Abstract
Purpose
To report a case of delayed orbital cellulitis with subperiosteal abscess after orbital floor fracture repair using an absorbable sheet implant (Macropore®, Medtronic Inc., Minneapolis, MN, USA).
Case summary: A 16-year-old male visited the oculoplastic clinic for left eye pain, lower eyelid swelling and vertical diplopia for 1 day. The patient had a history of inferior orbital wall fracture repair surgery using Macropore® 20 months prior. The orbital computed tomography scan showed a subperiosteal cystic mass with surrounding infiltration at the left orbital floor, and ethmoidal and maxillary sinusitis; however, sheet implant was not clearly observed. Despite systemic antibiotic treatment for 3 days, his clinical findings did not improve, thus we decided to drain the subperiosteal abscess through a transconjunctival approach. Intraoperatively, the Macropore® sheet was almost dissolved, but small pieces remained. The culture of drained contents showed no microorganisms. Systemic antibiotics were continued for 18 days after surgery, and clinical symptoms completely improved.
Conclusions
Delayed orbital cellulitis should be considered in patients with extraocular muscle movement limitation and painful orbital swelling if the patient has a history of orbital wall fracture repair, even if a bioresorbable implant was used. Prompt imaging evaluation should be emphasized for early diagnosis and proper treatment.
Go to : 
References
1. Enislidis G. Treatment of orbital fractures: the case for treatment with resorbable materials. J Oral Maxillofac Surg. 2004; 62:869–72.

2. Kontio R. Treatment of orbital fractures: the case for abdominal with autogenous bone. J Oral Maxillofac Surg. 2004; 62:863–8.
3. Potter JK, Ellis E. Biomaterials for reconstruction of the internal orbit. J Oral Maxillofac Surg. 2004; 62:1280–97.

4. Rubin PA, Bilyk JR, Shore JW. Orbital reconstruction using porous polyethylene sheets. Ophthalmology. 1994; 101:1697–708.

5. Han DH, Chi M. Comparison of the outcomes of blowout fracture repair according to the orbital implant. J Craniofac Surg. 2011; 22:1422–5.

6. Kent SS, Kent JS, Allen LH. Porous polyethylene implant abdominal with orbital cellulitis and intraorbital abscess. Can J Ophthalmol. 2012; 47:e38–9.
7. Ben Simon GJ, Bush S, Selva D, McNab AA. Orbital cellulitis: a rare complication after orbital blowout fracture. Ophthalmology. 2005; 112:2030–4.

8. Warrier S, Prabhakaran VC, Davis G, Selva D. Delayed complications of silicone implants used in orbital fracture repairs. Orbit. 2008; 27:147–51.

9. Jeong SM, Yim JS, Park DH, Kwak JY. A case of acute orbital abdominal following repair of orbital wall fracture with alloplastic implant. J Korean Ophthalmol Soc. 2007; 48:1706–10.
10. Mauriello JA Jr, Hargrave S, Yee S, et al. Infection after insertion of alloplastic orbital floor implants. Am J Ophthalmol. 1994; 117:246–52.

11. Ng SG, Madill SA, Inkster CF, et al. Medpor porous polyethylene implants in orbital blowout fracture repair. Eye (London). 2001; 15(Pt 5):578–82.

12. Romano JJ, Iliff NT, Manson PN. Use of Medpor porous abdominal implants in 140 patients with facial fractures. J Craniofac Surg. 1993; 4:142–7.
13. Lin J, German M, Wong B. Use of copolymer polylactic and abdominal acid resorbable plates in repair of orbital floor fractures. Facial Plast Surg. 2014; 30:581–6.
Go to : 
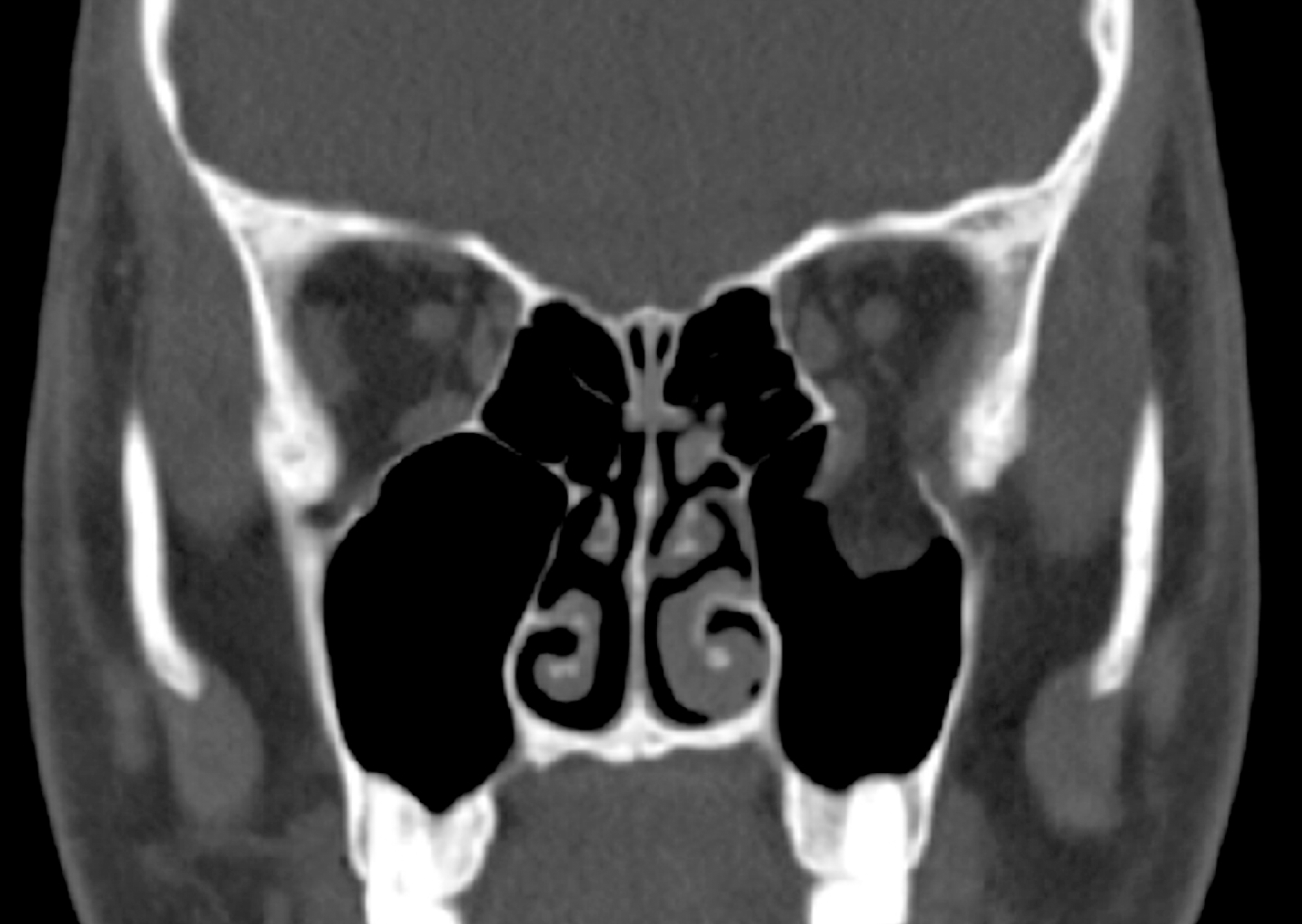 | Figure 1.Noncontrast computed tomography scan of the orbits (coronal view) before the surgical repair of the left orbital wall fracture. Discontinuity of the left orbital floor with downward herniation of orbital fat and inferior rectus muscle into the maxillary sinus was noted. There was no definite sinusitis. |
 | Figure 2.Photograph and orbital computed tomography of the patient. (A) An 16-year-old boy presented with erythematous swelling at the left lower eyelid. He also complained with ocular pain of the left eye and vertical diplopia. (B) Orbital computed tomography (coronal view) reveals fluid collection at the inferior subperiosteal space (arrows) and adjacent soft tissue enhancement (asterix), suggesting orbital cellulitis and inferior subperiosteal abscess. Note marked opacification in the both ethmoidal and maxillary sinuses. |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download