초록
Purpose:
To compare the accuracy and agreement of intraocular pressure (IOP) and central corneal thickness (CCT) measurements with noncontact tonometer Corvis Scheimpflug Technology (Corvis ST) versus noncontact tonometer (NCT), Goldmann applanation tonometer (GAT), rebound tonometer (RBT), and ultrasound-based corneal pachymetry (US-CCT). The secondary objective was to evaluate the corneal biomechanical values using Corvis ST tonometer in patients with glaucoma.
Methods:
Thirty-one healthy participants and 47 patients with primary open angle glaucoma and normal tension glaucoma were enrolled in this study. One eye was selected randomly. In each participant, GAT, NCT, RBT, US-CCT and measurements with Corvis ST (Corvis-IOP and Corvis-CCT) were obtained. IOP and CCT measurements of each device were compared. Device agreement was calculated by Bland-Altman analysis. Additionally, corneal highest concavity parameters were compared between healthy subjects and glaucoma patients.
Results:
Mean IOPs in all examined eyes were 13.28 ± 2.32 mm Hg for CST, 14.71 ± 2.95 mm Hg for GAT, 14.44 ± 3.10 mm Hg for NCT, and 13.23 ± 2.89 mm Hg for RBT. There was no statistical difference in IOP measurements among tonometers. Correlation analysis showed a high correlation between each pair of tonometers (all p < 0.0001). Bland-Altman plots of all devices revealed good agreement of the IOP and CCT measurements. In glaucoma patients, highest concavity time and peak distance of highest concavity parameters were statistically lower than in normal subjects (16.93 ± 0.66 ms vs. 16.48 ± 0.84 ms p = 0.020, 4.23 ± 1.34 mm vs. 3.41 ± 1.27 mm p = 0.017, respectively).
Conclusions:
The CST, a newly-developed tonometer with features of visualization and measurement of the corneal deformation response to an air impulse, can be considered a reliable alternative method for measuring IOP and CCT in healthy subjects and glaucoma patients. Highest concavity parameters could be another important indicator identifying corneal viscosity or elasticity in patients with glaucoma.
References
1. Comparison of glaucomatous progression between untreated patients with normal-tension glaucoma and patients with therapeuti-cally reduced intraocular pressures. Collaborative Normal-Tension Glaucoma Study Group. Am J Ophthalmol. 1998; 126:487–97.
2. Leske MC, Heijl A, Hyman L, et al. Predictors of long-term progression in the early manifest glaucoma trial. Ophthalmology. 2007; 114:1965–72.

3. Chihara E. Assessment of true intraocular pressure: the gap between theory and practical data. Surv Ophthalmol. 2008; 53:203–18.

4. Doughty MJ, Zaman ML. Human corneal thickness and its impact on intraocular pressure measures: a review and meta-analysis approach. Surv Ophthalmol. 2000; 44:367–408.
5. Liu J, Roberts CJ. Influence of corneal biomechanical properties on intraocular pressure measurement: quantitative analysis. J Cataract Refract Surg. 2005; 31:146–55.
6. Cook JA, Botello AP, Elders A, et al. Systematic review of the agreement of tonometers with Goldmann applanation tonometry. Ophthalmology. 2012; 119:1552–7.

7. Kotecha A, White ET, Shewry JM, Garway-Heath DF. The relative effects of corneal thickness and age on Goldmann applanation tonometry and dynamic contour tonometry. Br J Ophthalmol. 2005; 89:1572–5.

8. Broman AT, Congdon NG, Bandeen-Roche K, Quigley HA. Influence of corneal structure, corneal responsiveness, and other ocular parameters on tonometric measurement of intraocular pressure. J Glaucoma. 2007; 16:581–8.

9. Kwon TH, Ghaboussi J, Pecknold DA, Hashash Y. Role of corneal biomechanical properties in applanation tonometry measurements. J Refract Surg. 2010; 26:512–9.

10. Sullivan-Mee M, Billingsley SC, Patel AD, et al. Ocular Response Analyzer in subjects with and without glaucoma. Optom Vis Sci. 2008; 85:463–70.

11. Huseynova T, Waring GO 4th, Roberts C, et al. Corneal biomechanics as a function of intraocular pressure and pachymetry by dynamic infrared signal and Scheimpflug imaging analysis in normal eyes. Am J Ophthalmol. 2014; 157:885–93.

12. Luce DA. Determining in vivo biomechanical properties of the cornea with an ocular response analyzer. J Cataract Refract Surg. 2005; 31:156–62.

13. Hong J, Xu J, Wei A, et al. A new tonometer--the Corvis ST tonometer: clinical comparison with noncontact and Goldmann applanation tonometers. Invest Ophthalmol Vis Sci. 2013; 54:659–65.

14. Chang DH, Stulting RD. Change in intraocular pressure measurements after LASIK the effect of the refractive correction and the la-mellar flap. Ophthalmology. 2005; 112:1009–16.
15. Kotecha A. What biomechanical properties of the cornea are rele-vant for the clinician? Surv Ophthalmol. 2007; 52(Suppl 2):S109–14.

16. Morita T, Shoji N, Kamiya K, et al. Corneal biomechanical properties in normal-tension glaucoma. Acta Ophthalmol. 2012; 90:e48–53.

17. Terai N, Raiskup F, Haustein M, et al. Identification of biomechanical properties of the cornea: the ocular response analyzer. Curr Eye Res. 2012; 37:553–62.

18. Yu AY, Duan SF, Zhao YE, et al. Correlation between corneal biomechanical properties, applanation tonometry and direct intra-cameral tonometry. Br J Ophthalmol. 2012; 96:640–4.

19. Smedowski A, Weglarz B, Tarnawska D, et al. Comparison of three intraocular pressure measurement methods including biomechanical properties of the cornea. Invest Ophthalmol Vis Sci. 2014; 55:666–73.

20. Poostchi A, Mitchell R, Nicholas S, et al. The iCare rebound tonometer: comparisons with Goldmann tonometry, and influence of central corneal thickness. Clin Experiment Ophthalmol. 2009; 37:687–91.

21. Martinez-de-la-Casa JM, Garcia-Feijoo J, Castillo A, Garcia-Sanchez J. Reproducibility and clinical evaluation of rebound tonometry. Invest Ophthalmol Vis Sci. 2005; 46:4578–80.

Figure 1.
Intraocular pressure measurement by CST. A high speed Scheimpflug camera was equipped to record the movement of cornea. The output also includes central corneal thickness and corneal biomechanical properties (applanation time, applanation length, applanation velocity, and parameters of highest concavity). CST = Corvis scheimpflug technology; IOP = intraocular pressure.

Figure 2.
Analysis of variance between mean intraocular pressure values measured by different tonometers. There was no statistically significant difference in IOP measurement among the tonometers by ANOVA (CST vs GAT, p = 0.265 CST vs NCT, p = 0.057 CST vs RBT, p = 0.744). IOP = intraocular pressure; CST = Corvis scheimpflug technology; GAT = Goldmann applanation tonometer; NCT = noncontact tonometer; RBT = rebound tonometer.

Figure 3.
Bland-Altman plots between different tonometers. The solid line indicates mean difference of both tonometers. The dotted lines are 95% of limits of agreement. CST = Corvis scheimpflug technology; GAT = Goldmann applanation tonometer; NCT = noncontact tonometer; RBT = rebound tonometer.

Figure 4.
Correlation of CST, GAT, NCT and RBT. Significant positive correlations were noted between CST and GAT (R = 0.670, p < 0.001), between CST and NCT (R = 0.746, p < 0.001) and between CST and RBT (R = 0.679, p < 0.001) by Spearman correlation. CST = Corvis scheimpflug technology; GAT = Goldmann applanation tonometer; NCT = noncontact tonometer; RBT = rebound tonometer.
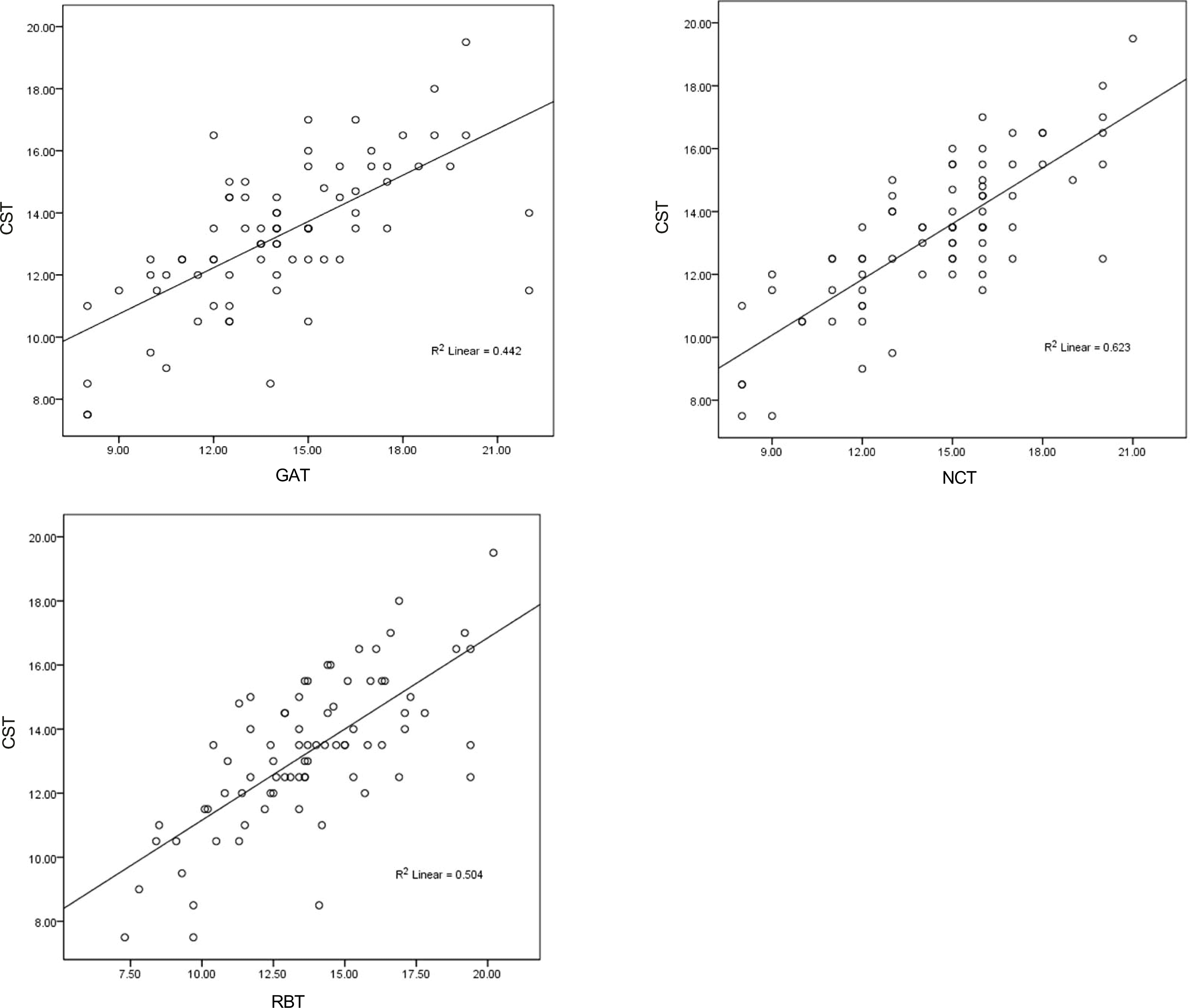
Figure 5.
Bland-Altman plots between US-CCT and Corvis-CCT. The solid line indicates mean difference of both tonometers. The dotted lines are 95% of limits of agreement. US = ultrasound; CCT = central corneal thickness.
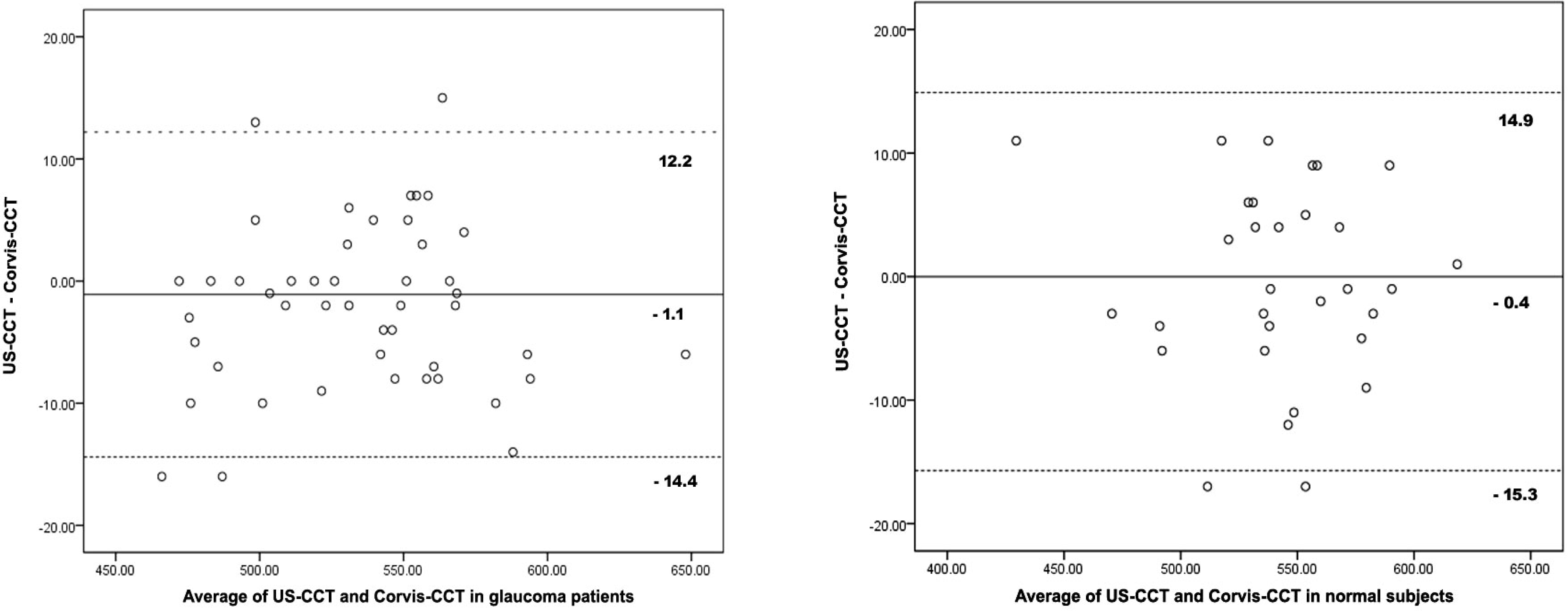
Table 1.
Demographic characteristics of study subjects
| Demographics | Values |
|---|---|
| Total (n) | 78 patients |
| (37 females and 41 males) | |
| Healthy subjects | 31 |
| Glaucoma patients | 47 (POAG:20, NTG:27) |
| Age (years) | |
| Healthy subjects | 51.6 ± 17.1 |
| Glaucoma patients | 59.0 ± 5.0 |
| p-value* | 0.057 |
| Axial length (mm) | |
| Healthy subjects | 24.36 ± 1.71 |
| Glaucoma patients | 24.75 ± 1.49 |
| p-value* | 0.312 |
| Central corneal thickness (μ m) | |
| Healthy subjects | 544.6 ± 34.9 |
| Glaucoma patients | 533.5 ± 39.1 |
| p-value* | 0.216 |
| Corneal curvature (mm) | |
| Healthy subjects | 7.68 ± 0.66 |
| Glaucoma patients | 7.82 ± 0.61 |
| p-value* | 0.387 |
| Corneal astigmatism (diopter) | |
| Healthy subjects | 1.13 ± 0.70 |
| Glaucoma patients | 0.96 ± 0.58 |
| p-value* | 0.245 |
Table 2.
Mean intraocular pressure values measured by different tonometers in normal subjects and glaucoma patients
| Tonometers | Values |
|---|---|
| Corvis ST tonometer (mm Hg) | |
| Healthy subjects | 13.37 ± 2.53 |
| Glaucoma patients | 12.77 ± 2.37 |
| Total | 13.28 ± 2.32 |
| p-value* | 0.298 |
| Goldmann applanation tonometer (mm Hg) | |
| Healthy subjects | 14.60 ± 2.98 |
| Glaucoma patients | 14.86 ± 2.94 |
| Total | 14.71 ± 2.95 |
| p-value* | 0.700 |
| Noncontact tonometer (mm Hg) | |
| Healthy subjects | 14.48 ± 3.50 |
| Glaucoma patients | 14.20 ± 2.88 |
| Total | 14.44 ± 3.10 |
| p-value* | 0.710 |
| Rebound tonometer (mm Hg) | |
| Healthy subjects | 13.01 ± 3.20 |
| Glaucoma patients | 13.56 ± 2.34 |
| Total | 13.23 ± 2.89 |
| p-value* | 0.420 |
Table 3.
Correlation between different tonometers
| CST | GAT | NCT | RBT | ||
|---|---|---|---|---|---|
| Spearman correlation | CST | 1 | 0.670* | 0.746* | 0.679* |
| GAT | 0.670 | 1 | 0.656 | 0.645 | |
| NCT | 0.746 | 0.656 | 1 | 0.684 | |
| RBT | 0.679 | 0.645 | 0.684 | 1 |
Table 4.
Mean CCT obtained with ultrasound pachymetry and Corvis ST tonometry of normal subjects and glaucoma patients
| Mean US-CCT | Mean Corvis-CCT | Correlation (Pearson’s coefficient) | |
|---|---|---|---|
| Glaucoma patients | 532.40 ± 38.18 | 534.87 ± 40.31 | 0.965 |
| p < 0.0001 | |||
| Normal subjects | 542.74 ± 35.93 | 547.29 ± 38.06 | 0.933 |
| p < 0.0001 |
Table 5.
Mean value parameters of highest concavity from Corvis ST for each subgroup of corneal compensated intraocular pressure groups
|
Highest concavity |
||||
|---|---|---|---|---|
| Time | Peak distance | Radius | Deformation amplitude | |
| Glaucoma patients | 16.48 ± 0.84 | 3.41 ± 1.27 | 6.85 ± 0.78 | 1.11 ± 0.16 |
| Normal subjects | 16.93 ± 0.66 | 4.23 ± 1.34 | 7.19 ± 0.78 | 1.18 ± 0.13 |
| p-value* | 0.020* | 0.017* | 0.088 | 0.051 |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download