Abstract
Purpose
To compare the outcomes of bilateral lateral rectus recession between 20 and 25 prism diopters (PD) for intermittent exotropia.
Methods
A retrospective study was performed with a total of 584 patients who underwent surgery for intermittent exotropia and were followed up for more than 12 months. The patients were classified into either the 20 PD group (5 mm bilateral rectus muscle recession [BLR]) or the 25 PD group (6 mm BLR). Successful postoperative motor alignment was defined as within 10 PD of exotropia and 4 PD of esotropia.
Results
Cumulative probabilities of surgical success rates for 24 months were 77.9% in the 20 PD group and 54.8% in the 25 PD group, respectively (p < 0.001). Postoperative deviations in recurrence patients were 13.41 ± 3.64 PD and 14.66 ± 3.87 PD (p = 0.062) at postoperative 12 months.
Conclusions
All patients with relatively small angle of exodeviation such as 20 PD had a higher success rate and small postoperative exodaviation at 12 months. Therefore, surgery could be considered when the eye is exodeviated with a relatively small angle. However, in the group with the exotropic drift, approximately 2/3 of the preoperative angle of deviation is measured with similar outcomes between preoperative and postoperative angles of deviation.
Go to : 
References
1. Park JY, Sohn HY, Cho YA. Is the nonsurgical treatment effective on intermittent exotropia in children of school-age? J Korean Ophthalmol Soc. 1995; 36:1561–7.
2. Maruo T, Kubota N, Sakaue T, Usui C. Intermittent exotropia surgery in children: long term outcome regarding changes in binocular alignment. A study of 666 cases. Binocul Vis Strabismus Q. 2001; 16:265–70.
3. Oh JY, Hwang JM. Survival analysis of 365 patients with exotropia after surgery. Eye (Lond). 2006; 20:1268–72.

4. Kim SJ, Choi DG. The clinical analysis after reoperation for recurrent intermittent exotropia. J Korean Ophthalmol Soc. 2007; 48:321–7.
5. Gezer A, Sezen F, Nasri N, Gözüm N. Factors influencing the outcome of strabismus surgery in patients with exotropia. J AAPOS. 2004; 8:56–60.

6. Ruttum MS. Initial versus subsequent postoperative motor alignment in intermittent exotropia. J AAPOS. 1997; 1:88–91.

7. Scott AB, Mash AJ, Jampolsky A. Quantitative guidelines for exotropia surgery. Invest Ophthalmol. 1975; 14:428–36.
8. Richard JM, Parks MM. Intermittent exotropia. Surgical results in different age groups. Ophthalmology. 1983; 90:1172–7.
9. Stoller SH, Simon JW, Lininger LL. Bilateral lateral rectus recession for exotropia: a survival analysis. J Pediatr Ophthalmol Strabismus. 1994; 31:89–92.

10. Kushner BJ. Selective surgery for intermittent exotropia based on distance/near differences. Arch Ophthalmol. 1998; 116:324–8.

11. Jeoung JW, Lee MJ, Hwang JM. Bilateral lateral rectus recession versus unilateral recess-resect procedure for exotropia with a dominant eye. Am J Ophthalmol. 2006; 141:683–8.

12. Ekdawi NS, Nusz KJ, Diehl NN, Mohney BG. Postoperative outcomes in children with intermittent exotropia from a population-based cohort. J AAPOS. 2009; 13:4–7.

13. Lee DE, Kwon JY. The effect of bilateral lateral rectus recession. J Korean Ophthalmol Soc. 1996; 37:167–72.
14. Cho HJ, Ma YR, Park YG. Comparison of surgical results between bilateral and unilateral lateral rectus recession in 20∼25 prism diopters intermittent exotropia. J Korean Ophthalmol Soc. 2002; 43:1993–9.
Go to : 
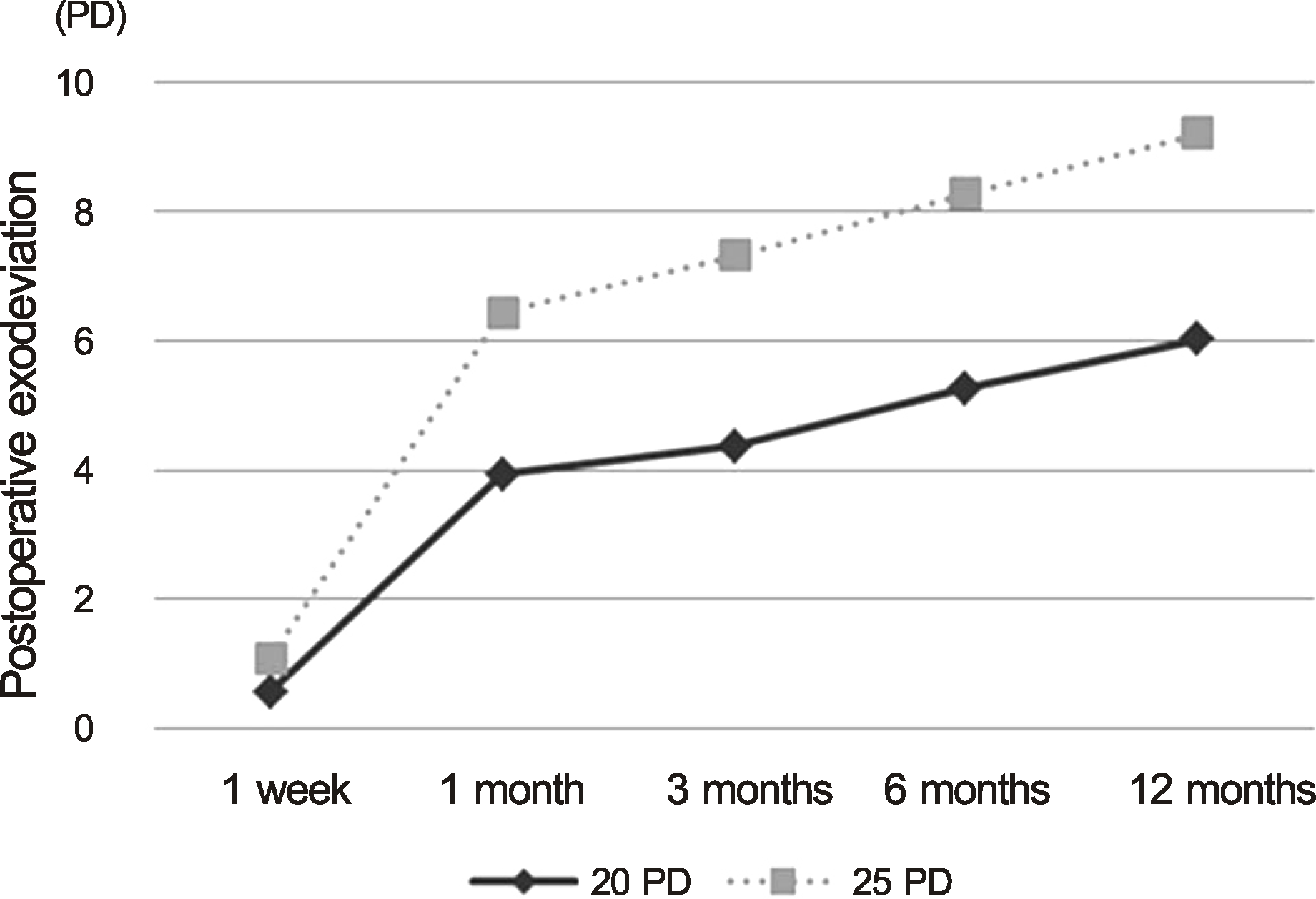 | Figure 1.Surgical outcomes of patients with intermittent exotropia of 20 PD group versus 25 PD group (p < 0.005). PD = prism diopters. |
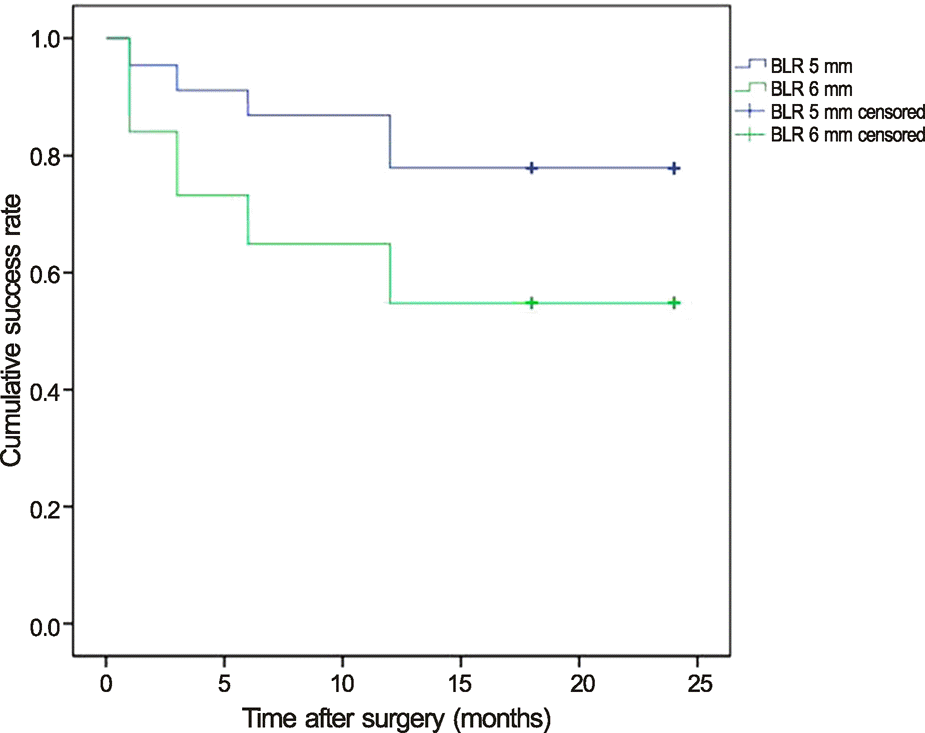 | Figure 2.Kaplan–Meier survival curve showing the cumulative probability of surgical success following a BLR procedure (p < 0.001, log rank test). BLR = bilateral lateral rectus muscle recession. |
Table 1.
Characteristics of patients with 20 PD group versus 25 PD group
| 20 PD group | 25 PD group | p-value | |
|---|---|---|---|
| No. of patients | 259 | 325 | − |
| Sex (M:F) | 131:128 | 150:175 | 0.288∗ |
| Mean age at onset (years) | 3.15 ± 2.13 | 2.95 ± 1.95 | 0.258† |
| Mean age at surgery (years) | 6.66 ± 1.79 | 6.38 ± 1.78 | 0.059† |
| Preoperative angle of exodeviation (PD) | 19.42 ± 1.23 | 24.83 ± 0.95 | − |
| Preoperative refraction (SE) | −0.01 ± 1.33 | 0.00 ± 1.41 | 0.931† |
| Amblyopia | 18 (6.9%) | 13 (4.1%) | 0.107∗ |
Table 2.
Surgical outcomes of patients of 20 PD group versus 25 PD group
|
Mean postoperative exodeviation (PD) |
|||
|---|---|---|---|
| 20 PD group | 25 PD group | p-value∗ | |
| 1 week | 0.57 ± 3.01 | 1.09 ± 3.21 | 0.043 |
| 1 month | 3.94 ± 3.91 | 6.45 ± 4.80 | 0.000 |
| 3 months | 4.37 ± 4.54 | 7.33 ± 5.31 | 0.000 |
| 6 months | 5.27 ± 4.65 | 8.28 ± 5.46 | 0.000 |
| 12 months | 6.03 ± 5.12 | 9.21 ± 6.00 | 0.000 |
Table 3.
Comparisons of cumulative probability of surgical success rate of 20 PD group versus 25 PD group
|
Success rate (%) |
p-value∗ | Odd ratio | ||
|---|---|---|---|---|
| 20 PD group (n = 259) | 25 PD group (n = 325) | |||
| 1 week | 100.0 | 100.0 | − | − |
| 1 month | 95.4 | 84.0 | 0.000 | 3.921 |
| 3 months | 92.7 | 76.9 | 0.000 | 3.789 |
| 6 months | 89.2 | 69.8 | 0.000 | 3.562 |
| 12 months | 83.0 | 59.4 | 0.000 | 3.342 |




 PDF
PDF ePub
ePub Citation
Citation Print
Print


 XML Download
XML Download