Abstract
Purpose
To report a case of Paecilomyces lilacinus fungal keratitis after cataract surgery in a patient with chronic systemic and autoimmune disease who was treated with medical therapy and penetrating keratoplasty.
Case summary
A 72-year-old female was referred for decreased visual acuity and ocular pain in the left eye. She underwent cataract surgery in the left eye 1 month earlier and was treated for 2 weeks for corneal edema and stromal infiltration around the corneal suture. She had a chronic systemic disease with hypertension, hyperlipidemia, hepatitis C and rheumatoid arthritis. Suspecting infectious keratitis, the patient was instructed to stop applying topical and systemic steroids and use topical amphotericin B (0.15%) and moxifloxacin (0.5%). However, without improvement, amphotericin B (0.15%) and moxifloxacin (0.5%) were changed to natamycin (5%) and topical voriconazole (2%) and systemic voriconazole was added. However, her systemic status deteriorated and corneal melting developed, scleral graft implantation and amniotic membrane implantation were performed to prevent corneal perforation 6 weeks after the initial visit. Paecilomyces lilacinus was identified in culture at 7 weeks and penetrating keratoplasty was performed 12 weeks after the initial visit. After penetrating keratoplasty, corneal status was stable for 6 months and no signs of recurrence were observed.
References
3. Malecha MA, Tarigopula S, Malecha MJ. Successful treatment of Paecilomyces lilacinus keratitis in a patient with a history of herpes simplex virus keratitis. Cornea. 2006; 25:1240–2.

4. Jacobs H, Gray SN, Crump DH. Interactions between nem-atophagous fungi and consequences for their potential as abdominal agents for the control of potato cystnematodes. Mycol Res. 2003; 107(Pt 1):47–56.
5. Okhravi N, Dart JK, Towler HM, Lightman S. Paecilomyces abdominal endophthalmitis with secondary keratitis: a case report and abdominal review. Arch Ophthalmol. 1997; 115:1320–4.
6. Chander J, Sharama A. Prevalence of fungal corneal ulcers in northern India. Infection. 1994; 22:207–9.

7. Tanure MA, Cohen EJ, Sudesh S, et al. Spectrum of fungal keratitis at Wills Eye Hospital, Philadelphia, Pennsylvania. Cornea. 2000; 19:307–12.

8. Hahn YH, Lee DJ, Kim MS, et al. Epidemiology of fungal keratitis in Korea: a Multi-center Study. J Korean Ophthalmol Soc. 2000; 41:1449–508.
9. Roumpos C. Ecological studies on Paecilomyces lilacinus strain 251 and their importance for biocontrol of plant-parasitic nemat-odes and environmental risk assessment. 1st ed.Göttingen: Cuvillier Verlag;2005. p. 16–39.
10. Hirst LW, Sebban A, Whitby RM, et al. Non-traumatic mycotic keratitis. Eye (Lond). 1992; 6(Pt 4):391–5.

11. Pastor FJ, Guarro J. Clinical manifestations, treatment and abdominals of Paecilomyces lilacinus infections. Clin Microbiol Infect. 2006; 12:948–60.
12. Yuan X, Wilhelmus KR, Matoba AY, et al. Pathogenesis and abdominal of Paecilomyces keratitis. Am J Ophthalmol. 2009; 147:691–6.
13. Wu PC, Lai CH, Tan HY, et al. The successful medical treatment of a case of Paecilomyces lilacinus keratitis. Cornea. 2010; 29:357–8.

14. Monden Y, Sugita M, Yamakawa R, Nishimura K. Clinical abdominal treating Paecilomycs lilacinus keratitis in four patients. Clin Ophthalmol. 2012; 6:949–53.
15. McLintock CA, Lee GA, Atkinson G. Management of recurrent Paecilomyces lilacinus keratitis. Clin Exp Optom. 2013; 96:343–5.

16. Won JY, Shin JY, Hwang JH, Joo CK. A case of fungal keratitis caused by Paecilomyces lilacinus after penerating keratoplasty. J Korean Ophthalmol Soc. 2014; 55:1384–7.
17. Bunya VY, Hammersmith KM, Rapuano CJ, et al. Topical and oral voriconazole in the treatment of fungal keratitis. Am J Ophthalmol. 2007; 143:151–3.

18. Byun DS, Yang HN, Cho HG, Cha YJ. A case of corneal ulcer caused by Paecilomyces in diabetic patient wearing soft contact lens. J Korean Ophthalmol Soc. 1987; 28:667–71.
Figure 1.
Slit lamp photography. (A) At the initial visit, the epithelial defect with round shape and feathery stromal infiltration was shown on left eye. (B) 4 days after treatment, there were fibrous membranes in the anterior chamber and more increased stromal infiltration than initial visit on left eye.
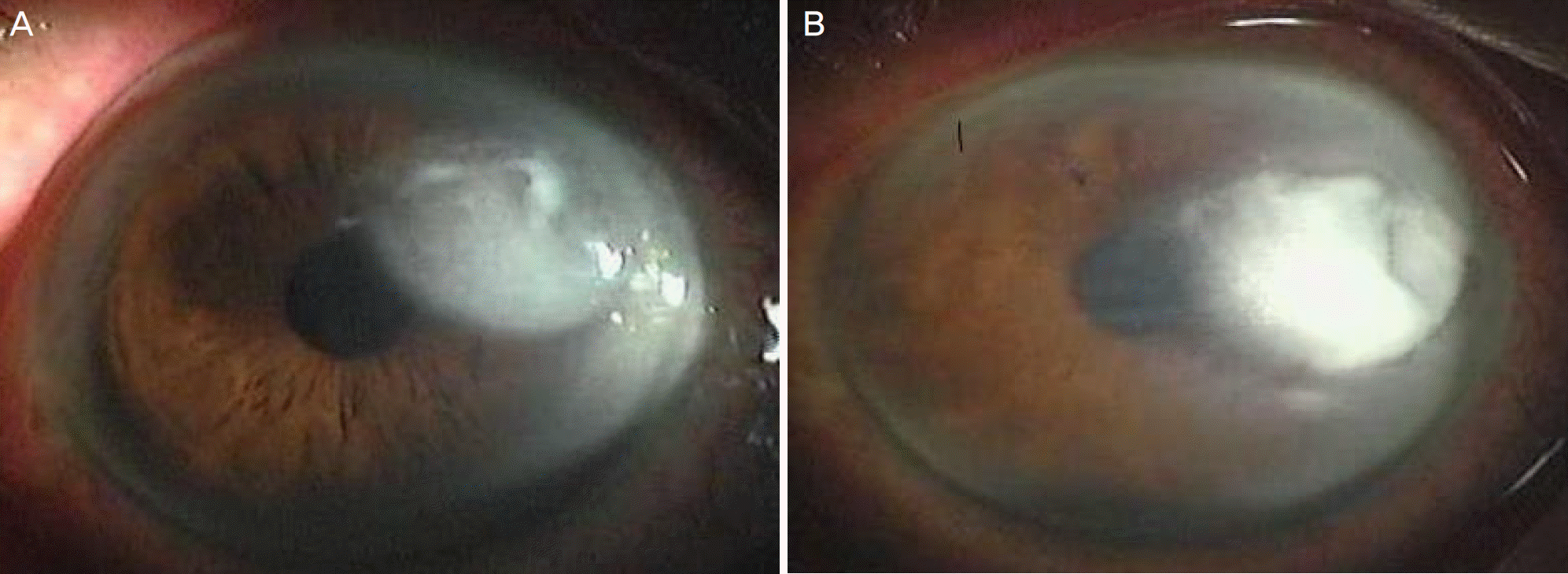
Figure 2.
Slit lamp photography. (A) 25 days after initial visit, corneal suture and conjunctival flap transposition were done on left eye. (B) After 10 days of admission, iris incarcerated at temporal melted corneal lesion and stromal infiltration was also increased.
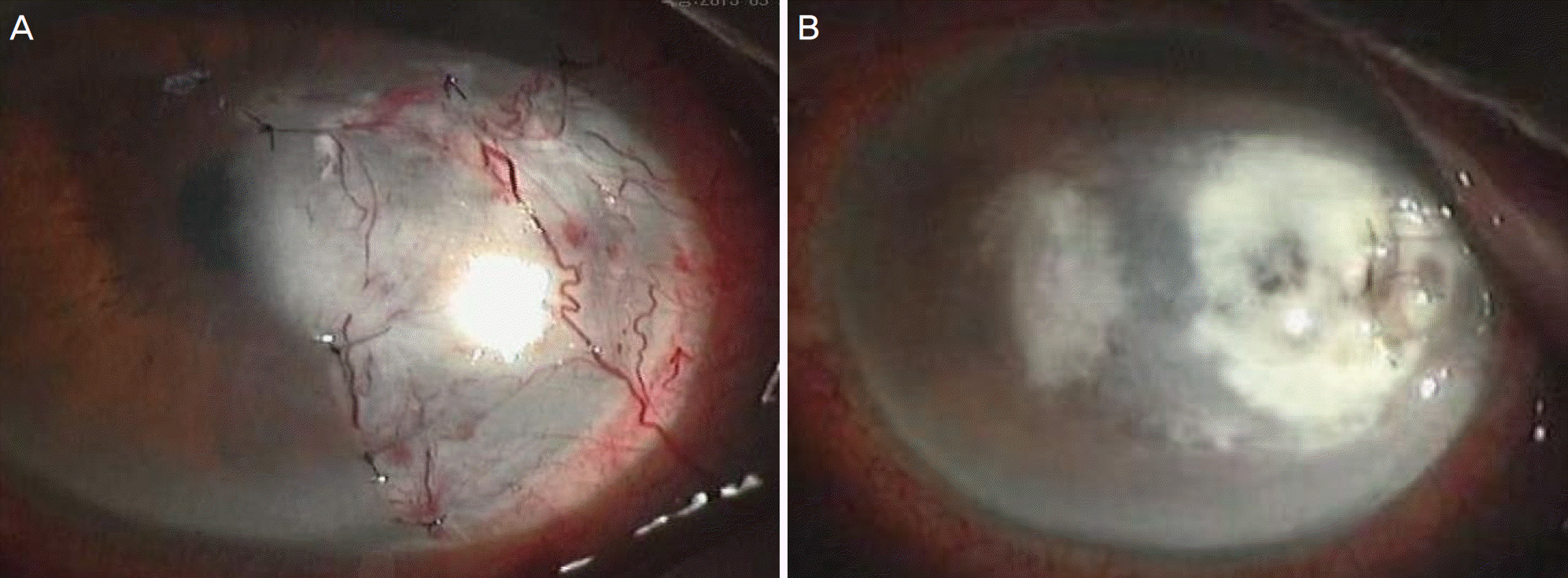
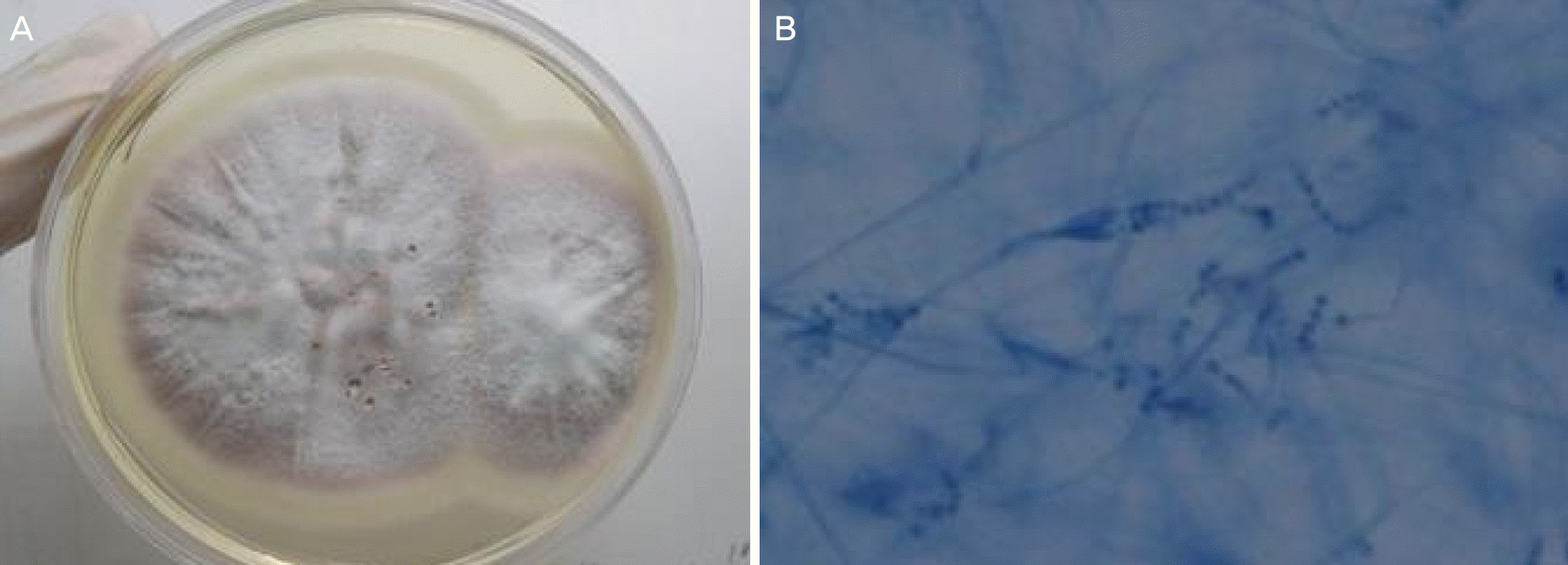
Figure 3.
Phtography of culture and photomicrograph. (A) Colony of Paecilomyces lilacinus (P. lilacinus) were isolated from infected cornea after incubating 2 weeks with pink-gray color on sabouraud dextrose agar. (B) Photomicrograph of P. lilacinus was demonstrated the long branching conidiophores arising from hyphae, tapering phialides, and chains of conidia (lactophenol cotton blue stain, ×400).




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download