Abstract
Purpose
To compare parameters of femtosecond laser and manual continuous curvilinear capsulorhexis (CCC) using anterior segment optical coherence tomography (AS-OCT).
Methods
Femtosecond laser cataract surgery was performed in 30 eyes of 30 patients, and conventional cataract surgery with a manual CCC in 30 eyes of 30 patients. One month after surgery, CCC diameters, circularity of capsulotomy, and distance between the CCC and pupil center were analyzed using the AS-OCT.
Results
Mean maximal CCC diameter was 4.96 ± 0.23 mm in the femtosecond laser group, and 4.70 ± 0.82 mm in the manual CCC group. Mean minimal CCC diameter was 4.91 ± 0.23 mm in the femtosecond group, and 4.48 ± 0.64 mm in the manual CCC group showing significant difference between the two groups (p = 0.000). Circularity of capsulotomy was 0.99 ± 0.01 in the femtosecond group and 0.91 ± 0.13 in the manual CCC group and was statistically different between the 2 groups (p = 0.000). The distance from the CCC center to the pupil center was 0.18 ± 0.09 mm in the femtosecond group and 0.26 ± 0.17 mm in the manual CCC group. The CCC center was closer to the pupil center in the femtosecond than in the manual CCC group (p = 0.038).
Go to : 
References
1. Nagy Z, Takacs A, Filkorn T, Sarayba M. Initial clinical evaluation of an intraocular femtosecond laser in cataract surgery. J Refract Surg. 2009; 25:1053–60.

2. Ratkay-Traub I, Ferincz IE, Juhasz T, et al. First clinical results with the femtosecond neodynium-glass laser in refractive surgery. J Refract Surg. 2003; 19:94–103.

3. Nordan LT, Slade SG, Baker RN, et al. Femtosecond laser flap creation for laser in situ keratomileusis: six-month follow-up of initial U. S. clinical series. J Refract Surg. 2003; 19:8–14.
4. Tran DB, Sarayba MA, Bor Z, et al. Randomized prospective clinical study comparing induced aberrations with IntraLase and Hansatome flap creation in fellow eyes: potential impact on wave-front-guided laser in situ keratomileusis. J Cataract Refract Surg. 2005; 31:97–105.
5. Gimbel HV, Neuhann T. Development, advantages, and methods of the continuous circular capsulorhexis technique. J Cataract Refract Surg. 1990; 16:31–7.

6. Gimbel HV, Neuhann T. Continuous curvilinear capsulorhexis. J Cataract Refract Surg. 1991; 17:110–1.

7. Subramaniam S, Tuft SJ. Early decentration of plate-haptic silicone intraocular lenses. J Cataract Refract Surg. 2001; 27:330–2.

8. Taketani F, Matuura T, Yukawa E, Hara Y. Influence of intraocular lens tilt and decentration on wavefront aberrations. J Cataract Refract Surg. 2004; 30:2158–62.

9. Baumeister M, Bühren J, Kohnen T. Tilt and decentration of spherical and aspheric intraocular lenses: effect on higher-order aberrations. J Cataract Refract Surg. 2009; 35:1006–12.

10. Lee AC, Qazi MA, Pepose JS. Biometry and intraocular lens power calculation. Curr Opin Ophthalmol. 2008; 19:13–7.

11. Aristodemou P, Knox Cartwright NE, Sparrow JM, Johnston RL. Formula choice: Hoffer Q, Holladay 1, or SRK/T and refractive outcomes in 8108 eyes after cataract surgery with biometry by partial coherence interferometry. J Cataract Refract Surg. 2011; 37:63–71.

12. Assia EI, Apple DJ, Tsai JC, Morgan RC. Mechanism of radial tear formation and extension after anterior capsulectomy. Ophthalmology. 1991; 98:432–7.

13. Hollick EJ, Spalton DJ, Meacock WR. The effect of capsulorhexis size on posterior capsular opacification: one-year results of a randomized prospective trial. Am J Ophthalmol. 1999; 128:271–9.

14. Peng Q, Apple DJ, Visessook N, et al. Surgical prevention of posterior capsule opacification. Part 2: Enhancement of cortical cleanup by focusing on hydrodissection. J Cataract Refract Surg. 2000; 26:188–97.
15. Aasuri MK, Kompella VB, Majji AB. Risk factors for and management of dropped nucleus during phacoemulsification. J Cataract Refract Surg. 2001; 27:1428–32.

16. Kránitz K, Takacs A, Miháltz K, et al. Femtosecond laser capsulotomy and manual continuous curvilinear capsulorrhexis parameters and their effects on intraocular lens centration. J Refract Surg. 2011; 27:558–63.

17. Nagy ZZ, Kránitz K, Takacs AI, et al. Comparison of intraocular lens decentration parameters after femtosecond and manual capsulotomies. J Refract Surg. 2011; 27:564–9.

18. Eppig T, Scholz K, Löffler A, et al. Effect of decentration and tilt on the image quality of aspheric intraocular lens designs in a model eye. J Cataract Refract Surg. 2009; 35:1091–100.

19. Ravalico G, Tognetto D, Palomba M, et al. Capsulorhexis size and posterior capsule opacification. J Cataract Refract Surg. 1996; 22:98–103.

20. Aykan U, Bilge AH, Karadayi K, Akin T. The effect of capsulorhexis size on development of posterior capsule opacification: small (4.5 to 5.0 mm) versus large (6.0 to 7.0 mm). Eur J Ophthalmol. 2003; 13:541–5.

21. Hollick EJ, Spalton DJ, Meacock WR. The effect of capsulorhexis size on posterior capsular opacification: one-year results of a randomized prospective trial. Am J Ophthalmol. 1999; 128:271–9.

22. Ram J, Pand, ey SK, Apple DJ, et al. Effect of in-the-bag intraocular lens fixation on the prevention of posterior capsule opacification. J Cataract Refract Surg. 2001; 27:1039–46.
23. Hayashi K, Hayashi H, Nakao F, Hayashi F. Anterior capsule contraction and intraocular lens decentration and tilt after hydrogel lens implantation. Br J Ophthalmol. 2001; 85:1294–7.

24. Hayashi H, Hayashi K, Nakao F, Hayashi F. Anterior capsule contraction and intraocular lens dislocation in eyes with pseudoexfoliation syndrome. Br J Ophthalmol. 1998; 82:1429–32.

25. Baumeister M, Bühren J, Kohnen T. Tilt and decentration of spherical and aspheric intraocular lenses: effect on higher-order aberrations. J Cataract Refract Surg. 2009; 35:1006–12.

26. Miháltz K, Knorz MC, Alió JL, et al. Internal aberrations and optical quality after femtosecond laser anterior capsulotomy in cataract surgery. J Refract Surg. 2011; 27:711–6.

Go to : 
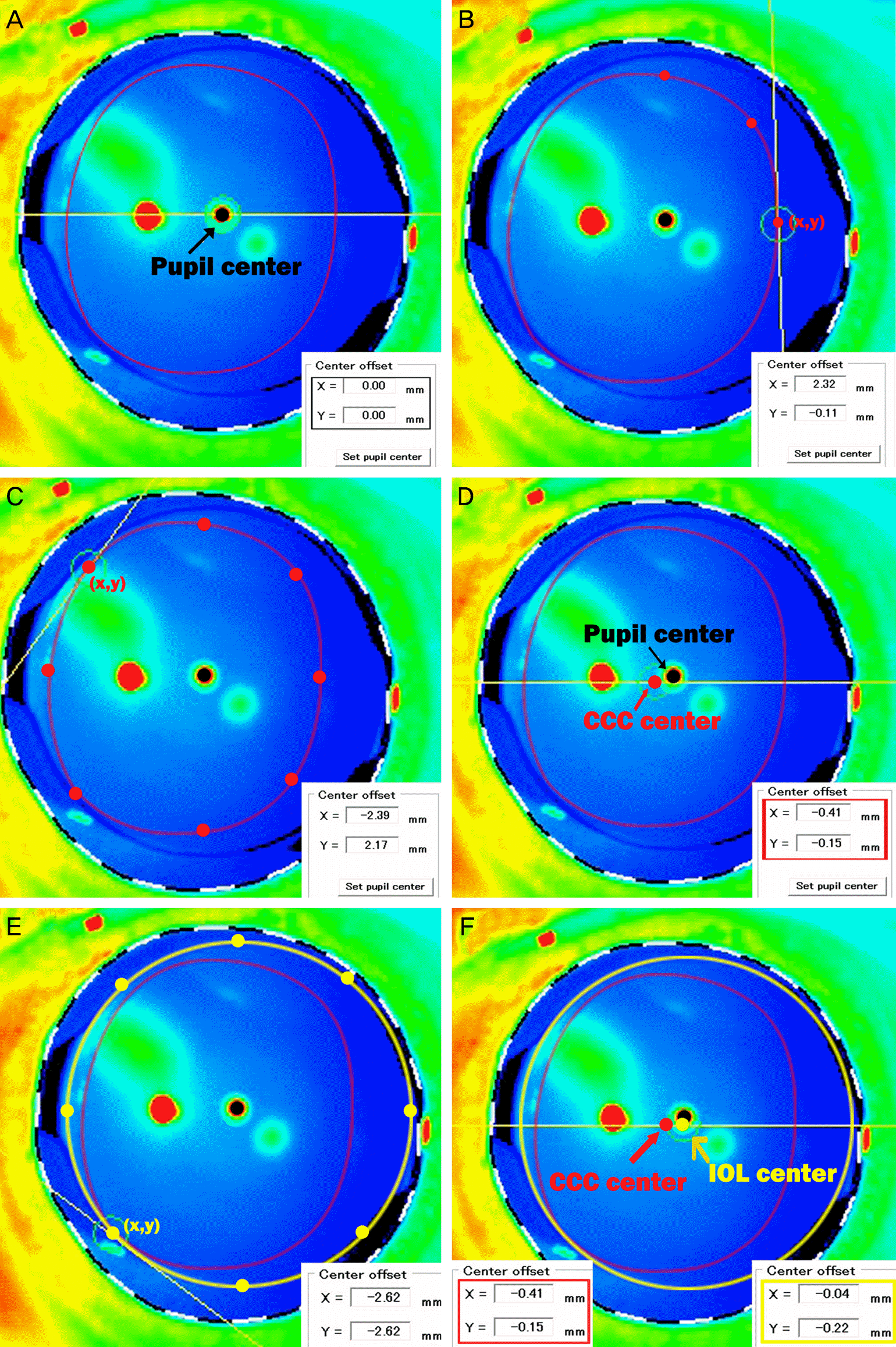 | Figure 1.Anterior segment optical coherence tomography (AS-OCT) images of manually created continuous curvilinear capsulorhexis (CCC) (red line). (A) With CASIA (Tomey, Tokyo, Japan), pupil center could be automatically calculated and setted as (x = 0, y = 0) mm. (B) Displayed value (x, y) of the red point means the distance from pupil (mm). (C) To get the value of CCC center, the values of 8 points in manual CCC margin (per 45 degree) were measured. (D) The mean value of 8 points are presented at the bottom of the image, and displayed as CCC center (red arrow). (E) Intraocular lens (IOL) margin is presented as yellow line. To get the value of IOL center, the values of 8 points in IOL margin (per 45 degree) were measured. (F) CCC center (red arrow) and the value of CCC center (red rectangle), IOL center and the value of IOL center (yellow rectangle). |
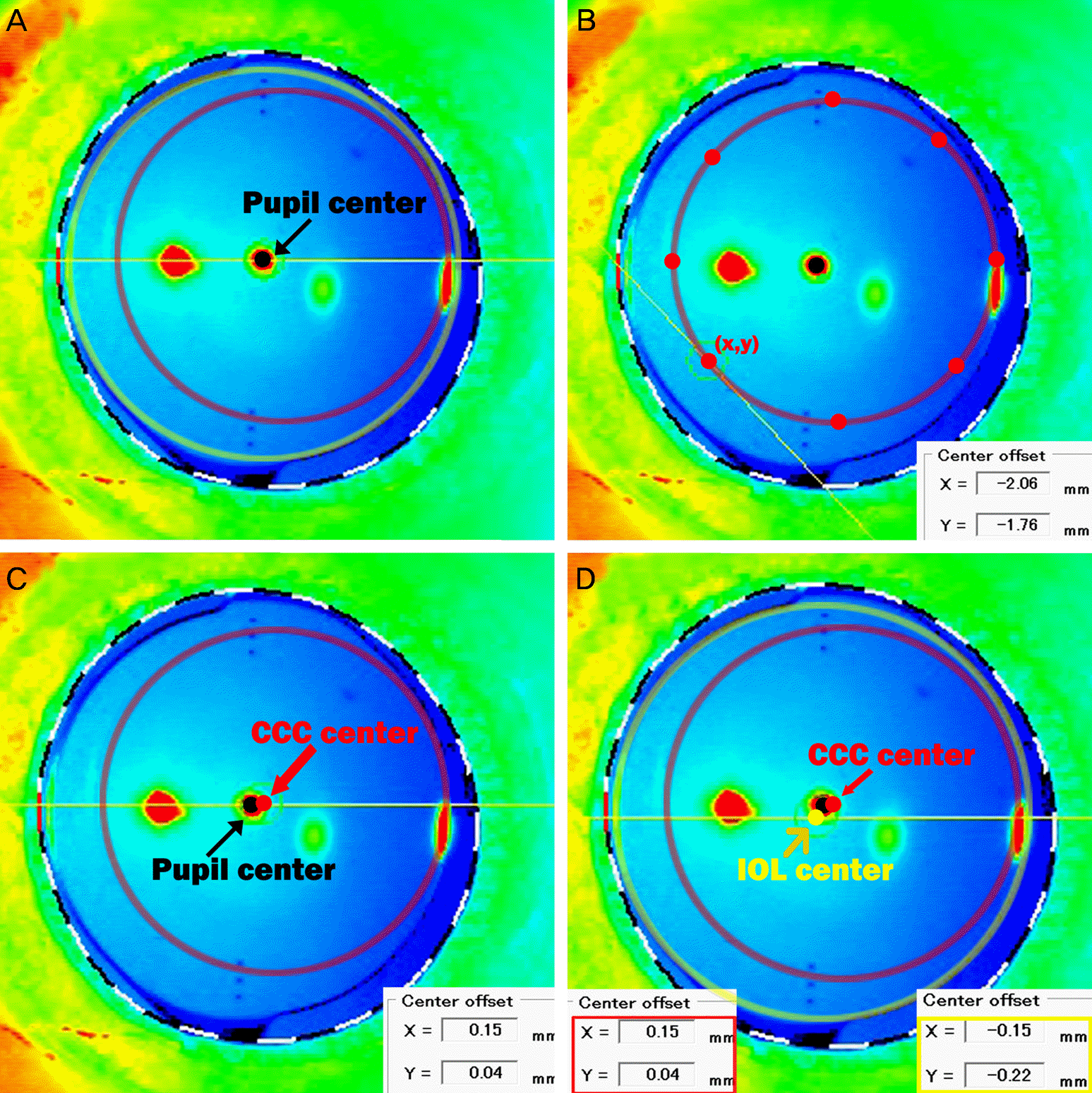 | Figure 2.Anterior segment optical coherence tomography (AS-OCT) images of femtosecond laser created continuous curvilinear capsulorhexis (CCC) (red line). (A) Note the perfectly round and regularly shaped CCC. Intraocular lens (IOL) margin is presented as yellow line. (B) The value of femtosecond laser CCC center was calculated by the same method as manual CCC. (C) The value of femtosecond laser CCC center is presented at the bottom of the image. (D) CCC center (red arrow) and the value of CCC center (red rectangle), IOL center and the value of IOL center (yellow rectangle). |
Table 1.
Demographic data of the patients
| Characteristic | Femtosecond CCC | Manual CCC | p-value |
|---|---|---|---|
| Number of eyes (patients) | 30 (30) | 30 (30) | |
| Age (years) | 64.5 ± 9.1 | 68.2 ± 9.2 | 0.188 |
| Sex (male:female) | 8:22 | 5:25 | 0.347* |
| MRSE (diopter) | −0.66 ± 2.18 | −0.36 ± 5.26 | 0.811 |
| Axial length (mm) | 24.04 ± 1.59 | 23.66 ± 0.90 | 0.249 |
| ACD (mm) | 3.28 ± 0.52 | 3.03 ± 0.64 | 0.190 |
| Mean corneal power (diopter) | 43.66 ± 1.93 | 44.07 ± 1.66 | 0.413 |
| Intraocular lens (number) | |||
| Akreos Adapt AO† | 14 | 0 | |
| iSert 251‡ | 10 | 0 | |
| SN6AT§ | 3 | 20 | |
| SN6AD∏ | 3 | 10 | |
Table 2.
Parameters of capsulorhexis and intraocular lens decentration between the 2 groups 1 month after surgery
Table 3.
Comparison of visual and refractive outcomes between the 2 groups 1 month after surgery




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download