Abstract
Purpose
To compare the clinical outcomes of glistening-free intraocular lens (IOL) and conventional 1-piece aspheric IOL in implanted in-the-bag.
Methods
After phacoemulsification performed by a single surgeon, 2 different IOLs were implanted: enVista MX60 (glistening-free 1-piece aspheric IOL) in 38 eyes (group A) and AcrySof IQ (conventional 1-piece aspheric IOL) in 46 eyes (group B). Glare symptom score (0-5) obtained by questionnaires, best corrected visual acuity (BCVA), Functional Acuity Contrast Test (FACT), posterior capsular opacity (PCO), glistening formation and spherical equivalent error were compared and analyzed preoperatively and 6 months and 12 months postoperatively.
Results
A statistically significant improvement of BCVA and contrast sensitivity postoperatively was observed in all groups. There was statistically significant increase of glistening in group B compared with group A. However, there was no significant difference of FACT scores of spatial frequency in A, B, C, D and E columns and glare symptom score (0-10) obtained by questionnaires 12 months after surgery. Spherical equivalent errors were -0.38 ± 0.27 D and -0.36 ± 0.28 D for groups A and B, respectively. PCO occurred in 2 eyes in group A and 4 eyes in group B.
Go to : 
REFERENCES
1). Dhaliwal DK, Mamalis N, Olson RJ, et al. Visual significance of glistenings seen in the AcrySof intraocular lens. J Cataract Refract Surg. 1996; 22:452–7.

2). Davison JA. Clinical performance of Alcon SA30AL and SA60AT single-piece acrylic intraocular lenses. J Cataract Refract Surg. 2002; 28:1112–23.

3). Waite A, Faulkner N, Olson RJ. Glistenings in the single-piece, hydrophobic, acrylic intraocular lenses. Am J Ophthalmol. 2007; 144:143–4.

4). Nishihara H, Kageyama T, Ohnishi T, et al. Glistenings in lathe-cut acrylic intraocular lens. Ganka Shujutsu. 2000; 13:227–30.
5). Omar O, Pirayesh A, Mamalis N, Olson RJ. In vitro analysis of AcrySof intraocular lens glistenings in AcryPak and Wagon Wheel packaging. J Cataract Refract Surg. 1998; 24:107–13.

6). Ayaki M, Nishihara H, Yaguchi S, Koide R. Effect of ophthalmic solution components on acrylic intraocular lenses. J Cataract Refract Surg. 2007; 33:122–6.

7). Oshika T, Shiokawa Y, Amano S, Mitomo K. Influence of glistenings on the optical quality of acrylic foldable intraocular lens. Br J Ophthalmol. 2001; 85:1034–7.

8). Choi YJ, Han KE, Ahn JM, et al. Comparisons of clinical results after implantation of three aspheric intraocular lenses. J Korean Ophthalmol Soc. 2013; 54:251–6.

9). Lee K, Yoon MH, Seo KY, et al. Comparisons of clinical results after implantation of three aspheric intraocular lenses. J Korean Ophthalmol Soc. 2013; 54:1213–8.

10). Han J, Han KE, Ahn JM, et al. Influence of pupil size on visual acuity after implantation of the TECNIS 1-piece intraocular lens. J Korean Ophthalmol Soc. 2012; 53:1615–20.

11). Kwak AY, Choi M, Seo KY, Ahn JM. Comparison of optical quality between two intraocular lenses using double-pass based optical quality analysis system. J Korean Ophthalmol Soc. 2013; 54:1818–23.

12). Parede TR, Torricelli AA, Mukai A, et al. Quality of vision in refractive and cataract surgery, indirect measurers: review article. Arq Bras Oftalmol. 2013; 76:386–90.

13). Cheon MH, Lee JE, Kim JH, et al. One-year outcome of monocular implant of aspheric multifocal IOL. J Korean Ophthalmol Soc. 2010; 51:822–8.

14). Wejde G, Kugelberg M, Zetterström C. Posterior capsule opacification: comparison of 3 intraocular lenses of different materials and design. J Cataract Refract Surg. 2003; 29:1556–9.

15). Ginsburg AP, Evans DW, Sekule R, Harp SA. Contrast sensitivity predicts pilots' performance in aircraft simulators. Am J Optom Physiol Opt. 1982; 59:105–9.

16). Pesudovs K, Hazel CA, Doran RM, Elliott DB. The usefulness of Vistech and FACT contrast sensitivity charts for cataract and refractive surgery outcomes research. Br J Ophthalmol. 2004; 88:11–6.

17). Holladay JT, Piers PA, Koranyi G, et al. A new intraocular lens design to reduce spherical aberration of pseudophakic eyes. J Refract Surg. 2002; 18:683–91.

18). Bae HW, Kim EK, Kim TI. Spherical aberration, contrast sensitivity and depth of focus with three aspherical intraocular lenses. J Korean Ophthalmol Soc. 2009; 50:1639–44.

19). Son SW, Seo JW, Shin SJ, Chung SK. Comparison of the stability between three-piece and single-piece aspheric intraocular lenses. J Korean Ophthalmol Soc. 2010; 51:1584–9.

20). Miyata A, Yaguchi S. Equilibrium water content and glistenings in acrylic intraocular lenses. J Cataract Refract Surg. 2004; 30:1768–72.

21). Apple DJ, Mamalis N, Olson RJ, Kincaid MC. Intraocular Lenses: evolution, designs, complications, and pathology. Baltimore: Williams & Wilkins;1989. p. 11–41.
22). Saylor DM, Coleman Richardson D, Dair BJ, Pollack SK. Osmotic cavitation of elastomeric intraocular lenses. Acta Biomater. 2010; 6:1090–8.

23). Gregori NZ, Spencer TS, Mamalis N, Olson RJ. In vitro comparison of glistening formation among hydrophobic acrylic intraocular lenses(1). J Cataract Refract Surg. 2002; 28:1262–8.
24). Packer M, Fry L, Lavery KT, et al. Safety and effectiveness of a glistening-free single-piece hydrophobic acrylic intraocular lens (enVista). Clin Ophthalmol. 2013; 7:1905–12.

25). Heiner P, Ligabue E, Fan A, Lam D. Safety and effectiveness of a single-piece hydrophobic acrylic intraocular lens (enVista[R]) - results of a European and Asian-Pacific study. Clin Ophthalmol. 2014; 8:629–35.
26). Leydolt C, Schriefl S, Stifter E, et al. Posterior capsule opacification with the iMics1 NY-60 and AcrySof SN60WF 1-piece hydrophobic acrylic intraocular lenses: 3-year results of a randomized trial. Am J Ophthalmol. 2013; 156:375–81. e2.

27). Colin J, Orignac I, Touboul D. Glistenings in a large series of hydrophobic acrylic intraocular lenses. J Cataract Refract Surg. 2009; 35:2121–6.

28). Hayashi K, Hirata A, Yoshida M, et al. Long-term effect of surface light scattering and glistenings of intraocular lenses on visual function. Am J Ophthalmol. 2012; 154:240–51. e2.

29). Christiansen G, Durcan FJ, Olson RJ, Christiansen K. Glistenings in the AcrySof intraocular lens: pilot study. J Cataract Refract Surg. 2001; 27:728–33.

Go to : 
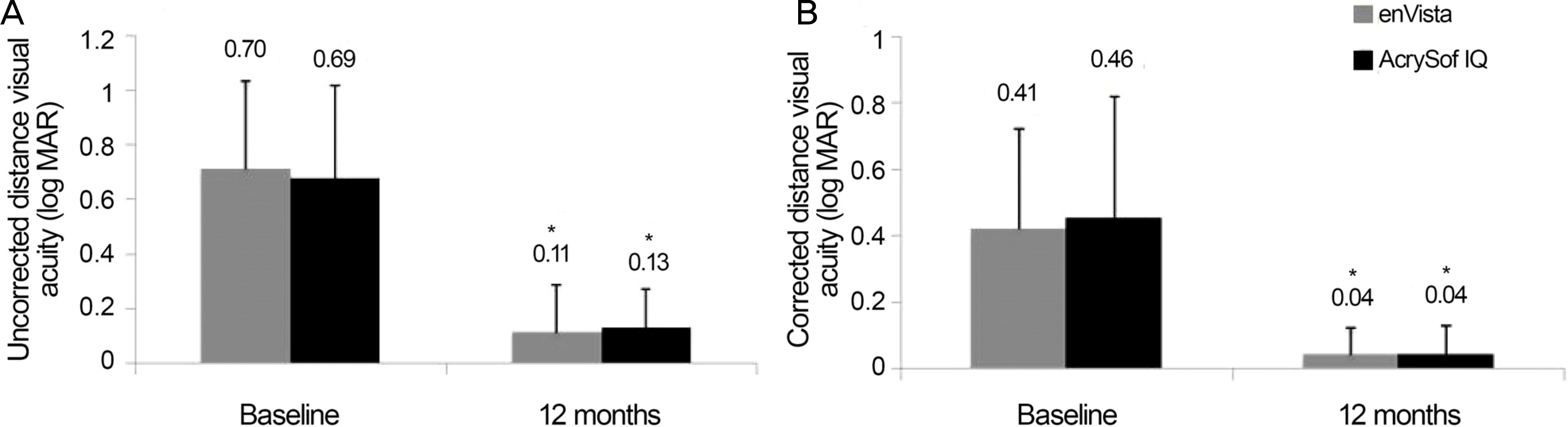 | Figure 1.Visual acuity (VA) at baseline and postoperative 12 months. (A) Uncorrected VA at baseline and postoperative 12 months. (B) Corrected VA at baseline and postoperative 12 months. log MAR =logarithm of the minimum angle of resolution. * p<0.001 compared with baseline. |
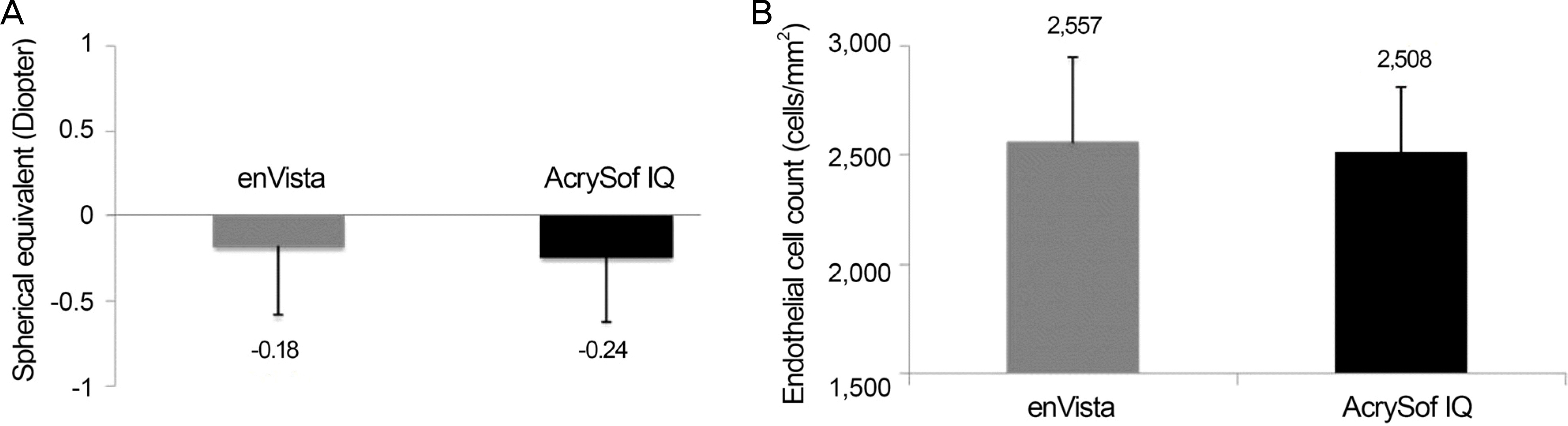 | Figure 2.Spherical equivalents and endothelial cell counts. (A) Spherical equivalents at postoperative 12 months in the enVista® MX60 and Acrysof® IQ SN60WF groups. (B) Endothelial cell counts at postoperative 12 months in the enVista® MX60 and Acrysof® IQ SN60WF groups. |
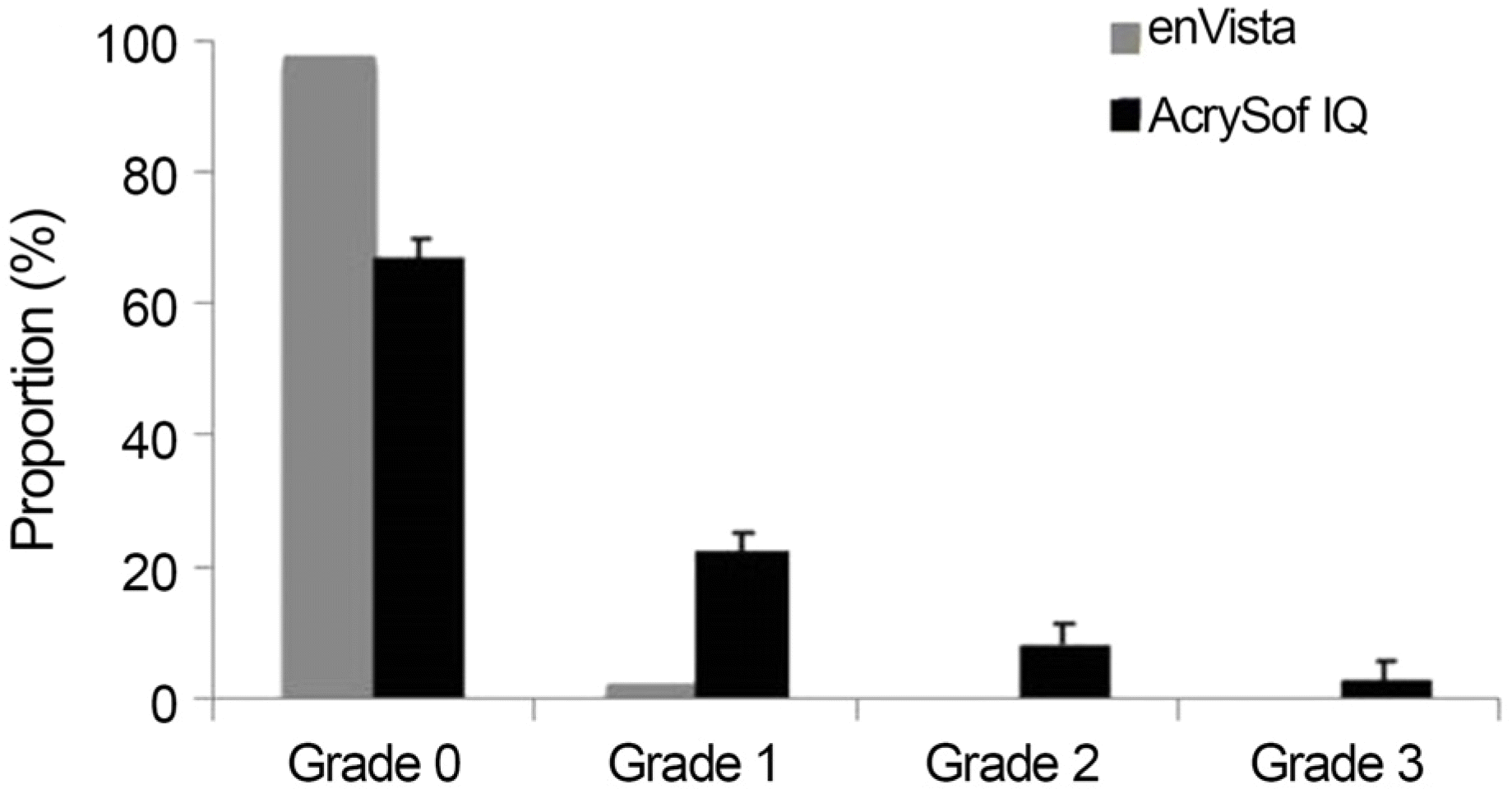
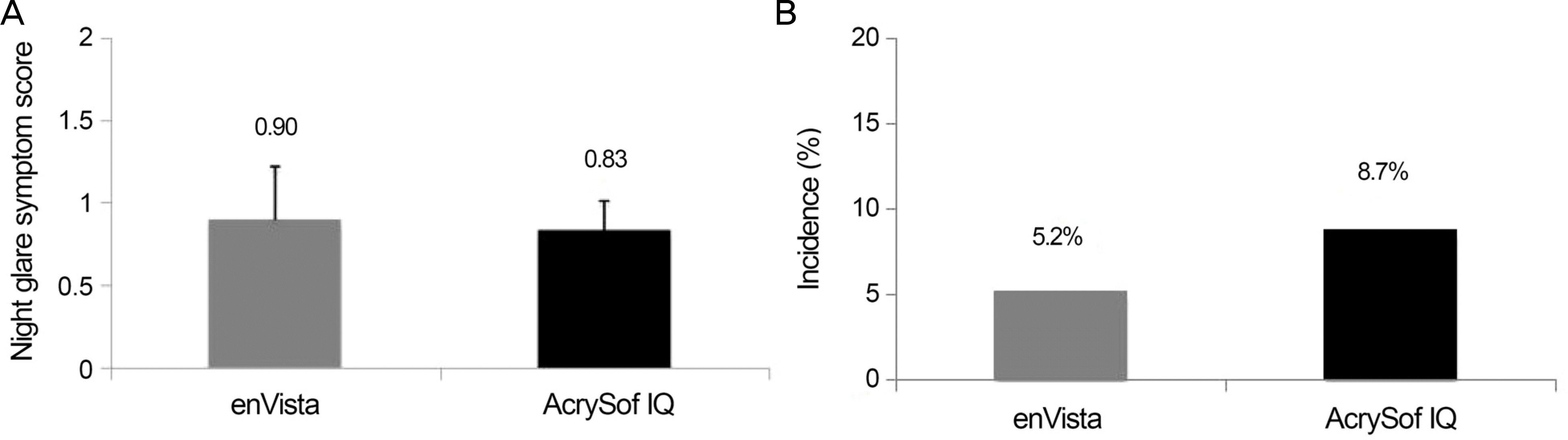 | Figure 3.Night glare symptom scores and incidence of posterior capsular opacity. (A) Night glare symptom scores at postoperative 12 months in the enVista® MX60 and Acrysof®IQ SN60WF groups. (B) Incidence of posterior capsular opacity at postoperative 12 months in the enVista® MX60 and Acrysof®IQ SN60WF groups. |
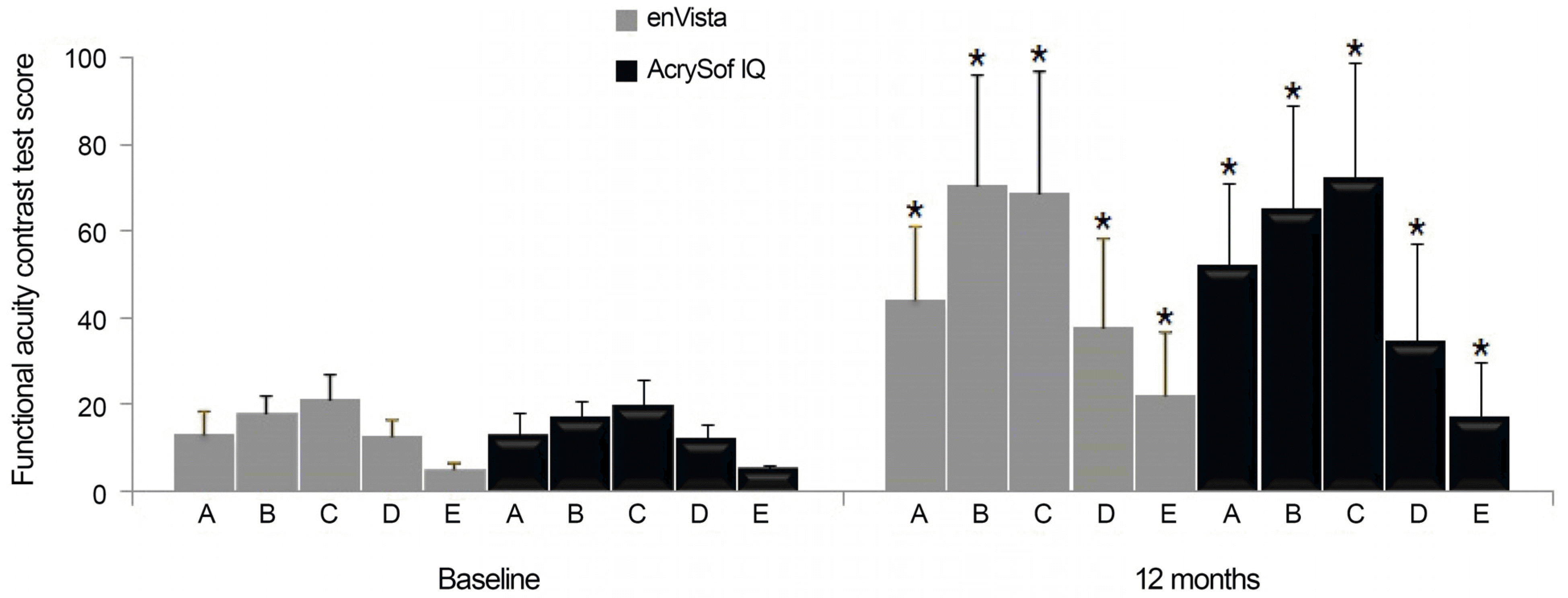 | Figure 5.Functional Acuity Contrast Test scores at baseline and postoperative 12 months. ‘A' means ‘spatial frequency = 1.5 cycles per degree', ‘B’ means ‘spatial frequency = 3 cycles per degree’, ‘C’ means ‘spatial frequency = 6 cycles per degree’, ‘D’ means ‘spatial frequency = 12 cycles per degree’, and ‘E’ means ‘spatial frequency = 18 cycles per degree’. * p<0.001 compared with baseline. |
Table 1.
Baseline characteristics of patients who underwent cataract surgery with IOL implantation
| Group A* (n = 38) | Group B† (n = 46) | p-value | |
|---|---|---|---|
| Sex (male:female) | 17:21 | 19:27 | 0.671 |
| Age (years) | 62.8 ± 12.9 | 62.3 ± 14.7 | 0.477 |
| UDVA (log MAR) | 0.70 ± 0.33 | 0.69 ± 0.32 | 0.805 |
| CDVA (log MAR) | 0.41 ± 0.31 | 0.46 ± 0.36 | 0.871 |
| Manifest refraction (SE, D) | 0.02 ± 5.54 | −1.18 ± 3.66 | 0.173 |
| Endothelial cell count (cells/mm2) | 2,584.9 ± 387.4 | 2,623.4 ± 392.3 | 0.752 |
| Functional acuity contrast test | |||
| Row A | 13.1 ± 5.2 | 12.8 ± 5.3 | 0.760 |
| Row B | 17.7 ± 4.2 | 16.9 ± 4.1 | 0.509 |
| Row C | 20.7 ± 5.8 | 19.9 ± 6.0 | 0.497 |
| Row D | 12.5 ± 3.5 | 12.1 ± 3.6 | 0.564 |
| Row E | 5.2 ± 1.3 | 5.1 ± 1.2 | 0.782 |
| Follow-up duration (months) | 12.5 ± 0.8 | 12.7 ± 0.9 | 0.691 |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download