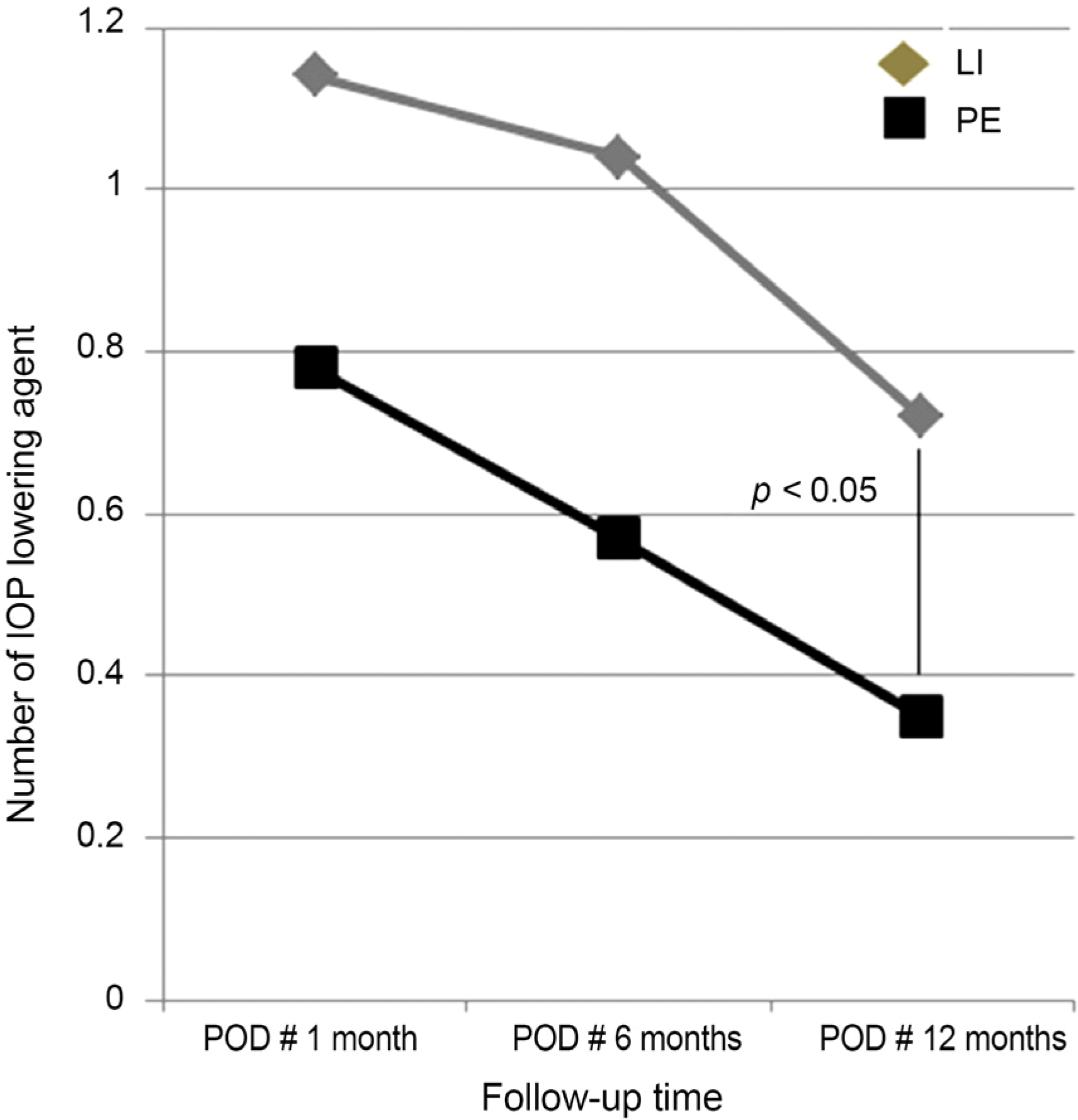 | Figure 3.The need for intraocular pressure lowering agent after laser iridotomy and phacoemulsification. The need for intraocular pressure lowering agent is lower in the initial laser iridotomy and primary phacoemulsification at the point of one year after the operation (p = 0.031, Mann-Whitney U-test). IOP = intraocular pressure; LI = laser iridotomy; PE = phacoemulsification; POD = postoperative day. |
Table 1.
Preoperative clinical characteristics
| LI (N = 45) | PE (N = 16) | p-value | |
|---|---|---|---|
| Age | 69.0 ± 8.53 | 66.8 ± 7.57 | 0.071* |
| Sex (male:female) | 14:31 | 3:13 | 0.344† |
| Direction (right:left) | 15:30 | 6:10 | 0.224† |
| Hypertension | 14 | 7 | 0.763† |
| Diabetes mellitus | 1 | 1 | 0.679† |
| IOP (mm Hg) | 50.34 ± 19.92 | 51.10 ± 18.55 | 0.661* |
| BCVA (log MAR) | 1.24 ± 0.43 | 1.75 ± 0.92 | 0.078* |
| Axial length (mm) | 22.13 ± 0.39 | 22.10 ± 0.44 | 0.483* |
| ACD (mm) | 2.37 ± 0.24 | 2.38 ± 0.46 | 0.321* |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download