Abstract
Purpose
To describe a case of Wyburn-Mason Syndrome, which is a rare phakomatosis, and its associated optical coherence tomography findings.
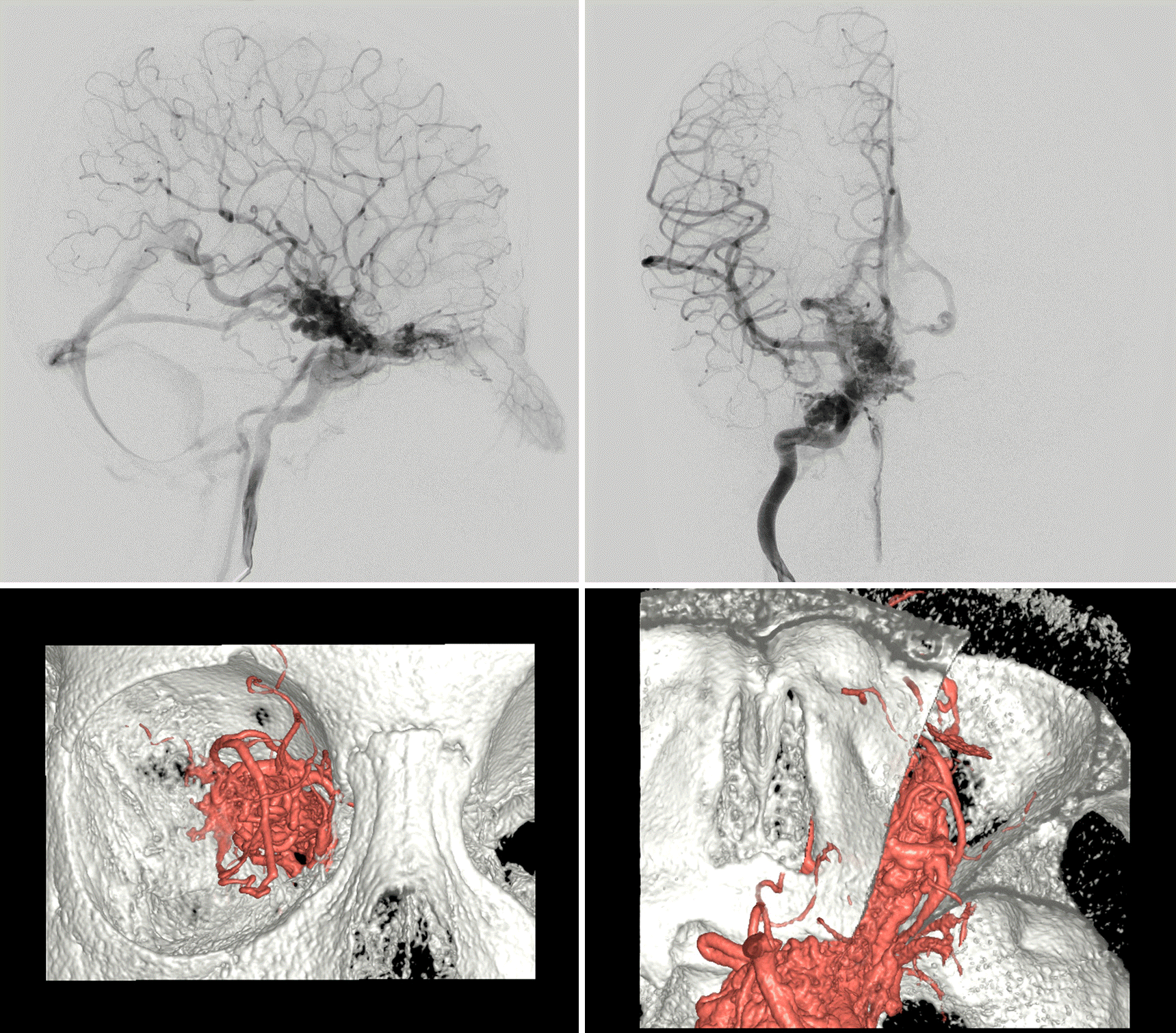
Case summary: A 5-year-old boy was referred to our clinic for decreased vision in his right eye. He had nevus flammeus on his right forehead, upper eyelid, and cheek. His best corrected visual acuity was hand motion in the right eye, in which a relative afferent pupillary defect was noted. Fundus examination of the right eye showed marked dilation and tortuosity of retinal vessels, which could not be discriminated between arteries and veins on the posterior pole. Optical coherence tomography showed multiple large intraretinal vessels without involvement of the internal limiting membrane. Cerebral angiography revealed arteriovenous malformations (AVMs) and feeder vessels from the internal carotid artery to the ophthalmic artery, extending to the ethmoidal artery in the nasal cavity.
Conclusions
Wyburn-Mason syndrome is a rare phakomatoses and shows unique retinal AVM. Misdiagnosis or undertreatment of Wyburn-Mason syndrome can lead to serious complications. Patients with facial nevus flammeus should undergo thorough ocular examinations to rule out this disorder. Optical coherence tomography is a useful method for understanding structural features of retinal vascular malformations in Wyburn-Mason syndrome.
Go to : 
References
1. Wyburn-Mason R. Arteriovenous aneurysm of midbrain and abdominal, facial naevi and mental changes. Brain. 1943; 66:163–203.
2. Chowaniec MJ, Suh DW, Boldt HC, et al. Anomalous optical abdominal tomography findings in Wyburn-Mason syndrome and isolated retinal arteriovenous malformation. J AAPOS. 2015; 19:175–7.
3. Bae HD, Kim BH, Shin DM. A case of congenital arteriovenous communications of the retina. J Korean Ophthalmol Soc. 1981; 22:647–51.
4. Joo JD, Lee JH. A case of bilateral congenital arteriovenous communication. J Korean Ophthalmol Soc. 1996; 37:1218–23.
5. Jang HS, Lee TK, Kim JW. A case of retinal racemose hemangioma. J Korean Ophthalmol Soc. 2001; 42:1232–5.
7. Schmidt D, Pache M, Schumacher M. The congenital unilateral abdominal vascular malformation syndrome (bonnet-dechaumeblanc syndrome or wyburn-mason syndrome): review of the literature. Surv Ophthalmol. 2008; 53:227–49.
8. Iwata A, Mitamura Y, Niki M, et al. Binarization of enhanced depth imaging optical coherence tomographic images of an eye with Wyburn-Mason syndrome: a case report. BMC Ophthalmol. 2015; 15:19.

9. Ponce FA, Han PP, Spetzler RF, et al. Associated arteriovenous malformation of the orbit and brain: a case of Wyburn-Mason abdominal without retinal involvement. Case report. J Neurosurg. 2001; 95:346–9.
10. Magnus H. Aneurysma arterioso-venosum retinale. Virchows Arch Pathol Anat Physiol Klin Med. 1874; 60:38–45.

11. Bonnet P, Dechaume J, Blanc M. L'aneurisme cirsoide de la retine (aneurysme racemeux). J Med Lyon. 1937; 18:165–78.
12. Bech K, Jensen OA. On the frequency of abdominal racemose hae-mangiomata of the retina and brain. Acta Psychiatr Scand. 1961; 36:47–56.
13. Théron J, Newton TH, Hoyt WF. Unilateral retinocephalic vascular malformations. Neuroradiology. 1974; 7:185–96.

14. Dayani PN, Sadun AA. A case report of Wyburn-Mason syndrome and review of the literature. Neuroradiology. 2007; 49:445–56.

15. Wilkins RH. Natural history of intracranial vascular malformations: a review. Neurosurgery. 1985; 16:421–30.

16. Ondra SL, Troupp H, George ED, Schwab K. The natural history of symptomatic arteriovenous malformations of the brain: a 24-year follow-up assessment. J Neurosurg. 1990; 73:387–91.

17. Brown RD Jr, Wiebers DO, Forbes G, et al. The natural history of unruptured intracranial arteriovenous malformations. J Neurosurg. 1988; 68:352–7.

18. Grigg JRB, Jamieson RV. Phakomatoses. Hoyt CS, Taylor D, editors. Pediatric Ophthalmology and Strabismus. 4th ed.New York: Elsevier;2013. chap. 65.

19. Telander DG, Choi SS, Zawadzki RJ, et al. Microstructural abdominal revealed by high resolution imaging systems in central macular arteriovenous malformation. Ophthalmic Surg Lasers Imaging. 2010; 9:1–4.
20. Onder HI, Alisan S, Tunc M. Serous retinal detachment and abdominal macular edema in a patient with Wyburn-Mason syndrome. Semin Ophthalmol. 2015; 30:154–6.
21. Rizzo R, Pavone L, Pero G, et al. A neurocutaneous disorder with a severe course: Wyburn-Mason's syndrome. J Child Neurol. 2004; 19:908–11.
Go to : 
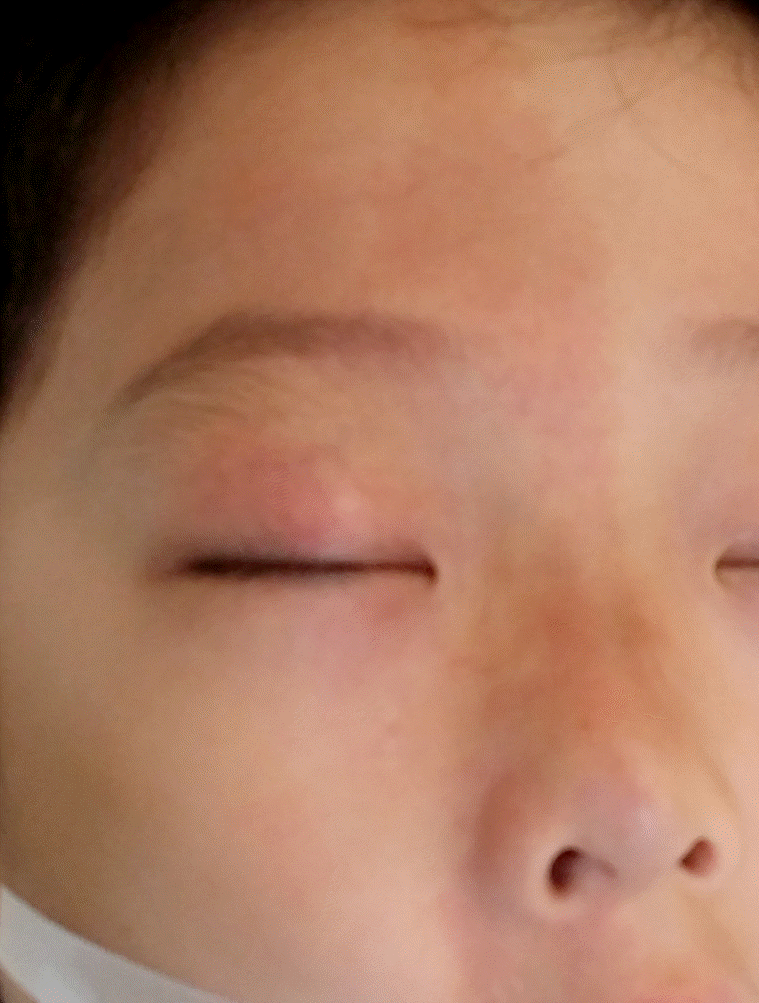 | Figure 1.Facial photo of the patient. Nevus flammeus was seen on the right forehead, nose, upper lid and cheek. |
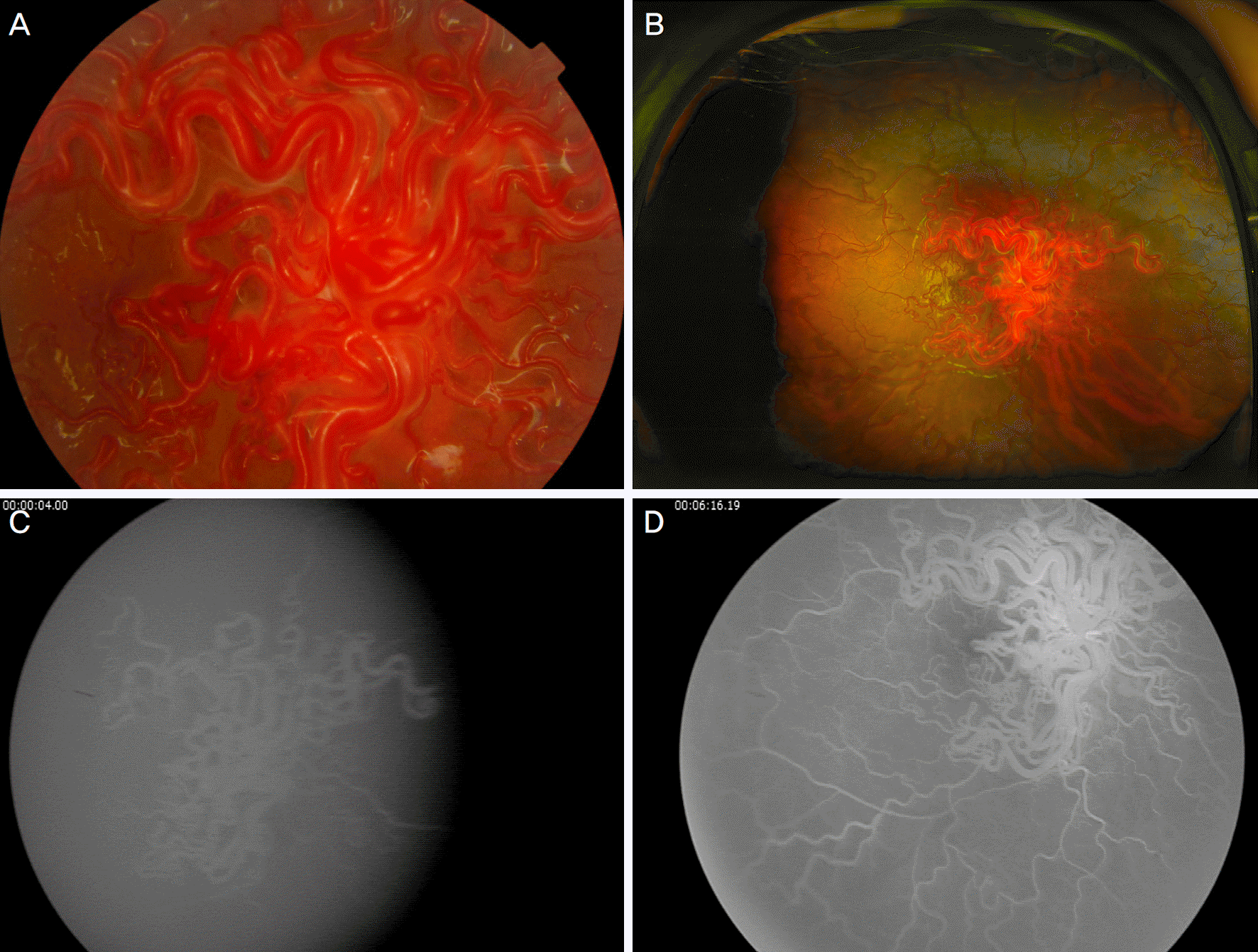 | Figure 2.Fundus findings of the patient. (A) The fundus photograph of the affected eye showed characteristic retinal vascular features of enlarged and tortuous vessels with “Bag of Worms” appearance. (B) The wide field fundus photograph of the affected eye showed vascular abnormality mostly confined to the posterior pole. (C) Fluorescein angiography of the affected eye. Very rapid arterial and venous filling was noted only at 4 seconds after injection. (D) No fluorescein leakage was noted even in the late phase. |
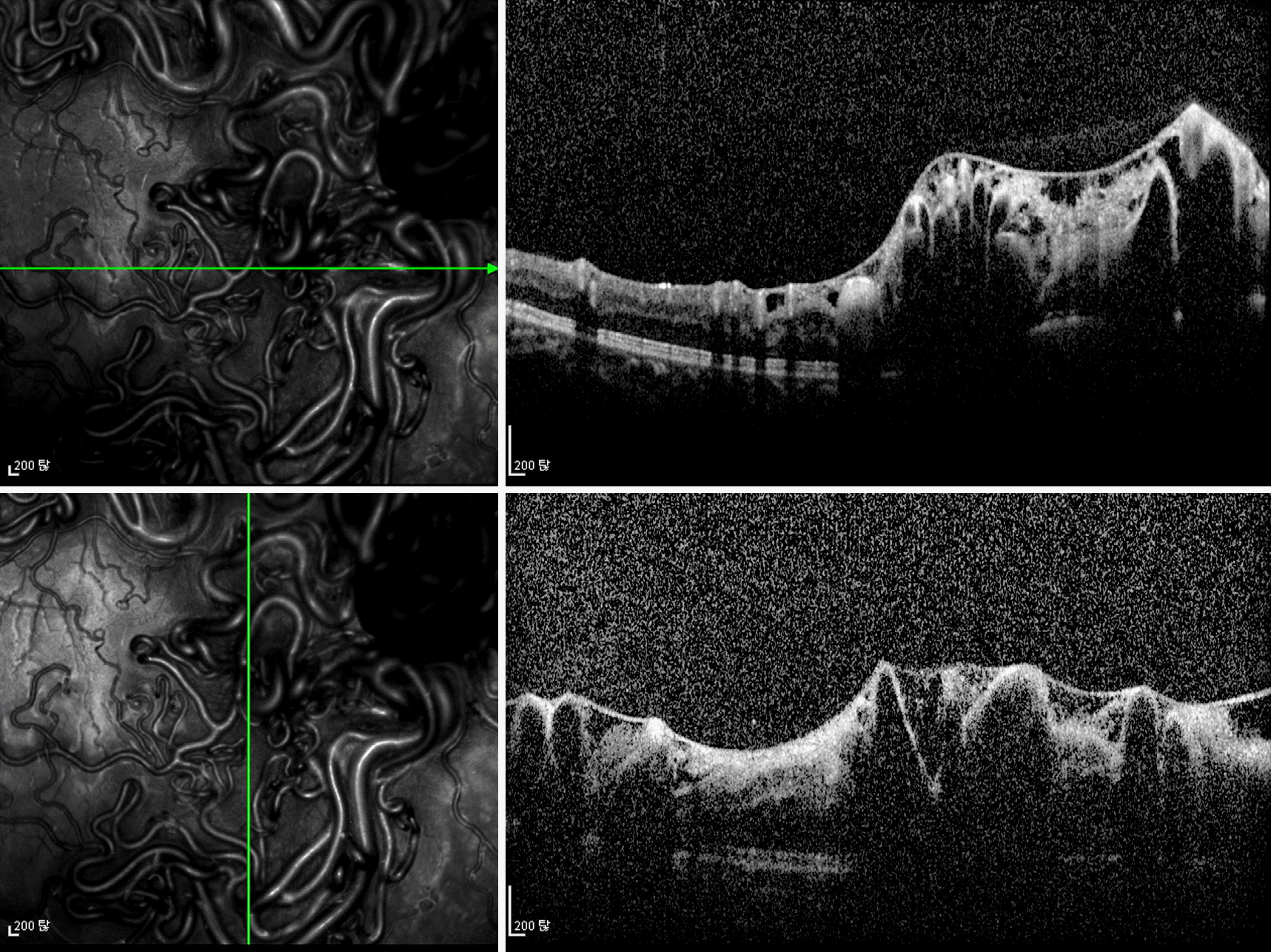 | Figure 3.Spectral domain optical coherence tomography of the affected eye. Multiple vascular enlargements within the retina caused prominent shadowing artifacts. Abnormal vascular structures were confined to the intraretinal structure without involvement of the highly reflective membrane structure regarded as the internal limiting membrane. |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download